Abstract
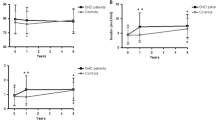
The aim of this study was to evaluate clinical and metabolic data in a cohort of Type 1 diabetes (T1DM) children before and after 2 yr of continuous sc insulin infusion (CSII). Forty seven T1DM patients were subdivided into two groups: Group A (20 pre-pubertal children, mean age 7.43±3.19 yr); Group B (27 pubertal adolescents, mean age 14.47±1.91 yr). No statistically significant differences in body mass index (BMI) occurred in either groups after starting CSII or during follow-up. The frequency of mild-hypoglycemias significantly declined during pump therapy only in Group A (p<0.05). Both pre-pubertal and pubertal patients required a significant reduction in their total insulin requirement after 12 and 24 months of CSII. The total percentage of daily insulin doses delivered as basal rates was similar in both groups and was negatively associated (β=−2.956, p=0.05) with glycosylated hemoglobin (HbA1c) values. No significant correlation was found between the percentage of the basal insulin rate and the number of daily boluses. Differences in timing of the highest insulin requirement were observed between the two groups. Group A had a higher insulin basal rate late in the evening (20:00–24:00 h), while Group B had a higher insulin requirement early in the morning (03:00–07:00 h). The HbA1c levels significantly improved in Group A after 6–12 and 24 months of CSII. In Group B a reduction of HbA1c values was observed only after 6 months of pump therapy (p=0.05). CSII is an effective therapy for all ages but different metabolic requirements should also be taken into account.
Similar content being viewed by others
References
The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 1993, 329: 977–86.
Effect of intensive diabetes treatment on the development and progression of long-term complications in adolescents with insulin-dependent diabetes mellitus: Diabetes Control and Complications Trial. Diabetes Control and Complications Trial Research Group. J Pediatr 1994, 125: 177–88.
Mortensen HB, Hougaard P. Comparison of metabolic control in a cross-sectional study of 2,873 children and adolescents with IDDM from 18 countries. The Hvidore Study Group on Childhood Diabetes. Diabetes Care 1997, 20: 714–20.
Danne T, Mortensen HB, Hougaard P, et al. Persistent differences among centers over 3 years in glycemic control and hypoglycemia in a study of 3.805 children and adolescents with type 1 diabetes from the Hvidøre Study Group. Diab Care 2001, 24: 1342–7.
Vanelli M, Cerutti F, Chiarelli F, Lorini R, Meschi F; MCDC-Italy Group. Nationwide cross-sectional survey of 3560 children and adolescents with diabetes in Italy. J Endocrinol Invest 2005, 28: 692–9.
Silverstein J, Klingensmith G, Copeland K, et al. Care of children and adolescents with type 1 diabetes: a statement of the American Diabetes Association. Diabetes Care 2005, 28: 186–212.
Fox LA, Buckloh LM, Smith SD, Wysocki T, Mauras N. A randomized controlled trial of insulin pump therapy in young children with type 1 diabetes. Diabetes Care 2005, 28: 1277–81.
Pickup J, Keen H. Continuous subcutaneous insulin infusion at 25 years: evidence base for the expanding use of insulin pump therapy in type 1 diabetes. Diabetes Care 2002, 25: 593–8.
Boland EA, Grey M, Oesterle A, Fredrickson L, Tamborlane WV. Continuous subcutaneous insulin infusion. A new way to lower risk of severe hypoglycemia, improve metabolic control, and enhance coping in adolescents with type 1 diabetes. Diabetes Care 1999, 22: 1779–84.
DiMeglio LA, Boyd SR, Pottorff TM, Cleveland JL, Fineberg N, Eugster EA. Preschoolers are not miniature adolescents: a comparison of insulin pump doses in two groups of children with type 1 diabetes mellitus. J Pediatr Endocrinol Metab 2004, 17: 865–70.
Conrad SC, McGrath MT, Gitelman SE. Transition from multiple daily injections to continuous subcutaneous insulin infusion in type 1 diabetes mellitus. J Pediatr 2002, 140: 235–40.
Di Meglio LA, Pottorff TM, Boyd SR, France L, Fineberg N, Eugster EA. A randomized, controlled study of insulin pump therapy in diabetic preschoolers. J Pediatr 2004, 145: 380–4.
Consensus guidelines 2000, International Society for Paediatric and Adolescent Diabetes. Medical Forum International, Zeist, Netherlands, 2000.
Gloyn AL, Pearson ER, Antcliff JF, et al. Activating mutations in the gene encoding the ATP-sensitive potassium-channel subunit Kir6.2 and permanent neonatal diabetes. N Engl J Med 2004, 350: 1838–49.
