Abstract
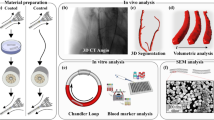
Subacute stent thrombosis, caused by undesired interactions between blood and the stent surface, is a major concern in the first few weeks following coronary artery stent implantation. The aim of this study was to establish a novel in vitro model for hemocompatibility testing of coronary artery stents according to ISO 10993-4. The model consists of a modified Chandler-Loop design with closed heparin-coated PVC Loops and a thermostated water bath. The tests were performed with anticoagulated human whole blood. After incubation in the loop, blood was analyzed for coagulation and inflammatory activation markers (TAT, β-TG, sP-selectin, SC5b-9 and PMN-elastase). Three different stent types with varying thrombogenicity were tested; statistically significant differences were found between the three stent types in measures of coagulation and platelet activation. The new Chandler-Loop model can be used as an alternative to animal and current in vitro models, especially for the determination of early events after stent implantation.






Similar content being viewed by others
References
Sigwart U, Puel J, Mirkovitch V, Joffre F, Kappenberger L. Intravascular stents to prevent occlusion and restenosis after transluminal angioplasty. N Engl J Med. 1987;316(12):701–6.
Thierry B, Merhi Y, Bilodeau L, Trepanier C, Tabrizian M. Nitinol versus stainless steel stents: acute thrombogenicity study in an ex vivo porcine model. Biomaterials. 2002;23(14):2997–3005.
Mrowietz C, Franke RP, Seyfert UT, Park JW, Jung F. Haemocompatibility of polymer-coated stainless steel stents as compared to uncoated stents. Clin Hemorheol Microcirc. 2005;32(2):89–103.
Arab D, Lewis B, Cho L, Steen L, Joyal D, Leya F. Antiplatelet therapy in anticoagulated patients requiring coronary intervention. J Invasive Cardiol. 2005;17(10):549–54.
Romano A, Jensen MR, McAlpine J. Toward the optimization of stent-based treatment for coronary artery disease. Curr Opin Drug Discov Devel. 2010;13(2):157–8.
Serruys PW, Strauss BH, Beatt KJ, Bertrand ME, Puel J, Rickards AF, et al. Angiographic follow-up after placement of a self-expanding coronary-artery stent. N Engl J Med. 1991;324(1):13–7.
Serruys PW, Di MC. Who was thrombogenic: the stent or the doctor? Circulation. 1995;91(6):1891–3.
Tamberella MR, Furman MI. The role of platelet inhibition in the drug-eluting stent era. Coron Artery Dis. 2004;15(6):327–9.
Palmaz JC. The 2001 Charles T. Dotter lecture: understanding vascular devices at the molecular level is the key to progress. J Vasc Interv Radiol. 2001;12(7):789–94.
Palmaz JC. Bring that pioneering spirit back! A 25-year perspective on the vascular stent. Cardiovasc Intervent Radiol. 2007;30(6):1095–8.
Davis C, Fischer J, Ley K, Sarembock IJ. The role of inflammation in vascular injury and repair. J Thromb Haemost. 2003;1(8):1699–709.
Chandler AB. In vitro thrombotic coagulation of the blood; a method for producing a thrombus. Lab Invest. 1958;7(2):110–4.
Song W, Lee J, Kim H, Shin J, Oh D, Tio F, et al. A new percutaneous porcine coronary model of chronic total occlusion. J Invasive Cardiol. 2005;17(9):452–4.
Tanigawa N, Sawada S, Kobayashi M. Reaction of the aortic wall to six metallic stent materials. Acad Radiol. 1995;2(5):379–84.
Kaminska M, Okroj W, Szymanski W, Jakubowski W, Komorowski P, Nosal A, et al. Interaction of parylene C with biological objects. Acta Bioeng Biomech. 2009;11(3):19–25.
Seyfert UT, Perkins S, Kummel M. Hemocompatibility testing of polymers. Beitr Infusionsther Transfusionsmed. 1996;33:241–6.
Seyfert UT, Biehl V, Schenk J. In vitro hemocompatibility testing of biomaterials according to the ISO 10993-4. Biomol Eng. 2002;19(2–6):91–6.
Szapary L, Bagoly E, Kover F, Feher G, Pozsgai E, Koltai K, et al. The effect of carotid stenting on rheological parameters, free radical production and platelet aggregation. Clin Hemorheol Microcirc. 2009;43(3):209–17.
Gupta V, Aravamuthan BR, Baskerville S, Smith SK, Gupta V, Lauer MA, et al. Reduction of subacute stent thrombosis (SAT) using heparin-coated stents in a large-scale, real world registry. J Invasive Cardiol. 2004;16(6):304–10.
Beythien C, Gutensohn K, Bau J, Hamm CW, Kuhnl P, Meinertz T, et al. Influence of stent length and heparin coating on platelet activation: a flow cytometric analysis in a pulsed floating model. Thromb Res. 1999;94(2):79–86.
Gemmell CH. Activation of platelets by in vitro whole blood contact with materials: increases in microparticle, procoagulant activity, and soluble P-selectin blood levels. J Biomater Sci Polym Ed. 2001;12(8):933–43.
Inoue T, Hikichi Y, Morooka T, Yoshida K, Fujimatsu D, Komoda H, et al. Comparison of changes in circulating platelet-derived microparticles and platelet surface P-selectin expression after coronary stent implantation. Platelets. 2006;17(6):416–20.
Tylman M, Bengtson JP, Bengtsson A. Activation of the complement system by different autologous transfusion devices: an in vitro study. Transfusion. 2003;43(3):395–9.
Beythien C, Terres W, Hamm CW. In vitro model to test the thrombogenicity of coronary stents. Thromb Res. 1994;75(6):581–90.
Hong J, Nilsson EK, Reynolds H, Larsson R, Nilsson B. A new in vitro model to study interaction between whole blood and biomaterials. Studies of platelet and coagulation activation and the effect of aspirin. Biomaterials. 1999;20(7):603–11.
Tu Q, Zhao Y, Xue X, Wang J, Huang N (2010) Improved endothelialization of titanium vascular implants by extracellular matrix secreted from endothelial cells. Tissue Eng A. 16(12):3635–45.
Acknowledgments
The authors thank Karl-Heinz Hellmer for the excellent support during the SEM procedures. Tests and stent delivery systems were sponsored by Boston Scientific Corporation, Natick, MA, USA. Furthermore the authors thank Barbara A. Huibregtse and Michael J. Eppihimer (Boston Scientific Corporation, Pre-clinical department, 1 Boston Scientific Place, Natick, MA 01760 USA), Kristin L. Hood (Boston Scientific Corporation, Scientific communications, 100 Boston Scientific Way, Marlborough, MA 01752-1234 USA) and Nic Van Dyck (Boston Scientific Corporation, Clinical department, Gaetano Martinolaan 50, 6229 GS Maastricht Netherlands) for their valuable work of reviewing the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sinn, S., Scheuermann, T., Deichelbohrer, S. et al. A novel in vitro model for preclinical testing of the hemocompatibility of intravascular stents according to ISO 10993-4. J Mater Sci: Mater Med 22, 1521–1528 (2011). https://doi.org/10.1007/s10856-011-4335-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10856-011-4335-2