Abstract
Objectives
To characterize determinants of 4-, 12-, and 24-month urinary control after robot-assisted laparoscopic prostatectomy (RALP).
Methods
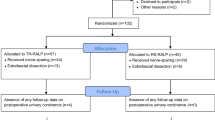
Adjusted comparative study using prospectively collected, patient self-reported urinary control for 602 consecutive RALPs. Urinary control defined as: (1) EPIC urinary function (UF) scored from 0 to 100 and (2) continence (zero pads per day).
Results
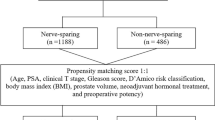
Both UF (62.8 vs. 42.4, P < 0.001) and continence rates (47.2 vs. 26.7%, P = 0.043) were better for bilateral nerve-sparing (BNS) vs. non-nerve-sparing (NNS) at 4 months, but only UF scores were significantly better at 12- (80.9 vs. 70.7, P = 0.014) and 24-month (89.2 vs. 77.4, P = 0.024) post-RALP. No difference in positive margin rates was observed. In multivariate analysis, older age (parameter estimate −0.42, 95% CI −0.80 to −0.04) and increasing gland volume (−0.13, CI −0.26 to −0.01) resulted in lower UF scores at 4 months, while higher pre-operative UF (0.25, CI 0.05–0.46), bladder neck-sparing technique (10.1, CI 3.79–16.35), BNS (19.1, CI 9.37–28.82), and unilateral nerve-sparing (19.00, CI 7.88–30.11) resulted in higher UF scores at 4 months. At 12 months, higher pre-operative UF (0.24, CI 0.083–0.40) and BNS (9.54, CI 1.92–17.16) resulted in higher UF scores. At 24 months, higher pre-operative UF (0.20, CI 0.06–0.33), bladder neck-sparing technique (7.80, CI 3.48–12.10), and BNS (7.86, CI 1.04–14.68) resulted in higher UF scores.
Conclusions
BNS, bladder neck-sparing technique, and higher pre-operative UF score result in improved 24-month urinary control after RALP.
Similar content being viewed by others
References
Litwin MS, Hays RD, Fink A et al (1995) Quality-of-life outcomes in men treated for localized prostate cancer. JAMA 273:129–135
Sanda MG, Dunn RL, Michalski J et al (2008) Quality of life and satisfaction with outcome among prostate-cancer survivors. N Engl J Med 358:1250–1261
Foote J, Yun S, Leach GE (1991) Postprostatectomy incontinence. Pathophysiology, evaluation, and management. Urol Clin North Am 18:229–241
Cambio AJ, Evans CP (2006) Minimising postoperative incontinence following radical prostatectomy: considerations and evidence. Eur Urol 50:903–913
Eastham JA, Kattan MW, Rogers E et al (1996) Risk factors for urinary incontinence after radical prostatectomy. J Urol 156:1707–1713
Kundu SD, Roehl KA, Eggener SE et al (2004) Potency, continence and complications in 3, 477 consecutive radical retropubic prostatectomies. J Urol 172:2227–2231
Steiner MS, Morton RA, Walsh PC (1991) Impact of anatomical radical prostatectomy on urinary continence. J Urol 145:512–514; (discussion 4-5)
Guru KA, Hussain A, Chandrasekhar R et al (2009) Current status of robot-assisted surgery in urology: a multi-national survey of 297 urologic surgeons. Can J Urol 16:4736–4741
Hu JC, Gu X, Lipsitz SR et al (2009) Comparative effectiveness of minimally invasive vs open radical prostatectomy. JAMA 302:1557–1564
Levinson AW, Pavlovich CP, Ward NT et al (2008) Association of surgeon subjective characterization of nerve sparing quality with potency following laparoscopic radical prostatectomy. J Urol 179:1510–1514
Freire MP, Weinberg AC, Lei Y et al (2009) Anatomic bladder neck preservation during robotic-assisted laparoscopic radical prostatectomy: description of technique and outcomes. Eur Urol 56:972–980
Berry A, Korkes F, Hu JC (2008) Landmarks for consistent nerve sparing during robotic-assisted laparoscopic radical prostatectomy. J Endourol 22:1565–1567
