Abstract
Objective
To analyze the in vivo effect of Escherichia coli Nissle 1917 (EcN) with different courses and different doses to Sprague–Dawley rats with trinitrobenzene sulfonic acid (TNBS)-induced colitis.
Methods
The probiotic was orally administered with different courses of treatment (with or without pre-administration) and different doses (107–109 CFU/day) to Sprague–Dawley rats with TNBS-induced colitis. Therapeutic effects, levels of cytokine in serum, mRNA and protein expression were analyzed.
Results
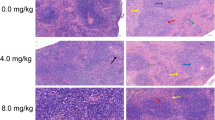
Oral EcN administration after TNBS-induced improved colitis dose dependently. In parallel, a reduction of disease activity index and colonic MPO activity together with a decreased level of TNF-α and a trend of increased IL-10 expression was detected. Pre-administration of 107 CFU/day EcN to TNBS-treated rats resulted in a significant protection against inflammatory response and colons isolated from these rats exhibited a more pronounced expression of ZO-1 than the other groups. In the group of pre-administration of 109 CFU/day, the condition was not improved but deteriorated.
Conclusions
This study convincingly demonstrates that pre-administration of probiotic EcN with low dose is able to protect colitis of rats and mediate up-regulation of ZO-1 expression, but long-term of high-dose EcN may do harm to colitis.






Similar content being viewed by others
References
Talley NJ, Abreu MT, Achkar JP, Bernstein CN, Dubinsky MC, Hanauer SB, et al. An evidence-based systematic review on medical therapies for inflammatory bowel disease. Am J Gastroenterol. 2011;106(Suppl 1):S2–25 quiz S26.
Wang Y, Ouyang Q. Ulcerative colitis in China: retrospective analysis of 3,100 hospitalized patients. J Gastroenterol Hepatol. 2007;22:1450–5.
Khor B, Gardet A, Xavier RJ. Genetics and pathogenesis of inflammatory bowel disease. Nature. 2011;474:307–17.
Huys G, Vanhoutte T, Vandamme P. Application of sequence-dependent electrophoresis fingerprinting in exploring biodiversity and population dynamics of human intestinal microbiota: what can be revealed? Interdiscip Perspect Infect Dis. 2008;2008:597603.
Lefkovitz AL, Zarowitz BJ. It’s a microscopic world after all: prebiotics, probiotics, and synbiotics. Geriatr Nurs. 2013;34:323–5.
McNabb B, Isakow W. Probiotics for the prevention of nosocomial pneumonia: current evidence and opinions. Curr Opin Pulm Med. 2008;14:168–75.
Wehkamp J, Harder J, Wehkamp K, Wehkamp-von Meissner B, Schlee M, Enders C, et al. NF-kappaB- and AP-1-mediated induction of human beta defensin-2 in intestinal epithelial cells by Escherichia coli Nissle, a novel effect of a probiotic bacterium. Infect Immun. 1917;2004(72):5750–8.
Tannock GW, Munro K, Harmsen HJ, Welling GW, Smart J, Gopal PK. Analysis of the fecal microflora of human subjects consuming a probiotic product containing Lactobacillus rhamnosus DR20. Appl Environ Microbiol. 2000;66:2578–88.
Lammers KM, Helwig U, Swennen E, Rizzello F, Venturi A, Caramelli E, et al. Effect of probiotic strains on interleukin 8 production by HT29/19A cells. Am J Gastroenterol. 2002;97:1182–6.
Malin M, Suomalainen H, Saxelin M, Isolauri E. Promotion of IgA immune response in patients with Crohn’s disease by oral bacteriotherapy with Lactobacillus GG. Ann Nutr Metab. 1996;40:137–45.
Schultz M, Linde HJ, Lehn N, Zimmermann K, Grossmann J, Falk W, et al. Immunomodulatory consequences of oral administration of Lactobacillus rhamnosus strain GG in healthy volunteers. J Dairy Res. 2003;70:165–73.
Mack DR, Michail S, Wei S, McDougall L, Hollingsworth MA. Probiotics inhibit enteropathogenic E. coli adherence in vitro by inducing intestinal mucin gene expression. Am J Physiol. 1999;276:G941–50.
Madsen K, Cornish A, Soper P, McKaigney C, Jijon H, Yachimec C, et al. Probiotic bacteria enhance murine and human intestinal epithelial barrier function. Gastroenterology. 2001;121:580–91.
