Abstract
Purpose
This prospective study aimed to investigate macular structural characteristics in children with Down syndrome compared to those in healthy children.
Methods
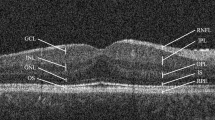
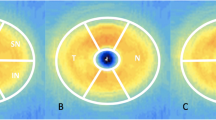
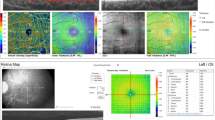
Two groups of children (aged 6–16 years) were enrolled: children with Down syndrome (Down syndrome group, N = 17) and age-matched healthy children who were full-term at birth (control group, N = 18). Eligible patients had visual acuity of 20/100 or better and gestational age at birth of ≥ 36 weeks. Fourier domain optical coherence tomography was used for imaging of the macular retinal structure, and retinal volume scans centered on the macula were obtained. Central subfield thickness (CST) and the thickness of the inner and outer retinal layer regions were analyzed using the instrument’s segmentation software. The analysis of data is provided for the right eye only, since there was no significant difference between right and left eyes for either the Down syndrome or control groups.
Results
Children in the Down syndrome group generally had identifiable retinal structure. The CST for the full retina and inner and outer retinal layers were all significantly greater in the Down syndrome group than the control group (independent t test, all p < 0.05). Despite the significantly thicker macula, only about 29 % (5 of 17) of the right eyes of patients with Down syndrome had macular thickness outside the normal range. Visual acuity in the Down syndrome group was not directly correlated with increased CST (t = 1.288, r = 0.326, p = 0.202).
Conclusions
On average, CST in the Down syndrome group was greater than that in the control group, suggesting abnormal macular development in children with Down syndrome.

Similar content being viewed by others
References
Cregg M, Woodhouse JM, Stewart RE, Pakeman VH, Bromham NR, Gunter HL, Trojanowska L, Parker M, Fraser WI (2003) Development of refractive error and strabismus in children with Down syndrome. Invest Ophthalmol Vis Sci 44(3):1023–1030
Little JA, Woodhouse JM, Lauritzen JS, Saunders KJ (2007) The impact of optical factors on resolution acuity in children with Down syndrome. Invest Ophthalmol Vis Sci 48(9):3995–4001. doi:10.1167/iovs.06-1387
Ljubic A, Trajkovski V, Stankovic B (2011) Strabismus, refractive errors and nystagmus in children and young adults with Down syndrome. Ophthalmic Genet 32(4):204–211. doi:10.3109/13816810.2011.592175
McCullough SJ, Little JA, Saunders KJ (2013) Higher order aberrations in children with Down syndrome. Invest Ophthalmol Vis Sci 54(2):1527–1535. doi:10.1167/iovs.12-10597
Woodhouse JM, Pakeman VH, Cregg M, Saunders KJ, Parker M, Fraser WI, Sastry P, Lobo S (1997) Refractive errors in young children with Down syndrome. Optom Vis Sci 74(10):844–851
Cregg M, Woodhouse JM, Pakeman VH, Saunders KJ, Gunter HL, Parker M, Fraser WI, Sastry P (2001) Accommodation and refractive error in children with Down syndrome: cross-sectional and longitudinal studies. Invest Ophthalmol Vis Sci 42(1):55–63
Felius J, Beauchamp CL, Stager DR Sr (2014) Visual acuity deficits in children with nystagmus and Down syndrome. Am J Ophthalmol 157(2):458–463. doi:10.1016/j.ajo.2013.09.023
John FM, Bromham NR, Woodhouse JM, Candy TR (2004) Spatial vision deficits in infants and children with Down syndrome. Invest Ophthalmol Vis Sci 45(5):1566–1572
