Abstract
Purpose
Trauma care poses many challenges in small hospitals in rural settings. This report was designed to assess the role of a rural general surgeon with trauma patients.
Methods
A cohort study was designed using a retrospective analysis of a cohort at Bozkır Community Hospital that included trauma patients admitted to the emergency department between June 2007 and May 2009. The patients of group 1 were those treated during the first year of the study period, when the hospital staff was only non-specialist physicians. In the second year, a general surgeon was added to the staff, and the patients from this period constituted group 2.
Results
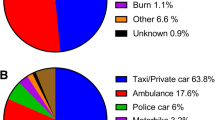
The top three leading causes of injuries were falls (46.5 %), piercing/cutting injuries (38.2 %), and assault (6.5 %). The frequency of trauma due to falls was higher in group 1, and assault and piercing/cutting injuries were higher in group 2 (p < 0.001 for each). The percentage of discharged and transferred patients was not significantly different between groups (p = 0.065 and p = 0.082, respectively). Similar mortality rates were also detected (group 1: 0.5 %, group 2: 0.3 %, p = 0.479).
Conclusions
The presence of a solo general surgeon was not found to be adequate for improving the outcome for trauma patients in a rural hospital.
Similar content being viewed by others
References
Rogers FB, Madsen L, Shackford S, Crookes B, Charash W, Morrow P, Osler T, Jawa R, Rebuck JA, Igneri P. A needs assessment for regionalization of trauma care in a rural state. Am Surg. 2005;71:690–3.
Coben JH, Tiesman HM, Bossarte RM, Furbee PM. Rural-urban differences in injury hospitalizations in the US, 2004. Am J Prev Med. 2009;36:49–55.
McSwain N, Rotondo M, Meade P, Duchesne J. A model for rural trauma care. Br J Surg. 2012;99:309–14.
Ball CG, Sutherland FR, Dixon E, Feliciano DV, Datta I, Rajani RR, Hannay S, Gomes A, Kirkpatrick AW. Surgical trauma referrals from rural level III hospitals: should our community colleagues be doing more, or less? J Trauma. 2009;67:180–4.
Kahramansoy N, Gürbüz N, Kurt F, Erkol H, Boztas G. Gender differences in trauma mechanisms, and outcomes in a rural hospital which is not designed as trauma centre. Emerg Med J. 2013;30:e16.
Kahramansoy N, Erkol H, Kurt F, Gürbüz N, Bozgeyik M, Kıyan A. Analysis of trauma patients in a rural hospital in Turkey. Ulus Travma Acil Cerrahi Derg. 2011;17:231–7.
Ruby BJ, Cogbill TH, Gardner RS. Role of the rural general surgeon in a statewide trauma system: the Wyoming experience. Bull Am Coll Surg. 2006;91:37–40.
Bintz M, Cogbill TH, Bacon J. Rural trauma care: role of the general surgeon. J Trauma. 1996;41:462–4.
National Census statistics, Statistical Agency of Turkey. http://www.tuik.gov.tr/. Accessed 8 Aug 2015.
American College of Surgeons Committee on Trauma. Statement on trauma center designation based upon system need. Bull Am Coll Surg. 2015;100:51–2.
Kappel DA, Rossi DC, Polack EP, Avtgis TA, Martin MM. Does the rural trauma team development course shorten the interval from trauma patient arrival to decision to transfer? J Trauma. 2011;70:315–9.
McCrum ML, McKee J, Lai M, Staples J, Switzer N, Widder SL. ATLS adherence in the transfer of rural trauma patients to a level I facility. Injury. 2013;44:1241–5.
Zulick L, Dietz PA, Brooks K. Trauma experience of a rural hospital. Arch Surg. 1991;126:1427–30.
Bowman SM, Zimmerman FJ, Sharar SR, Baker MW, Martin DP. Rural trauma: is trauma designation associated with better hospital outcomes? J Rural Health. 2008;24:263–8.
Padrón-Arredondo G. General surgery in a rural hospital in the State of Quintana Roo. Mex Cir Cir. 2006;74:115–20.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Author, Fatih Basak, declares that he has no conflict of interest.
Rights and permissions
About this article
Cite this article
Basak, F. Addition of a general surgeon without addition of appropriate support is inadequate to improve outcomes of trauma patients in a rural setting: a cohort study of 1962 consecutive patients. Eur J Trauma Emerg Surg 43, 835–839 (2017). https://doi.org/10.1007/s00068-016-0736-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-016-0736-8