Abstract
Purpose
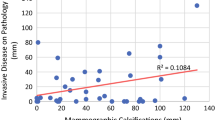
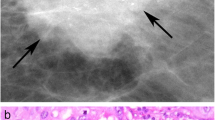
This study was designed to determine the relationship of microcalcification morphology and distribution with clinical, histopathologic, biologic features, and local recurrence (LR) in patients with pure ductal carcinoma in situ (DCIS) of the breast.
Methods
All patients with pure DCIS who underwent preoperative mammography at our institution from 1996 through 2009 were identified. Mammographic findings were classified according to the ACR BI-RADS lexicon. Associations between mammographic findings and clinical, histopathologic, biologic characteristics, and LR were analyzed. Statistical inference used multiple logistic regression and Cox proportional hazards regression adjusted for age and confounding due to bias from nonrandomized selection of radiation therapy.
Results
We identified 1657 patients with microcalcifications visualized on mammography. The mean age at diagnosis was 55 years (SD, 11). The mean follow-up was 7 years (range 1–16). Ipsilateral LR was 4 % in segmentectomy (987) and 1.5 % in mastectomy (670) patients. Increased LR risk was seen in patients with dense breast tissue (p < 0.05) and larger DCIS size (p < 0.01). Radiation therapy was associated with a 2.8-fold decrease in the LR risk. Fine linear (branching) microcalcifications were associated with 5.2-fold increase in LR. Extremely dense breast tissue was associated with positive/close margins (p = 0.04) and multicentricity (p < 0.01). Younger women were more likely to have extremely dense breast tissue (p < 0.0001), multicentric disease (p < 0.0004), and undergo mastectomy (p < 0.0001).
Conclusions
Dense breast tissue, large DCIS size, and fine linear (branching) microcalcifications were associated with increased LR, yet overall LR rates remained low. Extremely dense breast tissue was a risk factor for multicentricity and positive margins in DCIS.

Similar content being viewed by others
References
Ernster VL, Ballard-Barbash R, Barlow WE, et al. Detection of ductal carcinoma in situ in women undergoing screening mammography. J Natl Cancer Inst. 2002;94(20):1546–54.
Parker J, Dance DR, Davies DH, Yeoman LJ, Michell MJ, Humphreys S. Classification of ductal carcinoma in situ by image analysis of calcifications from digital mammograms. Br J Radiol. 1995;68(806):150–9.
Bijker N, Meijnen P, Peterse JL, et al. Breast-conserving treatment with or without radiotherapy in ductal carcinoma-in situ: ten-year results of European Organisation for Research and Treatment of Cancer randomized phase III trial 10853–a study by the EORTC Breast Cancer Cooperative Group and EORTC Radiotherapy Group. J Clin Oncol. 2006;24(21):3381–7.
Boyages J, Delaney G, Taylor R. Predictors of local recurrence after treatment of ductal carcinoma in situ: a meta-analysis. Cancer. 1999;85(3):616–28.
Menell JH, Morris EA, Dershaw DD, Abramson AF, Brogi E, Liberman L. Determination of the presence and extent of pure ductal carcinoma in situ by mammography and magnetic resonance imaging. Breast J. 2005;11(6):382–90.
Sue GR, Lannin DR, Killelea B, Chagpar AB. Predictors of microinvasion and its prognostic role in ductal carcinoma in situ. Am J Surg. 2013; 206: 478–81.
Zunzunegui RG, Chung MA, Oruwari J, Golding D, Marchant DJ, Cady B. Casting-type calcifications with invasion and high-grade ductal carcinoma in situ: a more aggressive disease? Arch Surg. 2003;138(5):537–40.
Stomper PC, Geradts J, Edge SB, Levine EG. Mammographic predictors of the presence and size of invasive carcinomas associated with malignant microcalcification lesions without a mass. AJR Am J Roentgenol. 2003;181(6):1679–84.
Roses RE, Arun BK, Lari SA, et al. Ductal carcinoma-in situ of the breast with subsequent distant metastasis and death. Ann Surg Oncol. 2011;18(10):2873–8.
Boughey JC, Gonzalez RJ, Bonner E, Kuerer HM. Current treatment and clinical trial developments for ductal carcinoma in situ of the breast. Oncologist. 2007;12(11):1276–87.
