Abstract
Introduction and hypothesis
The paravaginal defect has been a topic of active discussion concerning what it is, how to diagnose it, its role in anterior vaginal wall prolapse, and if and how to repair it. The aim of this article was to review the existing literature on paravaginal defect and discuss its role in the anterior vaginal wall support system, with an emphasis on anatomy and imaging.
Methods
Articles related to paravaginal defects were identified through a PubMed search ending 1 July 2015.
Results
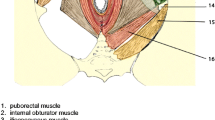
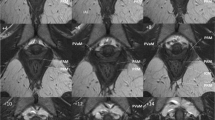
Support of the anterior vaginal wall is a complex system involving levator ani muscle, arcus tendineus fascia pelvis (ATFP), pubocervical fascia, and uterosacral/cardinal ligaments. Studies conclude that physical examination is inconsistent in detecting paravaginal defects. Ultrasound (US) and magnetic resonance imaging (MRI) have been used to describe patterns in the appearance of the vagina and bladder when a paravaginal defect is suspected. Different terms have been used (e.g., sagging of bladder base, loss of tenting), which all represent changes in pelvic floor support but that could be due to both paravaginal and levator ani defects.
Conclusion
Paravaginal support plays a role in supporting the anterior vaginal wall, but we still do not know the degree to which it contributes to the development of prolapse. Both MRI and US are useful in the diagnosis of paravaginal defects, but further studies are needed to evaluate their use.










Similar content being viewed by others
Abbreviations
- ATFP:
-
Arcus tendineus fascia pelvis
- US:
-
Ultrasound
- MRI:
-
Magnetic resonance imaging
References
Maher C, Feiner B, Baessler K, Schmid C. Surgical management of pelvic organ prolapse in women. Cochrane Database Syst Rev. 2013;4
Løwenstein E, Ottesen B, Gimbel H. Incidence and lifetime risk of pelvic organ prolapse surgery in Denmark from 1977 to 2009. Int Urogynecol J. 2015;26(1):49–55.
Gyhagen M, Bullarbo M, Nielsen TF, Milsom I. Prevalence and risk factors for pelvic organ prolapse 20 years after childbirth: a national cohort study in singleton primiparae after vaginal or caesarean delivery. BJOG. 2013;120(2):152–60.
Tegerstedt G, Miedel A, Maehle-Schmidt M, Nyrén O, Hammarström M. Obstetric risk factors for symptomatic prolapse: a population-based approach. Am J Obstet Gynecol. 2006;194(1):75–81.
Richardson AC, Edmonds PB, Williams NL. Treatment of stress urinary incontinence due to paravaginal fascial defect. Obstet Gynecol. 1981;57(3):357–62.
Richardson AC, Lyon JB, Williams NL. A new look at pelvic relaxation. Am J Obstet Gynecol. 1976;126(5):568–73.
White GR. Cystocele−a radical cure by suturing lateral sulci of the vagina to the white line of pelvic fascia. 1909. Int Urogynecol J Pelvic Floor Dysfunct. 1997;8(5):288–92.
Delancey JO. Fascial and muscular abnormalities in women with urethral hypermobility and anterior vaginal wall prolapse. Am J Obstet Gynecol. 2002;187(1):93–8.
Barber MD, Cundiff GW, Weidner AC, Coates KW, Bump RC, Addison WA. Accuracy of clinical assessment of paravaginal defects in women with anterior vaginal wall prolapse. Am J Obstet Gynecol. 1999;181(1):87–90.
Ostrzenski A, Osborne NG, Ostrzenska K. Method for diagnosing paravaginal defects using contrast ultrasonographic technique. J Ultrasound Med. 1997;16(10):673–7.
Ostrzenski A, Osborne NG. Ultrasonography as a screening tool for paravaginal defects in women with stress incontinence: a pilot study. Int Urogynecol J Pelvic Floor Dysfunct. 1998;9(4):195–9.
Hosni MM, El-Feky AE, Agur WI, Khater EM. Evaluation of three different surgical approaches in repairing paravaginal support defects: a comparative trial. Arch Gynecol Obstet. 2013;288(6):1341–8.
Behnia-Willison F, Seman EI, Cook JR, O’Shea RT, Keirse MJ. Laparoscopic paravaginal repair of anterior compartment prolapse. J Minim Invasive Gynecol. 2007;14(4):475–80.
Nguyen JK. Current concepts in the diagnosis and surgical repair of anterior vaginal prolapse due to paravaginal defects. Obstet Gynecol Surv. 2001;56(4):239–46.
DeLancey JO. Anatomic aspects of vaginal eversion after hysterectomy. Am J Obstet Gynecol. 1992;166(6 Pt 1):1717–24.
