Abstract
Objective
The study was designed to determine the distance between the visible “ice-ball” and the lethal temperature isotherm for normal renal tissue during cryoablation.
Methods
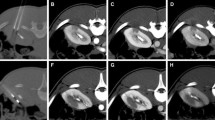
The Animal Care Committee approved the study. Nine adult swine were used: three to determine the optimum tissue stain and six to test the hypotheses. They were anesthetized and the left renal artery was catheterized under fluoroscopy. Under MR guidance, the kidney was ablated and (at end of a complete ablation) the nonfrozen renal tissue (surrounding the “ice-ball”) was stained via renal artery catheter. Kidneys were explanted and sent for slide preparation and examination. From each slide, we measured the maximum, minimum, and an in-between distance from the stained to the lethal tissue boundaries (margin). We examined each slide for evidence of “heat pump” effect.
Results
A total of 126 measurements of the margin (visible “ice-ball”–lethal margin) were made. These measurements were obtained from 29 slides prepared from the 6 test animals. Mean width was 0.75 ± 0.44 mm (maximum 1.15 ± 0.51 mm). It was found to increase adjacent to large blood vessels. No “heat pump” effect was noted within the lethal zone. Data are limited to normal swine renal tissue.
Conclusions
Considering the effects of the “heat pump” phenomenon for normal renal tissue, the margin was measured to be 1.15 ± 0.51 mm. To approximate the efficacy of the “gold standard” (partial nephrectomy, ~98 %), a minimum margin of 3 mm is recommended (3 × SD). Given these assumptions and extrapolating for renal cancer, which reportedly is more cryoresistant with a lethal temperature of −40 °C, the recommended margin is 6 mm.








Similar content being viewed by others
References
Ljunberg B, Campbell S, Cho H et al (2011) The epidemiology of renal cell carcinoma. Eur Urol 60(4):615–621
National Cancer Institute. Surveillance Epidemiology and End results. http://seer.cancer.gov/statfacts/html/kidrp.html
Campbell SC, Novick AC, Belldegrun A et al (2009) Guideline for management of the clinical T1 renal mass. J Urol 182:1271–1279
Georgiades CS, Rodriguez R, Littrup PJ et al (2010) Development of a research agenda for percutaneous renal tumor ablation: proceedings from a multidisciplinary research consensus panel. J Vasc Interv Radiol 21(12):1807–1816
Kang DC, Palmer DA, Zarei M et al (2012) Systematic review of the quality of evidence of ablative therapy for small renal masses. J Urol 187(1):44–47
Goyal J, Sidana A, Georgiades CS et al (2011) Renal function and oncologic outcomes after cryoablation or partial nephrectomy for renal tumors in solitary kidneys. Korean J Urol 52(6):384–389
Rodriguez R, Cizman Z, Hong K et al (2011) Prospective analysis of the safety and efficacy of percutaneous cryoablation for pT1NxMx biopsy-proven renal cell carcinoma. Cardiovasc Intervent Radiol 34(3):573–578
Sidana A, Aggarwal P, Feng Z et al (2010) Complications of renal cryoablation: a single center experience. J Urol 184(1):42–47
Georgiades CS, Hong K, Bizzell C et al (2008) Safety and efficacy of CT-guided percutaneous cryoablation for renal cell carcinoma. J Vasc Interv Radiol 19(9):1302–1310
Littrup PJ, Ahmed A, Aoun HD et al (2007) CT-guided percutaneous cryotherapy of renal masses. J Vasc Interv Radiol 18(3):383–392
Long CJ, Kutikov A, Canter DJ et al (2011) Percutaneous vs surgical cryoablation of the small renal mass: is efficacy compromised? BJU Int 107(9):1376–1380
Gildenberg P, Hardenbergh E (1964) The effect of immediate sympathectomy on tissue survival following experimental frostbite. Ann Surg 160(1):160–168
Kauk J, Aron M, Rewcastle J et al (2006) Cryotherapy: clinical end points and experimental foundations. Urology 68(Suppl 1A):38–44
Clarke D, Robilotto A, Rhee E et al (2007) Cryoablation of renal cancer: variables involved in freezing-induced cell death. Technol Cancer Res Treat 6(2):69–79
Williams SK, de la Rosette J, Landman J, Keely FX (2007) Cryoablation of small renal tumors. EAU-EBU Update Series 5:206–218
Weld KJ, Hruby G, Humphrey PA et al (2006) Precise characterization of renal parenchymal response to single and multiple cryoablation probes. J Urol 176:784–786
Campbell SC, Krishnamurthi V, Chow G et al (1998) Renal cryosurgery: experimental evaluations of treatment parameters. Urology 52(1):29–34
Jang TL, Wang R, Kim SC et al (2005) Histopathology of human renal tumors after laparoscopic renal cryosurgery. J Urol 173(3):720–724
Collyer WC, Landman J, Olweny EO et al (2001) Comparison of renal ablation with cryotherapy, dry radiofrequency, and saline augmented radiofrequency in a porcine model. J Am Coll Surg 193(5):505–513
Lagerveld BW, van Horssen P, Laguna MP et al (2011) Gradient changes in porcine renal arterial vascular anatomy and blood flow after cryoablation. J Urol 186(2):681–686
Blitstein J, Ghavamian R (2008) Laparoscopic partial nephrectomy in the treatment of renal cell carcinoma: a minimally invasive means to nephron preservation. Expert Rev Anticancer Ther 8(6):921–927
Antonelli A, Ficarra V, Bertini R et al (2012) Elective partial nephrectomy is equivalent to radical nephrectomy in patients with clinical T1 renal cell carcinoma: results of a retrospective, comparative, multi-institutional study. BJU Int 109(7):1013–1018
Conflict of interest
Christos Georgiades received financial support from Siemens Medical Solutions, USA, Inc. Ronald Rodriguez, Ezana Azene, Clifford Weiss, Alcides Chaux, Nilda Gonzalez-Roibon, and George Netto have no conflict of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Additional information
Grant Support: Financial support from Siemens Medical Solutions, USA, Inc.
Rights and permissions
About this article
Cite this article
Georgiades, C., Rodriguez, R., Azene, E. et al. Determination of the Nonlethal Margin Inside the Visible “Ice-Ball” During Percutaneous Cryoablation of Renal Tissue. Cardiovasc Intervent Radiol 36, 783–790 (2013). https://doi.org/10.1007/s00270-012-0470-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-012-0470-5