Abstract
Purpose
To study the impact of race in an equal access care institution with a predominantly African-American (AA) population.
Methods
We retrospectively reviewed data from 222 men with low risk (LR) or intermediate risk (IR) prostate cancer who underwent radical prostatectomy at the New York Harbor VA between 2003 and 2011. Biochemical relapse, distant control, and prostate cancer-specific survival were analyzed using the Kaplan–Meier method and compared using the log-rank test. Univariate and multivariate Cox regression modeling was performed to determine the impact of covariates on biochemical outcome.
Results
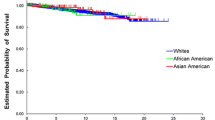
Most patients (65.3 %) were AA. The median follow-up was 58 months, and 89.6 % of patients were followed for a minimum of 2 years after their surgery. Analyzing the whole cohort, the biochemical control was improved in Caucasian patients compared with AA (90.2 vs. 75.4 %, p = 0.008). On subgroup analysis, for IR disease, this difference was no longer significant, 80.5 % for Caucasians versus 69.8 % for AA (p = 0.36). However, for LR disease, the 5-year biochemical control remained significantly improved for Caucasians compared with AA, with a 5-year biochemical control of 97.6 versus 81.7 %, p = 0.006. On multivariate analysis, AA race was a significant predictor for biochemical recurrence (HR 2.69, 95 % CI 1.27–5.65, p = 0.009). There were no differences between the two groups regarding distant control (p = 0.14) or prostate cancer-specific survival (p = 0.29).
Conclusions
In this predominant AA population with equal access to medical care, AA race is an independent predictor of biochemical recurrence after prostatectomy in men with LR or IR prostate cancer.



Similar content being viewed by others
References
Siegel R, Naishadham D, Jemal A (2013) Cancer statistics, 2013. CA Cancer J Clin 63(1):11–30
Chornokur G, Dalton K, Borysova M, Kumar N (2011) Disparities at presentation, diagnosis, treatment and survival in African American men affected by prostate cancer. Prostate 71(9):985–997
Hudson MA, Luo S, Chrusciel T et al (2014) Do racial disparities exist in the use of prostate cancer screening and detection tools for US Veterans? Urol Oncol 32(1):34.e9–34.e18
Skolarus TA, Chan S, Shelton JB et al (2013) Quality of prostate cancer care among rural men in the Vetrans Health Administration. Cancer 119(20):3629–3635
Sundi D, Ross AE, Humpreys EB et al (2013) African American men with very low risk prostate cancer exhibit adverse oncologic outcomes after radical prostatectomy: should active surveillance still be an option for them? J Clin Oncol 31(24):2991–2997
Iselin CE, Box JW, Vollmer RT, Layfield LJ, Robertson JE, Paulson DF (1998) Surgical control of clinically localized prostate carcinoma is equivalent in African-American and white males. Cancer 83(11):2353–2360
Eastham JA, Kattan MW (2000) Disease recurrence in black and white men undergoing radical prostatectomy for clinical stage T1–T2 prostate cancer. J Urol 163(1):143–145
Cross CK, Shultz D, Malkowicz SB et al (2002) Impact of race on prostate-specific antigen outcome after radical prostatectomy for clinically localized adenocarcinoma of the prostate. J Clin Oncol 20(12):2863–2868
Freedland SL, Jalkut M, Dorey F, Sutter ME, Aronsen EJ (2000) Race is not an independent predictor of biochemical recurrence after radical prostatectomy in an equal access medical center. Urology 56(1):87–91
Freedland SJ, Amling CL, Dorey F et al (2002) Race as an outcome predictor after radical prostatectomy: results from the Shared Equal Access Regional Cancer Hospital (SEARCH) database. Urology 60(4):670–674
Hamilton RJ, Aronson WJ, Presti JC Jr et al (2007) Race, biochemical disease recurrence, and prostate-specific antigen doubling time after radical prostatectomy: results from the SEARCH database. Cancer 110(10):2202–2209
Ritch CR, Morrison BF, Hruby G et al (2013) Pathological outcome and biochemical recurrence-free survival after radical prostatectomy in African-American, Afro-caribbean (Jamaican) and Caucasian-American men: an international comparison. BJU Int 111 (4 pt B):e186–e190
Chu DI, Moreira DM, Gerber L et al (2012) Effect of race and socioeconomic status on surgical margins and biochemical outcomes in an equal-access health care setting: results from the Shared Equal Access Regional Cancer Hospital (SEARCH) database. Cancer 118(20):4999–5007
Park HS, Lloyd S, Decker RH, Yu JB (2012) Limitations and biases of the surveillance, epidemiology and end results database. Curr Probl Cancer 36(4):216–224
National Cancer Care Network Guidelines for Prostate Cancer. http://www.nccn.org/professionals/physician_gls/pdf/prostate.pdf. Accessed 21 Nov 2013
Iremashvalli V, Soloway MS, Rosenberg DL, Manoharan M (2012) Clinical and demographic characteristics associated with prostate cancer progression in patients on active surveillance. Urology 187(5):1594–1599
Abern MR, Bassett MR, Tsivian M et al (2013) Race is associated with discontinuation of active surveillance of low risk prostate cancer: results from the Duke Prostate Center. Prostate Cancer Prostatic Dis 16(1):84–89
Conflict of interest
The authors have no conflict of interest to report.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schreiber, D., Levy, E.B., Schwartz, D. et al. Impact of race in a predominantly African-American population of patients with low/intermediate risk prostate cancer undergoing radical prostatectomy within an equal access care institution. Int Urol Nephrol 46, 1941–1946 (2014). https://doi.org/10.1007/s11255-014-0773-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-014-0773-3