Abstract
Background
Surgical resection remains the optimal therapy for cirrhotic patients with hepatocellular carcinoma (HCC) that are not suitable for liver transplantation (LT). Recently, various innovative techniques for liver resection have been developed.
Aim
The aim of the study was to compare radiofrequency-assisted parenchyma transection (RF-PT) with the traditional clamp-crushing (CC) technique to explore the preferred therapy in cirrhotic patients with HCC.
Methods
From January 2009 to December 2010, 75 cirrhotic patients with HCC who underwent hepatectomy were randomized to RF-PT (group 1, n = 38) or CC-PT (group 2, n = 37) groups. The primary endpoint was intraoperative blood loss. The secondary endpoints included hepatic transection time, total operating time, postoperative morbidity, mortality, length of intensive care unit and hospital stays, and liver function.
Results
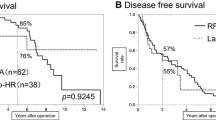
The characteristics of the two patient groups were closely matched. The Pringle maneuver was not used in RF-PT patients. The blood loss of the RF-PT group, total or during transection, was significantly lower than that of the CC-PT group (385 vs. 545 ml, p = 0.001; 105 vs. 260 ml, p = 0.000, respectively). Compared with CC-PT patients, the morbidity of the RF-PT group was lower though not statistically significant (28.9 vs. 38.8 %, p = 0.197). One death occurred in the RF-PT group 12 days postoperative due to a large area cerebral embolism.
Conclusion
RF-PT is a safe and feasible surgical resection method for patients with cirrhosis and concomitant HCC. In addition, RF-PT results in lower blood loss and lower morbidity than the CC technique during liver resection.

Similar content being viewed by others
References
El-Serag HB, Rudolph KL. Hepatocellular carcinoma: epidemiology and molecular carcinogenesis. Gastroenterology. 2007;132:2557–2576.
Caldwell S, Park SH. The epidemiology of hepatocellular cancer: from the perspectives of public health problem to tumor biology. J Gastroenterol. 2009;44:96–101.
Ishizaki Y, Kawasaki S. The evolution of liver transplantation for hepatocellular carcinoma(past, present, and future). J Gastroenterol. 2008;43:18–26.
Thomas MB, Zhu AX. Hepatocellular carcinoma: the need for progress. J Clin Oncol. 2005;23:2892–2899.
Torzilli G, Makuuchi M, Inoue K. The vascular control in liver resection: revisitation of a controversial issue. Hepatogastroenterology. 2002;49:28–31.
Cunningham JD, Fong Y, Shriver C, Melendez J, Marx WL, Blumgart LH. One hundred consecutive hepatic resections. Blood loss, transfusion and operative technique. Arch Surg. 1994;129:1050–1056.
Clavien PA, Yadav S, Sindram D, Bentley RC. Protective effects of ischemic preconditioning for liver resection performed under inflow occlusion in humans. Ann Surg. 2000;232:155–162.
Pai M, Kyriakides C, Mikhail S, Habib NA, et al. Radiofrequency-assisted hepatic resection. Ann Surg Oncol. 2011;18:3391.
Ayav A, Jiao L, Dickinson R, Nicholls J, et al. Liver resection with a new multiprobe bipolar radiofrequency device. Arch Surg. 2008;143:396–401.
Pai M, Jiao LR, Khorsandi S, Canelo R, Spalding DR, Habib NA. Liver resection with bipolar radiofrequency device: Habib 4X. HPB (Oxford). 2008;10:256–260.
Curro G, Jiao L, Scisca C, Baccarani U, et al. Radiofrequency-assisted liver resection in cirrhotic patients with hepatocellular carcinoma. J Surg Oncol. 2008;98:407–410.
Mitsuo M, Takahiro T, Yasuko T, Masayasu A, et al. Radiofrequency (RF)-assisted hepatectomy may induce severe postoperative liver damage. World J Surg. 2007;31:2208–2212.
