Abstract
Objective
This trial’s objective was to investigate the effect of an exercise program with and without cognitive-behavioral therapy (CBT), compared by a control group, on weight, functional capacity, and cardiometabolic profile of morbidly obese individuals while waiting for bariatric surgery.
Materials and Methods
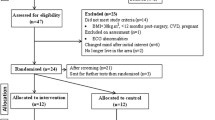
This randomized controlled trial investigated the effect of a 4-month low-intensity exercise program (two weekly sessions of 25 min each) on 66 morbidly obese individuals awaiting bariatric surgery. Participants were randomly divided into three groups: EXER, exercise program; EXER + CBT, exercise program plus support group sessions for lifestyle modification, with a CBT; and CONTROL, routine treatment. They were compared on weight, functional capacity, and cardiometabolic profile.
Results
The weight change (Kg) was −7.4 (−9.6 to 5,1); −4,2 (−6,8 to −1.6) and 2.9 (0.4 to 5.3) and the BMI change (kg/m2) was −2.7 (−3.6 to −1.8); −1.4 (−2.4 to −0.4) and 1.1 (0.1 to 2.1) for groups EXER, EXER + CBT, and CONTROL, respectively. Changes were significant when compared to the control group (p < 0.001), but there were no differences between the two intervention arms (p = 0.2). Functional capacity and cardiometabolic parameters significantly improved in the intervention arms and worsened in the control group. The adherence to the exercise program in both groups was above 78 %.
Conclusion
A 4-month, twice-weekly supervised program of low-intensity physical activity that encourages individuals to adopt a more active lifestyle can positively interfere with weight loss and improvement in functional capacity and cardiometabolic parameters of morbidly obese individuals with and without the aid of support group sessions.



Similar content being viewed by others
References
Elrazek AEMAA, Elbanna AEM, Bilasy SE. Medical management of patients after bariatric surgery: principles and guidelines. World Journal of Gastrointestinal Surgery. 2014;6(11):220–8. doi:10.4240/wjgs.v6.i11.220.
Barnes LT, Elder CL, Pujol TJ. Overweight and obese adults: pathology and treatment. National Strength and Conditioning Association. 2004;26(3):64–5.
Global Health Observatory (GHO) data web site [internet]. Overweight and Obesity Adults aged 18+. WHO 2016. Available from: http://www.who.int/gho/ncd/risk_factors/overweight_text/en/.
Flegal KM, Carroll MD, Kit BK, Ogden CL. Prevalence of obesity and trends in the distribution of body mass index among US adults, 1999-2010. JAMA. 2012;307(5):491–7. doi:10.1001/jama.2012.39.
Livhits M, Mercado C, Yermilov I, Patrick J, Dutson E, Mehran A, et al. Behavioral factors associated with successful weight loss after gastric bypass. Am Surgeon. 2010;76:1139–42.
Borisenko O, Adam D, Funch-Jensen P, Ahmed AR. e col: bariatric surgery can lead to net cost savings to health care systems: results from a comprehensive European decision analytic model. Obes Surg. 2015;25(9):1559–68. doi:10.1007/s11695-014-1567-5.
Peacock JC, Sloan SS, Cripps B. A qualitative analysis of bariatric patients’ post-surgical barriers to exercise. Obes Surg. 2014;24(2):292–8. doi:10.1007/s11695-013-1088-7.
Colquitt JL, Pickett K, Loveman E, Frampton GK. Surgery for weight loss in adults. Cochrane Database Syst Rev. 2014;8:CD003641. doi:10.1002/14651858.CD003641.pub4.
Fonseca Jr SJ, Sá CGAB, Rodrigues PAF, Oliveira AJ, Fernandes-Filho J. Physical exercise and morbid obesity: a systematic review. ABCD Arq Bras Cir Dig. 2013;26(1):67–73. doi:10.1590/S0102-67202013000600015.
Kolotkin RL, LaMonte MJ, Litwin S, Crosby RD, Gress R, et al. Cardiorespiratory fitness and health-related quality of life in bariatric surgery patients. Obes Surg. 2011;21(4):457–64. doi:10.1007/s11695-010-0261-5.
Marcon ER, Gus I, Neumann CR. Impact of a minimum program of supervised exercise in the cardiometabolic risk in patients with morbid obesity. Arq Bras Endocrinol Metab. 2011;55(5):331–8.
Murguia MS, Sierra AVE, Tamayo MT. Intervention cognitive-behavioral group for weight loss and quality of life of patients candidates for surgery. ActColomPsicol. 2014;17(1):25–34.
Wadden TA, Webb VL, Moran CH, Bailey BAE. Lifestyle modification for obesity: new developments in diet, physical activity, and behavior therapy. Circulation. 2012;125(9):1157–70. doi:10.1161/CIRCULATIONAHA.111.039453.
Vetter ML, Faulconbridge LF, Webb VL, Wadden TA. Behavioral and pharmacologic therapies for obesity. Nat Rev Endocrinol. 2010;6(10):578–88. doi:10.1038/nrendo.2010.121.
Mann DL. Heart failure and cor pulmonale. In: Fauci AS, Braunwald E, Kasper D, Hauser SL, Longo D, et al., editors. Harrison’s principles of internal medicine. 17th ed. New York: Mac GraW hil; 2008. p. 1448.
Neumann CR, Marcon ER, Molina CG. Obesity. In: Gusso G, Lopes JMC, editors. Treaty of family and community medicine: principles, practice and training, Porto Alegre/Brazil: art med; 2012. p. 1417–27.
Enrigh PL, Sherrill DL. Reference equations for six-minute walk in healthy adults. Am J Respir Crit Care Med. 1998;158(5 Pt 1):1384–7.
