Abstract
Purpose
Administration of remifentanii followed by propofol provides adequate conditions for tracheal intubation without muscle relaxants. Other hypnotic drugs have not been thoroughly investigated in this regard. Intubating conditions with remifentanil followed by propofol, thiopentone or etomidate are compared in this study.
Methods
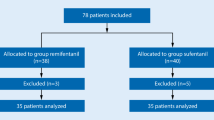
In a randomized, double-blind study 45 healthy males were assigned to one of three groups (n = 15). After iv atropine, remifentanil 3 μg· kg−1 were injected over 90 sec followed by propofol 2 mg· kg−1 (Group I), thiopentone 6 mg· kg−1 (Group II) or etomidate 0.3 mg· kg−1 (Group III), Ninety seconds after the administration of the hypnotic agent, laryngoscopy and intubation were attempted, Intubating conditions were assessed as excellent, good or poor on the basis of ease of ventilation, jaw relaxation, position of the vocal cords, and patient response to intubation and slow inflation of the endotracheal tube cuff.
Results
One patient in Group I, three patients in Group II and five patients in Group III could not be intubated on the first attempt. Clinically acceptable intubating conditions were observed in 93.3%, 66.7%, 40.0% of patients in Groups I, II and III, respectively. Overall conditions at intubation were significantly (P < 0,05) better, and the frequency of excellent conditions was significantly (P < 0.05) higher in the propofol group compared with the thiopentone and etomidate groups. No patient was treated for hypotension or bradycardia.
Conclusion
Propofol 2 mg· kg−1 was superior to thiopentone 6 mg· kg−1 and etomidate 0.3 mg· kg−1 for tracheal intubation when combined with remifentanil 3 μg· kg−1 and no muscle relaxant.
Résumé
Objectif
L’administration de rémifentanil suivie de propofol permet des conditions satisfaisantes d’intubation endotrachéale sans myorelaxants. D’autres hypnotiques n’ont pas encore été testés dans ces circonstances. Nous avons donc voulu comparé les conditions d’intubation avec le rémifentanil suivi du propofol, du thiopental ou de l’étomidate.
Méthode
L’étude randomisée et à double insu a été réalisée auprès de 45 hommes en bonne santé, répartis en trois groupes (n = 15). Après l’administration iv d’atropine, l’injection de 3 μg· kg−1 de rémifentanil, pendant 90 sec, a été suivie de 2 mg· kg−1 de propofol (Groupe I), de 6 mg· kg−1 de thiopentai (Groupe II) ou de 0,3 mg· kg−1 d’étomidate (Groupe III). Quatre-vingt-dix secondes après l’administration de l’agent hypnotique, la laryngoscope et l’intubation ont été tentées. Les conditions d’intubation ont été évaluées comme excellentes, bonnes ou pauvres d’après la facilité de ventilation, du relâchement de la mâchoire, la position des cordes vocales et la réponse du patient à l’intubation et au gonflement lent du ballonnet du tube endotrachéal.
Résultats
Un patient du Groupe I, trois du Groupe II et cinq du Groupe III n’ont pu être intubés au premier essai. Des conditions d’intubation acceptables ont été observées chez 93,3 %, 66,7 % et 40,0 % des patients des Groupes I, II et III. Dans l’ensembie, les conditions d’intubation ont été signifiativement (P < 0,05) meilleures, et la fréquence de conditions excellentes a été signifeativement (P < 0,05) plus élevée, avec le propofol, comparé au thiopentai et à l’étomidate. Aucun patient n’a dû recevoir de traitement pour hypotension ou bradycardie.
Conclusion
Les conditions d’intubation endotrachéale ont été meilleures avec l’usage de 2 mg· kg−1 de propofoi, comparés à 6 mg· kg−1 de thiopental et à 0,3 mg· kg−1 d’étomidate, combinés à 3 μg· kg−1de remifentanil et sans myorelaxants.
Article PDF
Similar content being viewed by others
References
Scheller MS, Zornow MH, Saidman LJ. Tracheal intubation without the use of muscle relaxants: a technique using propofol and varying doses of alfentanil. Anesth Analg 1992; 75: 788–93.
Davidson JA, Gillespie JA. Tracheal intubation after induction of anaesthesia with propofol, alfentanil and i.v. lidocaine. Br J Anaesth 1993; 70: 163–6.
Stevens JB, Vescovo MV, Harris KC, Walker SC, Hickey R. Tracheal intubation using alfentanil and no muscle relaxant: is the choice of hypnotic important? Anesth Analg 1997; 84: 1222–6.