Henker J, Laass M, Blokhin BM, Bolbot YK, Maydannik VG, Elze M, et al. The probiotic Escherichia coli strain Nissle 1917 (EcN) stops acute diarrhoea in infants and toddlers. Eur J Pediatr. 2007;166:311–8.
Henker J, Laass MW, Blokhin BM, Maydannik VG, Bolbot YK, Elze M, et al. Probiotic Escherichia coli Nissle 1917 versus placebo for treating diarrhea of greater than 4 days duration in infants and toddlers. Pediatr Infect Dis J. 2008;27:494–9.
Fric P, Zavoral M. The effect of non-pathogenic Escherichia coli in symptomatic uncomplicated diverticular disease of the colon. Eur J Gastroenterol Hepatol. 2003;15:313–5.
Schultz M. Clinical use of E. coli Nissle, in inflammatory bowel disease. Inflamm Bowel Dis. 1917;2008(14):1012–8.
Kruis W, Fric P, Pokrotnieks J, Lukas M, Fixa B, Kascak M, et al. Maintaining remission of ulcerative colitis with the probiotic Escherichia coli Nissle 1917 is as effective as with standard mesalazine. Gut. 2004;53:1617–23.
Hoffmann JC, Zeitz M, Bischoff SC, Brambs HJ, Bruch HP, Buhr HJ, et al. Diagnosis and therapy of ulcerative colitis: results of an evidence based consensus conference by the German society of digestive and metabolic diseases and the competence network on inflammatory bowel disease. Z Gastroenterol. 2004;42:979–83.
Malchow HA. Crohn’s disease and Escherichia coli. A new approach in therapy to maintain remission of colonic Crohn’s disease? J Clin Gastroenterol. 1997;25:653–8.
Gronbach K, Eberle U, Muller M, Olschlager TA, Dobrindt U, Leithauser F, et al. Safety of probiotic Escherichia coli strain Nissle 1917 depends on intestinal microbiota and adaptive immunity of the host. Infect Immun. 2010;78:3036–46.
Behnsen J, Deriu E, Sassone-Corsi M, Raffatellu M. Probiotics: properties, examples, and specific applications. Cold Spring Harb Perspect Med. 2013;3:a010074.
Camuesco D, Comalada M, Rodriguez-Cabezas ME, Nieto A, Lorente MD, Concha A, et al. The intestinal anti-inflammatory effect of quercitrin is associated with an inhibition in iNOS expression. Br J Pharmacol. 2004;143:908–18.
Bell CJ, Gall DG, Wallace JL. Disruption of colonic electrolyte transport in experimental colitis. Am J Physiol. 1995;268:G622–30.
Arribas B, Rodriguez-Cabezas ME, Camuesco D, Comalada M, Bailon E, Utrilla P, et al. A probiotic strain of Escherichia coli, Nissle 1917, given orally exerts local and systemic anti-inflammatory effects in lipopolysaccharide-induced sepsis in mice. Br J Pharmacol. 2009;157:1024–33.
Altenhoefer A, Oswald S, Sonnenborn U, Enders C, Schulze J, Hacker J, et al. The probiotic Escherichia coli strain Nissle 1917 interferes with invasion of human intestinal epithelial cells by different enteroinvasive bacterial pathogens. FEMS Immunol Med Microbiol. 2004;40:223–9.
Sartor RB. Therapeutic manipulation of the enteric microflora in inflammatory bowel diseases: antibiotics, probiotics, and prebiotics. Gastroenterology. 2004;126:1620–33.
Scholmerich J. Inflammatory bowel disease: pandora’s box, present and future. Ann N Y Acad Sci. 2006;1072:365–78.
Acknowledgments
This study was supported by grants from the National Scientific Support Project (nos. 20100202, 02012BAI06B03 and BSW11J013), National Natural Science Foundation of China (Nos. 81322037 and 81370504) and National Excellent Doctoral Dissertation of PR China (No. 201182).
Conflict of interest
There are no conflicts of interest to disclose in this paper.
Author information
Authors and Affiliations
Corresponding author
Additional information
Responsible Editor: Liwu Li.
Sumei Sha, Bin Xu, and Xiangyun Kong contributed equally to this work.
Rights and permissions
About this article
Cite this article
Sha, S., Xu, B., Kong, X. et al. Preventive effects of Escherichia coli strain Nissle 1917 with different courses and different doses on intestinal inflammation in murine model of colitis. Inflamm. Res. 63, 873–883 (2014). https://doi.org/10.1007/s00011-014-0761-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-014-0761-1