Berber E, Siperstei A. Radiofrequency(RF)-assisted hepatectomy may induce severe liver damage. World J Surg. 2008;32:1897–1898.
Subrt Z, Ferko A, Jon B, Cecka F. Radiofrequency-assisted liver resection: higher incidence of infectious complications? Acta Chir Belg. 2011;111:165–170.
Kim KH, Lee SG. Usefulness of Kelly clamp crushing technique during hepatic resection. HPB (Oxford). 2008;10:281–284.
Delis S, Bakoyiannis A, Tassopoulos N, Athanassiou K, et al. Clamp-crush technique vs. radiofrequency-assisted liver resection for primary and metastatic liver neoplasms. HPB (Oxford). 2009;11:339–344.
Lupo L, Gallerani A, Panzera P, Tandoi F, Di Palma G, Memeo V. Randomized clinical trial of radiofrequency- assisted versus clamp-crushing liver resection. Br J Surg. 2007;94:287–291.
Rahbari NN, Koch M, Schmidt T, Motschall E, et al. Meta-analysis of the clamp-crushing technique for transection of the parenchyma in elective hepatic resection: back to where we started? Ann Surg Oncol. 2009;16:630–639.
Pamecha V, Gurusamy KS, Sharma D, Davidson BR. Techniques for liver parenchymal transection: a meta-analysis of randomized controlled trials. HPB (Oxford). 2009;11:275–281.
Milićević M, Bulajić P, Zuvela M, Dervenis C, Basarić D, Galun D. A radiofrequency-assisted minimal blood loss liver parenchyma dissection technique. Dig Surg. 2007;24:306–313.
Weber JC, Navarra G, Jiao LR, Nicholls JP, Jensen SL, Habib NA. New technique for liver resection using heat coagulative necrosis. Ann Surg. 2002;236:560–563.
Arita J, Hasegawa K, Kokudo N, Sano K, Sugawara Y, Makuuchi M. Randomized clinical trial of the effect of asaline-linked radiofrequency coagulator on blood loss during hepatic resection. Br J Surg. 2005;92:954–959.
Haghighi KS, Wang F, King J, Daniel S, Morris DL. In-line radiofrequency ablation to minimize blood loss in hepatic parenchymal transection. Am J Surg. 2005;190:43–47.
Pai M, Frampton AE, Mikhail S, Resende V, et al. Radiofrequency assisted liver resection: analysis of 604 consecutive cases. Eur J Surg Oncol. 2012;38:274–280.
Galizia G, Castellano P, Pinto M, Zamboli A, et al. Radiofrequency-assisted liver resection with a comb-shaped bipolar device versus clamp crushing: a clinical study. Surg Innov. 2011;13:158–160.
Kleinert R, Wahba R, Bangard C, Prenzel K, Hölscher AH, Stippel D. Radiomorphology of the Habib sealer-induced resection plane during long-time follow-up: a longitudinal single center experience after 64 radiofrequency-assisted liver resections. HPB Surg. 2010;2010:403097.
Elias D, Sideris L, Pocard M, Dromain C, De Baere T. Intraductal cooling of the main bile ducts during radiofrequency ablation prevents biliary stenosis. J Am Coll Surg. 2004;198:717.
Mathur AK, Ghaferi AA, Osborne NH, Pawlik TM, et al. Body mass index and adverse perioperative outcomes following hepatic resection. J Gastrointest Surg. 2010;14:1285–1291.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
Min Li and Wei Zhang contributed equally to this study.
Rights and permissions
About this article
Cite this article
Li, M., Zhang, W., Li, Y. et al. Radiofrequency-Assisted Versus Clamp-Crushing Parenchyma Transection in Cirrhotic Patients with Hepatocellular Carcinoma: A Randomized Clinical Trial. Dig Dis Sci 58, 835–840 (2013). https://doi.org/10.1007/s10620-012-2394-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-012-2394-y