Abstract
Purpose
To investigate the protective mechanisms of an 85 % pure extract of (−) epigallocatechin gallate (EGCG) in the development of fibrosis, oxidative stress and inflammation in a recently developed dietary-induced animal model of non-alcoholic fatty liver disease (NAFLD).
Methods
Female Sprague–Dawley rats were fed with either normal rat diet or high-fat diet for 8 weeks to develop NAFLD. For both treatments, rats were treated with or without EGCG (50 mg/kg, i.p. injection, 3 times per week). At the end, blood and liver tissue samples were obtained for histology, molecular, and biochemical analyses.
Results
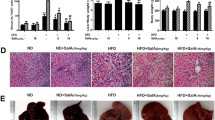
Non-alcoholic fatty liver disease (NAFLD) rats showed significant amount of fatty infiltration, necrosis, fibrosis, and inflammation. This was accompanied by a significant expressional increase in markers for fibrosis, oxidative stress, and inflammation. TGF/SMAD, PI3 K/Akt/FoxO1, and NF-κB pathways were also activated. Treatment with EGCG improved hepatic histology (decreased number of fatty score, necrosis, and inflammatory foci), reduced liver injury (from ~0.5 to ~0.3 of ALT/AST ratio), attenuated hepatic changes including fibrosis (reduction in Sirius Red and synaptophysin-positive stain) with down-regulation in the expressions of key pathological oxidative (e.g. nitrotyrosine formation) and pro-inflammatory markers (e.g. iNOS, COX-2, and TNF-α). EGCG treatment also counteracted the activity of TGF/SMAD, PI3 K/Akt/FoxO1, and NF-κB pathways. Treatment with EGCG did not affect the healthy rats.
Conclusions
Epigallocatechin gallate (EGCG) reduced the severity of liver injury in an experimental model of NAFLD associated with lower concentration of pro-fibrogenic, oxidative stress, and pro-inflammatory mediators partly through modulating the activities of TGF/SMAD, PI3 K/Akt/FoxO1, and NF-κB pathways. Therefore, green tea polyphenols and EGCG are useful supplements in the prevention of NAFLD.







Similar content being viewed by others
References
Harrison SA, Day CP (2007) Benefits of lifestyle modification in NAFLD. Gut 56:1760–1769
Mendez-Sanchez N, Arrese M, Zamora-Valdes D, Uribe M (2007) Treating nonalcoholic fatty liver disease. Liver int 27:1157–1165
Selmi C, Bowlus CL, Keen CL, Gershwin ME (2007) Non-alcoholic fatty liver disease: the new epidemic and the need for novel nutritional approaches. J Med Food 10:563–565
Yoneda M, Endo H, Nozaki Y, Tomimoto A, Fujisawa T, Fujita K, Yoneda K, Takahashi H, Saito S, Iwasaki T, Yamamoto S, Tsutsumi S, Aburatani H, Wada K, Hotta K, Nakajima A (2007) Life style-related diseases of the digestive system: gene expression in nonalcoholic steatohepatitis patients and treatment strategies. J Pharmacol Sci 105:151–156
Pitt HA (2007) Hepato-pancreato-biliary fat: the good, the bad and the ugly. HPB 9:92–97
Krasnoff JB, Painter PL, Wallace JP, Bass NM, Merriman RB (2008) Health-related fitness and physical activity in patients with nonalcoholic fatty liver disease. Hepatology (Baltimore, MD) 47:1158–1166
McCullough AJ (2006) Pathophysiology of nonalcoholic steatohepatitis. J Clin Gastroenterol 40(Suppl 1):S17–S29
French SW, Takahashi H, Wong K, Mendenhall CL (1991) Ito cell activation induced by chronic ethanol feeding in the presence of different dietary fats. Alcohol Alcohol Suppl 1:357–361
Nanji AA (2004) Role of different dietary fatty acids in the pathogenesis of experimental alcoholic liver disease. Alcohol 34:21–25
Lieber CS, Leo MA, Mak KM, Xu Y, Cao Q, Ren C, Ponomarenko A, DeCarli LM (2004) Model of nonalcoholic steatohepatitis. Am J Clin Nutr 79:502–509
Zou Y, Li J, Lu C, Wang J, Ge J, Huang Y, Zhang L, Wang Y (2006) High-fat emulsion-induced rat model of nonalcoholic steatohepatitis. Life Sci 79:1100–1107
Xiao J, Ching YP, Liong EC, Nanji AA, Fung ML, Tipoe GL (2012) Garlic-derived S-allylmercaptocysteine is a hepato-protective agent in non-alcoholic fatty liver disease in vivo animal model. Eur J Nutr. doi:10.1007/s00394-012-0301-0
Tipoe GL, Ho CT, Liong EC, Leung TM, Lau TY, Fung ML, Nanji AA (2009) Voluntary oral feeding of rats not requiring a very high fat diet is a clinically relevant animal model of non-alcoholic fatty liver disease (NAFLD). Histol Histopathol 24:1161–1169
