Background
Obesity and obesity-associated type 2 diabetes mellitus (T2DM) are frequently related to a low-grade chronic inflammatory state, which increases the risk of developing cardiovascular diseases. The aim of the present work was to evaluate the effect of obesity and T2DM on the concentrations of pro-inflammatory factors and to study the effect of weight loss after Roux-en-Y gastric bypass (RYGBP).
Methods
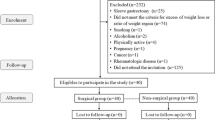
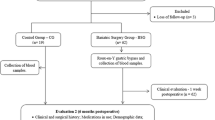
Plasma concentrations of monocyte chemoattractant protein-1 (MCP-1), tumor necrosis factor-α (TNF-α), serum amyloid A (SAA) and sialic acid (SA) were measured in 25 female volunteers. The concentrations of these cytokines were determined in 14 female obese patients before and after weight loss following RYGBP. Additionally, visceral adipose tissue (VAT) obtained from 15 females was used to quantify expression levels of MCP-1 and CD68 by Real-Time PCR.
Results
Both obese normoglycemic (NG) and T2DM groups exhibited significantly higher MCP-1 (P < 0.05), TNF-α (P < 0.01), SAA (P < 0.05) and SA (P < 0.05) concentrations, compared to the lean group. No differences were found between obese NG and obese T2DM subjects. A significant positive correlation was found between body fat percentage (BF) and all inflammatory markers (P < 0.05) studied. MCP-1 expression levels in VAT were upregulated in obese NG (P = 0.008) and obese T2DM (P = 0.032) patients compared to lean subjects, but no additional detrimental effect of T2DM was observed between both obese groups. After weight loss, SAA (P < 0.001) and SA (P < 0.05) concentrations diminished, whereas circulating levels of MCP-1 showed a tendency to decrease (P = 0.093) and TNF-α did not change.
Conclusion
The present findings suggest that elevated pro-inflammatory cytokine levels found in obese patients relate mainly to obesity rather than to T2DM. Moreover, surgery-induced weight loss reduces circulating concentrations of key pro-inflammatory factors, which contribute to the improvement in the cardiovascular co-morbidity following excess weight loss.
Similar content being viewed by others
References
Wellen KE, Hotamisligil GS. Inflammation, stress, and diabetes. J Clin Invest 2005; 115: 1111–9.
Hotamisligil GS. Inflammation and metabolic disorders. Nature 2006; 444: 860–7.
Despres JP, Lemieux I. Abdominal obesity and metabolic syndrome. Nature 2006; 444: 881–7.
Guzik TJ, Mangalat D, Korbut R. Adipocytokines - novel link between inflammation and vascular function? J Physiol Pharmacol 2006; 57: 505–28.
Van Gaal LF, Mertens IL, De Block CE. Mechanisms linking obesity with cardiovascular disease. Nature 2006; 444: 875–80.
Fantuzzi G, Mazzone T. Adipose tissue and atherosclerosis: exploring the connection. Arterioscler Thromb Vasc Biol 2007; 27: 996–1003.
Ritchie SA, Connell JM. The link between abdominal obesity, metabolic syndrome and cardiovascular disease. Nutr Metab Cardiovasc Dis 2007; 17: 319–26.
Trayhurn P, Wood IS. Signalling role of adipose tissue: adipokines and inflammation in obesity. Biochem Soc Trans 2005; 33: 1078–81.
Visser M, Bouter LM, McQuillan GM et al. Elevated C-reactive protein levels in overweight and obese adults. JAMA 1999; 282: 2131–5.
Sartipy P, Loskutoff DJ. Monocyte chemoattractant protein 1 in obesity and insulin resistance. Proc Natl Acad Sci USA 2003; 100: 7265–70.
Hotamisligil GS, Shargill NS, Spiegelman BM. Adipose expression of tumor necrosis factor-α: direct role in obesity-linked insulin resistance. Science 1993; 259: 87–91.
Kern PA, Ranganathan S, Li C et al. Adipose tissue tumor necrosis factor and interleukin-6 expression in human obesity and insulin resistance. Am J Physiol Endocrinol Metab 2001; 280: E745–51.
Gómez-Ambrosi J, Salvador J, Rotellar F et al. Increased serum amyloid A concentrations in morbid obesity decrease after gastric bypass. Obes Surg 2006; 16: 262–9.
Bastard JP, Jardel C, Bruckert E et al. Elevated levels of interleukin 6 are reduced in serum and subcutaneous adipose tissue of obese women after weight loss. J Clin Endocrinol Metab 2000; 85: 3338–42.
