Abstract
Purpose
Evidence suggests that difficulties identifying and describing one’s feelings, core components of alexithymia, are associated with attitudinal and behavioral symptoms of disordered eating; depressive symptoms also may underlie these associations. Specifically, research indicates that alexithymia is positively related to depressive symptoms, which in turn may promote both disordered-eating attitudes and certain disinhibited-eating behaviors (e.g., emotional eating). Findings also suggest that military-dependent youth with high weight may exhibit elevated depressive symptoms and disordered eating. As such, understanding associations among alexithymia, depressive symptoms, and disordered eating is particularly relevant for this vulnerable population.
Methods
We examined 149 adolescent military dependents (14.4 ± 1.6y; 55.0% female; 20.0% non-Hispanic Black; BMIz: 1.9 ± 0.4) at high risk for binge-eating disorder and obesity in adulthood. Participants completed questionnaires assessing two components of alexithymia (difficulty identifying feelings [DIF] and difficulty describing feelings [DDF]), depressive symptoms, emotional eating, and trait anxiety; disordered-eating attitudes were assessed via semi-structured interview.
Results
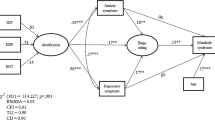
A series of regression-based models examined indirect relationships of DIF and DDF with disordered-eating attitudes and emotional eating through depressive symptoms. Bootstrapped 95% confidence intervals revealed a significant indirect path from each of the alexithymia components to disordered-eating attitudes via depressive symptoms; indirect paths to emotional eating were non-significant.
Conclusion
Results support the salience of depressive symptoms in the relationship between alexithymia and disordered-eating attitudes. Future research should utilize prospective designs and explore direct and indirect associations of alexithymia with other disordered-eating behaviors.
Level of evidence
Level III, evidence obtained from a well-designed cohort study.




Similar content being viewed by others
References
Lesser IM (1981) A review of the alexithymia concept. Psychosomat Med 43:531–543. https://doi.org/10.1097/00006842-198112000-00009
Fernandes J, Ferreira-Santos F, Miller K et al (2018) Emotional processing in obesity: a systematic review and exploratory meta-analysis. Obes Rev 19:111–120. https://doi.org/10.1111/obr.12607
Nowakowski ME, McFarlane T, Cassin S (2013) Alexithymia and eating disorders: a critical review of the literature. J Eat Disord 1:21. https://doi.org/10.1186/2050-2974-1-2
Treasure J, Schmidt U (2013) The cognitive-interpersonal maintenance model of anorexia nervosa revisited: a summary of the evidence for cognitive, socio-emotional and interpersonal predisposing and perpetuating factors. J Eat Disord 1:1–10. https://doi.org/10.1186/2050-2974-1-13
Pinna F, Sanna L, Carpiniello B (2015) Alexithymia in eating disorders: therapeutic implications. Psychol Res Behav Manag 8:1. https://doi.org/10.2147/PRBM.S52656
Courty A, Godart N, Lalanne C et al (2015) Alexithymia, a compounding factor for eating and social avoidance symptoms in anorexia nervosa. Compr Psychiatry 56:217–228. https://doi.org/10.1016/j.comppsych.2014.09.011
Karukivi M, Hautala L, Korpelainen J et al (2010) Alexithymia and eating disorder symptoms in adolescents. Eat Disord 18:226–238. https://doi.org/10.1080/10640261003719518
Ridout N, Thom C, Wallis DJ (2010) Emotion recognition and alexithymia in females with non-clinical disordered eating. Eat Behav 11:1–5. https://doi.org/10.1016/j.eatbeh.2009.07.008