Cahalin L, Mathier MA, Semigran MJ, Dec GW, DiSalvo TG. The six-minute walk test predicts peak oxygen uptake and survival in patients with advanced heart failure. Chest. 1996;110(2):325–32.
Ross RM, Murthy JN, Wollak ID, Jackson AS. The six minute walk test accurately estimates mean peak oxygen uptake. BMC Pulm Med. 2010;10:31.
American Thoracic Society ATS Statement. Guidelines for the six-minute walk test. Am J Respir Crit Care Med. 2002;166:111–7.
Borg GAV. Psychophysical bases of perceived exertion. Med Sci Sports Exerc. 1982;14:377–81. 14.
D’Agostino RB, Vasan RS, Pencina MJ, Wolf PA, Cobain M, Massaro JM, Kannel WB. General cardiovascular risk profile for use in primary care: the Framingham heart study. Circulation. 2008;117(6):743–53. doi:10.1161/CIRCULATIONAHA.107.699579.
Gushiken CS, Vulcano DSB, Tardivo AP, Rasera Jr I, Leite CVS, Maria Oliveira RM. Evolution of weight loss among individuals in the wating line for bariatric surgery in a multidisciplinary secondary healthcare outpatient clinic. Medicina (Ribeirão Preto). 2010;43(1):20–8.
Lakoff JM, Ellsmere J, Ransom T. Cause of death in patients awaiting bariatric surgery. Can J Surg. 2015;58(1):15–8. doi:10.1503/cjs.002914.
Gaber CE, Blissmer B, Deschenes MR, Franklin BA, Lamonte MJ, Lee IM, Nieman DC, Swain DP. American College of Sports Medicine. American College of Sports Medicine position. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal and neuromotor fitness in apparently healthy adults: guidance for prescribing exercise. Med Sci Sports Exer. 2011;43(7):1334–59. doi:10.1249/MSS.0b013e318213fefb.
Poirier P, Cornier MA, Mazzone T, et al. American Heart Association Obesity Committee of the Council on Nutrition, Physical Activity, and Metabolism. Bariatric surgery and cardiovascular risk factors: a scientific statement from the American Heart Association. Circulation. 2011;123(15):1683–701. doi:10.1161/CIR.0b013e3182149099.
American Society of Metabolic and Bariatric Surgery.. [Accessed 2 Feb 2012] ASMBS Public and Professional Education a Committee Bariatric Surgery: Postoperative Concerns. Avaliable at: http// s3.amazonaws.com/publicASMBS/GuidelinesStatements/Guidelines/asbs_bspc.pdf.)
King WC, Bond DS. The importance of pre and postoperative physical activity counseling in bariatric surgery. Exerc Sport Sci Rev. 2013;41(1):26–35. doi:10.1097/JES.0b013e31826444e0.
Ekelund U, Ward HA, Norat T, Luan J, et al. Activity and all-cause mortality across levels of overall and abdominal adiposity in European men and women: the European Prospective Investigation into Cancer and utrition Study (EPIC). Am J Clin Nutr. 2015;101(3):613–21. doi:10.3945/ajcn.114.100065.
Gallagher MJ, Franklin BA, Ehrman JK, Keteyian SJ, Brawner CA, DeJong AT, et al. Comparative impact of morbid obesity vs. heart failure on cardiorespiratory fitness. Chest. 2005;127(6):2197–203.
Zavorsky GS, Murias JM, Kim DJ, Gow J, Christou NV. Poor compensatory hyperventilation in morbidly obese women at peak exercise. Respir Physiol Neurobiol. 2007;159(2):187–95.
Hullens M, Vansant G, Claessens AL, Lysens R, Muls E. Predictors of 6 minute walk test results in lean, obese and morbidly obese women. Scand J Med Sci Sports. 2003;13(2):98–105.
Wing RR. Reduction in weight and cardiovascular disease (CVD) risk factors in subjects with type 2 diabetes (T2DM): four-year results of look AHEAD [abstract 06-0R]. Obesity. 2009;17(Suppl 2):S49.
Wing REA. Long-term effects of a lifestyle intervention on weight and cardiovascular risk factors in individuals with type 2 diabetes mellitus: four-year results of the look AHEAD trial. Arch Intern Med. 2011;170(17):1566–75. doi:10.1001/archinternmed.2010.334.
Unick J, Beavers D, Jakicic J. Effectiveness of lifestyle interventions for individuals with severe obesity and type 2 diabetes results from the look AHEAD trial. Diabetes Care. 2011;34(10):2152–7. doi:10.2337/dc11-0874.
Livhits M, Mercado C, Yermilov I, Parikh JA, Dutson E, Mehran A, et al. Does weight loss immediately before bariatric surgery improve outcomes: a systematic review. Surg Obes Relat Dis. 2009;5(6):713–21. doi:10.1016/j.soard.2009.08.014.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was approved by the research ethics committee of Hospital de Clínicas de Porto Alegre, protocol number 100–328
Financial Support
This study was supported by the Hospital de Clínicas de Porto Alegre Research and Events Incentive Fund (FIPE), Higher Education Coordination of Improvement (CAPES).
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Trial Registration NCT02406976
Rights and permissions
About this article
Cite this article
Marcon, E.R., Baglioni, S., Bittencourt, L. et al. What Is the Best Treatment before Bariatric Surgery? Exercise, Exercise and Group Therapy, or Conventional Waiting: a Randomized Controlled Trial. OBES SURG 27, 763–773 (2017). https://doi.org/10.1007/s11695-016-2365-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-016-2365-z