MacDonald HR, Silverstein MJ, Mabry H, et al. Local control in ductal carcinoma in situ treated by excision alone: incremental benefit of larger margins. Am J Surg. 2005;190(4):521–5.
Yi M, Krishnamurthy S, Kuerer HM, et al. Role of primary tumor characteristics in predicting positive sentinel lymph nodes in patients with ductal carcinoma in situ or microinvasive breast cancer. Am J Surg. 2008;196(1):81-7.
Holland R, Hendriks JH. Microcalcifications associated with ductal carcinoma in situ: mammographic-pathologic correlation. Sem Diagn Pathol. 1994;11(3):181–92.
Hofvind S, Iversen BF, Eriksen L, Styr BM, Kjellevold K, Kurz KD. Mammographic morphology and distribution of calcifications in ductal carcinoma in situ diagnosed in organized screening. Acta Radiol. 2011;52(5):481–7.
Barreau B, de Mascarel I, Feuga C, et al. Mammography of ductal carcinoma in situ of the breast: review of 909 cases with radiographic-pathologic correlations. Eur J Radiol. 2005;54(1):55–61.
Poplack SP, Wells WA. Ductal carcinoma in situ of the breast: mammographic-pathologic correlation. AJR Am J Roentgenol. 1998;170(6):1543–9.
Bai HX, Motwani SB, Higgins SA, et al. Breast conservation therapy for ductal carcinoma in situ (DCIS): does presentation of disease affect long-term outcomes? Int J Clin Oncol. 2013; 19:460–66
Shaitelman SF, Wilkinson JB, Kestin LL, et al. Long-term outcome in patients with ductal carcinoma in situ treated with breast-conserving therapy: implications for optimal follow-up strategies. Int J Radiat Oncol Biol Phys. 2012;83(3):e305–12.
Vargas C, Kestin L, Go N, et al. Factors associated with local recurrence and cause-specific survival in patients with ductal carcinoma in situ of the breast treated with breast-conserving therapy or mastectomy. Int J Radiat Oncol Biol Phys. 2005;63(5):1514–21.
Yi M, Meric-Bernstam F, Kuerer HM, et al. Evaluation of a breast cancer nomogram for predicting risk of ipsilateral breast tumor recurrences in patients with ductal carcinoma in situ after local excision. J Clin Oncol. 2012;30(6):600–7.
Tse G, Tan PH, Pang AL, Tang AP, Cheung HS. Calcification in breast lesions: pathologists’ perspective. J Clin Pathol. 2008;61(2):145–51.
Tabar L, Chen HH, Duffy SW, et al. A novel method for prediction of long-term outcome of women with T1a, T1b, and 10-14 mm invasive breast cancers: a prospective study. Lancet. 2000;355 (9202):429–33.
Tabar L, Tony Chen HH, Amy Yen MF, et al. Mammographic tumor features can predict long-term outcomes reliably in women with 1-14-mm invasive breast carcinoma. Cancer. 2004;101(8):1745–59.
Palka I, Ormandi K, Gaal S, Boda K, Kahan Z. Casting-type calcifications on the mammogram suggest a higher probability of early relapse and death among high-risk breast cancer patients. Acta Oncol. 2007;46(8):1178–83.
Rauch GM, Kuerer HM, Scoggins ME, et al. Clinicopathologic, mammographic, and sonographic features in 1,187 patients with pure ductal carcinoma in situ of the breast by estrogen receptor status. Breast Cancer Res Treat. 2013;139(3):639–47.
D’Orsi C, Mendelson E, Ikeda D. Breast imaging reporting and data system: ACR BI-RADS—Breast Imaging Atlas. Reston, VA: American College of Radiology; 2003.
Fine JP, Gray RJ. A proportional hazards model for the subdistribution of a competing risk. J Am Stat Assoc. 1999;94(446):496–509.
Austin PC. An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivar Behav Res. 2011;46(3):399–424.
Stomper PC, Connolly J. Ductal carcinoma in situ of the breast: correlation between mammographic calcification and tumor subtype. AJR Am J Roentgenol. 1992;159(3):483–85.
Evans AJ, Pinder S, Ellis IO, et al. Screening-detected and symptomatic ductal carcinoma in situ: mammographic features with pathologic correlation. Radiology. 1994;191(1):237–40.
Thomson JZ, Evans AJ, Pinder SE, Burrell HC, Wilson AR, Ellis IO. Growth pattern of ductal carcinoma in situ (DCIS): a retrospective analysis based on mammographic findings. Br J Cancer. 2001;85(2):225–7.
