Abstract
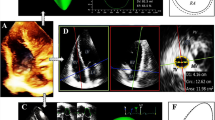
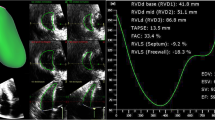
According to current recommendations, patients could benefit from tricuspid valve (TV) annuloplasty at the time mitral valve (MV) surgery if tricuspid regurgitation is severe or if tricuspid annulus (TA) dilatation is present. Therefore, an accurate pre-operative echocardiographic study is mandatory for left but also for right cardiac structures. Aims of this study are to assess right atrial (RA), right ventricular (RV) and TA geometry and function in patients undergoing MV repair without or with TV annuloplasty. We studied 103 patients undergoing MV surgery without (G1: 54 cases) or with (G2: 49 cases) concomitant TV annuloplasty and 40 healthy subjects (NL) as controls. RA, RV and TA were evaluated by three-dimensional (3D) transthoracic echocardiography. Comparing the pathological to the NL group, TA parameters and 3D right chamber volumes were significantly larger. RA and RV ejection fraction and TA% reduction were lower in pathological versus NL, and in G2 versus G1. In pathological patients, TA area positively correlated to systolic pulmonary pressure and negatively with RV and RA ejection fraction. Patients undergoing MV surgery and TV annuloplasty had an increased TA dimensions and a more advanced remodeling of right heart chambers probably reflecting an advanced stage of the disease.




Similar content being viewed by others
References
Koelling TM, Aaronson KD, Cody RJ, Bach DS, Armstrong WF (2002) Prognostic significance of mitral regurgitation and tricuspid regurgitation in patients with left ventricular systolic dysfunction. Am Heart J 144(3):524–529
Shiran A, Sagie A (2009) Tricuspid regurgitation in mitral valve disease incidence, prognostic implications, mechanism, and management. J Am Coll Cardiol 53(5):401–408
Varadarajan P, Pai RG (2010) Tricuspid regurgitation in patients with severe mitral regurgitation and normal left ventricular ejection fraction: risk factors and prognostic implications in a cohort of 895 patients. J Heart Valve Dis 19(4):412–419
Varadarajan P, Pai RG (2012) Prognostic implications of tricuspid regurgitation in patients with severe aortic regurgitation: results from a cohort of 756 patients. Interact CardioVasc Thorac Surg 14(5):580–584
Neuhold S, Huelsmann M, Pernicka E, Graf A, Bonderman D, Adlbrecht C, Binder T, Maurer G, Pacher R, Mascherbauer J (2013) Impact of tricuspid regurgitation on survival in patients with chronic heart failure: unexpected findings of a long-term observational study. Eur Heart J 34(11):844–852
Tei C, Pilgrim JP, Shah PM, Ormiston JA, Wong M (1982) The tricuspid valve annulus: study of size and motion in normal subjects and in patients with tricuspid regurgitation. Circulation 66(3):665–671
Badano LP, Muraru D, Enriquez-Sarano M (2013) Assessment of functional tricuspid regurgitation. Eur Heart J 34(25):1875–1885
le Tourneau T (2013) Right ventricle impairment: are we changing the paradigm in organic mitral regurgitation? Arch Cardiovasc Dis 106(8–9):419–422
Nath J, Foster E, Heidenreich PA (2004) Impact of tricuspid regurgitation on long-term survival. J Am Coll Cardiol 43(3):405–409
Dreyfus GD, Corbi PJ, Chan KM, Bahrami T (2005) Secondary tricuspid regurgitation or dilatation: which should be the criteria for surgical repair? Ann Thorac Surg 79(1):127–132
Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP 3rd, Guyton RA, O’Gara PT, Ruiz CE, Skubas NJ, Sorajja P, Sundt TM 3rd, Thomas JD, American College of Cardiology, American Heart Association Task Force on Practice Guidelines (2014) 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 63(22):57–185
Benedetto U, Melina G, Angeloni E, Refice S, Roscitano A, Comito C, Sinatra R (2012) Prophylactic tricuspid annuloplasty in patients with dilated tricuspid annulus undergoing mitral valve surgery. J Thorac Cardiovasc Surg 143(3):632–638
Topilsky Y, Tribouilloy C, Michelena HI, Pislaru S, Mahoney DW, Enriquez-Sarano M (2010) Pathophysiology of tricuspid regurgitation: quantitative Doppler echocardiographic assessment of respiratory dependence. Circulation 122(15):1505–1513
Fukuda S, Saracino G, Matsumura Y, Daimon M, Tran H, Greenberg NL, Hozumi T, Yoshikawa J, Thomas JD, Shiota T (2006) Three-dimensional geometry of the tricuspid annulus in healthy subjects and in patients with functional tricuspid regurgitation: a real-time, 3-dimensional echocardiographic study. Circulation 114(1 Suppl):I492–I498
Ton-Nu TT, Levine RA, Handschumacher MD, Dorer DJ, Yosefy C, Fan D, Hua L, Jiang L, Hung J (2006) Geometric determinants of functional tricuspid regurgitation: insights from 3-dimensional echocardiography. Circulation 114(2):143–149