Tominaga T, Choi H, Nagoshi Y et al (2014) Relationship between alexithymia and coping strategies in patients with somatoform disorder. Neuropsychiatr Dis Treat 10:55–62. https://doi.org/10.2147/NDT.S55956
Alpaslan AH, Soylu N, Kadriye A et al (2015) Disordered eating attitudes, alexithymia and suicide probability among Turkish high school girls. Psychiatry Res 226:224–229. https://doi.org/10.1016/j.psychres.2014.12.052
Conti C, Di Francesco G, Lanzara R et al (2019) Alexithymia and binge eating in obese outpatients who are starting a weight-loss program: a structural equation analysis. Eur Eat Disord Rev 27:628–640. https://doi.org/10.1002/erv.2696
de Berardis D, Serroni N, Campanella D et al (2009) Alexithymia and its relationships with dissociative experiences, body dissatisfaction and eating disturbances in a non-clinical female sample. Cogn Ther Res 33:471–479. https://doi.org/10.1007/s10608-009-9247-9
Fenwick AS, Sullivan KA (2011) Potential link between body dysmorphic disorder symptoms and alexithymia in an eating-disordered treatment-seeking sample. Psychiatry Res 189:299–304
Pinaquy S, Chabrol H, Simon C et al (2003) Emotional eating, alexithymia, and binge-eating disorder in obese women. Obes Res 11:195–201. https://doi.org/10.1038/oby.2003.31
Shank LM, Tanofsky-Kraff M, Kelly NR et al (2019) The association between alexithymia and eating behavior in children and adolescents. Appetite 142:104381. https://doi.org/10.1016/j.appet.2019.104381
Noli G, Cornicelli M, Marinari GM et al (2010) Alexithymia and eating behaviour in severely obese patients. J Hum Nutr Diet 23:616–619. https://doi.org/10.1111/j.1365-277X.2010.01079.x
Luminet O, Bagby RM, Taylor GJ (2018) Alexithymia: advances in research, theory, and clinical practice. Cambridge University Press, Cambridge
Westwood H, Kerr-Gaffney J, Stahl D et al (2017) Alexithymia in eating disorders: systematic review and meta-analyses of studies using the Toronto alexithymia scale. J Psychosom Res 99:66–81. https://doi.org/10.1016/j.jpsychores.2017.06.007
Ohmann S, Popow C, Wurzer M et al (2013) Emotional aspects of anorexia nervosa: results of prospective naturalistic cognitive behavioral group therapy. Neuropsychiatr 27:119–128. https://doi.org/10.1007/s40211-013-0065-7
Panayiotou G, Panteli M, Vlemincx E (2019) Adaptive and maladaptive emotion processing and regulation, and the case of alexithymia. Vital Health Stat. https://doi.org/10.1080/02699931.2019.1671322
Spence S, Courbasson C (2012) The role of emotional dysregulation in concurrent eating disorders and substance use disorders. Eat Behav 13:382–385. https://doi.org/10.1016/j.eatbeh.2012.05.006
Juarascio AS, Felton JW, Borges AM et al (2016) An investigation of negative affect, reactivity, and distress tolerance as predictors of disordered eating attitudes across adolescence. J Adolesc 49:91–98. https://doi.org/10.1016/j.adolescence.2016.02.005
Swart M, Kortekaas R, Aleman A (2009) Dealing with feelings: characterization of trait alexithymia on emotion regulation strategies and cognitive-emotional processing. PLoS ONE 4:e5751. https://doi.org/10.1371/journal.pone.0005751
Luminet O, Nielson KA, Ridout N (2021) Having no words for feelings: alexithymia as a fundamental personality dimension at the interface of cognition and emotion. Cogn Emot 35:435–448. https://doi.org/10.1080/02699931.2021.1916442
Chester DS, Pond RS Jr, DeWall CN (2015) Alexithymia is associated with blunted anterior cingulate response to social rejection: implications for daily rejection. Soc Cog Affect Neurosci 10:517–522. https://doi.org/10.1093/scan/nsu082
Lulé D, Schulze UME, Bauer K et al (2014) Anorexia nervosa and its relation to depression, anxiety, alexithymia and emotional processing deficits. Eat Weight Disord 19:209–216. https://doi.org/10.1007/s40519-014-0101-z
