Abstract
Purpose of Review
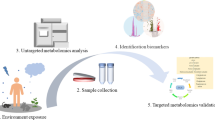
The purpose of this review is to summarize the application of untargeted metabolomics to identify the perturbation of metabolites or metabolic pathways associated with air pollutant exposures.
Recent Findings
Twenty-three studies were included in this review, in adults, children, or pregnant women. The most commonly measured air pollutant is particulate matter smaller than 2.5 μm. Size-fractioned particles, particle chemical species, gas pollutants, or organic compounds were also investigated. The reviewed studies used a wide range of air pollution measurement techniques and metabolomics analyses. Identified metabolites were primarily related to oxidative stress and inflammatory responses, and a few were related to the alterations of steroid metabolic pathways. The observed metabolic perturbations can differ by disease status, sex, and age. Air pollution-related metabolic changes were also associated with health outcomes in some studies.
Summary
Our review shows that air pollutant exposures are associated with metabolic pathways primarily related to oxidative stress, inflammation, as assessed through untargeted metabolomics in 23 studies. More metabolomic studies with larger sample sizes are needed to identify air pollution components most responsible for adverse health effects, elaborate on mechanisms for subpopulation susceptibility, and link air pollution exposure to specific adverse health effects.


Similar content being viewed by others
Abbreviations
- COPD:
-
chronic obstructive pulmonary disease
- IHD:
-
ischemic heart disease
- TRAP:
-
traffic-related air pollution
- O3 :
-
ozone
- PAHs:
-
polycyclic aromatic hydrocarbons
- PM:
-
particulate matter
- CO:
-
carbon monoxide
- NOx:
-
nitrogen oxides
- PM2.5 :
-
particulate matter with diameter ≤ 2.5 μm
- PM10 :
-
particulate matter with diameter ≤ 10 μm
- UFP:
-
ultrafine particles (particulate matter of nanoscale size, < 0.1 μm)
- PM2.5–10 :
-
particulate matter with a diameter between 2.5 and 10 μm
- TSP:
-
total suspended particles
- Pb-PAH:
-
particle-bound polycyclic aromatic hydrocarbons
- PNC:
-
particle number concentration
- BC:
-
black carbon
- EC:
-
elemental carbon
- OC:
-
organic carbon
- LDSA:
-
lung deposited surface area
- V:
-
vanadium
- 1-OHP:
-
1-hydroxypyrene
- LC-MS:
-
liquid chromatography coupled to mass spectrometry
- HILIC:
-
hydrophilic interaction liquid chromatography
- GC-MS:
-
gas chromatography coupled to mass spectrometry
- C18:
-
C18 hydrophobic reversed-phase chromatography
- ESI:
-
electrospray ionization
- TOF:
-
time-of-flight
- HMBD:
-
Human Metabolome Database
- KEGG:
-
Kyoto Encyclopedia of Genes and Genomes
- LC-MS/MS:
-
liquid chromatography coupled to tandem mass spectrometry
- PLS-DA:
-
partial least squares discriminant analysis
- OPLS-DA:
-
orthogonal PLS-DA
- ANOVA:
-
analysis of variance
- ANCOVA:
-
analysis of covariance
- ROS:
-
reactive oxygen species
- PUFA:
-
polyunsaturated fatty acids
- 13-HODE:
-
13-hydroperoxyoctadecadenoic acid
- 4-HNE:
-
4-hydroxynonenal
- FEV1:
-
forced expiratory volume in 1 s
- Pb-PAHs:
-
particle-bound polycyclic aromatic hydrocarbons
- AOA:
-
adult-onset asthma
- CCVD:
-
cardio-cerebrovascular diseases
References
Walker, D.I., et al., The metabolome: a key measure for exposome research in epidemiology. Current Epidemiology Reports, 2019: p. 1–11.
Patti GJ, Yanes O, Siuzdak G. Metabolomics: the apogee of the omics trilogy. Nat Rev Mol Cell Biol. 2012;13(4):263–9.
Dettmer K, Aronov PA, Hammock BD. Mass spectrometry-based metabolomics. Mass Spectrom Rev. 2007;26(1):51–78.
Rattray NJ, et al. Beyond genomics: understanding exposotypes through metabolomics. Human genomics. 2018;12(1):4.
Cohen AJ, Brauer M, Burnett R, Anderson HR, Frostad J, Estep K, et al. Estimates and 25-year trends of the global burden of disease attributable to ambient air pollution: an analysis of data from the Global Burden of Diseases Study 2015. Lancet. 2017;389(10082):1907–18.
Turner MC, Jerrett M, Pope CA III, Krewski D, Gapstur SM, Diver WR, et al. Long-term ozone exposure and mortality in a large prospective study. Am J Respir Crit Care Med. 2016;193(10):1134–42.