Little JA, McCullough S, McClelland J, Jackson AJ, Saunders KJ (2013) Low-contrast acuity measurement: does it add value in the visual assessment of down syndrome and cerebral palsy populations? Invest Ophthalmol Vis Sci 54(1):251–257. doi:10.1167/iovs.12-10506
Little JA, Woodhouse JM, Lauritzen JS, Saunders KJ (2009) Vernier acuity in Down syndrome. Invest Ophthalmol Vis Sci 50(2):567–572. doi:10.1167/iovs.08-2250
Paudel N, Leat SJ, Adhikari P, Woodhouse JM, Shrestha JB (2010) Visual defects in Nepalese children with Down syndrome. Clin Exp Optom 93(2):83–90. doi:10.1111/j.1444-0938.2010.00458.x
Woodhouse JM, Meades JS, Leat SJ, Saunders KJ (1993) Reduced accommodation in children with Down syndrome. Invest Ophthalmol Vis Sci 34(7):2382–2387
Provis JM, Hendrickson AE (2008) The foveal avascular region of developing human retina. Arch Ophthalmol 126(4):507–511. doi:10.1001/archopht.126.4.507
Springer AD, Hendrickson AE (2004) Development of the primate area of high acuity. 2. Quantitative morphological changes associated with retinal and pars plana growth. Vis Neurosci 21(5):775–790. doi:10.1017/S0952523804215115
Wang J, Spencer R, Leffler JN, Birch EE (2012) Critical period for foveal fine structure in children with regressed retinopathy of prematurity. Retina 32(2):330–339. doi:10.1097/IAE.0b013e318219e685
Yuodelis C, Hendrickson A (1986) A qualitative and quantitative analysis of the human fovea during development. Vis Res 26(6):847–855
Candy TR, Crowell JA, Banks MS (1998) Optical, receptoral, and retinal constraints on foveal and peripheral vision in the human neonate. Vis Res 38(24):3857–3870
Wallman J, Winawer J (2004) Homeostasis of eye growth and the question of myopia. Neuron 43(4):447–468
Huynh SC, Samarawickrama C, Wang XY, Rochtchina E, Wong TY, Gole GA, Rose KA, Mitchell P (2009) Macular and nerve fiber layer thickness in Amblyopia: the Sydney childhood Eye study. Ophthalmology 116(9):1604–1609. doi:10.1016/j.ophtha.2009.03.013
Altintas O, Yuksel N, Ozkan B, Caglar Y (2005) Thickness of the retinal nerve fiber layer, macular thickness, and macular volume in patients with strabismic amblyopia. J Pediatr Ophthalmol Strabismus 42(4):216–221
Al-Haddad CE, El Mollayess GM, Mahfoud ZR, Jaafar DF, Bashshur ZF (2013) Macular ultrastructural features in amblyopia using high-definition optical coherence tomography. Br J Ophthalmol 97(3):318–322. doi:10.1136/bjophthalmol-2012-302434
Wang BZ, Taranath D (2012) A comparison between the amblyopic eye and normal fellow eye ocular architecture in children with hyperopic anisometropic amblyopia. J AAPOS 16(5):428–430. doi:10.1016/j.jaapos.2012.06.006
Pang Y, Goodfellow GW, Allison C, Block S, Frantz KA (2011) A prospective study of macular thickness in amblyopic children with unilateral high myopia. Invest Ophthalmol Vis Sci 52(5):2444–2449. doi:10.1167/iovs.10-5550
Yoon SW, Park WH, Baek SH, Kong SM (2005) Thicknesses of macular retinal layer and peripapillary retinal nerve fiber layer in patients with hyperopic anisometropic amblyopia. Korean J Ophthalmol 19(1):62–67
Aziz HA, Ruggeri M, Berrocal AM (2011) Intraoperative OCT of bilateral macular coloboma in a child with Down syndrome. J Pediatr Ophthalmol Strabismus 48:e37–39. doi:10.3928/01913913-20110712-03
Al-Hemidan AI, Al-Hazzaa SA, Chavis P, Al-Hussein H (1999) Optic disc elevation in Down syndrome. Ophthalmic Genet 20(1):45–51
Altun A, Altun G, Kurna SA, Olcaysu OO, Aki SF (2014) Unilateral morning glory optic disc anomaly in a case with Down syndrome. BMC Ophthalmol 14:48. doi:10.1186/1471-2415-14-48