Tabár L, Tot T, Dean PB. Casting type calcifications: sign of a subtype with deceptive features. Thieme; 2007.
Stomper PC, Margolin FR. Ductal carcinoma in situ: the mammographer’s perspective. AJR Am J Roentgenol. 1994;162(3):585–91.
Alvarado R, Lari SA, Roses RE, et al. Biology, treatment, and outcome in very young and older women with DCIS. Ann Surg Oncol. 2012;19(12):3777–84.
Ho A, Goenka A, Ishill N, et al. The effect of age in the outcome and treatment of older women with ductal carcinoma in situ. Breast. 2011;20(1):71–7.
Fitzsullivan E, Lari SA, Smith B, et al. Incidence and consequence of close margins in patients with ductal carcinoma-in situ treated with mastectomy: is further therapy warranted? Ann Surg Oncol. 2013;20(13):4103–12.
Biglia N, Bounous VE, Martincich L, et al. Role of MRI (magnetic resonance imaging) versus conventional imaging for breast cancer presurgical staging in young women or with dense breast. Eur J Surg Oncol. 2011;37(3):199–204.
Kuhl CK, Schrading S, Bieling HB, et al. MRI for diagnosis of pure ductal carcinoma in situ: a prospective observational study. Lancet. 2007;370(9586):485–92.
Lehman CD. Magnetic resonance imaging in the evaluation of ductal carcinoma in situ. J Natl Cancer Inst Monogr. 2010;2010(41):150–1.
Kuerer HM, Albarracin CT, Yang WT, et al. Ductal carcinoma in situ: state of the science and roadmap to advance the field. J Clin Oncol. 2009;27(2):279–88.
Lari SA, Kuerer HM. Biological markers in DCIS and risk of breast recurrence: a systematic review. J Cancer. 2011;2:232–61.
Allegra CJ, Aberle DR, Ganschow P, et al. National Institutes of Health State-of-the-Science Conference statement: diagnosis and management of ductal carcinoma in situ, September 22-24, 2009. J Natl Cancer Inst. 2010;102(3):161–9.
Rudloff U, Jacks LM, Goldberg JI, et al. Nomogram for predicting the risk of local recurrence after breast-conserving surgery for ductal carcinoma in situ. J Clin Oncol. 2010;28(23):3762–9.
Wang F, Li H, Tan PH, et al. Validation of a nomogram in the prediction of local recurrence risks after conserving surgery for Asian women with ductal carcinoma in situ of the breast. Clin Oncol. 2014; 26: 684–91.
Pinsky RW, Rebner M, Pierce LJ, et al. Recurrent cancer after breast-conserving surgery with radiation therapy for ductal carcinoma in situ: mammographic features, method of detection, and stage of recurrence. AJR Am J Roentgenol. 2007;189(1):140–4.
Rakovitch E, Pignol JP, Hanna W, et al. Significance of multifocality in ductal carcinoma in situ: outcomes of women treated with breast-conserving therapy. J Clin Oncol. 2007;25(35):5591–6.
Yerushalmi R, Tyldesley S, Woods R, Kennecke HF, Speers C, Gelmon KA. Is breast-conserving therapy a safe option for patients with tumor multicentricity and multifocality? Ann Oncol. 2011;23(4):876–81.
Holmberg L, Wong YN, Tabar L, et al. Mammography casting-type calcification and risk of local recurrence in DCIS: analyses from a randomised study. Br J Cancer. 2013;108(4):812–9.
Kuerer HM. Ductal carcinoma in situ: treatment or active surveillance? Expert Rev Anticancer Ther. 2015;15(7):777–85.
Acknowledgments
Supported by the NIH/NCI under Award Number P30CA016672 and used the Biostatistics Resource Group from the Department of Biostatistics. The authors thank Stephanie Deming for assistance in editing of this manuscript.
Disclosure
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rauch, G.M., Hobbs, B.P., Kuerer, H.M. et al. Microcalcifications in 1657 Patients with Pure Ductal Carcinoma in Situ of the Breast: Correlation with Clinical, Histopathologic, Biologic Features, and Local Recurrence. Ann Surg Oncol 23, 482–489 (2016). https://doi.org/10.1245/s10434-015-4876-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-015-4876-6