Abstract
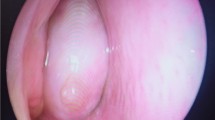
Background True mesenchymal, non-cartilaginous neoplasms of the larynx are rare. Extrapleural solitary fibrous tumor (SFT) is a localized neoplasm characterized by proliferation of thin-walled vessels and collagen-producing cells and is considered within the “hemangiopericytoma-solitary fibrous tumor” spectrum. SFT primary in the larynx is exceptional. Design Case report set in a comparison with other cases reported in the English literature (MEDLINE 1966 to 2007). Results A 49-year old white male presented with difficulty breathing, progressive over the past 2 years. He denied dysphagia and weight loss. Past medical history was significant for asthma. He denied cigarette smoking or alcohol abuse. There were no cervical deformities on physical exam. Fiberoptic laryngoscopy was performed upon stabilization of respiratory function. A smooth, round, submucosal mass measuring 2.3 cm in greatest diameter arising from the inferior surface of left true vocal cord was causing near total obstruction of the endolaryngeal space. The mass was excised. The surface mucosa was intact and unremarkable. A cellular, spindle cell neoplasm was arranged in loose fascicles, associated with heavy collagen fiber deposition. The collagen was wiry and heavy. Cells were bland with cytoplasmic extensions. The nuclei were vesicular to hyperchromatic and elongated with inconspicuous nucleoli. Vessels were prominent and delicate, with patulous spaces. Mitotic figures were easily identified, but atypical forms were not present. The cells were strongly and diffusely immunoreactive with CD34 and bcl-2, while non-reactive with cytokeratin, EMA, actin, ALK-1, S100, desmin, and CD117. These findings confirmed a diagnosis of extraplural solitary fibrous tumor. Without further disease, the patient is alive without evidence of disease, 12 months after surgery. Conclusions The characteristic histologic pattern of solitary fibrous tumor can be noted in extrapulmonary locations. Development in the larynx is uncommon, but the tumor presents as a polypoid mass with characteristic histologic and immunophenotypic features. Conservative local excision is the treatment of choice to yield an excellent prognosis.






Similar content being viewed by others
References
Guillou L, Fletcher JA, Fletcher CDM, Mandahl N. Extrapleural solitary fibrous tumour and haemangiopericytoma. In: Fletcher CDM, Unni K, Mertens F, editors. Pathology and genetics of tumours of soft tissue and bone, world health organization classification of tumours. Kleihues P, Sobin LH, series editors. Lyon, France: IARC Press, 2002:86–90.
Klemperer P, Rabin CB. Primary neoplasms of the pleura. A report of five cases. Arch Pathol 1931;11:385–412.
Hasegawa T, Matsuno Y, Shimoda T, et al. Extrathoracic solitary fibrous tumors: their histological variability and potentially aggressive behavior. Hum Pathol 1999;30:1464–73.
Gold JS, Antonescu CR, Hajdu C, et al. Clinicopathologic correlates of solitary fibrous tumors. Cancer 2002;94:1057–68.
Graadt van Roggen JF, Hogendoorn PCW. Solitary fibrous tumor: the emerging clinicopathologic spectrum of an entity and its differential diagnosis. Curr Diagn Pathol 2004;10:229–35.
Scharifker D, Kaneko M. Localized fibrous “mesothelioma” of pleura (submesothelial fibroma): a clinicopathologic study of 18 cases. Cancer 1979;43:627–35.
Suster S, Nascimento AG, Miettinen M, et al. Solitary fibrous tumors of soft tissue. A clinicopathologic and immunohistochemical study of 12 cases. Am J Surg Pathol 1995;19:1257–66.
Dotto JE, Ahrens W, Lesnik DJ, et al. Solitary fibrous tumor of the larynx: a case report and review of the literature. Arch Pathol Lab Med 2006;130:213–6.
Chan JK. Solitary fibrous tumour–everywhere, and a diagnosis in vogue. Histopathology 1997;31:568–76.
Brunnemann RB, Ro JY, Ordonez NG, et al. Extrapleural solitary fibrous tumor: a clinicopathologic study of 24 cases. Mod Pathol 1999;12:1034–42.
Nielsen GP, O’Connell JX, Dickersin GR, et al. Solitary fibrous tumor of soft tissue: a report of 15 cases, including 5 malignant examples with light microscopic, immunohistochemical, and ultrastructural data. Mod Pathol 1997;10:1028–37.