Macura KJ. Magnetic resonance imaging of pelvic floor defects in women. Top Magn Reson Imaging. 2006;17(6):417–26.
Athanasiou S, Chaliha C, Toozs-Hobson P, Salvatore S, Khullar V, Cardozo L. Direct imaging of the pelvic floor muscles using two-dimensional ultrasound: a comparison of women with urogenital prolapse versus controls. BJOG. 2007;114(7):882–8.
Huddleston HT, Dunnihoo DR, Huddleston 3rd PM, Meyers Sr PC. Magnetic resonance imaging of defects in DeLancey’s vaginal support levels I, II, and III. Am J Obstet Gynecol. 1995;172(6):1778–82.
Mauroy B, Goullet E, Stefaniak X, Bonnal JL, Amara N. Tendinous arch of the pelvic fascia: application to the technique of paravaginal colposuspension. Surg Radiol Anat. 2000;22(2):73–9.
Pit MJ, De Ruiter MC, Lycklama A, Nijeholt AA, Marani E, Zwartendijk J. Anatomy of the arcus tendineus fasciae pelvis in females. Clin Anat. 2003;16(2):131–7.
Fritsch H, Zwierzina M, Riss P. Accuracy of concepts in female pelvic floor anatomy: facts and myths! World J Urol. 2012;30:429–35.
Ersoy M, Sagsoz N, Bozkurt MC, Apaydin N, Elhan A, Tekdemir I. Important anatomical structures used in paravaginal defect repair: cadaveric study. Eur J Obstet Gynecol Reprod Biol. 2004;112(2):206–13.
Albright TS, Gehrich AP, Davis GD, Sabi FL, Buller JL. Arcus tendineus fascia pelvis: a further understanding. Am J Obstet Gynecol. 2005;193(3 Pt 1):677–81.
Cosson M, Boukerrou M, Lacaze S, Lambaudie E, Fasel J, Mesdagh H, et al. A study of pelvic ligament strength. Eur J Obstet Gynecol Reprod Biol. 2003;109(1):80–7.
Shull BL, Baden WF. A six-year experience with paravaginal defect repair for stress urinary incontinence. Am J Obstet Gynecol. 1989;160(6):1432–9.
Claydon CS, Maccarone JL, Grody MH, Steinberg A, Oyama I, Holzberg AS, et al. The distance between the perceived and the actual arcus tendineus fascia pelvis during vaginal paravaginal repair. Am J Obstet Gynecol. 2005;192(5):1707–11.
Miklos JR, Kohli N. Laparoscopic paravaginal repair plus burch colposuspension: review and descriptive technique. Urology. 2000;4(56):64–9.
Larson KA, Hsu Y, Chen L, Ashton-Miller JA, DeLancey JO. Magnetic resonance imaging-based three-dimensional model of anterior vaginal wall position at rest and maximal strain in women with and without prolapse. Int Urogynecol J. 2010;21(9):1103–9.
Larson KA, Luo J, Guire KE, Chen L, Ashton-Miller JA, DeLancey JO. 3D analysis of cystoceles using magnetic resonance imaging assessing midline, paravaginal, and apical defects. Int Urogynecol J. 2012;23(3):285–93.
Summers A, Winkel LA, Hussain HK, DeLancey JO. The relationship between anterior and apical compartment support. Am J Obstet Gynecol. 2006;194(5):1438–43.
Rooney K, Kenton K, Mueller ER, FitzGerald MP, Brubaker L. Advanced anterior vaginal wall prolapse is highly correlated with apical prolapse. Am J Obstet Gynecol. 2006;195(6):1837–40.
Hsu Y, Chen L, Summers A, Ashton-Miller JA, DeLancey JO. Anterior vaginal wall length and degree of anterior compartment prolapse seen on dynamic MRI. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19(1):137–42.
Ramanah R, Berger MB, Parratte BM, DeLancey JO. Anatomy and histology of apical support: a literature review concerning cardinal and uterosacral ligaments. Int Urogynecol J. 2012;23(11):1483–94.
Buller JL, Thompson JR, Cundiff GW, Krueger Sullivan L, Schön Ybarra MA, Bent AE. Uterosacral ligament: description of anatomic relationships to optimize surgical safety. Obstet Gynecol. 2001;97(6):873–9.
Umek WH, Morgan DM, Ashton-Miller JA, DeLancey JO. Quantitative analysis of uterosacral ligament origin and insertion points by magnetic resonance imaging. Obstet Gynecol. 2004;103(3):447–51.
Range RL, Woodburne RT. The gross and microscopic anatomy of the transverse cervical ligaments. Am J Obstet Gynecol. 1964;90:460.
DeLancey JO, Starr RA. Histology of the connection between the vagina and levator ani muscles. Implications for urinary tract function. J Reprod Med. 1990;35(8):765–71.
