Abstract
Background
Most cultures in sub-Saharan Africa subscribe to the belief that the root cause of psychosis is supernatural. Individuals in the community who hold a religiomagical explanatory model of causation have been shown to exhibit more stigmatizing attitudes towards people with psychosis. Self-stigma among individuals with psychosis is less frequently studied.
Method
We used a mixed-method approach, consisting of key informant’s interviews to elicit information on explanatory models of causation of psychosis and questionnaire assessment of internalized stigma with an adapted version of the Scale for Internalized Stigma of Mental Illness. Twenty-four, 31, and 30 subjects with recent experience of utilizing the service of traditional or faith healers for severe mental disorders in Ibadan (Nigeria), Kumasi (Ghana), and Nairobi (Kenya), respectively, were interviewed.
Results
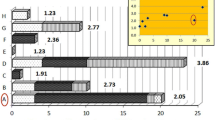
About 44 % (42.1 %) of the Nigerian respondents had a high (severe) level of self-stigma with the respective proportions among Ghanaian and Kenyan respondents being 20.7 and 37.5 %. Compared with 4 out of a total of 12 respondents (33.3 %) who reported low self-stigma reported supernatural attribution, 14 out of 20 respondents (70 %) with the highest level of self-stigma reported supernatural attribution across the three sites. When low scorers ascribed supernatural causation, it was often with a religious focus.
Conclusion
There is a greater tendency for persons with high levels of self-stigma than those with low levels to ascribe supernatural attribution to their experience of a severe mental health condition.

Similar content being viewed by others
References
World Health Report (2001) Mental health: new understanding, new hope. World Health Organisation, Geneva
Sorsdahl K, Stein DJ, Grimsrud A, Seedat S, Flisher AJ, Williams DR, Myer L (2009) Traditional healers in the treatment of common mental disorders in South Africa. J Nerv Ment Dis 197(6):434
Charles H, Manoranjitham SD, Jacob KS (2007) Stigma and explanatory models among people with schizophrenia and their relatives in Vellore, South India. Int J Soc Psychiatry 53(4):325–332
Ilechukwu ST (1988) Inter-relationships of beliefs about mental illness, psychiatric diagnoses and mental health care delivery among Africans. Int J Soc Psychiatry 34(3):200–206 (1988 Autumn)
Angermeyer MC, Matschinger H (1996) Public attitude towards psychiatric treatment. Acta Psychiatr Scand 94(5):326–336
Al-Krenawi A, Graham JR (1997) Spirit possession and exorcism: the integration of modern and traditional mental health care systems in the treatment of a Bedouin patient. Clin Soc Work J 25:211–222
Razali SM, Khan UA, Hasanah CI (1996) Belief in supernatural causes of mental illness among Malay patients: impact on treatment. Acta Psychiatr Scand 94(4):229–233
Nwoko KC (2009) Traditional psychiatric healing in Igbo land, Southeastern Nigeria. Afr J Hist Cult (AJHC) 1(2):036–043
Kabir M, Iliyasu Z, Abubakar IS, Aliyu MH (2004) Perception and beliefs about mental illness among adults in Karfi village, northern Nigeria. BMC Int Health Hum Rights 20:3. doi:10.1186/1472-698X-4-3
Abbo C, Okello E, Ekblad S, Waako P, Musisi S (2008) Lay concepts of psychosis in Busoga, Eastern Uganda: a pilot study. World Cult Psychiatry Res Rev 3(3):132–145
Sorsdahl KR, Stein DJ (2010) Knowledge of and stigma associated with mental disorders in a South African community sample. J Nerv Ment Dis 198:742–747
Atilola O (2015) Level of community mental health literacy in sub-Saharan Africa: current studies are limited in number, scope, spread, and cognizance of cultural nuances. Nord J Psychiatry 69:93–101
Krenawi Al (1999) Explanations of psychiatric symptoms by bedouin Arabs of the Negev. Int J Soc Psyhciatry 45(1):56–64
Al Isaa I (1990) Culture and mental illness in Algeria. Int J Of Soc Psychiatry 36:230–240
Khoury NM, Kaiser BN, Keys HM, Brewster ART, Kohrt BA (2012) Explanatory models and mental health treatment: is vodou an obstacle to psychiatric treatment in rural Haiti? Cult Med Psychiatry 36(3):514–534
Shankar BR, Saravanan B, Jacob KS (2006) Explanatory models of common mental disorders among traditional healers and their patients in rural south India. Int J Soc Psychiatry 52(3):221–233
Stephen M, Suryani LK (2000) Shamanism, psychosis and autonomous imagination. Cult Med Psychiatry 24(1):5–38
Goffman E (1963) Stigma: notes on the management of spoiled identity. Prentice-Hall, New York
Link BG, Phelan JC (2001) Conceptualizing stigma. Ann Rev Sociol 27:363–385
Sathyaseelan M, Seema P, Maret J, Saravanan B, Ezhilrasu P, Jacob KS (2001) Patient perspectives on psychosis. Indian J Psychiatry 43:72
Gureje O, Olley B, Olusola F, Kola L (2006) Do beliefs about causation influence attitudes to mental illness?. World Psychiatry 5:104–107
Yanos PT, Roe D, Marcus K, Lysaker PH (2008) Pathway between internalized stigma outcomes related to recovery in schizophrenia spectrum disorders. Psychiatric Serv 59:1437–1442
Lysaker PH, Tsai J, Yanos P, Roe D (2008) Associations of multiple domains of self-esteem with four dimensions of stigma in schizophrenia. Schizophr Res 98:194–200
