Abstract
The purpose of this study is to evaluate whether follicle-stimulating hormone treatment improves sperm DNA parameters and pregnancy outcome in infertile male candidates to in-vitro fertilization.
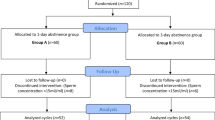
Observational study in 166 infertile male partners of couples undergoing in-vitro fertilization. Eighty-four patients were receiving follicle-stimulating hormone treatment (cases) and 82 refused treatment (controls). Semen parameters, sexual hormones, and sperm nucleus (fluorescence in-situ hybridization, acridine orange, TUNEL, and γH2AX) were evaluated at baseline (T0) and after 3 months (T1), when all subjects underwent assisted reproduction techniques. Statistical analysis was performed by analysis of variance.
Compared to baseline, cases showed significant improvements in seminal parameters and DNA fragmentation indexes after follicle-stimulating hormone therapy (all P < 0.05), whereas no changes were observed in controls. Within cases, follicle-stimulating hormone treatment allowed to perform intrauterine insemination in 35 patients with a pregnancy rate of 23.2 %. Intracytoplasmic sperm injection was performed in all controls and in 49 patients from cases, with pregnancy rates of 23.2 and 40.8 %, respectively (P < 0.05). After 3 months (T0 vs. T1) of follicle-stimulating hormone therapy, cases with positive outcome had reduced DNA fragmentation index and lower double strand breaks (P < 0.05 and P < 0.001 vs. negative outcome, respectively).
In this observational study, we showed that follicle-stimulating hormone treatment improves sperm DNA fragmentation, which in turn leads to increased pregnancy rates in infertile males undergoing in-vitro fertilization. In particular, double strand breaks (measured with γH2AX test) emerged as the most sensible parameter to follicle-stimulating hormone treatment in predicting reproductive outcome.


Similar content being viewed by others
References
D.M. de Kretser, Male infertility. Lancet 349, 787–790 (1997)
E.S. Jungheim, G.L. Ryan, E.D. Levens, A.F. Cunningham, G.A. Macones, K.R. Carson, A.N. Beltsos, R.R. Odem, Embryo transfer practices in the United States: a survey of clinics registered with the Society for Assisted Reproductive Technology. Fertil. Steril. 94, 1432–1436 (2010)
B. Baccetti, E. Strehler, S. Capitani, G. Collodel, M. De Santo, E. Moretti, P. Piomboni, R. Wiedeman, K. Sterzik, The effect of follicle stimulating hormone therapy on human sperm structure (Notulae seminologicae 11). Hum. Reprod. 12, 1955–1968 (1997)
H. Tournaye, Male factor infertility and ART. Asian J. Androl. 14, 103–108 (2012)
A.M. Attia, A.M. Abou-Setta, H.G. Al-Inany, Gonadotrophins for idiopathic male factor subfertility. Cochrane Database Syst. Rev. 8, CD005071 (2013)
A. Kamischke, H.M. Behre, M. Bergmann, M. Simoni, T. Schäfer, E. Nieschlag, Recombinant human follicle stimulating hormone for treatment of male idiopathic infertility: a randomized, double-blind, placebo-controlled, clinical trial. Hum. Reprod. 13, 596–603 (1998)
R. Matorras, C. Perez, B. Corcostegui, J.I. Pijoan, O. Ramon, P. Delgado, F.J. Rodríguez-Escudero, Treatment of the male with follicle-stimulating hormone in intrauterine insemination with husband’s spermatozoa: a randomized study. Hum. Reprod. 12, 24–28 (1997)
A.M. Attia, H.G. Al-Inany, C. Farquhar, M. Proctor, Gonadotrophins for idiopathic male factor subfertility. Cochrane Database Syst. Rev. 17, CD005071 (2007)
A.A. Acosta, S. Oehninger, H. Ertunc, C. Philput, Possible role of pure human follicle-stimulating hormone in the treatment of severe male infertility by assisted reproduction: preliminary report. Fertil. Steril. 55, 1150–1156 (1991)
B. Bartoov, F. Eltes, E. Lunenfeld, Sperm quality of subfertile males before and after treatment with human follicle-stimulating hormone. Fertil. Steril. 61, 727–734 (1994)
H.J. Glander, J. Kratzsch, Effects of pure human follicle-stimulating hormone (pFSH) on sperm quality correlate with the hypophyseal response to gonadotropin-releasing hormone (GnRH). Andrologia 29, 23–28 (1997)
