Abstract
Objectives
Due to high rates of fetal alcohol spectrum disorder (FASD) in South Africa, reducing alcohol use during pregnancy is a pressing public health priority. The aim of this study was to qualitatively explore knowledge and attitudes about maternal alcohol consumption among women who reported alcohol use during pregnancy.
Methods
The study was conducted in Cape Town, South Africa. Participants were pregnant or within 1 year postpartum and self-reported alcohol use during pregnancy. In-depth interviews explored personal experiences with drinking during pregnancy, community norms and attitudes towards maternal drinking, and knowledge about FASD. Transcripts were analyzed using a content analytic approach, including narrative memos and data display matrices.
Results
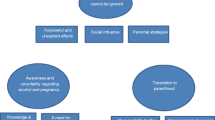
Interviews revealed competing attitudes. Women received anti-drinking messages from several sources, but these sources were not highly valued and the messages often contradicted social norms. Women were largely unfamiliar with FASD, and their knowledge of impacts of fetal alcohol exposure was often inaccurate. Participants’ personal experiences influenced their attitudes about the effects of alcohol during pregnancy, which led to internalization of misinformation. The data revealed a moral conflict that confronted women in this setting, leaving women feeling judged, ambivalent, or defensive about their behaviors, and ultimately creating uncertainty about their alcohol use behaviors.
Conclusions
Data revealed the need to deliver accurate information about the harms of fetal alcohol exposure through sources perceived as trusted and reliable. Individual-level interventions to help women reconcile competing attitudes and identify motivations for reducing alcohol use during pregnancy would be beneficial.
Similar content being viewed by others
Notes
Participant numbers are linked to data in Table 1.
References
May, P. A., Blankenship, J., Marais, A. S., et al. (2013). Approaching the prevalence of the full spectrum of fetal alcohol spectrum disorders in a South African population-based study. Alcoholism, Clinical and Experimental Research, 37(5), 818–830. doi:10.1111/acer.12033.
May, P. A., Blankenship, J., Marais, A. S., et al. (2013). Maternal alcohol consumption producing fetal alcohol spectrum disorders (FASD): Quantity, frequency, and timing of drinking. Drug and Alcohol Dependence, 133(2), 502–512. doi:10.1016/j.drugalcdep.2013.07.013.
May, P. A., Tabachnick, B. G., Gossage, J. P., et al. (2013). Maternal factors predicting cognitive and behavioral characteristics of children with fetal alcohol spectrum disorders. Journal of Developmental and Behavioral Pediatrics, 34(5), 314–325. doi:10.1097/DBP.0b013e3182905587.
May, P. A., & Gossage, J. P. (2011). Maternal risk factors for fetal alcohol spectrum disorders: Not as simple as it might seem. Alcohol Research & Health: The Journal of the National Institute on Alcohol Abuse and Alcoholism, 34(1), 15–26.
Martinez, P., Roislien, J., Naidoo, N., et al. (2011). Alcohol abstinence and drinking among African women: Data from the World Health Surveys. BMC Public Health, 11, 160. doi:10.1186/1471-2458-11-160.
May, P. A., Gossage, J. P., Brooke, L. E., et al. (2005). Maternal risk factors for fetal alcohol syndrome in the Western cape province of South Africa: A population-based study. American Journal of Public Health, 95(7), 1190–1199. doi:10.2105/ajph.2003.037093.
Daley, S. (1999). Workers’ free wine ends, but South Africans still pay. New York Times (archived by Vancouver Sun). http://blogs.vancouversun.com/2010/02/03/when-wine-instead-of-money-is-the-payment-nothing-good-flows/.
Merten, M. (2003). New Liquor Bill outlaws ‘dop’ system. Mail & Guardian. http://mg.co.za/article/2003-09-05-new-liquor-bill-outlaws-dop-system.
London, L. (1999). The ‘dop’ system, alcohol abuse and social control amongst farm workers in South Africa: A public health challenge. Social Science and Medicine, 48(10), 1407–1414.
London, L., Sanders, D., & te Naude, J. W. (1998). Farm workers in South Africa–the challenge of eradicating alcohol abuse and the legacy of the ‘dop’ system. South African Medical Journal, 88(9), 1092–1095.
Gossage, J. P., Snell, C. L., Parry, C. D., et al. (2014). Alcohol use, working conditions, job benefits, and the legacy of the “Dop” system among farm workers in the Western Cape Province, South Africa: Hope despite high levels of risky drinking. International Journal of Environmental Research and Public Health, 11(7), 7406–7424. doi:10.3390/ijerph110707406.
Sanders, D., & Chopra, M. (2006). Key challenges to achieving health for all in an inequitable society: The case of South Africa. American Journal of Public Health, 96(1), 73–78. doi:10.2105/ajph.2005.062679.
Stuckler, D., Basu, S., & McKee, M. (2011). Health care capacity and allocations among South Africa’s provinces: Infrastructure-inequality traps after the end of apartheid. American Journal of Public Health, 101(1), 165–172. doi:10.2105/ajph.2009.184895.
Tomlinson, M., O’Connor, M. J., le Roux, I. M., et al. (2014). Multiple risk factors during pregnancy in South Africa: The need for a horizontal approach to perinatal care. Prevention Science: The Official Journal of the Society for Prevention Research, 15(3), 277–282. doi:10.1007/s11121-013-0376-8.
