Abstract
Purpose
Near infrared spectroscopy (NIRS) is a promising noninvasive method for continuous monitoring of cerebral oxygenation during cardiac surgery with cardiopulmonary bypass (CPB). This study was designed to study the agreement between tissue oxygen index (TOI) measured by spatially resolved spectroscopy (NIRO- 300) and jugular bulb oxygen saturation (SjO2) in patients undergoing warm coronary bypass surgery.
Methods
Seventeen patients undergoing warm coronary artery bypass surgery were studied. NIRS was continuously monitored and was averaged before CPB, five, 20, 40, 60 min on CPB, five minutes before end of CPB and ten minutes after CPB to coincide with SjO2 measurements. Bypass temperature was maintained at 34–37°C.
Results
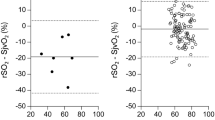
Bland and Altman analysis showed a bias (TOI-SjO2) of- 6.7%, and wide limits of agreement (from 16% to –28%) between the two methods. In addition, mean TOI was lower than mean SjO2 during and after CPB. We observed a statistically significant correlation between arterial carbon dioxide and SjO2 measurements (r2=0.33;P=0.0003), but the former did not correlate with TOI values (r2=0.001;P=0.7).
Conclusion
Our results demonstrate a lack of agreement between SjO2 and TOI for monitoring cerebral oxygenation during cardiac surgery. We conclude that the two methods are not interchangeable.
Résumé
Objectif
La spectroscope proche infrarouge (SPIR) est une méthode non effractive et prometteuse de monitorage continu de l’oxygénation cérébraie utilisée en chirurgie cardiaque sous circulation extracorporelle (CEC). L’étude actuelle voulait tester la concordance entre l’index d’oxygène tissuiaire (I0T) mesuré par spectroscope à résoiution spatiaie (NIRO- 300) et la saturation en oxygène du golfe de la jugulaire (SjO2) pendant une cardioplégie chaude.
Méthode
Dix sept patients subissant un pontage coronarien sous cardiopiégie chaude ont été étudiés. La SPIR a été surveillée continûment et ajustée avant la CEC, à cinq, 20, 40, 60 min pendant la CEC, cinq minutes avant la fin de la CEC et dix minutes après pour coïncider avec les mesures moyennes de SjO2. La température a été maintenue à 34– 37°C pendant la CEC.
Résultats
L’analyse de Bland et Altman a montré un biais (IOT- SjO2) de − 6,7 % et de larges limites de concordance (de 16% à − 28 %) entre les deux méthodes. De plus, l’IOT moyen était plus bas que la SjO2 moyenne pendant et après la CEC. Il existait une corrélation statistiquement significative entre le gaz carbonique artériel et les mesures de SjO2(r2 = 0,33; P = 0,0003), mais non entre le CO2 et les valeurs de l’IOT (r2 = 0,001; P = 0,7).
Conclusion
Nos résultats démontrent un manque de concordance entre la SjO2 et l’IOT lors du monitorage de l’oxygénation cérébrale pendant une intervention cardiaque. Les deux méthodes ne sont donc pas interchangeables.
Article PDF
Similar content being viewed by others
References
Nakajima F, Ohsumi H, Kuro M. Accuracy of continuous jugular bulb venous oximetry during cardiopulmonary bypass. Anesth Analg 1993; 77: 1111–5.
Croughwell ND, Newman MF, Blumenthal JA, et al. Jugular bulb saturation and cognitive dysfunction after cardiopulmonary bypass. Ann Thorac Surg 1994; 58: 1702–8.
Croughwell ND, Frasco P, Blumenthal JA, Leone BJ, White WD, Reves JG. Warming during cardiopulmonary bypass is associated with jugular bulb desaturation. Ann Thorac Surg 1992; 53: 827–32.
Cook DJ, Oliver WC Jr, Orszulak TA, Daly RC. A prospective, randomized comparison of cerebral venous oxygen saturation during normothermic and hypothermie cardiopulmonary bypass. J Thorac Cardiovasc Surg 1994; 107: 1020–9.
Jöbsis FF. Noninvasive, infrared monitoring of cerebral and myocardial oxygen sufficiency and circulatory parameters. Science 1977; 198: 1264–7.
Nollert G, Shin’oka T, Jonas RA. Near-infrared spectrophotometry of the brain in cardiovascular surgery. Thorac Cardiovasc Surg 1998; 46: 167–75.
Kurth CD, Steven JM, Nicolson SC, Jacobs ML. Cerebral oxygenation during cardiopulmonary bypass in children. J Thorac Cardiovasc Surg 1997; 113: 71–9.