Cottam DR, Mattar SG, Barinas-Mitchell E, et al. The chronic inflammatory hypothesis for the morbidity associated with morbid obesity: implications and effects of weight loss. Obes Surg 2004; 14: 589–600.
Clement K, Viguerie N, Poitou C et al. Weight loss regulates inflammation-related genes in white adipose tissue of obese subjects. FASEB J 2004; 18: 1657–69.
Ryan AS, Nicklas BJ. Reductions in plasma cytokine levels with weight loss improve insulin sensitivity in overweight and obese postmenopausal women. Diabetes Care 2004; 27: 1699–705.
Vazquez LA, Pazos F, Berrazueta JR et al. Effects of changes in body weight and insulin resistance on inflammation and endothelial function in morbid obesity after bariatric surgery. J Clin Endocrinol Metab 2005; 90: 316–22.
Cancello R, Henegar C, Viguerie N et al. Reduction of macrophage infiltration and chemoattractant gene expression changes in white adipose tissue of morbidly obese subjects after surgery-induced weight loss. Diabetes 2005; 54: 2277–86.
Fried SK, Bunkin DA, Greenberg AS. Omental and subcutaneous adipose tissues of obese subjects release interleukin-6: depot difference and regulation by glucocorticoid. J Clin Endocrinol Metab 1998; 83: 847–50.
Bruun JM, Lihn AS, Madan AK et al. Higher production of IL-8 in visceral vs. subcutaneous adipose tissue. Implication of nonadipose cells in adipose tissue. Am J Physiol Endocrinol Metab 2004; 286: E8–13.
Lihn AS, Bruun JM, He G et al. Lower expression of adiponectin mRNA in visceral adipose tissue in lean and obese subjects. Mol Cell Endocrinol 2004; 219: 9–15.
Neels JG, Olefsky JM. Inflamed fat: what starts the fire? J Clin Invest 2006; 116: 33–5.
Muller S, Martin S, Koenig W et al. Impaired glucose tolerance is associated with increased serum concentrations of interleukin 6 and co-regulated acute-phase proteins but not TNF-α or its receptors. Diabetologia 2002; 45: 805–12.
Bruun JM, Verdich C, Toubro S et al. Association between measures of insulin sensitivity and circulating levels of interleukin-8, interleukin-6 and tumor necrosis factor-α. Effect of weight loss in obese men. Eur J Endocrinol 2003; 148: 535–42.
Das SK, Roberts SB, Kehayias JJ et al. Body composition assessment in extreme obesity and after massive weight loss induced by gastric bypass surgery. Am J Physiol Endocrinol Metab 2003; 284: E1080–8.
Matthews DR, Hosker JP, Rudenski AS et al. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 1985; 28: 412–9.
Katz A, Nambi SS, Mather K et al. Quantitative insulin sensitivity check index: a simple, accurate method for assessing insulin sensitivity in humans. J Clin Endocrinol Metab 2000; 85: 2402–10.
Gómez-Ambrosi J, Catalán V, Diez-Caballero A et al. Gene expression profile of omental adipose tissue in human obesity. FASEB J 2004; 18: 215–7.
Catalán V, Gómez-Ambrosi J, Rotellar F et al. The obestatin receptor (GPR39) is expressed in human adipose tissue and is down-regulated in obesity-associated type 2 diabetes mellitus. Clin Endocrinol 2007; 66: 598–601.
Cottam DR, Mattar SG, Barinas-Mitchell E et al. The chronic inflammatory hypothesis for the morbidity associated with morbid obesity: implications and effects of weight loss. Obes Surg 2004; 14: 589–600.
Frühbeck G, Salvador J. Role of adipocytokines in metabolism and disease. Nutr Res 2004; 24: 803–26.
Browning LM, Jebb SA, Mishra G et al. Elevated sialic acid, but not CRP, predicts features of the metabolic syndrome independently of BMI in women. Int J Obes 2004; 28: 1004–10.
Yang RZ, Lee MJ, Hu H et al. Acute-phase serum amyloid A: an inflammatory adipokine and potential link between obesity and its metabolic complications. PLoS Med 2006; 3: e287.
Shoelson SE, Herrero L, Naaz A. Obesity, inflammation, and insulin resistance. Gastroenterology 2007; 132: 2169–80.
Frühbeck G. Screening and interventions for obesity in adults. Ann Intern Med 2004; 141: 245–6.
Herder C, Muller-Scholze S, Rating P et al. Systemic monocyte chemoattractant protein-1 concentrations are independent of type 2 diabetes or parameters of obesity: results from the Cooperative Health Research in the Region of Augsburg Survey S4 (KORA S4). Eur J Endocrinol 2006; 154: 311–7.
Zietz B, Buchler C, Herfarth H et al. Caucasian patients with type 2 diabetes mellitus have elevated levels of monocyte chemoattractant protein-1 that are not influenced by the -2518 A–G promoter polymorphism. Diabetes Obes Metab 2005; 7: 570–8.
Hotamisligil GS, Arner P, Caro JF et al. Increased adipose tissue expression of tumor necrosis factor-α in human obesity and insulin resistance. J Clin Invest 1995; 95: 2409–15.
Katsuki A, Sumida Y, Murashima S et al. Serun levels of tumor necrosis- are increased in obese patients with noninsulin-dependent diabetes mellitus. J Clin Endocrinol Metab 1998; 83: 859–62.
Muller S, Martin S, Koenig W et al. Impaired glucose tolerance is associated with increased serum concentrations of interleukin 6 and co-regulated acute-phase proteins but not TNF-α or its receptors. Diabetologia 2002; 45: 805–12.
Dominguez H, Storgaard H, Rask-Madsen C et al. Metabolic and vascular effects of tumor necrosis factor-α blockade with etanercept in obese patients with type 2 diabetes. J Vasc Res 2005; 42: 517–25.
Englyst NA, Crook MA, Lumb P et al. Percentage of body fat and plasma glucose predict plasma sialic acid concentration in type 2 diabetes mellitus. Metabolism 2006; 55: 1165–70.
Bruun JM, Lihn AS, Pedersen SB et al. Monocyte chemoattractant protein-1 release is higher in visceral than subcutaneous human adipose tissue (AT): implication of macrophages resident in the AT. J Clin Endocrinol Metab 2005;90: 2282–9.
Christiansen T, Richelsen B, Bruun JM. Monocyte chemoattractant protein-1 is produced in isolated adipocytes, associated with adiposity and reduced after weight loss in morbid obese subjects. Int J Obes 2005; 29: 146–50.
Chacon MR, Fernández-Real JM, Richart C et al. Monocyte chemoattractant protein-1 in obesity and type 2 diabetes. Insulin sensitivity study. Obesity 2007; 15: 664–72.
Dahlman I, Kaaman M, Olsson T et al. A unique role of monocyte chemoattractant protein 1 among chemokines in adipose tissue of obese subjects. J Clin Endocrinol Metab 2005; 90: 5834–40.
Patriti A, Facchiano E, Sanna A et al. The enteroinsular axis and the recovery from type 2 diabetes after bariatric surgery. Obes Surg 2004; 14: 840–8.
Mathier MA, Ramanathan RC. Impact of obesity and bariatric surgery on cardiovascular disease. Med Clin North Am 2007; 91: 415–31.
Vazquez LA, Pazos F, Berrazueta JR et al. Effects of changes in body weight and insulin resistance on inflammation and endothelial function in morbid obesity after bariatric surgery. J Clin Endocrinol Metab 2005; 90: 316–22.
Dandona P, Weinstock R, Thusu K et al. Tumor necrosis factor-α in sera of obese patients: fall with weight loss. J Clin Endocrinol Metab 1998; 83: 2907–10.
Ziccardi P, Nappo F, Giugliano G et al. Reduction of inflammatory cytokine concentrations and improvement of endothelial functions in obese women after weight loss over one year. Circulation 2002; 105: 804–9.
Laimer M, Ebenbichler CF, Kaser S et al Markers of chronic inflammation and obesity: a prospective study on the reversibility of this association in middle-aged women undergoing weight loss by surgical intervention. Int J Obes 2002; 26: 659–62.
Kopp HP, Kopp CW, Festa A et al. Impact of weight loss on inflammatory proteins and their association with the insulin resistance syndrome in morbidly obese patients Arterioscler Thromb Vasc Biol 2003; 23: 1042–7.
Manco M, Fernández-Real JM, Equitani F et al. Effect of massive weight loss on inflammatory adipocytokines and the innate immune system in morbidly obese women. J Clin Endocrinol Metab 2007; 92: 483–90.
Havel PJ. Update on adipocyte hormones: regulation of energy balance and carbohydrate/lipid metabolism. Diabetes 2004; 53: S143–S151.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Catalán, V., Gómez-Ambrosi, J., Ramirez, B. et al. Proinflammatory Cytokines in Obesity: Impact of Type 2 Diabetes Mellitus and Gastric Bypass. OBES SURG 17, 1464–1474 (2007). https://doi.org/10.1007/s11695-008-9424-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-008-9424-z