G. Merino, S. Carranza-Lira, J.C. Martinez-Chequer, Sperm characteristics and hormonal profile before and after treatment with follicle-stimulating hormone in infertile patients. Arch. Androl. 37, 197–200 (1996)
E. Strehler, K. Sterzik, M. De Santo, M. Abt, R. Wiedemann, U. Bellati, G. Collodel, P. Piomboni, B. Baccetti, The effect of follicle-stimulating hormone therapy on sperm quality: an ultrastructural mathematical evaluation. J. Androl. 18, 439–447 (1997)
C. Foresta, A. Bettella, A. Ferlin, A. Garolla, M. Rossato, Evidence for a stimulatory role of follicle-stimulating hormone on the spermatogonial population in adult males. Fertil. Steril. 69, 636–642 (1998)
C. Foresta, A. Bettella, A. Garolla, G. Ambrosini, A. Ferlin, Treatment of male idiopathic infertility with recombinant human follicle-stimulating hormone: a prospective, controlled, randomized clinical study. Fertil. Steril. 84, 654–661 (2005)
N. Colacurci, M.G. Monti, F. Fornaro, G. Izzo, P. Izzo, C. Trotta, D. Mele, P. De Franciscis, Recombinant human FSH reduces sperm DNA fragmentation in men with idiopathic oligoasthenoteratozoospermia. J. Androl. 33, 588–593 (2012)
G. Ruvolo, M.C. Roccheri, A.M. Brucculeri, S. Longobardi, E. Cittadini, L. Bosco, Lower sperm DNA fragmentation after r-FSH administration in functional hypogonadotropic hypogonadism. J. Assist. Reprod. Genet. 30, 497–503 (2013)
A.A. Acosta, E. Khalifa, S. Oehninger, Pure human follicle stimulating hormone has a role in the treatment of severe male infertility by assisted reproduction: Norfolk’s total experience. Hum. Reprod. 7, 1067–1072 (1992)
J. Ashkenazi, I. Bar-Hava, J. Farhi, T. Levy, D. Feldberg, R. Orvieto, Z. Ben-Rafael, The role of purified follicle stimulating hormone therapy in the male partner before intracytoplasmic sperm injection. Fertil. Steril. 72, 670–673 (1999)
A. Garolla, R. Selice, B. Engl, A. Bertoldo, M. Menegazzo, L. Finos, A. Lenzi, C. Foresta, Spermatid count as a predictor of response to FSH therapy. Reprod. Biomed. Online 29, 102–112 (2014)
World Health Organization. WHO Laboratory Manual for the Examination and Processing of Human Semen. 5th edn. (WHO Press, Geneva, Switzerland, 2010)
W.A. Robbins, J.E. Baulch, D. Moore 2nd, H.U. Weier, D. Blakey, A.J. Wyrobek, Three-probe fluorescence in situ hybridization to assess chromosome X, Y, and 8 aneuploidy in sperm of 14 men from two healthy groups: evidence or a paternal age effect on sperm aneuploidy. Reprod. Fertil. Dev. 7, 799–809 (1995)
W. Eggert-Kruse, G. Rohr, H. Kerbel, B. Schwalbach, T. Demirakca, K. Klinga, W. Tilgen, B. Runnebaum, The Acridine Orange test: a clinically relevant screening method for sperm quality during infertility investigation. Hum. Reprod. 11, 784–789 (1996)
R.K. Sharma, E. Sabanegh, R. Mahfouz, S. Gupta, A. Thiyagarajan, A. Agarwal, TUNEL as a test for sperm DNA damage in the evaluation of male infertility. Urology 76, 1380–1386 (2010)
Z. Li, J. Yang, H. Huang, Oxidative stress induces H2AX phosphorylation in human spermatozoa. FEBS Lett. 580, 6161–6168 (2006)
A. Giwercman, L. Lindstedt, M. Larsson, M. Bungum, M. Spano, R.J. Levine, L. Rylander, Sperm chromatin structure assay as an independent predictor of fertility in vivo: a case-control study. Int. J. Androl. 33, e221–227 (2010)
M. Spanò, J.P. Bonde, H.I. Hjøllund, H.A. Kolstad, E. Cordelli, G. Leter, Sperm chromatin damage impairs human fertility. The Danish First Pregnancy Planner Study Team. Fertil. Steril. 73, 43–50 (2000)
E.H. Duran, M. Morshedi, S. Taylor, S. Oehninger, Sperm DNA quality predicts intrauterine insemination outcome: a prospective cohort study. Hum. Reprod. 17, 3122–3128 (2002)
S. Malić Vončina, B. Golob, A. Ihan, A.N. Kopitar, M. Kolbezen, B. Zorn, Sperm DNA fragmentation and mitochondrial membrane potential combined are better for predicting natural conception than standard sperm parameters. Fertil. Steril. 105, 637–644 (2016)
L. Robinson, I.D. Gallos, S.J. Conner, M. Rajkhowa, D. Miller, S. Lewis, J. Kirkman-Brown, A. Coomarasamy, The effect of sperm DNA fragmentation on miscarriage rates: a systematic review and meta-analysis. Hum. Reprod. 27, 2908–2917 (2012)