Nollert G, Möhnle P, Tassani-Prell P, Reichart B. Determinants of cerebral oxygenation during cardiac surgery. Circulation 1995; 92(suppl II): II-327–II-33.
Rigg CD, Clutton-Brock TH. Near-infrared spectroscopy changes during hypothermic circulatory arrest with retrograde cerebral perfusion. Anaesthesia 1997; 52: 356–63.
Fallon P, Roberts I, Kirkham FJ, et al. Cerebral hemodynamics during cardiopulmonary bypass in children using near-infrared spectroscopy. Ann Thorac Surg 1993; 56: 1473–7.
Williams IM, Picton AJ, Hardy SC, Mortimer AJ, McCollum CN. Cerebral hypoxia detected by near infrared spectroscopy. Anaesthesia 1994; 49: 762–6.
Kirkpatrick PJ, Smielewski P, Lam JMK, Al-Rawi P. Use of near infrared spectroscopy for the clinical monitoring of adult brain. J Biomed Opt 1996; 1: 363–72.
Owen-Reece H, Smith M, Elwell CE, Goldstone JC. Near infrared spectroscopy. Br J Anaesth 1999; 82: 418–26.
Matta BF, Lam AM. The rate of blood withdrawal affects the accuracy of jugular venous bulb. Oxygen saturation measurements. Anesthesiology 1997; 4: 806–8.
Bland JM, Altman DG. Statistical methods for assessing agreement of two methods of clinical measurement. Lancet 1986; 1: 307–10.
Daubeney PEF, Pilkington SN, Janke E, Charlton GA, Smith DC, Webber SA. Cerebral oxygenation measured by near infrared spectroscopy: comparison with jugular bulb oximetry. Ann Thorac Surg 1996; 61: 930–4.
Brown R, Wright G, Royston D. A Comparison of two systems for assessing cerebral venous oxyhaemoglobin saturation during cardiopulmonary bypass in humans. Anaesthesia 1993; 48: 697–700.
Lewis SB, Myburgh JA, Thornton EL, Reilly PL. Cerebral oxygenation monitoring by near-infrared spectroscopy is not clinically useful in patients with severe closed-head injury: a comparison with jugular venous bulb oximetry. Crit Care Med 1996; 24: 1334–8.
Minassian AT, Poirier N, Pierrot M, et al. Correlation between cerebral oxygen saturation measured by nearinfrared spectroscopy and jugular oxygen saturation in patients with severe closed head injury. Anesthesiology 1999; 91: 985–90.
Buunk G, van der Hoeven JG, Meinders AE. A comparison of near-infrared spectroscopy and jugular bulb oximetry in comatose patients resuscitated from a cardiac arrest. Anaesthesia 1998; 53: 13–9.
Sapire KJ, Gopinath SP, Farhat G, et al. Cerebral oxygenation during warming after cardiopulmonary bypass. Crit Care Med 1997; 25: 1655–62.
Germon TJ, Young AER, Manara AR, Nelson RJ. Extracerebral absorption of near infrared light influences the detection of increased cerebral oxygenation monitored by near infrared spectroscopy. J Neurol Neurosurg Psychiatry 1995; 58: 477–9.
Okada E, Firbank M, Delpy DT. The effect of overlying tissue on the spatial sensitivity profile of nearinfrared spectroscopy. Phys Med Biol 1995; 40: 2093–108.
Owen-Reece H, Elwell CE, Harkness W, et al. Use of near infrared spectroscopy to estimate cerebral blood flow in conscious and anaesthetized adult subjects. Br J Anaesth 1996; 76: 43–8.
Young AER, Germon TJ, Barnett NJ, Manara AR, Nelson RJ. Behaviour of near-infrared light in the adult human head: implications for clinical near-infrared spectroscopy. Br J Anaesth 2000; 84: 38–42.
Matta B. Advances in monitoring cerebral oxygenation. Curr Opin Anaesth 1996; 9: 365–70.
Germon T, Kane NM, Manara AR, Nelson RJ. Near infrared spectroscopy in adults: effects of extracranial ischemia and intracranial hypoxia on estimation of cerebral oxygenation. Br J Anaesth 1994; 73: 503–6.
Tateishi A, Maekawa T, Soejima Y, et al. Qualitative comparison of carbon dioxide-induced change in cerebral near-infrared spectroscopy versus jugular venous oxygen saturation in adults with acute brain disease. Crit Care Med 1995; 23: 1734–8.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ali, M.S., Harmer, M., Vaughan, R.S. et al. Spatially resolved spectroscopy (NIRO-300) does not agree with jugular bulb oxygen saturation in patients undergoing warm bypass surgery. Can J Anesth 48, 497–501 (2001). https://doi.org/10.1007/BF03028317
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03028317