Lysaker PH, Roe D, Yanos PT (2007) Toward understanding the insight paradox: internalised stigma moderates the association between insight and social functioning, hope and self-esteem among people with schizophrenia spectrum disorders. Schizophr Bull 33:192–199
Ritsher JB, Otilingam PG, Grajales M (2003) Internalized stigma of mental illness: psychometric properties of a new measure. Psychiatry Res 121(1):31–49
Watson AC, Corrigan P, Larson JE, Sells M (2007) Self-stigma in people with mental illness. Schizophr Bull 33(6):1312–1318
Vauth R, Kleim B, Wirtz M, Corrigan PW (2007) Self-efficacy and empowerment as outcomes of self-stigmatizing and coping in schizophrenia. Psychiatry Res 150(1):71–80
Corrigan PW, Calabrese JD (2005) Strategies for assessing and diminishing self-stigma. In: Corrigan PW (ed) On the stigma of mental illness: practical strategies for research and social change. American Psychological Association, Washington, DC, pp 239–256
Corrigan PW, Watson AC (2002) The paradox of self stigma and mental illness. Clin Psychol 9:35–53
MacInnes DL, Lewis M (2008) The evaluation of a short group programme to reduce self-stigma in people with serious and enduring mental health problems. J Psychiatr Ment Health Nurs 15:59–65
Ritsher JB, Phelan JC (2004) Internalized stigma predicts erosion of morale among psychiatric outpatients. Psychiatry Res 129(3):257–265
Groleau D, Young A, Kirmayer LJ (2006) The McGill Illness Narrative Interview (MINI): an interview schedule to elicit meanings and modes of reasoning related to illness experience. Transcult psychiatry 43(4):671–691
Hwang TY, Lee WK, Han ES, Kwon EJ (2006) A study on the reliability and validity of the korean version of internalized stigma of mental illness scale (K-ISMI) [in Korean]. J Korean Neuropsychiatr Assoc 45:418–426
Ersoy MA, Varan A (2007) Reliability and validity of the Turkish version of the internalized stigma of mental illness scale [in Turkish]. Turk Psikiyatri Derg 18:163–171
Sibitz I, Friedrich ME, Unger A, Bachmann A, Benesch T et al (2013) Internalized stigma of schizophrenia: validation of the German version of the internalized stigma of mental illness-scale (ISMI) [in German]. Psychiatr Prax 40:83–91
Boyd JE, Adler EP, Otilingam PG, Peters T (2014) Internalized stigma of mental illness (ISMI) scale: a multinational review. Compr Psychiatry 55(1):221–231. doi:10.1016/j.comppsych.2013.06.005 (Epub 2013 Sep 21)
Adewuya AO, Owoeye AO, Erinfolami AO, Ola BA (2010) Correlates of self-stigma among outpatients with mental illness in Lagos, Nigeria. Int J Soc Psychiatry 57:418–427
Mosanya TJ, Adelufosi AO, Adebowale OT, Ogunwale A, Adebayo OK (2014) Self-stigma, quality of life and schizophrenia: an outpatient clinic survey in Nigeria. Int J Soc Psychiatry 60(4):377–386. doi:10.1177/0020764013491738 (Epub 2013 Jul 3)
Gureje O, Lasebikan V, Ephraim-Oluwanuga O, Olley B, Kola L (2005) Community study of knowledge and attitude to mental illness in Nigeria. Br J Psychiatry 186:436–441
Adewuya A, Makanjuola R (2008) Social distance towards people with mental illness in South-Western Nigeria. Aust N Z J Psychiatry 42:389–395
Dickerson F, Sommerville J, Origoni A, Ringel N, Parente F (2002) Experience of stigma among outpatients with Schizophrenia. Schizophr Bull 28:143–155
Dinos S, Stevens S, Serfaty M, Weich S, King M (2004) Stigma: the feelings and experiences of 46 people with mental illness: qualitative study. Br J Psychiatry 184:176–181
Brohan E, Elgie R, Sartorious N, Thornicroft G (2010) Self-stigma, empowerment and perceived discrimination among people with schizophrenia in 14 European countries: the Gamian-Europe Study. Schizophr Res 122:232–238
Barke A, Nyarko S, Klecha D (2011) The stigma of mental illness in Southern Ghana: attitudes of the urban population and patients’ views. Soc Psychiatry Psychiatr Epidemiol 46(11):1191–1202
Quinn N (2007) Beliefs and community responses to mental illness in Ghana: the experiences of family carers. Int J Soc Psychiatry 53(2):175–188
Dako-Gyeke M, Asumang ES (2013) Stigmatization and discrimination experiences of persons with mental illness: insights from a Qualitative Study in Southern Ghana. Soc Work Soc 11(1):1–14
Franklin RR, Sarr D, Gueye M, Sylla O, Collignon R (1996) Cultural response to mental illness in senegal: reflections through patient companions–Part 1. methods and descriptive data. Soc Sci Med 42(3):325–338
Johnson S, Sathyaseelan M, Charles H, Jeyaseelan V, Jacob KS (2012) Insight, psychopathology, explanatory models and outcome of schizophrenia in India: a prospective 5-year cohort study. BMC psychiatry 12(1):159
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical standards
This study was approved by the ethics review committee of the participating institutions and has been carried out in full compliance with standards laid down in the 1964 declaration of Helsinki and its later amendments. All respondent gave informed consent prior to the interviews.
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Rights and permissions
About this article
Cite this article
Makanjuola, V., Esan, Y., Oladeji, B. et al. Explanatory model of psychosis: impact on perception of self-stigma by patients in three sub-saharan African cities. Soc Psychiatry Psychiatr Epidemiol 51, 1645–1654 (2016). https://doi.org/10.1007/s00127-016-1274-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-016-1274-8