Grant S, Noble S, Woods A, Murdoch J, Davidson A. Assessment of intubating conditions in adults after induction with propofol and varying doses of remifentanil. Br J Anaesth 1998; 81: 540–3.
Stevens JB, Wheatley L. Tracheal intubation in ambulatory surgery patients: using remifentanil and propofol without muscle relaxants. Anesth Analg 1998; 86: 45–9.
Klemola UM, Mennander S, Saarnivaara L. Tracheal intubation without the use of muscle relaxants: remifentanil or alfentanil in combination with propofol. Acta Anaesthesiol Scand 2000; 44: 465–9.
Heier T, Steen PA. Awareness in anaesthesia: incidence, consequences and prevention. Acta Anaesthesiol Scand 1996; 40: 1073–86.
Ghoneim MM, Block RI. Learning and consciousness during general anesthesia. Anesthesiology 1992; 76: 279–305.
Glass PSA, Hardman D, Kamiyama Y, et al. Preliminary pharmacokinetics and pharmacodynamics of an ultra-short-acting opioid: remifentanil (G187084B). Anesth Analg 1993; 77: 1031–40.
Egan TD, Minto CF, Hermann DJ, Barr J Muir KT, Shafer SL. Remifentanil versus alfentanil: comparative phamiacokinetics and pharmacodynamics in healthy adult male volunteers. Anesthesiology 1996; 84: 821–33.
Reves JG, Glass PSA, Lubarsky DA. Nonbarbiturate intravenous anesthetics. In: Miller RD (Ed.). Anesthesia, fifth ed. Pennsylvania: Churchill Livingstone Inc., 2000: 228–72.
Mallampati SR, Gatt SP, Gugino LD, et al. A clinical sign to predict difficult tracheal intubation: a prospective study. Can Anaesth Soc J 1985; 32: 429–34.
Kazama T, Ikeda K, Morita, K. Reduction by fentanyl of the CP50 values of propofol and hemodynamic responses to various noxious stimuli. Anesthesiology 1997; 87: 213–27.
Gill RS, Scott RPF. Etomidate shortens the onset time of neuromuscular block. Br J Anaesth 1992; 69: 444–6.
Kuizenga K, Wierda JMK, Kalkman CJ. Biphasic EEG changes in relation to loss of consciousness during induction with thiopental, propofol, etomidate, midazolam or sevoflurane. Br J Anaesth 2001; 86: 354–60.
Price ML, Millar B, Grounds M, Cashman J. Changes in cardiac index and estimated sysemic vascular resisance during induction of anaesthesia with thiopentone, methohexitone, propofol and etomidate. Br J Anaesth 1992; 69: 172–6.
Avram MJ, Sanghvi R, Henthorn TK, Krejcie TC. Determinants of thiopental induction dose requirements. Anesth Analg 1993; 76: 10–7.
McKeating K, Bali IM, Dundee JW. The effects of thiopentone and propofol on upper airway integrity. Anaesthesia 1988; 43: 638–40.
Barker P, Langten JA, Wilson IG, Smith G. Movements of the vocal cords on induction of anaesthesia with thiopentone or propofol. Br J Anaesth 1992; 69: 23–5.
Eames WO, Rooke GA, Wu RSC, Bishop MJ. Comparison of the effects of etomidate, propofol, and thiopental on respiratory resistance after tracheal intubation. Anesthesiology 1996; 84: 1307–11.
Hovarka J, Honkavaara P, Korttila K. Tracheal intubation after induction of anaesthesia with thiopentone or propofol without muscle relaxants. Acta Anaesthesiol Scand 1991; 35: 326–8.
Morgan GA, Mikhail MS. Nonvolatile anesthetic agents. In: Morgan GA, Mikhail MS (Eds.). Clinical Anesthesiology, second ed., Stomford: Appleton & Lange; 1996: 128–48.
Thompson JP, Hall AP, Russell J, Cagney B, Rowbotham DJ. Effect of remifentanil on the haemodynamic response to orotracheal intubation. Br J Anaesth 1998; 80: 467–9.
Woods A, Grant S, Davidson A. Duration of apnoea with two different intubating doses of remifentanil. Eur J Anaesthesiol 1999; 16: 634–7.
Fragen RJ, Avram MJ. Barbiturates. In: Miller RD (Ed.). Anesthesia, fifth ed. Pennsylvania: Churchill Livingstone Inc.; 2000: 209–27.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Erhan, E., Ugur, G., Gunusen, I. et al. Propofol — not thiopental or etomidate — with remifentanil provides adequate intubating conditions in the absence of neuromuscular blockade. Can J Anaesth 50, 108–115 (2003). https://doi.org/10.1007/BF03017840
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03017840