Malley CS, Kuylenstierna JCI, Vallack HW, Henze DK, Blencowe H, Ashmore MR. Preterm birth associated with maternal fine particulate matter exposure: a global, regional and national assessment. Environ Int. 2017;101:173–82.
Schraufnagel DE, Balmes JR, Cowl CT, de Matteis S, Jung SH, Mortimer K, et al. Air pollution and noncommunicable diseases: a review by the Forum of International Respiratory Societies’ Environmental Committee, part 1: the damaging effects of air pollution. Chest. 2019;155(2):409–16.
Schraufnagel DE, Balmes JR, Cowl CT, de Matteis S, Jung SH, Mortimer K, et al. Air pollution and noncommunicable diseases: a review by the Forum of International Respiratory Societies’ Environmental Committee, part 2: air pollution and organ systems. Chest. 2019;155(2):417–26.
van Veldhoven K, Kiss A, Keski-Rahkonen P, Robinot N, Scalbert A, Cullinan P, et al. Impact of short-term traffic-related air pollution on the metabolome - results from two metabolome-wide experimental studies. Environ Int. 2019;123:124–31.
Liang DH, et al. Perturbations of the arginine metabolome following exposures to traffic-related air pollution in a panel of commuters with and without asthma. Environ Int. 2019;127:503–13.
de Oliveira BFA, Chacra APM, Frauches TS, Vallochi A, Hacon S. A curated review of recent literature of biomarkers used for assessing air pollution exposures and effects in humans. Journal of Toxicology and Environmental Health, Part B. 2014;17(7–8):369–410.
Kelly, F.J. and J.C. Fussell, Metabolomics as a tool to unravel the oxidative stress-induced toxicity of ambient air pollutants, in Oxidative Stress. 2020, Elsevier. p. 463–488.
Mu, L.N., et al., Metabolomics profiling before, during, and after the Beijing Olympics: a panel study of within-individual differences during periods of high and low air pollution. Environ Health Perspect, 2019. 127(5).
Ladva, C.N., et al., Particulate metal exposures induce plasma metabolome changes in a commuter panel study. PLoS One, 2018. 13(9).
Shen S, Zhang R, Zhang J, Wei Y, Guo Y, Su L, et al. Welding fume exposure is associated with inflammation: a global metabolomics profiling study. Environ Health. 2018;17(1):68.
Wei, Y., et al., Global metabolomic profiling reveals an association of metal fume exposure and plasma unsaturated fatty acids. PLoS One, 2013. 8(10).
Vlaanderen JJ, Janssen NA, Hoek G, Keski-Rahkonen P, Barupal DK, Cassee FR, et al. The impact of ambient air pollution on the human blood metabolome. Environ Res. 2017;156:341–8.
Li, H.C., et al., Particulate matter exposure and stress hormone levels a randomized, double-blind, crossover trial of air purification. Circulation, 2017. 136(7): p. 618−+.
Miller DB, Ghio AJ, Karoly ED, Bell LN, Snow SJ, Madden MC, et al. Ozone exposure increases circulating stress hormones and lipid metabolites in humans. Am J Respir Crit Care Med. 2016;193(12):1382–91.
Chen C, Li H, Niu Y, Liu C, Lin Z, Cai J, et al. Impact of short-term exposure to fine particulate matter air pollution on urinary metabolome: a randomized, double-blind, crossover trial. Environ Int. 2019;130:104878.
Zhang Y, Chu M, Zhang J, Duan J, Hu D, Zhang W, et al. Urine metabolites associated with cardiovascular effects from exposure of size-fractioned particulate matter in a subway environment: a randomized crossover study. Environ Int. 2019;130:104920.
Yan Q, Liew Z, Uppal K, Cui X, Ling C, Heck JE, et al. Maternal serum metabolome and traffic-related air pollution exposure in pregnancy. Environ Int. 2019;130:104872.
Chen C-HS, Kuo TC, Kuo HC, Tseng YJ, Kuo CH, Yuan TH, et al. Metabolomics of children and adolescents exposed to industrial carcinogenic pollutants. Environmental science & technology. 2019;53(9):5454–65.
Walker, D.I., et al., Metabolomic assessment of exposure to near-highway ultrafine particles. Journal of exposure science & environmental epidemiology, 2018: p. 1.
Yuan T-H, et al. Metabolic profiling of residents in the vicinity of a petrochemical complex. Sci Total Environ. 2016;548:260–9.
Menni C, Metrustry SJ, Mohney RP, Beevers S, Barratt B, Spector TD, et al. Circulating levels of antioxidant vitamins correlate with better lung function and reduced exposure to ambient pollution. Am J Respir Crit Care Med. 2015;191(10):1203–7.