Wei JT, Dunn RL, Litwin MS et al (2000) Development and validation of the expanded prostate cancer index composite (EPIC) for comprehensive assessment of health-related quality of life in men with prostate cancer. Urology 56:899–905
Konety BR, Sadetsky N, Carroll PR et al (2007) Recovery of urinary continence following radical prostatectomy: the impact of prostate volume-analysis of data from the CaPSURETM database. J Urol 177:1423–1426
Poore RE, McCullough DL, Jarow JP (1998) Puboprostatic ligament sparing improves urinary continence after radical retropubic prostatectomy. Urology 51:67–72
Paparel P, Akin O, Sandhu J et al (2009) Recovery of urinary continence after radical prostatectomy: association with urethral length and urethral fibrosis measured by preoperative and postoperative endorectal magnetic resonance imaging. Eur Urol 55:629–639
John Wei (2009) Personal communication of unpublished data
Krupski TL, Saigal CS, Litwin MS (2003) Variation in continence and potency by definition. J Urol 170:1291–1294
van der Poel HG, de Blok W, Joshi N, van Muilekom E (2009) Preservation of lateral prostatic fascia is associated with urine continence after robotic-assisted prostatectomy. Eur Urol 55:892–900
Potdevin L, Ercolani M, Jeong J et al (2009) Functional and oncologic outcomes comparing interfascial and intrafascial nerve sparing in robot-assisted laparoscopic radical prostatectomies. J Endourol 23:1479–1484
Nelles JL, Freedland SJ, Presti JC Jr et al (2009) Impact of nerve sparing on surgical margins and biochemical recurrence: results from the SEARCH database. Prostate Cancer Prostatic Dis 12:172–176
Burkhard FC, Kessler TM, Fleischmann A et al (2006) Nerve sparing open radical retropubic prostatectomy–does it have an impact on urinary continence? J Urol 176:189–195
Sacco E, Prayer-Galetti T, Pinto F et al (2006) Urinary incontinence after radical prostatectomy: incidence by definition, risk factors and temporal trend in a large series with a long-term follow-up. BJU Int 97:1234–1241
Kaiho Y, Nakagawa H, Ikeda Y et al (2005) Intraoperative electrophysiological confirmation of urinary continence after radical prostatectomy. J Urol 173:1139–1142
Hollabaugh RS Jr, Dmochowski RR, Kneib TG et al (1998) Preservation of putative continence nerves during radical retropubic prostatectomy leads to more rapid return of urinary continence. Urology 51:960–967
Wei JT, Dunn RL, Marcovich R et al (2000) Prospective assessment of patient reported urinary continence after radical prostatectomy. J Urol 164:744–748
Nelson CP, Montie JE, McGuire EJ et al (2003) Intraoperative nerve stimulation with measurement of urethral sphincter pressure changes during radical retropubic prostatectomy: a feasibility study. J Urol 169:2225–2228
Marien TP, Lepor H (2008) Does a nerve-sparing technique or potency affect continence after open radical retropubic prostatectomy? BJU Int 102:1581–1584
Narayan P, Konety B, Aslam K et al (1995) Neuroanatomy of the external urethral sphincter: implications for urinary continence preservation during radical prostate surgery. J Urol 153:337–341
Acknowledgments
This project was funded by the Department of Defense research grant to Dr. Hu (W81XWH-08-1-0283).
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
W. W. Choi and M. P. Freire are contributed equally.
Rights and permissions
About this article
Cite this article
Choi, W.W., Freire, M.P., Soukup, J.R. et al. Nerve-sparing technique and urinary control after robot-assisted laparoscopic prostatectomy. World J Urol 29, 21–27 (2011). https://doi.org/10.1007/s00345-010-0601-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-010-0601-z