I. Zidi-Jrah, A. Hajlaoui, S. Mougou-Zerelli, M. Kammoun, I. Meniaoui, A. Sallem, I. Zidi-Jrah, S. Brahem, M. Fekih, M. Bibi, A. Saad, S. Ibala-Romdhane, Relationship between sperm aneuploidy, sperm DNA integrity, chromatin packaging, traditional semen parameters, and recurrent pregnancy loss. Fertil. Steril. 105, 58–64 (2016)
D. Santi, A.R. Granata, M. Simoni, FSH treatment of male idiopathic infertility improves pregnancy rate: a meta-analysis. Endocr. Connect. 4, R46–58 (2015)
A. Zini, Are sperm chromatin and DNA defects relevant in the clinic?. Syst. Biol. Reprod. Med. 57, 78–85 (2011)
Practice Committee of the American Society for Reproductive Medicine, The clinical utility of sperm DNA integrity testing: a guideline. Fertil. Steril. 99, 673–677 (2013)
H.M. Fisher, R.J. Aitken, Comparative analysis of the ability of precursor germ cells and epididymal spermatozoa to generate reactive oxygen metabolites. J. Exp. Zool. 277, 390–400 (1997)
L. Marcon, G. Boissonneault, Transient DNA strand breaks during mouse and human spermiogenesis new insights in stage specificity and link to chromatin remodeling. Biol. Reprod. 70, 910–918 (2004)
D. Sakkas, E. Mariethoz, G. Manicardi, D. Bizzaro, P.G. Bianchi, U. Bianchi, Origin of DNA damage in ejaculated human spermatozoa. Rev. Reprod. 4, 31–37 (1999)
F. Bauché, M.H. Fouchard, B. Jégou, Antioxidant system in rat testicular cells. FEBS Lett. 349, 392–396 (1994)
R.D. Wood, M. Mitchell, T. Lindahl, Human DNA repair genes, 2005. Mutat. Res. 577, 275–83 (2005)
S. Jaroudi, S. SenGupta, DNA repair in mammalian embryos. Mutat Res 635, 53–77 (2007)
F. Leduc, G.B. Nkoma, G. Boissonneault, Spermiogenesis and DNA repair: a possible etiology of human infertility and genetic disorders. Syst. Biol. Reprod. Med. 54, 3–10 (2008)
A. Calogero, R. Polosa, A. Perdichizzi, F. Guarino, S. La Vignera, A. Scarfia, E. Fratantonio, R. Condorelli, O. Bonanno, N. Barone, N. Burrello, R. D’Agata, E. Vicari, Cigarette smoke extract immobilizes human spermatozoa and induces sperm apoptosis. Reprod. Biomed. Online 19, 564–571 (2009)
D. Sakkas, J.G. Alvarez, Sperm DNA fragmentation: mechanisms of origin, impact on reproductive outcome, and analysis. Fertil. Steril. 93, 1027–1036 (2010)
C. Paul, B. Robaire, Ageing of the male germ line. Nat. Rev. Urol. 10, 227–234 (2013)
A. Garolla, I. Cosci, A. Bertoldo, B. Sartini, E. Boudjema, C. Foresta, DNA double strand breaks in human spermatozoa can be predictive for assisted reproductive outcome. Reprod. Biomed. Online 31, 100–107 (2015)
S.M. Ruwanpura, R.I. McLachlan, S.J. Meachem, Hormonal regulation of male germ cell development. J. Endocrinol. 205, 117–131 (2010)
Acknowledgments
We thank Massimo Menegazzo, Sara Corrò, Sabina Magagna, Adriano Presciutti and Giorgia Romanato, for technical assistance and all the staff of the Pathology of Human Reproduction Unit for helpful discussion. Special thanks to Mrs Karyn Ashley Cecchini BSc, PGDip, for her careful editing.
Author contribution All the authors had full access to the original data, reviewed the data analysis, contributed to data interpretation and to the writing of the report, made final decisions on all parts of the report and approved the final version of the submitted report. A.G., B.E. and C.F. conceived the study and participated in study design and A.G., M.G. and B.E. enrolled subjects and I.C., B.S., A.B. made semen and molecular analyses and A.G., A.B., and A.D.N. and undertook statistical analysis and A.G., M.G., A.B., and A.D.N. contributed to data collection and generation of tables and figures and A.G., M.G., B.E. and C.F. wrote and revised the manuscript
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Garolla, A., Ghezzi, M., Cosci, I. et al. FSH treatment in infertile males candidate to assisted reproduction improved sperm DNA fragmentation and pregnancy rate. Endocrine 56, 416–425 (2017). https://doi.org/10.1007/s12020-016-1037-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-016-1037-z