Quinton S, Wagner HL (2005) Alexithymia, ambivalence over emotional expression, and eating attitudes. Personal Individ Differ 38:1163–1173. https://doi.org/10.1016/j.paid.2004.07.013
Speranza M, Corcos M, Loas G et al (2005) Depressive personality dimensions and alexithymia in eating disorders. Psychiatr Res 135:153–163. https://doi.org/10.1016/j.psychres.2005.04.001
Berger SS, Elliott C, Ranzenhofer LM et al (2014) Interpersonal problem areas and alexithymia in adolescent girls with loss of control eating. Compr Psychiatry 55:170–178. https://doi.org/10.1016/j.comppsych.2013.08.005
Brechan I, Kvalem IL (2015) Relationship between body dissatisfaction and disordered eating: mediating role of self-esteem and depression. Eat Behav 17:49–58. https://doi.org/10.1016/j.eatbeh.2014.12.008
Maraldo TM, Zhou W, Dowling J et al (2016) Replication and extension of the dual pathway model of disordered eating: the role of fear of negative evaluation, suggestibility, rumination, and self-compassion. Eat Behav 23:187–194. https://doi.org/10.1016/j.eatbeh.2016.10.008
Porter AC, Zelkowitz RL, Cole DA (2018) The unique associations of self-criticism and shame-proneness to symptoms of disordered eating and depression. Eat Behav 29:64–67. https://doi.org/10.1016/j.eatbeh.2018.02.008
Heatherton TF, Baumeister RF (1991) Binge eating as escape from self-awareness. Psychol Bull 110:86. https://doi.org/10.1037/0033-2909.110.1.86
Fairburn CG, Cooper Z, Shafran R (2003) Cognitive behaviour therapy for eating disorders: a “transdiagnostic” theory and treatment. Behav Res Ther 41:509–528. https://doi.org/10.1016/S0005-7967(02)00088-8
Cooper MJ, Wells A, Todd G (2004) A cognitive model of bulimia nervosa. Br J Clin Psychol 43:1–16. https://doi.org/10.1348/014466504772812931
Lavender JM, Wonderlich SA, Engel SG et al (2015) Dimensions of emotion dysregulation in anorexia nervosa and bulimia nervosa: a conceptual review of the empirical literature. Clin Psychol Rev 40:111–122. https://doi.org/10.1016/j.cpr.2015.05.010
van Strien T, van de Laar FA, van Leeuwe JFJ et al (2007) The dieting dilemma in patients with newly diagnosed type 2 diabetes: does dietary restraint predict weight gain 4 years after diagnosis? Health Psychol 26:105. https://doi.org/10.1037/0278-6133.26.1.105
Arnow B, Kenardy J, Agras WS (1995) The emotional eating scale: the development of a measure to assess coping with negative affect by eating. Int J Eat Disord 18:79–90. https://doi.org/10.1002/1098-108X(199507)18:1%3c79:AID-EAT2260180109%3e3.0.CO;2-V
Tanofsky-Kraff M, Theim KR, Yanovski SZ et al (2007) Validation of the emotional eating scale adapted for use in children and adolescents (EES-C). Int J Eat Disord 40:232–240. https://doi.org/10.1002/eat.20362
Karukivi M, Pölönen T, Vahlberg T et al (2014) Stability of alexithymia in late adolescence: results of a 4-year follow-up study. Psychiatry Res 219:386–390. https://doi.org/10.1016/j.psychres.2014.05.058
Zonnevijlle-Bendek MJ, van Goozen SHM, Cohen-Kettenis PT et al (2002) Do adolescent anorexia nervosa patients have deficits in emotional functioning? Eur Child Adolesc Psychiatr 11:38–42. https://doi.org/10.1007/s007870200006
Sfärlea A, Dehning S, Keller LK et al (2019) Alexithymia predicts maladaptive but not adaptive emotion regulation strategies in adolescent girls with anorexia nervosa or depression. J Eat Disord 7:1–9. https://doi.org/10.1186/s40337-019-0271-1
Ballarotto G, Porreca A, Erriu M et al (2017) Does alexithymia have a mediating effect between impulsivity and emotional-behavioural functioning in adolescents with binge eating disorder? Clin Neuropsychiatr: J Treat Eval 14:247–256
Woodard K, Pollak SD (2020) