Abstract
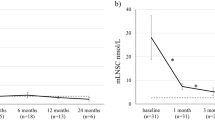
Octreotide (OCT) is ineffective in patients with Cushing’s disease (CD) due to the cortisol-induced down-regulation of somatostatin receptor subtype 2 which was shown to be reversible in vitro by using anti-glucocorticoid mifepristone. This study aimed to verify, in vivo, if mifepristone can modulate response to acute OCT administration in patients with CD. Three men and two postmenopausal women (age 52.5 ± 2 years) with CD were enrolled in the study. OCT (100 μg, s.c.) was administered alone on the first day (OCT-only), and it was then given after mifepristone administration (2 × 200 mg, p.os, 12 and 1 h before OCT), 3 days later (OCT-mif). ACTH and cortisol levels were measured before OCT administration and every 60 min thereafter for 6 h. Baseline ACTH and cortisol values, nadir values and percentage decrements (Δn) were compared during both tests. Mean ACTH-Δn did not differ significantly during the two tests. Both tests induced a <30 % decrease in plasma ACTH in three patients (#1, 2 and 3) and a >50 % decrease in the other two cases (#4 and 5). Cortisol decreased in patients #4 and 5, during both tests. ACTH-Δn did not correlate with morning cortisol nor with urinary free cortisol values. Patients #4 and 5 with the highest ACTH-Δn had the lowest cortisol values after 1 mg of dexamethasone. Brief mifepristone pre-treatment does not modify ACTH and cortisol response to acute OCT administration in CD. However, OCT seems to be more effective in patients with partially preserved cortisol inhibitory feedback.


Similar content being viewed by others
References
J. Newell-Price, X. Bertagna, A.B. Grossman, L.K. Nieman, Cushing’s syndrome. Lancet 367, 1605–1617 (2006)
X. Bertagna, L. Guignat, Approach to the Cushing’s disease patient with persistent/recurrent hypercortisolism after pituitary surgery. J. Clin. Endocrinol. Metab. 98(4), 1307–1318 (2013)
S. Cannavo, B. Almoto, C. Dall’Asta, S. Corsello, R.M. Lovicu, E. De Menis, F. Trimarchi, B. Ambrosi, Long-term results of treatment in patients with ACTH-secreting pituitary macroadenomas. Eur. J. Endocrinol. 149(3), 195–200 (2003)
B.M. Biller, A.B. Grossman, P.M. Stewart, S. Melmed, X. Bertagna, J. Bertherat, M. Buchfelder, A. Colao, A.R. Hermus, L.J. Hofland, A. Klibanski, A. Lacroix, J.R. Lindsay, J. Newell-Price, L.K. Nieman, S. Petersenn, N. Sonino, G.K. Stalla, B. Swearingen, M.L. Vance, J.A. Wass, M. Boscaro, Treatment of adrenocorticotropin-dependent Cushing’s syndrome: a consensus statement. J. Clin. Endocrinol. Metab. 93(7), 2454–2462 (2008)
R. Pivonello, M.C. De Martino, P. Cappabianca, M. De Leo, A. Faggiano, G. Lombardi, L.J. Hofland, S.W. Lamberts, A. Colao, The medical treatment of Cushing’s disease: effectiveness of chronic treatment with the dopamine agonist cabergoline in patients unsuccessfully treated by surgery. J. Clin. Endocrinol. Metab. 94(1), 223–230 (2009)
I. Shimon, L. Rot, E. Inbar, Pituitary-directed medical therapy with pasireotide for a corticotroph macroadenoma: pituitary volume reduction and literature review. Pituitary 15(4), 608–613 (2012)
