Abstract
Purpose: Activated protein C (APC) is the first anti-inflammatory drug to be approved for the treatment of severe sepsis. However, the underlying mechanisms are not completely elucidated. Therefore, the aim of our study was to evaluate the effects of APC on the microcirculation (mesenteric leukocyte-endothelial interaction, plasma extravasation) using intravital microscopy (IVM) and on cytokine release during experimental endotoxemia in rats.
Methods: We divided forty, male, Lewis rats into four groups (n=10 per group): Controls, LPS (15 mg·kg−1 lipopolysaccharideiv), APC (2 mg·kg−1 APCiv), and LPS+APC. We determined mesenteric leukocyte-endothelial interactions and plasma extravasation at zero, one and two hours following administration of LPS and APC by IVM. Plasma levels of tumour necrosis factor-α, IL-1β, interleukin (IL)-6, and IL-10 were measured at zero and at two hours.
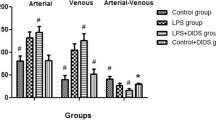
Results: Leukocyte adherence (−74%) and plasma extravasation (−28%) during endotoxemia were diminished significantly following APC treatment, compared to untreated LPS animals (P=0.0001 andP=0.0004, respectively). Interleukin-1β release was also significantly reduced by APC treatment (2567.4 ± 320.9 pg·mL−1 in the LPS groupvs 1626.1 ± 427.2 pg·mL−1 in the LPS+APC group;P=0.001).
Conclusion: These rodent experiments showed that APC treatment significantly attenuated deterioration of the mesenteric microcirculation and systemic IL-1β release caused by endotoxin challenge. Because of the crucial role of the microcirculation in ongoing sepsis pathogenesis and multiple organ dysfunction syndrome, these effects may be of clinical importance.
Résumé
Objectif: La protéine C activée (PCA) est le premier médicament anti-inflammatoire à être approuvé pour le traitement des septicémies sévères. Cependant, les mécanismes sous-jacents de cette protéine ne sont pas encore complètement compris. C’est pourquoi notre étude avait pour but d’évaluer les effets de la PCA sur la microcirculation (interaction mésentérique leucocytaire-endothéliale, extravasation plasmatique) en utilisant la microscopie intravitale (IVM) ainsi que ses effets sur la libération de cytokines pendant une endotoxémie expérimentale chez les rats.
Méthode: Nous avons randomisé quarante rats Lewis mâles en quatre groupes (n=10 par groupe) : témoin, LPS (15 mg·kg−1 lipopolysaccharide iv), PCA (2 mg·kg−1 PCA iv), et LPS+PCA. Nous avons évalué les interactions mésentériques leucocytaires-endothéliales et l’extravasation plasmatique à zéro, une et deux heures après l’administration de LPS et de PCA par MIV. Les niveaux plasmatiques de facteur onconécrosant-α, d’IL-1β, d’interleukine (IL)-6, et d’IL-10 ont été mesurés à zéro et deux heures.
Résultats: L’adhérence leucocytaire (−74 %) et l’extravasation plasmatique (−28 %) pendant l’endotoxémie ont été significativement réduites après un traitement avec PCA, par rapport aux animaux LPS non traités (P=0,0001 et P=0,0004, respectivement). La libération d’interleukine-1β était également réduite de façon significative par le traitement avec PCA (2567,4 ± 320,9 pg·mL−1 dans le groupe LPS vs 1626,1 ± 427,2 pg·mL−1 dans le groupe LPS+PCA ; P=0,001).
Conclusion: Ces expériences sur les rongeurs ont montré que le traitement à base de PCA atténuait de manière significative la détérioration de la microcirculation mésentérique ainsi que la libération systémique d’IL-1β provoquées par le choc endotoxique. En raison du rôle primordial de la microcirculation dans la pathogenèse continue de la septicémie et dans le syndrome de défaillance multisystémique, ces effets pourraient avoir une importance clinique.
Article PDF
Similar content being viewed by others
References
Martin GS, Mannino DM, Eaton S, Moss M. The epidemiology of sepsis in the United States from 1979 through 2000. N Engl J Med 2003; 348: 1546–54.
Angus DC, Linde-Zwirble WT, Lidicker J, Clermont G, Carcillo J, Pinsky MR. Epidemiology of severe sepsis in the United States: analysis of incidence, outcome, and associated costs of care. Crit Care Med 2001; 29: 1303–10.
Bernard GR, Vincent JL, Laterre PF, et al. Efficacy and safety of recombinant human activated protein C for severe sepsis. N Engl J Med 2001; 344: 699–709.
Walker FJ, Sexton PW, Esmon CT. The inhibition of blood coagulation by activated protein C through the selective inactivation of activated factor V. Biochim Biophys Acta 1979; 571: 333–42.
