Abstract
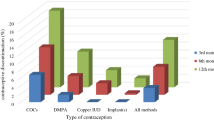
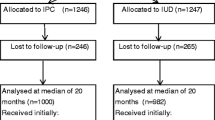
The objectives of this study were to evaluate performance and causes of discontinuation of the Copper T380A IUD by users at the Family Planning Service at Hospital Arzobispo Loayza in Lima, Peru, during a period of three years. The study included 3167 acceptors of the CuT380A attending the service during 1992-1994. IUDs were inserted during interval timing. Follow-up was at 1, 12, 24 and 36 months after insertion. The following events were recorded: number of pregnancies, expulsions and all causes of discontinuation. The cumulative rates per 100 woman-years using the life-table method was calculated. Also calculated were the relative risks for expulsion and for pregnancy. At the end of the study, 361 women had discontinued the method for various reasons, whereas 1667 women continued using the method. The lost-to-follow-up proportion increased over time from 35.9 per 100 woman-years for the first year to 38.2 for the third year. The cumulative discontinuation rate over three years was 22.6±1.3 (cumulative rate±standard error) per 100 woman-years. The cumulative pregnancy rate for three years was 1.2±0.4 per 100 woman-years, whereas the cumulative rate of expulsion was 4.9±0.4 for the first, 6.4 for the second and 6.8 for the third year. The main cause of discontinuation during the first year of use was expulsion (4.9 per 100 woman-years) followed by personal reasons (2.1 per 100 woman-years). At the end of the third year, the main cause was personal reasons (11.4) and the second cause was expulsion (6.8). A higher probability of expulsion, pregnancy and discontinuation for bleeding and/or pain was associated with age less than 20 years. In conclusion, the effectiveness of the CuT380A IUD after three years of use was 98.8 per 100 woman-years, whereas continuation was 39.2, and loss to follow-up increased over time.
Similar content being viewed by others
References
Sivin I, Stern J. Long-acting, more effective Copper T IUDs: A summary of US experience, 1970-75. Stud Fam Plann. 1979;10:263-81.
Boateng J, Chi I-C, Jones DB. An evaluationn of six new intrauterine devices. Adv Contracept. 1994;10:57-70.
Edelman DA, Berger GS, Keith LG. Intrauterine Devices and their Complications. Boston: CK Hall, 1979:40-1.
Theiry M, van Kets H, van der Pas H. Immediate post-placental IUD insertion: the expulsion problem. Contraception. 1985;31:331-49.
Instituto Nacional de Estadistica e Informatica. PERU. Encuesta Demografica y de Salud Familiar. ENDES, 1996. Informe Principal. Lima: INEI, 1997:338.
O'Hanley K, Huber DH. Postpartum IUDs: keys for success. Contraception. 1992;45:351-61.
Chi I-C, Potts M, Wilkens LR, Champion CB. Performance of the copper T 380A intrauterine device in breastfeeding women. Contraception. 1989;39:603-18.
Faundes D, Bahamondes L, Faundes A et al. No relationship between IUD position evaluated by ultrasound and complaints of bleeding and pain. Contraception. 1997;56:43-7.
World Health Organization. The CuT380A, CuT220C, Multiload 250 and Nova T IUDs at 3, 5 and 7 years of use. Results from three randomized multicentre trials. Contraception. 1990;42:141-58.
Sivin I, Tatum HJ. Four years of experience with CuT380A intrauterine contraceptive device. Fertil Steril. 1981;36:159-63.
Indian Council of Medical Research. Randomized clinical trial with intrauterine devices (levonorgestrel intrauterine device, CuT380A, CuT220C and CuT200B). A 36 month study. Contraception. 1989;3:37-52.
Roy S, Casagrande J, Cooper DL, Mishell Dr Jr. Comparison of three different models of the copper T intrauterine device. Am J Obstet Gynecol. 1979;134:568-74.
Champion BC, Behlilovic B, Arosemena JM et al. A three year evaluation of CuT 380A and Multiload Cu 375 intrauterine devices. Contraception. 1988;38:631-9.
Chi I-C, Farr G, Thompson K et al. Is the copper T 380A device associated with an increased risk of removal due to bleeding and/or pain? An analysis. Contraception. 1990;42:159-69.
Milsom I, Rybo G, Lindstedt G. The influence of copper surface area on menstrual blood loss and iron status in women fitted with an IUD. Contraception. 1990;41:271-81.
Guillebaud J, Bonnar J. Longer though lighter menstrual and intermenstrual bleeding with copper as compared to inert intrauterine devices. Br J Obstet Gynecol. 1978;85:707-12.
Rybo G. The IUD and endometrial bleeding. J Reprod Med. 1978;20:175-82.
Kivijarvi A, Timonen H, Rajamaki A, Gronroos M. Iron deficiency in women using modern copper intrauterine devices. Obstet Gynecol. 1979;86:51-5.
Chi I-C, Farr G, Dominik R, Robinson N. Do retroverted uteri adversely affect insertions and performance of IUDs? Contraception. 1990;41:495-506.
Flesh G, Weiner JM, Corlett RC et al. The intrauterine contraceptive device and acute salpingitis. A multifactor analysis. Am J Obstet Gynecol. 1979;135:402-8.
Edelman DA. Pelvic inflammatory disease and contraceptive practice. Adv Contracept. 1986;2:141-4.
Lidegaard O, Helm P. Pelvic inflammatory disease: The influence of contraceptive, sexual, and social life events. Contraception. 1990;41:475-83.
Rosenberg MJ, Foldesy R, Mishell DR Jr et al. Performance of the CuT380A and CU-fix IUDs in an international randomized trial. Contraception. 1996;53:197-203.
Diaz J, Mendess PA, Bahamondes L et al. Performance of the copper T 200 in parous adolescents: Are copper IUDs suitable for these women? Contraception. 1993;48:23-8.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Escudero, F., Gonzales, G., Delgadillo, L. et al. Factors associated with discontinuation rates of the Copper T380A IUD in a Peruvian public hospital. Advances in Contraception 15, 303–311 (1999). https://doi.org/10.1023/A:1006792409169
Issue Date:
DOI: https://doi.org/10.1023/A:1006792409169