Background
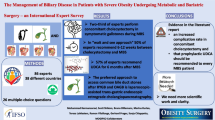
Binge-eating disorder (BED) may be associated with unsatisfactory weight loss in obese patients submitted to bariatric procedures.This study aims to investigate whether the presence of binge eating before Roux-en-Y gastric bypass (RYGBP) influences weight outcomes.
Methods
In a prospective design, 216 obese patients (37 males, 178 females, BMI––5.9 ±–.0 kg/m2) were assessed for the lifetime prevalence of BED and classified at structured interview into 3 subgroups: no binge eating (NBE––3), sub-threshold binge eating (SBE––29), and binge-eating disorder (BED––4). All patients were encouraged to take part in a multidisciplinary program following surgery, and weight loss at follow-up was used as the outcome variable.
Results
At 1-year follow-up, NBE patients (n––1) showed percent excess BMI loss (%EBL) significantly higher than SBE patients (n––12) (P––.027), although this effect was not significantly different between NBE and BED patients (n––4). At 2-year follow-up, NBE patients (n––3) showed %EBL higher than SBE (n––4) (P––.003) and BED patients (n––4) (P–lt;–.001). Nevertheless, we found no significant weight loss differences between SBE (subclinical) and BED (full criteria) patients at any period of followup. Preliminary results at 3-year follow-up suggest that such an effect may be enduring.
Conclusion
The presence of a history of binge eating prior to treatment is associated with poorer weight loss in obese patients submitted to RYGBP. Because BED is highly prevalent in obese patients seeking bariatric surgery, its early recognition and treatment may be of important clinical value.
Similar content being viewed by others
References
Stunkard AJ. Eating patterns and obesity. Psych Quarterly 1959; 33: 284–5.
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 4th edn. Washington 1994: 729–1.
Dymek-Valentine M, Rienecke-Hoste R, Alverdy J. Assessment of binge eating disorder in morbidly obese patients evaluated for gastric bypass: SCID versus QEWP-R. Eat Weight Disord 2004; 9: 211–.
Adami GF, Gandolfo P, Bauer B et al. Binge eating in massively obese patients undergoing bariatric surgery. Int J Eat Disord 1995; 17: 45–0.
Powers PS, Perez A, Boyd F et al. Eating pathology before and after bariatric surgery: a prospective study. Int J Eat Disord 1999; 25: 293–00.
Saunders R. Binge eating in gastric bypass patients before surgery. Obes Surg 1999; 9: 72–.
Lang T, Hauser R, Buddeberg C et al. Impact of gastric banding on eating behavior and weight. Obes Surg 2002; 12: 100–.
Striegel-Moore RH, Franko DL. Epidemiology of binge eating disorder. Int J Eat Disord 2003; 34: S19–S29.
Hsu LKG, Benotti PN, Dwyer J et al. Nonsurgical factors that influence the outcome of bariatric surgery: a review. Psychosom Med 1998; 60: 338–6.
Saunders R. “Grazing– a high-risk behavior. Obes Surg 2004; 14: 98–02.
van Hout GCM, Verschure SKM, van Heck GL. Psychosocial predictors of success following bariatric surgery. Obes Surg 2005; 15: 552–0.
Guisado Macias JA, Vaz Leal FJ. Psychopathological differences between morbidly obese binge eaters and non-binge eaters after bariatric surgery. Eat Weight Disord 2003; 8: 315–.
Green AE, Dymek-Valentine M, Pytluk S et al. Psychosocial outcome of gastric bypass surgery for patients with and without binge eating. Obes Surg 2004; 14: 975–5.
Pekkarinen T, Koskela K, Huikuri K et al. Long-term results of gastroplasty for morbid obesity: Binge-eating as a predictor of poor outcome. Obes Surg 1994; 4: 248–5.
Kalarchian MA, Marcus MD, Wilson GT et al. Binge eating among gastric bypass patients at long-term follow-up. Obes Surg 2002; 12: 270–.
Larsen JK, van Ramshorst B, Geenen R et al. Binge eating and its relationship to outcome after laparoscopic adjustable gastric banding. Obes Surg 2004; 14: 1111–.
Busetto L, Segato G, De Marchi F et al. Outcome predictors in morbidly obese recipients of an adjustable gastric band. Obes Surg 2002; 12: 83–2.
Burgmer R, Grigutsch K, Zipfel S et al. The influence of eating behavior and eating pathology on weight loss after gastric restriction operations. Obes Surg 2005; 15: 684–1.
Bocchieri-Ricciardi LE, Chen EY, Munoz D et al. Pre-surgery binge eating status: effect on eating behavior and weight outcome after gastric bypass. Obes Surg 2006; 16: 1198–04.
Cooper PJ, Taylor M, Cooper Z et al. The development and validation of the body shape questionnaire. Int J Eat Dis 1987; 6: 485–4.
Beck AT, Ward CH, Mendelson M et al. Inventory for measuring depression. Arch Gen Psychiatr 1961; 4: 53–3.
Hamilton, M. The assessment of anxiety states by rating. Br J Med Psychol 1959; 32: 50–.
First MB, Spitzer RL, Gibbon M et al. Structured Clinical Interview for DSM-IV Axis I Disorders, Patient Edition (SCID-P), version 2. New York State Psychiatric Institute, Biometric Research 1996.
Deitel M, Greenstein RJ. Recommendations for reporting weight loss. Obes Surg 2003; 13: 159–0.
Yanovski SZ, Nelson JE, Dubbert BK et al. Association of binge eating disorder and psychiatric comorbidity in obese subjects. Am J Psychiatry 1993; 150: 1472–.
Bulik CM, Sullivan PF, Kendler KS. Medical and psychiatric morbidity in obese women with and without binge eating. Int J Eat Disord 2002; 32: 72–.
Stunkard AJ, Allison KC. Binge eating disorder: disorder or marker? Int J Eat Disord 2003; 34: S107–S116.
Greenberg I, Perna F, Kaplan M et al. Behavioral and psychological factors in the assessment and treatment of obesity surgery patients. Obes Res 2005; 13: 244–.
Dixon JB, Dixon ME, O’Brien PE. Depression in association with severe obesity: Changes with weight loss. Arch Intern Med 2003; 163: 2058–5.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sallet, P.C., Sallet, J.A., Dixon, J.B. et al. Eating Behavior as a Prognostic Factor for Weight Loss after Gastric Bypass. OBES SURG 17, 445–451 (2007). https://doi.org/10.1007/s11695-007-9077-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-007-9077-3