Abstract
Introduction
Precision error in bone mineral density (BMD) measurement can be affected by patient positioning, variations in scan analysis, automation of software, and both short- and long-term fluctuations of the densitometry equipment. Minimization and characterization of these errors is essential for reliable assessment of BMD change over time.
Methods
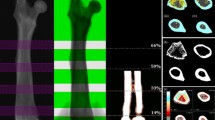
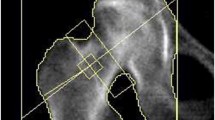
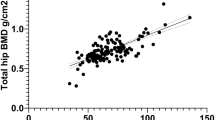
We compared the short-term precision error of two dual-energy X-ray absorptiometry (DXA) devices: the Lunar Prodigy (GE Healthcare) and the Delphi (Hologic). Both are fan-beam DXA devices predominantly used to measure BMD of the spine and proximal femur. In this study, 87 women (mean age 61.6±8.9 years) were measured in duplicate, with repositioning, on both systems, at one of three clinical centers. The technologists were International Society for Clinical Densitometry (ISCD) certified and followed manufacturer-recommended procedures. All scans were acquired using 30-s scan modes. Precision error was calculated as the root-mean-square standard deviation (RMS-SD) and coefficient of variation (RMS-%CV) for the repeated measurements. Right and left femora were evaluated individually and as a combined dual femur precision. Precision error of Prodigy and Delphi measurements at each measurement region was compared using an F test to determine significance of any observed differences.
Results
While precision errors for both systems were low, Prodigy precision errors were significantly lower than Delphi at L1–L4 spine (1.0% vs 1.2%), total femur (0.9% vs 1.3%), femoral neck (1.5% vs 1.9%), and dual total femur (0.6% vs 0.9%). Dual femur modes decreased precision errors by approximately 25% compared with single femur results.
Conclusions
This study suggests that short-term BMD precision errors are skeletal-site and manufacturer specific. In clinical practice, precision should be considered when determining: (a) the minimum time interval between baseline and follow-up scans and (b) whether a statistically significant change in the patient’s BMD has occurred.




Similar content being viewed by others
References
Riggs BL, Wahner HW, Melton LJd, Richelson LS, Judd HL, Offord KP (1986) Rates of bone loss in the appendicular and axial skeletons of women. Evidence of substantial vertebral bone loss before menopause. J Clin Invest 77(5):1487–1491
Cummings SR, Karpf DB, Harris F, Genant HK, Ensrud K, LaCroix AZ, Black DM (2002) Improvement in spine bone density and reduction in risk of vertebral fractures during treatment with antiresorptive drugs. Am J Med 112(4):281–289
Pocock NA, Noakes KA, Griffiths M, Bhalerao N, Sambrook PN, Eisman JA, Freund J (1997) A comparison of longitudinal measurements in the spine and proximal femur using lunar and hologic instruments. J Bone Miner Res 12(12):2113–2118
Faulkner KG (2003) Improving femoral bone density measurements. J Clin Densitom 6(4):353–358
White J, Harris SS, Dallal GE, Dawson-Hughes B (2003) Precision of single vs bilateral hip bone mineral density scans. J Clin Densitom 6(2):159–162
Ellis KJ, Shypailo RJ (1998) Bone mineral and body composition measurements: cross-calibration of pencil-beam and fan-beam dual-energy X-ray absorptiometers. J Bone Miner Res 13(10):1613–1618
Tothill P, Hannan WJ (2000) Comparisons between Hologic QDR 1000W, QDR 4500A, and Lunar Expert dual-energy X-ray absorptiometry scanners used for measuring total body bone and soft tissue. Ann N Y Acad Sci 904:63–71
Gillette-Guyonnet S, Andrieu S, Nourhashemi F, Cantet C, Grandjean H, Vellas B (2003) Comparison of bone mineral density and body composition measurements in women obtained from two DXA instruments. Mech Ageing Dev 124(3):317–321
Tothill P, Avenell A (1994) Errors in dual-energy X-ray absorptiometry of the lumbar spine owing to fat distribution and soft tissue thickness during weight change. Br J Radiol 67(793):71–75
Tataranni P, Pettitt D, Ravussin E (1996) Dual energy X-ray absorptiometry: inter-machine variability. Int J Obes Relat Metab Disord 20:1048-1050
Hui SL, Gao S, Zhou XH, Johnston CC, Jr., Lu Y, Gluer CC, Grampp S, Genant H (1997) Universal standardization of bone density measurements: a method with optimal properties for calibration among several instruments. J Bone Miner Res 12(9):1463–1470
Lu Y, Fuerst T, Hui S, Genant HK (2001) Standardization of bone mineral density at femoral neck, trochanter and Ward’s triangle. Osteoporos Int 12(6):438–444
Genant HK, Grammp S, Gluer CC, Faulkner KG, Jergas MJ, Engelke K, Hagiwara S, Van Kuijk C (1995) Universal standardization for dual x-ray absorptiometry: Patient and phantom cross-calibrations results. J Bone Miner Res 9(10): 1503–1514
El Maghraoui A, Do Santos Zounon AA, Jroundi I, Nouijai A, Ghazi M, Achemlal L, Bezza A, Tazi MA, Abouqual R (2005) Reproducibility of bone mineral density measurements using dual X-ray absorptiometry in daily clinical practice. Osteoporos Int
Leslie WD, Ward LM (2004) Bone density monitoring with the total hip site: time for a re-evaluation? J Clin Densitom 7(3):269–274
Acknowledgement
This work was supported by a grant from GE Healthcare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shepherd, J.A., Fan, B., Lu, Y. et al. Comparison of BMD precision for Prodigy and Delphi spine and femur scans. Osteoporos Int 17, 1303–1308 (2006). https://doi.org/10.1007/s00198-006-0127-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-006-0127-9