Higdon JV, Frei B (2003) Tea catechins and polyphenols: health effects, metabolism, and antioxidant functions. Crit Rev Food Sci Nutr 43:89–143
Singh BN, Shankar S, Srivastava RK (2011) Green tea catechin, epigallocatechin-3-gallate (EGCG): mechanisms, perspectives and clinical applications. Biochem Pharmacol 82:1807–1821
Tipoe GL, Leung TM, Hung MW, Fung ML (2007) Green tea polyphenols as an anti-oxidant and anti-inflammatory agent for cardiovascular protection. Cardiovasc Hematol Disord: Drug Targets 7:135–144
Khan N, Afaq F, Saleem M, Ahmad N, Mukhtar H (2006) Targeting multiple signaling pathways by green tea polyphenol (−)-epigallocatechin-3-gallate. Cancer Res 66:2500–2505
Bruno RS, Dugan CE, Smyth JA, DiNatale DA, Koo SI (2008) Green tea extract protects leptin-deficient, spontaneously obese mice from hepatic steatosis and injury. J Nutr 138:323–331
Fu Y, Zheng S, Lu SC, Chen A (2008) Epigallocatechin-3-gallate inhibits growth of activated hepatic stellate cells by enhancing the capacity of glutathione synthesis. Mol Pharmacol 73:1465–1473
Kuzu N, Bahcecioglu IH, Dagli AF, Ozercan IH, Ustundag B, Sahin K (2008) Epigallocatechin gallate attenuates experimental non-alcoholic steatohepatitis induced by high fat diet. J Gastroenterol Hepatol 23:e465–e470
Skrzydlewska E, Ostrowska J, Farbiszewski R, Michalak K (2002) Protective effect of green tea against lipid peroxidation in the rat liver, blood serum and the brain. Phytomedicine 9:232–238
Nanji AA, Jokelainen K, Fotouhinia M, Rahemtulla A, Thomas P, Tipoe GL, Su GL, Dannenberg AJ (2001) Increased severity of alcoholic liver injury in female rats: role of oxidative stress, endotoxin, and chemokines. American journal of physiology. Gastrointest liver physiol 281:G1348–G1356
Cassiman D, van Pelt J, De Vos R, Van Lommel F, Desmet V, Yap SH, Roskams T (1999) Synaptophysin: a novel marker for human and rat hepatic stellate cells. Am J Pathol 155:1831–1839
Hung MW, Tipoe GL, Poon AM, Reiter RJ, Fung ML (2008) Protective effect of melatonin against hippocampal injury of rats with intermittent hypoxia. J Pineal Res 44:214–221
Tipoe GL, Leung TM, Liong E, So H, Leung KM, Lau TY, Tom WM, Fung ML, Fan ST, Nanji AA (2006) Inhibitors of inducible nitric oxide (NO) synthase are more effective than an NO donor in reducing carbon-tetrachloride induced acute liver injury. Histol Histopathol 21:1157–1165
Leung TM, Fung ML, Liong EC, Lau TY, Nanji AA, Tipoe GL (2011) Role of nitric oxide in the regulation of fibrogenic factors in experimental liver fibrosis in mice. Histol Histopathol 26:201–211
Nanji AA, Jokelainen K, Rahemtulla A, Miao L, Fogt F, Matsumoto H, Tahan SR, Su GL (1999) Activation of nuclear factor kappa B and cytokine imbalance in experimental alcoholic liver disease in the rat. Hepatology (Baltimore, MD) 30:934–943
Feldstein AE, Papouchado BG, Angulo P, Sanderson S, Adams L, Gores GJ (2005) Hepatic stellate cells and fibrosis progression in patients with nonalcoholic fatty liver disease. Clin Gastroenterol Hepatol 3:384–389
Iredale JP (2001) Hepatic stellate cell behavior during resolution of liver injury. Semin Liver Dis 21:427–436
Adachi M, Osawa Y, Uchinami H, Kitamura T, Accili D, Brenner DA (2007) The fork head transcription factor FoxO1 regulates proliferation and transdifferentiation of hepatic stellate cells. Gastroenterology 132:1434–1446
dela Peña A, Leclercq I, Field J, George J, Jones B, Farrell G (2005) NF-κB activation, rather than TNF, mediates hepatic inflammation in a murine dietary model of steatohepatitis. Gastroenterology 129:1663–1674
Butt MS, Sultan MT (2009) Green tea: nature’s defense against malignancies. Crit Rev Food Sci Nutr 49:463–473
Chen JH, Tipoe GL, Liong EC, So HS, Leung KM, Tom WM, Fung PC, Nanji AA (2004) Green tea polyphenols prevent toxin-induced hepatotoxicity in mice by down-regulating inducible nitric oxide-derived prooxidants. American J clin nut 80:742–751
Chung MY, Park HJ, Manautou JE, Koo SI, Bruno RS (2012) Green tea extract protects against nonalcoholic steatohepatitis in ob/ob mice by decreasing oxidative and nitrative stress responses induced by proinflammatory enzymes. J Nutr Biochem 23:361–367