Safneck JR, guacil-Garcia A, Dort JC, et al. Solitary fibrous tumour: report of two new locations in the upper respiratory tract. J Laryngol Otol 1993;107:252–6.
Benlyazid A, Lescanne E, Lefrancq T, et al. Solitary fibrous tumour of the larynx: report of a case. J Laryngol Otol 1998;112:286–9.
Alobid I, Alos L, Maldonado M, et al. Laryngeal solitary fibrous tumor treated with CO2 laser excision: case report. Eur Arch Otorhinolaryngol 2005;262:286–8.
Alobid I, Bernal-Sprekelsen M, Benitez P, et al. Solitary fibrous tumor of the larynx. Otolaryngol Head Neck Surg 2005;133:163–5.
Fan CY, Van Hemert RL, Thomas JR, et al. Atypical solitary fibrous tumor of the larynx. Otolaryngol Head Neck Surg 2006;134:880–2.
Stomeo F, Padovani D, Bozzo C, et al. Laryngeal solitary fibrous tumour. Auris Nasus Larynx 2007;34:405–8.
Westra WH, Gerald WL, Rosai J. Solitary fibrous tumor. Consistent CD34 immunoreactivity and occurrence in the orbit. Am J Surg Pathol 1994;18:992–8.
Chilosi M, Facchettti F, Dei Tos AP, et al. bcl-2 expression in pleural and extrapleural solitary fibrous tumours. J Pathol 1997;181:362–7.
England DM, Hochholzer L, McCarthy MJ. Localized benign and malignant fibrous tumors of the pleura. A clinicopathologic review of 223 cases. Am J Surg Pathol 1989;13:640–58.
Krismann M, Adams H, Jaworska M, et al. Patterns of chromosomal imbalances in benign solitary fibrous tumours of the pleura. Virch Arch 2000;437:248–55.
Donner LR, Silva MT, Dobin SM. Solitary fibrous tumor of the pleura: a cytogenetic study. Cancer Genet Cytogenet 1999;111:169–71.
Miettinen M, el Rifai W, Sarlomo-Rikala M, et al. Tumor size-related DNA copy number changes occur in solitary fibrous tumors but not in hemangiopericytomas. Mod Pathol 1997;10:1194–200.
Thompson LD, Wieneke JA, Miettinen M, et al. Spindle cell (sarcomatoid) carcinomas of the larynx: a clinicopathologic study of 187 cases. Am J Surg Pathol 2002;26:153–70.
Loos BM, Wieneke JA, Thompson LD. Laryngeal angiosarcoma: a clinicopathologic study of five cases with a review of the literature. Laryngoscope 2001;111:1197–202.
Knott PD, Gannon FH, Thompson LDR. Mesenchymal chondrosarcoma of the sinonasal tract: A clinicopathologic study of 13 cases with a review of the literature. Laryngoscope 2003;113:783–90.
Thompson LD, Miettinen M, Wenig BM. Sinonasal-type hemangiopericytoma: a clinicopathologic and immunophenotypic analysis of 104 cases showing perivascular myoid differentiation. Am J Surg Pathol 2003;27:737–49.
Wenig BM. Tumours of the hypopharynx, larynx and trachea: mucosal malignant melanoma. In: Barnes EL, Eveson JW, Reichart P, Sidransky D, editors. Pathology and genetics of tumours of the head and neck, world health organization classification of tumours. Kleihues P, Sobin LH, series editors. Lyon, France: IARC Press, 2005:160–1.
Thompson LDR, Fanburg-Smith JC. Tumours of the hypopharynx, larynx and trachea: benign soft tissue tumours. In: Barnes EL, Eveson JW, Reichart P, Sidransky D, editors. Pathology and genetics of tumours of the head and neck, world health organization classification of tumours. Kleihues P, Sobin LH, series editors. Lyon, France: IARC Press, 2005:152–5.
Wenig BM. Tumours of the hypopharynx, larynx and trachea: inflammatory myofibroblastic tumour. In: Barnes EL, Eveson JW, Reichart P, Sidransky D, editors. Pathology and genetics of tumours of the head and neck, world health organization classification of tumours. Kleihues P, Sobin LH, series editors. Lyon, France: IARC Press, 2005:150–1.
Acknowledgements
The opinions or assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the University of California or Southern California Permanente Medical Group.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Thompson, L.D.R., Karamurzin, Y., Wu, M.Lc. et al. Solitary Fibrous Tumor of the Larynx. Head and Neck Pathol 2, 67–74 (2008). https://doi.org/10.1007/s12105-008-0044-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12105-008-0044-7