Anwar AM, Geleijnse ML, Soliman OI, McGhie JS, Frowijn R, Nemes A, van den Bosch AE, Galema TW, Ten Cate FJ (2007) Assessment of normal tricuspid valve anatomy in adults by real-time three-dimensional echocardiography. Int J Cardiovasc Imaging 23(6):717–724
Tamborini G, Brusoni D, Torres Molina JE, Galli CA, Maltagliati A, Muratori M, Susini F, Colombo C, Maffessanti F, Pepi M (2008) Feasibility of a new generation three-dimensional echocardiography for right ventricular volumetric and functional measurements. Am J Cardiol 102(4):499–505
Tamborini G, Marsan NA, Gripari P, Maffessanti F, Brusoni D, Muratori M, Caiani EG, Fiorentini C, Pepi M (2010) Reference values for right ventricular volumes and ejection fraction with real-time three-dimensional echocardiography: evaluation in a large series of normal subjects. J Am Soc Echocardiogr 23(2):109–115
Muraru D, Badano LP, Sarais C, Soldà E, Iliceto S (2011) Evaluation of tricuspid valve morphology and function by transthoracic three-dimensional echocardiography. Curr Cardiol Rep 13(3):242–249
Maffessanti F, Muraru D, Esposito R, Gripari P, Ermacora D, Santoro C, Tamborini G, Galderisi M, Pepi M, Badano LP (2013) Age-, body size-, and sex-specific reference values for right ventricular volumes and ejection fraction by three-dimensional echocardiography: a multicenter echocardiographic study in 507 healthy volunteers. Circ Cardiovasc Imaging 6(5):700–710
Badano LP, Agricola E, Perez de Isla L, Gianfagna P, Zamorano JL (2009) Evaluation of the tricuspid valve morphology and function by transthoracic real-time three-dimensional echocardiography. Eur J Echocardiogr 10(4):477–484
Mahmood F, Kim H, Chaudary B, Bergman R, Matyal R, Gerstle J, Gorman JH 3rd, Gorman RC, Khabbaz KR (2013) Tricuspid annular geometry: a three-dimensional transesophageal echocardiographic study. J Cardiothorac Vasc Anesth 27(4):639–646
Miller D, Farah MG, Liner A, Fox K, Schluchter M, Hoit BD (2004) The relation between quantitative right ventricular ejection fraction and indices of tricuspid annular motion and myocardial performance. J Am Soc Echocardiogr 17(5):443–447
Pepi M, Tamborini G, Galli C, Barbier P, Doria E, Berti M, Guazzi M, Fiorentini C (1994) A new formula for echo-Doppler estimation of right ventricular systolic pressure. J Am Soc Echocardiogr 7(1):20–26
Calafiore AM, Iacò AL, Romeo A, Scandura S, Meduri R, Varone E, Di Mauro M (2011) Echocardiographic-based treatment of functional tricuspid regurgitation. J Thorac Cardiovasc Surg 142(2):308–313
Taramasso M, Vanermen H, Maisano F, Guidotti A, La Canna G, Alfieri O (2012) The growing clinical importance of secondary tricuspid regurgitation. J Am Coll Cardiol 59(8):703–710
Kim JB, Jung SH, Choo SJ, Chung CH, Lee JW (2013) Clinical and echocardiographic outcomes after surgery for severe isolated tricuspid regurgitation. J Thorac Cardiovasc Surg 146(2):278–284
Shiran A, Najjar R, Adawi S, Aronson D (2014) Risk factors for progression of functional tricuspid regurgitation. Am J Cardiol 113(6):995–1000
Kammerlander AA, Marzluf BA, Graf A, Bachmann A, Kocher A, Bonderman D, Mascherbauer J (2014) Right ventricular dysfunction, but not tricuspid regurgitation, is associated with outcome late after left heart valve procedure. J Am Coll Cardiol 64(24):2633–2642
Kawut SM, Lima JA, Barr RG, Chahal H, Jain A, Tandri H, Praestgaard A, Bagiella E, Kizer JR, Johnson WC, Kronmal RA, Bluemke DA (2011) Sex and race differences in right ventricular structure and function: the multi-ethnic study of atherosclerosis-right ventricle study. Circulation 123(22):2542–2551
Niemann PS, Pinho L, Balbach T, Galuschky C, Blankenhagen M, Silberbach M, Broberg C, Jerosch-Herold M, Sahn DJ (2007) Anatomically oriented right ventricular volume measurements with dynamic three-dimensional echocardiography validated by 3-Tesla magnetic resonance imaging. J Am Coll Cardiol 50(17):1668–1676
Sugeng L, Mor-Avi V, Weinert L, Niel J, Ebner C, Steringer-Mascherbauer R, Bartolles R, Baumann R, Schummers G, Lang RM, Nesser HJ (2010) Multimodality comparison of quantitative volumetric analysis of the right ventricle. JACC Cardiovasc Imaging 3(1):10–18
Tamborini G, Muratori M, Maltagliati A, Galli CA, Naliato M, Zanobini M, Alamanni F, Salvi L, Sisillo E, Fiorentini C, Pepi M (2010) Pre-operative transthoracic real-time three-dimensional echocardiography in patients undergoing mitral valve repair: accuracy in cases with simple vs. complex prolapse lesions. Eur J Echocardiogr 11(9):778–785
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Tamborini, G., Fusini, L., Muratori, M. et al. Right heart chamber geometry and tricuspid annulus morphology in patients undergoing mitral valve repair with and without tricuspid valve annuloplasty. Int J Cardiovasc Imaging 32, 885–894 (2016). https://doi.org/10.1007/s10554-016-0846-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-016-0846-8