Yan SB, Dhainaut JF. Activated protein C versus protein C in severe sepsis. Crit Care Med 2001; 29(7 Suppl): S69–74.
Lehmann C, Meissner K, Knock A, et al. Activated protein C improves intestinal microcirculation in experimental endotoxaemia in the rat. Crit Care 2006; 10: R157.
Clark JA, Coopersmith CM. Intestinal crosstalk: a new paradigm for understanding the gut as the “motor” of critical illness. Shock 2007; 28: 384–93.
Birnbaum J, Hein OV, Luhrs C, et al. Effects of coagulation factor XIII on intestinal functional capillary density, leukocyte adherence and mesenteric plasma extravasation in experimental endotoxemia. Crit Care 2006; 10: R29.
Iba T, Kidokoro A, Fukunaga M, Nagakari K, Shirahama A, Ida Y. Activated protein C improves the visceral microcirculation by attenuating the leukocyte-endothelial interaction in a rat lipopolysaccharide model. Crit Care Med 2005; 33: 368–72.
Pavlovic D, Frieling H, Lauer KS, et al. Thermostatic tissue platform for intravital microscopy: ‘the hanging drop’ model. J Microsc 2006; 224: 203–10.
Lehmann C, Konig JP, Dettmann J, Birnbaum J, Kox WJ. Effects of iloprost, a stable prostacyclin analog, on intestinal leukocyte adherence and microvascular blood flow in rat experimental endotoxemia. Crit Care Med 2001; 29: 1412–6.
Lehmann C, Birnbaum J, Luhrs C, et al. Effects of C1 esterase inhibitor administration on intestinal functional capillary density, leukocyte adherence and mesenteric plasma extravasation during experimental endotoxemia. Intensive Care Med 2004; 30: 309–14.
Grinnell BW, Hermann RB, Yan SB. Human protein C inhibits selectin-mediated cell adhesion: role of unique fucosylated oligosaccharide. Glycobiology 1994; 4: 221–5.
Murakami K, Okajima K, Uchiba M, et al. Activated protein C attenuates endotoxin-induced pulmonary vascular injury by inhibiting activated leukocytes in rats. Blood 1996; 87: 642–7.
Hoffmann JN, Vollmar B, Laschke MW, et al. Microhemodynamic and cellular mechanisms of activated protein C action during endotoxemia. Crit Care Med 2004; 32: 1011–7.
Yadav R, Larbi KY, Young RE, Nourshargh S. Migration of leukocytes through the vessel wall and beyond. Thromb Haemost 2003; 90: 598–606.
Liu L, Kubes P. Molecular mechanisms of leukocyte recruitment: organ-specific mechanisms of action. Thromb Haemost 2003; 89: 213–20.
Weber C. Novel mechanistic concepts for the control of leukocyte transmigration: specialization of integrins, chemokines, and junctional molecules. J Mol Med 2003; 81: 4–19.
Piper RD, Pitt-Hyde ML, Anderson LA, Sibbald WJ, Potter RF. Leukocyte activation and flow behavior in rat skeletal muscle in sepsis. Am J Respir Crit Care Med 1998; 157: 129–34.
Warren BL, Eid A, Singer P, et al. Caring for the critically ill patient. High-dose antithrombin III in severe sepsis: a randomized controlled trial. JAMA 2001; 286: 1869–78.
Macias WL, Yan SB, Williams MD, et al. New insights into the protein C pathway: potential implications for the biological activities of drotrecogin alfa (activated). Crit Care 2005; (9 Suppl 4): S38–45.
Mizutani A, Okajima K, Uchiba M, Noguchi T. Activated protein C reduces ischemia/reperfusion-induced renal injury in rats by inhibiting leukocyte activation. Blood 2000; 95: 3781–7.
Choi G, Hofstra JJ, Roelofs JJ, et al. Recombinant human activated protein C inhibits local and systemic activation of coagulation without influencing inflammation during Pseudomonas aeruginosa pneumonia in rats. Crit Care Med 2007; 35: 1362–8.
Jesch NK, Dorger M, Messmer K, Krombach F. Formation of nitric oxide by rat and hamster alveolar macrophages: an interstrain and interspecies comparison. Toxicol Lett 1998; 96–97: 47–51.
Deschepper CF, Olson JL, Otis M, Gallo-Payet N. Characterization of blood pressure and morphological traits in cardiovascular-related organs in 13 different inbred mouse strains. J Appl Physiol 2004; 97: 369–76.
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclosure: Activated protein C was provided by Lilly Deutschland GmbH.
Note: The first and the second author contributed equally to the manuscript.
Rights and permissions
About this article
Cite this article
Lehmann, C., Scheibe, R., Schade, M. et al. Effects of activated protein C on the mesenteric microcirculation and cytokine release during experimental endotoxemia. Can J Anesth 55, 155–162 (2008). https://doi.org/10.1007/BF03016089
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03016089