Jung SA, Pretorius DH, Padda BS, Weinstein MM, Nager CW, den Boer DJ, et al. Vaginal high-pressure zone assessed by dynamic 3-dimensional ultrasound images of the pelvic floor. Am J Obstet Gynecol. 2007;197(1):52.e1–7.
DeLancey JO, Morgan DM, Fenner DE, Kearney R, Guire K, Miller JM, et al. Comparison of levator ani muscle defects and function in women with and without pelvic organ prolapse. Obstet Gynecol. 2007;109(2 Pt 1):295–302.
Dietz HP, Simpson JM. Levator trauma is associated with pelvic organ prolapse. BJOG. 2008;115(8):979–84.
Lammers K, Fütterer JJ, Prokop M, Vierhout ME, Kluivers KB. Diagnosing pubovisceral avulsions: a systematic review of the clinical relevance of a prevalent anatomical defect. Int Urogynecol J. 2012;23(12):1653–64.
Berger MB, Morgan DM, DeLancey JO. Levator ani defect scores and pelvic organ prolapse: is there a threshold effect? Int Urogynecol J. 2014;25(10):1375–9.
Shull BL. Clinical evaluation of women with pelvic support defects. Clin Obstet Gynecol. 1993;36(4):939–51.
Segal JL, Vassallo BJ, Kleeman SD, Silva WA, Karram MM. Paravaginal defects: prevalence and accuracy of preoperative detection. Int Urogynecol J Pelvic Floor Dysfunct. 2004;15(6):378–83.
Whiteside JL, Barber MD, Paraiso MF, Hugney CM, Walters MD. Clinical evaluation of anterior vaginal wall support defects: interexaminer and intraexaminer reliability. Am J Obstet Gynecol. 2004;191(1):100–4.
Martan A, Masata J, Halaska M, Otcenásek M, Svabik K. Ultrasound imaging of paravaginal defects in women with stress incontinence before and after paravaginal defect repair. Ultrasound Obstet Gynecol. 2002;19:496–500.
Nguyen JK, Hall CD, Taber E, Bhatia NN. Sonographic diagnosis of paravaginal defects: a standardization of technique. Int Urogynecol J Pelvic Floor Dysfunct. 2000;11(6):341–5.
Ochsenbein N, Kurmanavicius J, Huch R, Huch A, Wisser J. Volume sonography of the pelvic floor in nulliparous women and after elective cesarean section. Acta Obstet Gynecol Scand. 2001;80(7):611–5.
Dietz HP, Pang S, Korda A, Benness C. Paravaginal defects: a comparison of clinical examination and 2D/3D ultrasound imaging. Aust N Z J Obstet Gynaecol. 2005;45(3):187–90.
Cassadó-Garriga J, Wong V, Shek K, Dietz HP. Can we identify changes in fascial paravaginal supports after childbirth? Aust N Z J Obstet Gynaecol. 2015;55(1):70–5.
Spahlinger DM, Newcomb L, Ashton-Miller JA, DeLancey JO, Chen L. Relationship between intra-abdominal pressure and vaginal wall movements during Valsalva in women with and without pelvic organ prolapse: technique development and early observations. Int Urogynecol J. 2014;25(7):873–.1.
Aronson MP, Bates SM, Jacoby AF, Chelmow D, Sant GR. Periurethral and paravaginal anatomy: an endovaginal magnetic resonance imaging study. Am J Obstet Gynecol. 1995;173(6):1702–8.
Huebner M, Margulies RU, DeLancey JO. Pelvic architectural distortion is associated with pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19(6):863–7.
Larson KA, Luo J, Yousuf A, Ashton-Miller JA, Delancey JO. Measurement of the 3D geometry of the fascial arches in women with a unilateral levator defect and “architectural distortion”. Int Urogynecol J. 2012;23(1):57–63.
Tillack AA, Joe BN, Yeh BM, Jun SL, Kornak J, Zhao S, et al. Vaginal shape at resting pelvic MRI: predictor of pelvic floor weakness? Clin Imaging. 2015;39(2):285–8.
Acknowledgments
Dr. DeLancey gratefully acknowledges NIH grants P50 HD044406 and R01 HD038665 that provide support for his effort.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
LTS Arenholt has accepted travel grant from Astellas and has consulted Astellas on topics not relevant to this manuscript. M. Glavind-Kristensen and K. Glavind have accepted travel grants from Astellas.
Rights and permissions
About this article
Cite this article
Arenholt, L.T.S., Pedersen, B.G., Glavind, K. et al. Paravaginal defect: anatomy, clinical findings, and imaging. Int Urogynecol J 28, 661–673 (2017). https://doi.org/10.1007/s00192-016-3096-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-016-3096-3