Parsa CF, Almer Z (2008) Supranumerary optic disc vessels may indicate reduced systemic angiogenesis in Down syndrome. Br J Ophthalmol 92(3):432–433. doi:10.1136/bjo.2007.124248
Stirn Kranjc B (2012) Ocular abnormalities and systemic disease in Down syndrome. Strabismus 20(2):74–77. doi:10.3109/09273972.2012.680234
Fimiani F, Iovine A, Carelli R, Pansini M, Sebastio G, Magli A (2007) Incidence of ocular pathologies in Italian children with Down syndrome. Eur J Ophthalmol 17(5):817–822
Bambo MP, Garcia-Martin E, Otin S, Sancho E, Fuertes I, Herrero R, Satue M, Pablo L (2014) Influence of cataract surgery on repeatability and measurements of spectral domain optical coherence tomography. Br J Ophthalmol 98 (1):52–58. doi:10.1136/bjophthalmol-2013-303752
Comyn O, Heng LZ, Ikeji F, Bibi K, Hykin PG, Bainbridge JW, Patel PJ (2012) Repeatability of Spectralis OCT measurements of macular thickness and volume in diabetic macular edema. Invest Ophthalmol Vis Sci 53 (12):7754–7759. doi:10.1167/iovs.12-10895
Wu WC, Lin RI, Shih CP, Wang NK, Chen YP, Chao AN, Chen KJ, Chen TL, Hwang YS, Lai CC, Huang CY, Tsai S (2012) Visual acuity, optical components, and macular abnormalities in patients with a history of retinopathy of prematurity. Ophthalmology 119(9):1907–1916. doi:10.1016/j.ophtha.2012.02.040
Marmor MF, Choi SS, Zawadzki RJ, Werner JS (2008) Visual insignificance of the foveal pit: reassessment of foveal hypoplasia as fovea plana. Arch Ophthalmol 126(7):907–913. doi:10.1001/archopht.126.7.907
Recchia FM, Recchia CC (2007) Foveal dysplasia evident by optical coherence tomography in patients with a history of retinopathy of prematurity. Retina 27(9):1221–1226. doi:10.1097/IAE.0b013e318068de2e
Meyer CH, Lapolice DJ, Freedman SF (2002) Foveal hypoplasia in oculocutaneous albinism demonstrated by optical coherence tomography. Am J Ophthalmol 133(3):409–410
Wang J, Smith HA, Donaldson DL, Haider KM, Roberts GJ, Sprunger DT, Neely DE, Plager DA (2014) Macular structural characteristics in children with congenital and developmental cataracts. J AAPOS. doi:10.1016/j.jaapos.2014.05.008
Laguna A, Barallobre MJ, Marchena MA, Mateus C, Ramirez E, Martinez-Cue C, Delabar JM, Castelo-Branco M, de la Villa P, Arbones ML (2013) Triplication of DYRK1A causes retinal structural and functional alterations in Down syndrome. Hum Mol Genet 22(14):2775–2784. doi:10.1093/hmg/ddt125
Odell D, Dubis AM, Lever JF, Stepien KE, Carroll J (2011) Assessing Errors Inherent in OCT-Derived Macular Thickness Maps. J Ophthalmol 2011:692574. doi:10.1155/2011/692574
Doyle SJ, Bullock J, Gray C, Spencer A, Cunningham C (1998) Emmetropisation, axial length, and corneal topography in teenagers with Down’s syndrome. Br J Ophthalmol 82(7):793–796
Acknowledgments
We thank Afiah Hasnie, Alexander Walls, Jessica Felker and Paxton Ott for helping obtain patient data.
Conflict of interest
All authors certify that they have NO affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Financial support
This study is supported by an Indiana University–Purdue University Indianapolis (IUPUI) EMPOWER [Enhanced Mentoring Program with Opportunities for Ways to Excel in Research] award to Dr. Wang and a Research to Prevent Blindness (RPB) unrestricted grant to the Glick Eye Institute.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
O’Brien, S., Wang, J., Smith, H.A. et al. Macular structural characteristics in children with Down syndrome. Graefes Arch Clin Exp Ophthalmol 253, 2317–2323 (2015). https://doi.org/10.1007/s00417-015-3088-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-015-3088-x