Abstract
Background
This study was undertaken to determine the feasibility of an inpatient low-calorie program for a substantial decrease of preoperative weight (>10 points in BMI) in superobese patients.
Methods
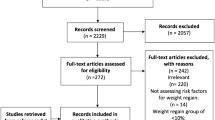
Five patients were hospitalized for an average of 11 weeks and were placed on a low-calorie liquid diet (<900 kcal/day) and an exercise program. Following a drop of ten points in BMI, they underwent a Roux-en-Y gastric bypass (RYGB). Hemoglobin A1c and lipid profiles were obtained at the beginning of the diet, prior to surgery and at the last follow-up appointment. Our results were compared to the National Surgical Quality Improvement Program (NSQIP) database, which included 1,046 bariatric operations performed at VA centers between October 1999 and August 2007.
Results
All five patients were massively obese men (body mass index (BMI) = 64.3 ± 2.1 kg/m2; 54.7 ± 2.6 years old; four of five were white) with multiple comorbid conditions, which placed them in a substantially higher risk for bariatric surgery. Of the four diabetic patients, two were insulin dependent. There was an average decrease in BMI by 12.7 points (85.8 ± 6.0 lb) during the preoperative diet period (11 weeks). All patients underwent RYGB without complications. This cohort of patients further decreased their BMI by 10.6 points (88.4 ± 29.4 lb) following surgical intervention. The total combined preoperative and postoperative excess body weight loss was 89% (10.6-month average follow-up). Sleep apnea resolved following gastric bypass but did not improve during the preoperative weight loss period. Hypertension, osteoarthritis, and dyslipidemia all improved following surgical intervention. Hemoglobin A1c decreased by 1.9% during diet-induced weight loss with no further improvement being noted after surgery. The two insulin-dependent diabetic patients discontinued insulin therapy following surgery. The NSQIP database contained 77 patients with similar characteristics to our cohort of patients. The 30-day mortality for this cohort of patients was 3.9% with a complication rate of 33.8%.
Conclusions
Massive preoperative weight loss is possible to achieve with a liquid protein diet in superobese patients greatly facilitating gastric bypass surgery in an otherwise high-risk patient population.



Similar content being viewed by others
References
Wang A, Kinsinger LS, Kahwati LC, et al. Obesity and weight control practices in 2000 among veterans using VA facilities. Obes Res. 2005;13:1405–11.
National Heart, Lung, and Blood Institute. Clinical guidelines on the identification, evaluation and treatment of overweight and obesity in adults: the evidence report. Washington, DC: National Heart, Lung and Blood Institute; 1998.
Livingston EH, Huerta S, Arthur D, et al. Male gender is a predictor of morbidity and age a predictor of mortality for patients undergoing gastric bypass surgery. Ann Surg. 2002;236:576–82.
Livingston EH, Arterburn D, Schifftner TL, et al. National surgical quality improvement program analysis of bariatric operations: modifiable risk factors contribute to bariatric surgical adverse outcomes. J Am Coll Surg. 2006;203:625–33.
Huerta S, Dredar S, Hayden E, et al. Preoperative weight loss decreases the operative time of gastric bypass at a Veterans Administration hospital. Obes Surg. 2008;18:508–12.
Alvarado R, Alami RS, Hsu G, et al. The impact of preoperative weight loss in patients undergoing laparoscopic Roux-en-Y gastric bypass. Obes Surg. 2005;15:1282–6.
Alami RS, Morton JM, Schuster R, et al. Is there a benefit to preoperative weight loss in gastric bypass patients? A prospective randomized trial. Surg Obes Relat Dis. 2007;3:141–5.
Huerta S, Kohan D, Siddiqui A, et al. Assessment of comorbid conditions in veteran patients after Roux-en-Y gastric bypass. Am J Surg. 2007;194:48–52.
Buchwald H. Bariatric surgery for morbid obesity: health implications for patients, health professionals, and third-party payers. J Am Coll Surg. 2005;200:593–604.
Maggard MA, Shugarman LR, Suttorp M, et al. Meta-analysis: surgical treatment of obesity. Ann Intern Med. 2005;142:547–59.
Pories WJ, Swanson MS, MacDonald KG, et al. Who would have thought it? An operation proves to be the most effective therapy for adult-onset diabetes mellitus. Ann Surg. 1995;222:339–50.
Alexandrides TK, Skroubis G, Kalfarentzos F. Resolution of diabetes mellitus and metabolic syndrome following Roux-en-Y gastric bypass and a variant of biliopancreatic diversion in patients with morbid obesity. Obes Surg. 2007;17:176–84.
Anvari M. Is type 2 diabetes a surgical disease? Can J Surg. 2007;50:249–50.
Camastra S, Manco M, Mari A, et al. Beta-cell function in severely obese type 2 diabetic patients: long-term effects of bariatric surgery. Diabetes Care. 2007;30:1002–4.
Cohen RV, Schiavon CA, Pinheiro JS, et al. Duodenal-jejunal bypass for the treatment of type 2 diabetes in patients with body mass index of 22–34 kg/m2: a report of 2 cases. Surg Obes Relat Dis. 2007;3:195–7.
Cummings DE, Flum DR. Gastrointestinal surgery as a treatment for diabetes. JAMA. 2008;299:341–3.
Dixon JB, O'Brien PE, Playfair J, et al. Adjustable gastric banding and conventional therapy for type 2 diabetes: a randomized controlled trial. JAMA. 2008;299:316–23.
Ferchak CV, Meneghini LF. Obesity, bariatric surgery and type 2 diabetes—a systematic review. Diabetes Metab Res Rev. 2004;20:438–45.
Gan SS, Talbot ML, Jorgensen JO. Efficacy of surgery in the management of obesity-related type 2 diabetes mellitus. ANZ J Surg. 2007;77:958–62.
Levy P, Fried M, Santini F, Finer N. The comparative effects of bariatric surgery on weight and type 2 diabetes. Obes Surg. 2007;17:1248–56.
Meneghini LF. Impact of bariatric surgery on type 2 diabetes. Cell Biochem Biophys. 2007;48:97–102.
Pories WJ. Diabetes: the evolution of a new paradigm. Ann Surg. 2004;239:12–3.
Rosa G, Mingrone G, Manco M, et al. Molecular mechanisms of diabetes reversibility after bariatric surgery. Int J Obes (Lond). 2007;31:1429–36.
Rubino F, Gagner M. Potential of surgery for curing type 2 diabetes mellitus. Ann Surg. 2002;236:554–9.
Rubino F. Bariatric surgery: effects on glucose homeostasis. Curr Opin Clin Nutr Metab Care. 2006;9:497–507.
Knowler WC, Barrett-Connor E, Fowler SE, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med. 2002;346:393–403.
Unger RH. Reinventing type 2 diabetes: pathogenesis, treatment, and prevention. JAMA. 2008;299:1185–7.
Acknowledgements
This pilot study undertook a great deal of effort by a number of individuals who in addition to their routine busy activities took time to assist with the program. The authors specially acknowledge the participation and help of: Elizabeth Hayden, MS/RD; David Hales, MD; Theresa Hale, Ph.D.; Daniel Villarreal, PA; Emily Armour-Serold, PA; Wanda Frey, RN; Catherine Gordon, MD; Rhonda Harmon, MD; Ali Siddiqui, MD; and KC Murphy.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Huerta, S., Li, Z., Anthony, T. et al. Feasibility of a Supervised Inpatient Low-Calorie Diet Program for Massive Weight Loss Prior to RYGB in Superobese Patients. OBES SURG 20, 173–180 (2010). https://doi.org/10.1007/s11695-009-0001-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-009-0001-x