Huang, Q., Hu D., Wang X., Chen Y., Wu Y., Pan L., Li H., Zhang J., Deng F., Guo X., Shen H., The modification of indoor PM2.5 exposure to chronic obstructive pulmonary disease in Chinese elderly people: a meet-in-metabolite analysis. Environ Int, 2018. 121: p. 1243–1252.
Chen C-HS, Yuan TH, Shie RH, Wu KY, Chan CC. Linking sources to early effects by profiling urine metabolome of residents living near oil refineries and coal-fired power plants. Environ Int. 2017;102:87–96.
Wang Z, Zheng Y, Zhao B, Zhang Y, Liu Z, Xu J, et al. Human metabolic responses to chronic environmental polycyclic aromatic hydrocarbon exposure by a metabolomic approach. J Proteome Res. 2015;14(6):2583–93.
Kuo C-H, Wang KC, Tian TF, Tsai MH, Chiung YM, Hsiech CM, et al. Metabolomic characterization of laborers exposed to welding fumes. Chem Res Toxicol. 2012;25(3):676–86.
Liang DH, et al. Use of high-resolution metabolomics for the identification of metabolic signals associated with traffic-related air pollution. Environ Int. 2018;120:145–54.
Jeong A, Fiorito G, Keski-Rahkonen P, Imboden M, Kiss A, Robinot N, et al. Perturbation of metabolic pathways mediates the association of air pollutants with asthma and cardiovascular diseases. Environ Int. 2018;119:334–45.
Maniscalco M, Paris D, Melck D, Chiariello N, di Napoli F, Manno M, et al. Biomonitoring of workers using nuclear magnetic resonance-based metabolomics of exhaled breath condensate: a pilot study. Toxicol Lett. 2018;298:4–12.
Cheng W, Duncan KE, Ghio AJ, Ward-Caviness C, Karoly ED, Diaz-Sanchez D, et al. Changes in metabolites present in lung-lining fluid following exposure of humans to ozone. Toxicol Sci. 2018;163(2):430–9.
Haggarty J, Burgess KE. Recent advances in liquid and gas chromatography methodology for extending coverage of the metabolome. Curr Opin Biotechnol. 2017;43:77–85.
Wishart DS, Tzur D, Knox C, Eisner R, Guo AC, Young N, et al. HMDB: the Human Metabolome Database. Nucleic Acids Res. 2007;35(Database issue):D521–6.
Kanehisa M, Goto S. KEGG: Kyoto Encyclopedia of Genes and Genomes. Nucleic Acids Res. 2000;28(1):27–30.
Smith CA, Maille GO??, Want EJ, Qin C, Trauger SA, Brandon TR, et al. METLIN: a metabolite mass spectral database. Ther Drug Monit. 2005;27(6):747–51.
Griffin JL, Nicholls AW, Daykin CA, Heald S, Keun HC, Schuppe-Koistinen I, et al. Standard reporting requirements for biological samples in metabolomics experiments: mammalian/in vivo experiments. Metabolomics. 2007;3(3):179–88.
Spicer RA, Salek R, Steinbeck C. Compliance with minimum information guidelines in public metabolomics repositories. Scientific data. 2017;4:170137.
Viant MR, Kurland IJ, Jones MR, Dunn WB. How close are we to complete annotation of metabolomes? Curr Opin Chem Biol. 2017;36:64–9.
Barnes S, Benton HP, Casazza K, Cooper SJ, Cui X, du X, et al. Training in metabolomics research. I. Designing the experiment, collecting and extracting samples and generating metabolomics data. J Mass Spectrom. 2016;51(7):461–75.
Barnes S, Benton HP, Casazza K, Cooper SJ, Cui X, du X, et al. Training in metabolomics research. II. Processing and statistical analysis of metabolomics data, metabolite identification, pathway analysis, applications of metabolomics and its future. J Mass Spectrom. 2016;51(8):535–48.
Di Guida R, et al. Non-targeted UHPLC-MS metabolomic data processing methods: a comparative investigation of normalisation, missing value imputation, transformation and scaling. Metabolomics. 2016;12(5):93.
Guyatt G, Oxman AD, Akl EA, Kunz R, Vist G, Brozek J, et al. GRADE guidelines: 1. Introduction-GRADE evidence profiles and summary of findings tables. J Clin Epidemiol. 2011;64(4):383–94.
Lin, E.Z., et al., The fresh air wristband: a wearable air pollutant sampler. Environmental Science & Technology Letters, 2020.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Susceptibility Factors in Environmental Health
Supplementary Information
ESM 1
(XLSX 580 kb)
Rights and permissions
About this article
Cite this article
Jin, L., Godri Pollitt, K.J., Liew, Z. et al. Use of Untargeted Metabolomics to Explore the Air Pollution-Related Disease Continuum. Curr Envir Health Rpt 8, 7–22 (2021). https://doi.org/10.1007/s40572-020-00298-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40572-020-00298-x