Bronfenbrenner, U. (1999). Environments in developmental perspective: Theoretical and operational models. In S. Friedman & T. Wachs (Eds.), Measuring environment across the life span: Emerging methods and concepts (pp. 3–28). Washington, DC: American Psychological Association Press.
Dahlberg, L., & Krug, E. (2002). Violence-a global public health problem. In E. Krug, L. Dahlberg, J. Mercy, et al. (Eds.), World report on violence and health (pp. 1–56). Geneva: World Health Organization.
Ethen, M. K., Ramadhani, T. A., Scheuerle, A. E., et al. (2009). Alcohol consumption by women before and during pregnancy. Maternal and Child Health Journal, 13(2), 274–285. doi:10.1007/s10995-008-0328-2.
Choi, K. W., Abler, L. A., Watt, M. H., et al. (2014). Drinking before and after pregnancy recognition among South African women: The moderating role of traumatic experiences. BMC Pregnancy and Childbirth, 14, 97. doi:10.1186/1471-2393-14-97.
Parry, C., London, L., & Myers, B. (2014). Delays in South Africa’s plans to ban alcohol advertising. Lancet, 383(9933), 1972. doi:10.1016/S0140-6736(14)60954-5.
Parry, C. (2014). African experience supports view that the global alcohol industry should have no role in the formulation of public health policies. Addiction, 109(7), 1211–1212. doi:10.1111/add.12582.
Watt, M. H., Eaton, L. A., Choi, K. W., Velloza, J., Kalichman, S. C., Skinner, D., et al. (2014). “It’s better for me to drink, at least the stress is going away”: Perspectives on alcohol use during pregnancy among South African women attending drinking establishments. Social Science and Medicine, 116, 119–125. doi:10.1016/j.socscimed.2014.06.048.
City of Cape Town. (2013). 2011 Census—delft profile. Compiled by Strategic Development Information and GIS Department, City of Cape Town, using 2011 Census data supplied by Statistics South Africa.
Sikkema, K. J., Watt, M. H., Meade, C. S., Ranby, K. W., Kalichman, S. C., Skinner, D., et al. (2011). Mental health and HIV sexual risk behavior among patrons of alcohol serving venues in Cape Town, South Africa. Journal of Acquired Immune Deficiency Syndromes, 57(3), 230–237. doi:10.1097/QAI.0b013e3182167e7a.
Watt, M. H., Aunon, F. M., Skinner, D., Sikkema, K. J., Kalichman, S. C., & Pieterse, D. (2012). “Because he has bought for her, he wants to sleep with her”: Alcohol as a currency for sexual exchange in South African drinking venues. Social Science & Medicine, 74(7), 1005–1012. doi:10.1016/j.socscimed.2011.12.022.
Watt, M. H., Ranby, K. W., Meade, C. S., Sikkema, K. J., MacFarlane, J. C., Skinner, D., et al. (2012). Posttraumatic stress disorder symptoms mediate the relationship between traumatic experiences and drinking behavior among women attending alcohol-serving venues in a South African township. Journal of Studies on Alcohol and Drugs, 73(4), 549–558.
Miles, M. B., & Huberman, A. M. (1994). Qualitative data analysis: An expanded sourcebook (2nd ed.). Thousand Oaks: Sage Publications.
Eaton, L. A., Pitpitan, E. V., Kalichman, S. C., et al. (2014). Beliefs about fetal alcohol spectrum disorder among men and women at alcohol serving establishments in South Africa. The American Journal of Drug and Alcohol Abuse, 40(2), 87–94. doi:10.3109/00952990.2013.830621.
Handmaker, N. S., Miller, W. R., & Manicke, M. (1999). Findings of a pilot study of motivational interviewing with pregnant drinkers. Journal of Studies on Alcohol, 60(2), 285–287.
Chang, G., McNamara, T. K., Orav, E. J., et al. (2005). Brief intervention for prenatal alcohol use: A randomized trial. Obstetrics and Gynecology, 105(5 Pt 1), 991–998. doi:10.1097/01.aog.0000157109.05453.84.
Miller, W. R., & Rollnick, S. (2013). Motivational interviewing: Helping people change (3rd ed.). New York, NY: Guilford Press.
Rendall-Mkosi, K., Morojele, N., London, L., et al. (2013). A randomized controlled trial of motivational interviewing to prevent risk for an alcohol-exposed pregnancy in the Western Cape, South Africa. Addiction, 108(4), 725–732. doi:10.1111/add.12081.
Acknowledgments
This project was funded by a Grant from the National Institute of Alcohol Abuse and Alcoholism (R01 AA018074) and supported by the Duke Center for AIDS Research (P30 AI064518) and the HIV/AIDS, Substance Abuse, and Trauma Training Program (R25 DA035692). We are grateful to all the women who participated in this study. We would like to acknowledge Desiree Pieterse, who coordinated data collection, and the local interview team that collected the data, specifically Tembeka Fikizolo and Mariana Bolumole.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Watt, M.H., Eaton, L.A., Dennis, A.C. et al. Alcohol Use During Pregnancy in a South African Community: Reconciling Knowledge, Norms, and Personal Experience. Matern Child Health J 20, 48–55 (2016). https://doi.org/10.1007/s10995-015-1800-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-015-1800-4