C. Beglinger, K. Hu, Y. Wang, E. Bouillaud, C. Darstein, Y. Wang, P. Mohideen, Multiple once-daily subcutaneous doses of pasireotide were well tolerated in healthy male volunteers: a randomized, double-blind, placebo-controlled, cross-over, Phase I study. Endocrine 42(2), 366–374 (2012)
A. Colao, S. Petersenn, J. Newell-Price, J.W. Findling, F. Gu, M. Maldonado, U. Schoenherr, D. Mills, L.R. Salgado, B.M. Biller, A 12-month Phase 3 study of pasireotide in Cushing’s disease. N. Engl. J. Med. 366(10), 914–924 (2012)
R.A. Feelders, W.W. de Herder, S.J. Neggers, A.J. van der Lely, L.J. Hofland, Pasireotide, a multi-somatostatin receptor ligand with potential efficacy for treatment of pituitary and neuroendocrine tumors. Drugs Today (Barc.) 49(2), 89–103 (2013)
J. van der Hoek, S.W. Lamberts, L.J. Hofland, The role of somatostatin analogs in Cushing’s disease. Pituitary 7(4), 257–264 (2004)
L.J. Hofland, Somatostatin and somatostatin receptors in Cushing’s disease. Mol. Cell. Endocrinol. 286, 199–205 (2008)
A. Ben-Shlomo, H. Schmid, K. Wawrowsky, O. Pichurin, E. Hubina, V. Chesnokova, N.A. Liu, M. Culler, S. Melmed, Differential ligand-mediated pituitary somatostatin receptor subtype signaling: implications for corticotroph tumor therapy. J. Clin. Endocrinol. Metab. 94(11), 4342–4350 (2009)
F. Kelestimur, C. Utas, O. Ozbakir, A. Selçuklu, O. Kandemir, N. Ozcan, The effects of octreotide in a patient with Nelson’s syndrome. Postgrad. Med. J. 72(843), 53–54 (1996)
L.J. Hofland, S.W. Lamberts, R.A. Feelders, Role of somatostatin receptors in normal and tumoral pituitary corticotropic cells. Neuroendocrinology 92(Suppl 1), 11–16 (2010)
Arregger, A.L., Cardoso, E.M., Sandoval, O.B., Monardes Tumilasci, E.G., Sanchez, R., Contreras, L.N.: Hormonal secretion and quality of life in Nelson syndrome and Cushing disease after long acting repeatable octreotide: a short series and update. Am. J. Ther. (2012) (Epub ahead of print)
G.K. Stalla, S.J. Brockmeier, U. Renner, C. Newton, M. Buchfelder, J. Stalla, O.A. Muller, Octreotide exerts different effects in vivo and in vitro in Cushing’s disease. Eur. J. Endocrinol. 130, 125–131 (1994)
J. van der Hoek, M. Waaijers, P.M. van Koetsveld, D. Sprij-Mooij, R.A. Feelders, H.A. Schmid, P. Schoeffter, D. Hoyer, D. Cervia, J.E. Taylor, M.D. Culler, S.W. Lamberts, L.J. Hofland, Distinct functional properties of native somatostatin receptor subtype 5 compared with subtype 2 in the regulation of ACTH release by corticotroph tumor cells. Am. J. Physiol. Endocrinol. Metab. 289, 278–287 (2005)
C. de Bruin, R.A. Feelders, A.M. Waaijers, P.M. van Koetsveld, D.M. Sprij-Mooij, S.W. Lamberts, L.J. Hofland, Differential regulation of human dopamine D2 and somatostatin receptor subtype expression by glucocorticoids. J. Mol. Endocrinol. 42, 47–56 (2009)
F. Vignati, P. Loli, Additive effect of ketoconazole and octreotide in the treatment of severe adrenocorticotropin-dependent hypercortisolism. J. Clin. Endocrinol. Metab. 81(8), 2885–2890 (1996)
J.D. Carmichael, M. Fleseriu, Mifepristone: is there a place in the treatment of Cushing’s disease? Endocrine 44, 20–32 (2013)