Park HJ, Lee JY, Chung MY, Park YK, Bower AM, Koo SI, Giardina C, Bruno RS (2012) Green tea extract suppresses NFκB activation and inflammatory responses in diet-induced obese rats with nonalcoholic steatohepatitis. J Nutr 142:57–63
Masterjohn C, Bruno RS (2012) Therapeutic potential of green tea in nonalcoholic fatty liver disease. Nutr Rev 70:41–56
Nakagawa K, Okuda S, Miyazawa T (1997) Dose-dependent incorporation of tea catechins, (−)-epigallocatechin-3-gallate and (−)-epigallocatechin, into human plasma. Biosci Biotechnol Biochem 61:1981–1985
Tang LX, He RH, Yang G, Tan JJ, Zhou L, Meng XM, Huang XR, Lan HY (2012) Asiatic acid inhibits liver fibrosis by blocking TGF-beta/Smad signaling in vivo and in vitro. PLoS ONE 7:e31350
Adachi M, Brenner DA (2008) High molecular weight adiponectin inhibits proliferation of hepatic stellate cells via activation of adenosine monophosphate-activated protein kinase. Hepatology (Baltimore, MD) 47:677–685
Chen D, Milacic V, Chen MS, Wan SB, Lam WH, Huo C, Landis-Piwowar KR, Cui QC, Wali A, Chan TH, Dou QP (2008) Tea polyphenols, their biological effects and potential molecular targets. Histol Histopathol 23:487–496
Frei B, Higdon JV (2003) Antioxidant activity of tea polyphenols in vivo: evidence from animal studies. J Nutr 133:3275S–3284S
Yumei F, Zhou Y, Zheng S, Chen A (2006) The antifibrogenic effect of (−)-epigallocatechin gallate results from the induction of de novo synthesis of glutathione in passaged rat hepatic stellate cells. Lab Invest 86:697–709
Wang F, Wang LY, Wright D, Parmely MJ (1999) Redox imbalance differentially inhibits lipopolysaccharide-induced macrophage activation in the mouse liver. Infect Immun 67:5409–5416
Aktas O, Prozorovski T, Smorodchenko A, Savaskan NE, Lauster R, Kloetzel PM, Infante-Duarte C, Brocke S, Zipp F (2004) Green tea epigallocatechin-3-gallate mediates T cellular NF-kappa B inhibition and exerts neuroprotection in autoimmune encephalomyelitis. J immunol (Baltimore, Md.: 1950) 173:5794–5800
Yang F, Oz HS, Barve S, de Villiers WJ, McClain CJ, Varilek GW (2001) The green tea polyphenol (−)-epigallocatechin-3-gallate blocks nuclear factor-kappa B activation by inhibiting I kappa B kinase activity in the intestinal epithelial cell line IEC-6. Mol Pharmacol 60:528–533
Lin YL, Lin JK (1997) (−)-Epigallocatechin-3-gallate blocks the induction of nitric oxide synthase by down-regulating lipopolysaccharide-induced activity of transcription factor nuclear factor-kappaB. Mol Pharmacol 52:465–472
Gupta S, Hastak K, Afaq F, Ahmad N, Mukhtar H (2004) Essential role of caspases in epigallocatechin-3-gallate-mediated inhibition of nuclear factor kappa B and induction of apoptosis. Oncogene 23:2507–2522
Afaq F, Adhami VM, Ahmad N, Mukhtar H (2003) Inhibition of ultraviolet B-mediated activation of nuclear factor kappaB in normal human epidermal keratinocytes by green tea Constituent (-)-epigallocatechin-3-gallate. Oncogene 22:1035–1044
Shimizu M, Deguchi A, Joe AK, McKoy JF, Moriwaki H, Weinstein IB (2005) EGCG inhibits activation of HER3 and expression of cyclooxygenase-2 in human colon cancer cells. J Exp Ther Oncol 5:69–78
Nakamoto K, Takayama F, Mankura M, Hidaka Y, Egashira T, Ogino T, Kawasaki H, Mori A (2009) Beneficial effects of fermented green tea extract in a rat model of non-alcoholic steatohepatitis. J Clin Biochem Nutr 44:239–246
Acknowledgments
We would like to thank Miss Carman Leung for her technical assistance in this project. This study was partly supported by the Small Project Funding of Research, University Research Committee, The University of Hong Kong, Hong Kong.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Jia Xiao and Chi Tat Ho have equally contributed to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Xiao, J., Ho, C.T., Liong, E.C. et al. Epigallocatechin gallate attenuates fibrosis, oxidative stress, and inflammation in non-alcoholic fatty liver disease rat model through TGF/SMAD, PI3 K/Akt/FoxO1, and NF-kappa B pathways. Eur J Nutr 53, 187–199 (2014). https://doi.org/10.1007/s00394-013-0516-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-013-0516-8