Abstract
Purpose
Oxford microplasty (MP) instrumentation has been developed to facilitate the reproducible and consistent performance of minimally invasive unicompartmental knee arthroplasty (MI-UKA) operation. The aim of this study was to compare the clinical and radiographic results of two groups of patients implanted using either a conventional instrumentation technique or an MP technique.
Methods
A prospective cohort study of 108 knees in 108 patients who underwent an MI-UKA procedure using either conventionally instrumented UKA (CI-UKA) (52 knees of 52 patients) or MP-assisted UKA (MP-UKA) (56 knees of 56 patients). The clinical assessment included the Oxford Knee Score (OKS), the Knee Society Score (KSS), a visual analogue scale (VAS) for pain, and range of motion (ROM). Complications were also recorded.
Results
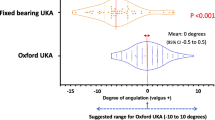
No significant differences were observed between the two groups regarding OKS, KSS, VAS, and ROM. There were also no significant differences in terms of mechanical limb alignment and tibia implant alignment. However, the MP-UKA group showed significantly more accurate positioning of the femoral component than the CI-UKA group. Additionally, the MP-UKA group had more femoral prostheses implanted in the “satisfactory” range and fewer “outliers” than the CI-UKA group. No significant difference in complications was noted between the two groups.
Conclusion
This study suggested that compared with CI-UKA, MP-UKA provides significant improvements in increasing the accuracy of sagittal and coronal implantation of the femoral component and in reducing the numbers of outliers for femoral prosthetic alignment. It is advocated that the MP system should be considered when MI-UKA is performed.
Level of evidence
Therapeutic study, Level IV.


Similar content being viewed by others
References
Dawson J, Fitzpatrick R, Murray D, Carr A (1998) Questionnaire on the perceptions of patients about total knee replacement. J Bone Jt Surg Br 80-B:63–69
Emerson RH Jr, Hansborough T, Reitman RD, Rosenfeldt W, Higgins LL (2002) Comparison of a mobile with a fixed-bearing unicompartmental knee implant. Clin Orthop Relat Res 404:62–70
Ewald FC (1989) The Knee Society total knee arthroplasty roentgenographic evaluation and scoring system. Clin Orthop Relat Res 248:9–12
Faour-Martín O, Valverde-García JA, Martín-Ferrero MA, Vega-Castrillo A, de la Red Gallego MA, Suárez de Puga CC, Amigo-Liñares L (2013) Oxford phase 3 unicondylar knee arthroplasty through a minimally invasive approach: long-term results. Int Orthop 37(5):833–838
Fisher DA, Watts M, Davis KE (2003) Implant position in knee surgery: a comparison of minimally invasive, open unicompartmental, and total knee arthroplasty. J Arthroplast 18(7 Suppl 1):2–8
Gulati A, Weston-Simons S, Evans D, Jenkins C, Gray H, Dodd CA, Pandit H, Murray DW (2014) Radiographic evaluation of factors affecting bearing dislocation in the domed lateral Oxford unicompartmental knee replacement. Knee 21(6):1254–1257
Hernigou P, Deschamps G (2004) Alignment influences wear in the knee after medial unicompartmental arthroplasty. Clin Orthop Relat Res 423:161–165
Huang TW, Peng KT, Huang KC, Lee MS, Hsu RW (2014) Differences in component and limb alignment between computer-assisted and conventional surgery total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 22(12):2954–2961
Keene G, Simpson D, Kalairajah Y (2006) Limb alignment in computer-assisted minimally-invasive unicompartmental knee replacement. J Bone Jt Surg Br 88:44–48
Kort NP, van Raay JJ, Cheung J, Jolink C, Deutman R (2007) Analysis of Oxford medial unicompartmental knee replacement using the minimally invasive technique in patients aged 60 and above: an independent prospective series. Knee Surg Sports Traumatol Arthrosc 15(11):1331–1334
Kort NP, van Raay JJ, Thomassen BJ (2007) Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty: a study in 10 cadaver femora. Knee 14:280–283
Lim HC, Bae JH, Song SH, Kim SJ (2012) Oxford phase 3 unicompartmental knee replacement in Korean patients. J Bone Jt Surg Br 94(8):1071–1076
Ma B, Long W, Rudan JF, Ellis RE (2006) Three-dimensional analysis of alignment error in using femoral intramedullary guides in unicompartmental knee arthroplasty. J Arthroplasty 21(2):271–278
Mayman DJ, Rudan J, Watson D, Ellis R (2004) Computer-enhanced insertion of the Oxford unicompartmental arthroplasty: a fluoroguide technique. Comput Aided Surg 9:81–85
Murray DW, Goodfellow JW, O’Connor JJ (1998) The Oxford medial unicompartmental arthroplasty: a ten year survival study. J Bone Jt Surg Br 80:983–989
Murray DW, Goodfellow JW, O’Connor JJ, Dodd CA (1999) Oxford unicompartmental knee: manual of the surgical technique. Biomet UK Ltd, Bridgend, pp 1–40
Pandit H, Jenkins C, Barker K, Dodd CA, Murray DW (2006) The Oxford medial unicompartmental knee replacement using a minimally-invasive approach. J Bone Jt Surg Br 88(1):54–60
Rosenberger RE, Fink C, Quirbach S, Attal R, Tecklenburg K, Hoser C (2008) The immediate effect of navigation on implant accuracy in primary mini-invasive unicompartmental knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 16:1133–1140
Skowroński J, Jatskewych J, Długosz J, Skowroński R, Bielecki M (2005) The Oxford II medial unicompartmental knee replacement. A minimum 10-year follow-up study. Ortop Traumatol Rehabil 7(6):620–625
Stulberg SD, Loan P, Sarin V (2002) Computer-assisted navigation in total knee replacement: results of an initial experience in thirty-five patients. J Bone Jt Surg Am 84:90–98
Svärd VC, Price AJ (2001) Oxford medial unicompartmental arthroplasty: a survival analysis of an independent series. J Bone Jt Surg Br 83:191–194
Tu Y, Xue H, Cai M, Ma T, Liu X, Xia Z (2014) Improvement of femoral component size prediction using a C-arm intensifier guide and our established algorithm in unicompartmental knee arthroplasty: a report from a Chinese population. Knee 21(2):435–438
Vasso M, Del Regno C, D’Amelio A, Viggiano D, Corona K, Schiavone Panni A (2015) Minor varus alignment provides better results than neutral alignment in medial UKA. Knee 22(2):117–121
Yoshida K, Tada M, Yoshida H, Takei S, Fukuoka S, Nakamura H (2013) Oxford phase 3 unicompartmental knee arthroplasty in Japan—clinical results in greater than one thousand cases over ten years. J Arthroplasty 28(9 Suppl):168–171
Acknowledgments
This study was supported by the National Natural Science Foundation of China (No. 81301566), Shanghai Municipal Public Health and Family Planning Commission (No. 2013040) and Shanghai Municipal Science and Technology Commission (No. 134119b1400). The authors wish to thank Dr. David W. Murray, Professor of Orthopaedics at the Nuffield Orthopaedics Centre, Oxford University, for his contribution to technical guidance and manuscript preparation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tu, Y., Xue, H., Ma, T. et al. Superior femoral component alignment can be achieved with Oxford microplasty instrumentation after minimally invasive unicompartmental knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 25, 729–735 (2017). https://doi.org/10.1007/s00167-016-4173-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-016-4173-3