G. Arnaldi, A. Angeli, A.B. Atkinson, X. Bertagna, F. Cavagnini, G.P. Chrousos, G.A. Fava, J.W. Findling, R.C. Gaillard, A.B. Grossman, B. Kola, A. Lacroix, T. Mancini, F. Mantero, J. Newell-Price, L.K. Nieman, N. Sonino, M.L. Vance, A. Giustina, M. Boscaro, Diagnosis and complications of Cushing’s syndrome: a consensus statement. J. Clin. Endocrinol. Metab. 88(12), 5593–5602 (2003)
A. Utz, B.M. Biller, The role of bilateral inferior petrosal sinus sampling in the diagnosis of Cushing’s syndrome. Arq. Bras. Endocrinol. Metabol. 51(8), 1329–1338 (2007)
L.K. Nieman, Update in the medical therapy of Cushing’s disease. Curr. Opin. Endocrinol. Diabetes Obes. 20(4), 330–334 (2013)
T. Tateno, M. Kato, Y. Tani, K. Oyama, S. Yamada, Y. Hirata, Differential expression of somatostatin and dopamine receptor subtype genes in adrenocorticotropin (ACTH)-secreting pituitary tumors and silent corticotroph adenomas. Endocr. J. 56(4), 579–584 (2009)
C. de Bruin, L.J. Hofland, L.K. Nieman, P.M. van Koetsveld, A.M. Waaijers, D.M. Sprij-Mooij, M. van Essen, S.W.J. Lamberts, W.W. de Herder, R.A. Feelders, Mifepristone effects on tumor somatostatin receptor expression in two patients with Cushing’s syndrome due to ectopic adrenocorticotropin secretion. J. Clin. Endocrinol. Metab. 97(2), 455–462 (2012)
van der Pas, R., Feelders, R.A., Gatto, F., de Bruin, C., Pereira, A.M., van Koetsveld, P.M., Sprij-Mooij, D.M., Waaijers, A.M., Dogan, F., Schulz, S., Kros, J.M., Lamberts, S.W.J., Hofland, L.J.: Preoperative normalization of cortisol levels in Cushing’s disease after medical treatment: consequences for somatostatin and dopamine receptor subtype expression and in vitro response to somatostatin analogs and dopamine agonists. J. Clin. Endocrinol. Metab. (2013) (Epub ahead of print)
B. Ambrosi, D. Bochicchio, C. Fadin, P. Colombo, G. Faglia, Failure of somatostatin and octreotide to acutely affect the hypothalamic–pituitary–adrenal function in patients with corticotropin hypersecretion. J. Endocrinol. Invest. 13, 257–261 (1990)
N.J. Woodhouse, S. Dagogo-Jack, M. Ahmed, R. Judzewitsch, Acute and long-term effects of octreotide in patients with ACTH-dependent Cushing’s syndrome. Am. J. Med. 95(3), 305–308 (1993)
X. Bertagna, C. Bertagna, M.H. Laudat, J.M. Husson, F. Girard, J.P. Luton, Pituitary–adrenal response to the antiglucocorticoid action of RU 486 in Cushing’s syndrome. J. Clin. Endocrinol. Metab. 63(3), 639–643 (1986)
S. Johanssen, B. Allolio, Mifepristone (RU 486) in Cushing’s syndrome. Eur. J. Endocrinol. 157, 561–569 (2007)
F. Castinetti, M. Fassnacht, S. Johanssen, M. Terzolo, P. Bouchard, P. Chanson, C. Do Cao, I. Morange, A. Pico, S. Ouzounian, J. Young, S. Hahner, T. Brue, B. Allolio, B. Conte-Devolx, Merits and pitfalls of mifepristone in Cushing’s syndrome. Eur. J. Endocrinol. 160, 1003–1010 (2009)
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ferrau, F., Trimarchi, F. & Cannavo, S. Adrenocorticotropin responsiveness to acute octreotide administration is not affected by mifepristone premedication in patients with Cushing’s disease. Endocrine 47, 550–556 (2014). https://doi.org/10.1007/s12020-013-0163-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-013-0163-0