Sagen JV, Raeder H, Hathout E, et al. Permanent neonatal diabetes due to mutations in KCNJ11 encoding Kir6.2: patient characteristics and initial response to sulfonylurea therapy. Diabetes 2004, 53: 2713–8.
Njølstad PR, Søvik O, Cuesta-Muñoz A, et al. Neonatal Diabetes mellitus due to complete glucokinase deficiency. N Engl J Med 2001, 344: 1588–92.
American Diabetes Association and the American Dietetic association. The First Step in Diabetes Meal Planning. Alexandria, VA: ADA; 1995.
Dunger DB, Sperling MA, Acerini CL, et al. ESPE/LWPES consensus statement on diabetic ketoacidosis in children and adolescents. Arch Dis Child 2004, 89: 188–94.
Cacciari E, Milani S, Balsamo A, et al. Italian cross-sectional growth charts for height, weight and BMI (2 to 20 yr). J Endocrinol Invest 2006, 29: 581–93.
Willi SM, Planton J, Egede L, Schwarz S. Benefits of continuous subcutaneous insulin infusion in children with type 1 diabetes. J Pediatr 2003, 143: 796–801.
Plotnick LP, Clark LM, Brancati FL, Erlinger T. Safety and effectiveness of insulin pump therapy in children and adolescents with type 1 diabetes. Diabetes Care 2003, 26: 1142–6.
Weinzimer SA, Ahem JAH, Doyle EA, et al. Persistence of benefits of continuous subcutaneous insulin infusion in very young children with type 1 diabetes: a follow-up report. Pediatrics 2004, 114: 1601–5.
Wilson DM, Buckingham BA, Kunselman EL, Sullivan MM, Paguntalan HU, Gitelman SE. A two-center randomized controlled feasibility trial of insulin pump therapy in young children with diabetes. Diabetes Care 2005, 28: 15–9.
Mack-Fogg JE, Orlowski CC, Jospe N. Continuous subcutaneous insulin infusion in toddlers and children with type 1 diabetes mellitus is safe and effective. Pediatr Diabetes 2005, 6: 17–21.
Weintrob N, Benzaquen H, Galatzer A, et al. Comparison of continuous subcutaneous insulin infusion and multiple daily injection regimens in children with type 1 diabetes: a randomized open crossover trial. Pediatrics 2003, 112: 559–64.
Boland EA, Grey M, Oesterle A, Fredrickson L, Tamborlane WV. Continuous subcutaneous insulin infusion: a new way to lower risk of severe hypoglycemia, improve metabolic control, and enhance coping in adolescents with type 1 diabetes. Diabetes Care 1999, 22: 1779–84.
The DCCT Research Group. Weight gain associated with intensive therapy in Diabetes Control and Complications Trial. Diabetes Care 1998, 11: 567–73.
Burdick J, Chase P, Slover RH, et al. Missed insulin meal boluses and elevated haemoglobin A1c levels in children receiving insulin pump therapy. Paediatrics 2004, 113: e221–4.
Bolli GB, Perriello G, Fanelli CG, De Feo P. Nocturnal blood glucose control in type I diabetes mellitus. Diab Care 1993, 16: 71–89.
Cotterill AM, Daly F, Holly JM, et al. The ‘dawn phenomenon’ in adolescents with insulin dependent diabetes mellitus: possible contribution of insulin-like growth factor binding protein-1. Clin Endocrinol (Oxf) 1995, 43: 567–74.
Kaufman FR, Halvorson M, Kim C, Pitukcheewanont P. Use of insulin pump therapy at nighttime only for children 7–10 years of age with type 1 diabetes. Diabetes Care 2000, 23: 579–82.
Rose SR, Municchi G, Barnes KM, et al. Spontaneous growth hormone secretion increases during puberty in normal girls and boys. J Clin Endocrinol Metab 1991, 73: 428–35.
Mortensen HB, Robertson KJ, Aanstoot H-J, et al. Insulin management and metabolic control of type 1 diabetes mellitus in childhood and adolescents in 18 countries. Hvidore Study Group on Childhood Diabetes. Diabet Med 1998, 15: 752–9.
Kordonouri O, Hartmann R, Lauterborn R, Barnekow C, Hoeffe J, Deiss D. Age-specific advantages of continuous subcutaneous insulin infusion as compared with multiple daily injections in pediatric patients: one-year follow-up comparison by matched-pair analysis. Diabetes Care 2006, 29: 133–4.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rabbone, I., Bobbio, A., Berger, K. et al. Age-related differences in metabolic response to continuous subcutaneous insulin infusion in pre-pubertal and pubertal children with Type 1 diabetes mellitus. J Endocrinol Invest 30, 477–483 (2007). https://doi.org/10.1007/BF03346331
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03346331