Abstract
Introduction
In this study, coagulation of the blood at the wound side is evoked using a 980-nm-wavelength diode laser. The laser is used to approximate incision wound edges to be compared with the healing of the sutured incision. Clinical observations, histological slides, and tensile strength measurement are performed to assess the quality of healing.
Material and methods
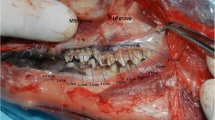
The study is conducted on 24 albino rabbits; an intraoral incision in the hard palate is done on both sides, right and left, for each rabbit. One side serves as a control group where the incision is sutured, while the other side’s incision is welded by a 980-nm-wavelength laser. The laser is operated in continuous wave mode (CW) 20 W/cm2 power density for 27 s exposure time.
Results
Clinically, there was some loss of tissue details (smooth feature) on the welded side in comparison with the conventionally treated side. Histopathologically, healing of the epithelial layer was perfect, while the submucosal layer showed loss of angiogenesis and loose connective tissue replacing the normal structure. The tensile strength measurement shows comparable results for the welded incision and the sutured incision; moreover, the immediate and first-day tensile strength of the welded incision shows superior results to the sutured incision.
Recommendation
Further studies are needed to monitor histologically the healing after laser welding and measure the development in the tensile strength to assess the validity of the 980-nm-wavelength laser beam as a tool in tissue welding.
Conclusion
Nine hundred eighty-nanometer-wavelength laser beam is a suitable tool for welding incisions in the oral cavity at areas subjected to stress, such as a socket after tooth extraction.








Similar content being viewed by others
References
Niemz Markolf H (2007) Laser-tissue interactions fundamentals and applications, third enlarged edition, Springer, P :1–79
Poppas DP, Choma TJ, Rooke CT, Klioze SD, Schlossberg SM (1993) Preparation of human albumin solder for laser tissue welding. Lasers Surg Med 13:577–580
Devoisselle JM, Soulie-Begu S, Mordon S, Desmettre T, Maillols H (1998) A preliminary study of the in vivo behavior of an emulsion formulation of indocyanine green. Lasers Med Sci 13:279–282
Mirdan BM (2012) Histopathological examination of oral mucosal incisions welded by 980 nm diode laser in vivo. J Dent Lasers 6(2):40
Rasca E, Nyssen-Behets C, Tielemans M, Peremans A, Hendaoui N, Heysselaer D, Romeo U, Nammour S (2014) Gingiva laser welding: preliminary study on an ex vivo porcine model. Photomed Laser Surg 32(8):437–443
Lucas MA, Fretto LJ, McKee PA (1983) The binding of human plasminogen to fibrin and fibrinogen. J Biol Chem 258(7):4249–4256
Tabakoğlu HÖ, Gülsoy M (2010) In vivo comparison of near infrared lasers for skin welding. Lasers Med Sci 25(3):411–421
Matteini P, Rossi F, Menabuoni L, Pini R (2007) Microscopic characterization of collagen modifications induced by low-temperature diode-laser welding of corneal tissue. Lasers Surg Med 39(7):597–604
Berger NA, Eeg PH (2008) Veterinary laser surgery: a practical guide. John Wiley & Sons
Abergel RP, Lyons R, Dwyer R, White RR, Uitto J (1986) Use of lasers for closure of cutaneous wounds: experience with Nd: YAG, argon and CO2 lasers. J Dermatol Surg Oncol 12(11):1181–1185
Sriramoju V, Alfano RR (2015) In vivo studies of ultrafast near-infrared laser tissue bonding and wound healing. J Biomed Opt 20(10):108001
Small W IV, Celliers PM, Kopchok GE, Reiser KM, Heredia NJ, Maitland DJ, Eder DC, London RA, Heilbron M, Hussain F, White RA (1998) Temperature feedback and collagen cross-linking in argon laser vascular welding. Lasers Med Sci 13(2):98–105
Liu C-H, Wang WB, Kartazaev V, Savage H, Alfano RR (2010) “Changes of collagen, elastin, and tryptophan contents in laser welded porcine aorta tissues studied using fluorescence spectroscopy,” Proc. SPIE 7561, Optical Biopsy VII, 756115
Fenner J, Martin W, Moseley H, Wheatley DJ (1992) Shear strength of tissue bonds as a function of bonding temperature: a proposed mechanism for laser-assisted tissue welding. Lasers Med Sci 7(1–4):39–43
Romeo U, Del Vecchio A, Ripari F, Palaiad G, Chiappafreddo C, Tenore G, Visca P (2007) Effects of different laser devices on oral soft tissues: in vitro experience. J Oral Laser Appl ;7(3)
Müller HP, Schaller N, Eger T, Heinecke A (2000) Thickness of masticatory mucosa. J Clin Periodontol 27(6):431–436
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This experiment on the rabbits was conducted under a protocol approved by the Institutional Animal Research and Care Ethics Committee at Bogazici University.
Conflict of interest
The research was perform on rabbits to create surgical incisions using surgical scalpel at keratinized oral mucosa of the hard palate. Each incision was welded using diode laser 980nm instue. Each sample was monitored clinically and studied histologically during the healing phases in addition to the tensile strength measurement which was performed. All the previously mentioned teste were compared with conventional sutured technique which is used now day.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(PDF 196 kb)
Rights and permissions
About this article
Cite this article
Mirdan, B.M., Naji, S., Sarp, A.S.K. et al. The tensile strength of laser welding of an incision in the keratinized oral mucosa of rabbits in vivo. Laser Dent Sci 3, 183–189 (2019). https://doi.org/10.1007/s41547-019-00059-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41547-019-00059-6