Abstract
Purpose
It is not uncommon for patients to undergo less invasive spine surgery (LISS) prior to succumbing to lumbar fusion; however, the effect of failed LISS on subsequent fusion outcomes is relatively unknown. The aim of this study was to test the hypothesis that patients who suffered failed LISS would afford inferior subsequent fusion outcomes when compared to patients who did not have prior LISS.
Methods
After IRB approval, registry from a spine surgeon was queried for consecutive patients who underwent fusion for intractable low back pain. The 47 qualifying patients were enrolled and split into two groups based upon a history for prior LISS: a prior surgery group (PSG) and a non-prior surgery group (nPSG).
Results
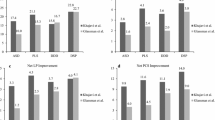
Typical postoperative outcome questionnaires, which were available in 80.9 % of the patients (38/47) at an average time point of 40.4 months (range, 13.5–66.1 months), were comparatively analysed and failed to demonstrate significant difference between the groups, e.g. PSG v. nPSG: ODI—14.6 ± 10.9 vs. 17.2 ± 19.4 (P = 0.60); SF12-PCS—10.9 ± 11.0 vs. 8.7 ± 12.4 (p = 0.59); bNRS—3.0 (range −2–7) vs. 2.0 (range −3–8) (p = 0.91). Patient satisfaction, return to work rates, peri-operative complications, success of fusion and rate of revision surgery were also not different.
Conclusions
Although limited by size and retrospective design, the results of this rare investigation suggest that patients who experience a failed LISS prior to undergoing fusion will not suffer inferior fusion outcomes when compared to patients who did not undergo prior LISS.
Similar content being viewed by others
References
Jarvik JG, Hollingworth W, Heagerty PJ et al (2005) Three-year incidence of low back pain in an initially asymptomatic cohort: clinical and imaging risk factors. Spine 30:1541–1548
Walker BF (2000) The prevalence of low back pain: a systematic review of the literature from 1966 to 1998. J Spinal Disord 13:205–217
Von Korff M, Saunders (1996) The course of back pain in primary care. Spine 21:2833–2837, discussion 8–9
Johannes CB, Le TK, Zhour X et al (2010) The prevalence of chronic pain in United States adults: results of an Internet-based survey. J Pain 11:1230–1239
Dagenais S, Caro J, Haldeman S (2008) A systematic review of low back pain cost of illness studies in the United States and internationally. Spine J 8:8–20
Frank JW, Der MS, Brooker AS et al (1996) Disability resulting from occupational low back pain. Part I: what do we know about primary prevention? A review of the scientific evidence on prevention before disability begins. Spine 21:2908–2917
Wardlaw D, Rithchie IK, Sabboubeh AF et al (2013) Prospective randomized trial of chemonucleolysis compared with surgery for soft disc herniation with one-year, intermediate, and long-term outcome: part I: the clinical outcome. Spine 38:E1051–E1057
Kasch R, Mensel B, Schmidt F et al (2012) Disc volume reduction with percutaneous nucleoplasty in an animal model. PloS One 7:e500211
Adam D, Pevzner E, Gepstein R (2013) Comparison of percutaneous nucleoplasty and open discectomy in patients with lumbar disc protrusions. Chir (Bucur) 108:94–98
Quigley MR (1996) Percutaneous laser discectomy. Neurosurg Clin N Am 1:37–42
Steppan J, Meaders T, Muto M, Murphy KJ (2010) A meta-analysis of the effectiveness and safety of ozone treatments for herniated lumbar discs. J Vasc Interv Radiol 21:534–548
Tsou HK, Chao SC, Kao TH et al (2010) Intradiscal electrothermal therapy in the treatment of chronic low back pain: experience with 93 patients. Surg Neurol Int 4:1–37
Lee SH, Kang HS (2010) Percutaneous endoscopic laser annuloplasty for discogenic low back pain. World Neurosurg 73:198–206, discussion e33
Tsou PM, Yeung C, Yeung AT (2004) Posterolateral transforaminal selective endoscopic discectomy and thermal annuloplasty for chronic lumbar discogenic pain: a minimal access visualize intradiscal surgical procedure. Spine J 4:564–573
Kapural L, Vrooman B, Sarwar S et al (2013) A randomized, placebo-controlled trial of transdiscal radiofrequency, biacuplasty for the treatment of discogenic low back pain. Pain Med 14:362–373
Jenkins LT, Jones AL, Harms JJ (1994) Prognostic factors in lumbar spinal fusion. Contemp Orthop 3:173–180
Kalb S, Perez-Orribo L, Kalani MY et al (2012) The influence of common medical conditions on the outcome of anterior lumbar interbody fusion. J Spinal Disord Tech. Dec 27 [Epub ahead of print]
Harms JG, Jeszenszky D (1998) The posterior, lumbar, interbody fusion in unilateral transforaminal technique. Oper Orthop Traumatol 10:90–102
Glassman SD, Carreon LY, Djurasovic M et al (2008) RhBMP-2 versus iliac crest bone graft for lumbar spine fusion: a randomized controlled trial in patients over 60 years of age. Spine 33:2843–2849
Chen Z, Ba G, Shen T (2012) Recombinant human bone morphogenetic protein versus autogenous iliac crest bone graft for lumbar fusion: a meta-analysis of 10 randomized controlled trials. Arch Orthop Trauma Surg 132:1725–1740
Vanti C, Prosperi D, Boschi M (2013) The Prolo Scale: history, evolution and psychometric properties. J Orthop Traumatol. May 10 [Epub ahead of print]
Acknowledgments
The source of funding for this investigation was a general research grant from Med-Equip Inc., a medical supply company. However, this manufacturer’s products were not involved or discussed in this study and the company had no influence on study design, outcomes, or conclusions.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gillard, D.M., Corenman, D.S. & Dornan, G.J. Failed less invasive lumbar spine surgery as a predictor of subsequent fusion outcomes. International Orthopaedics (SICOT) 38, 811–815 (2014). https://doi.org/10.1007/s00264-013-2167-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-013-2167-z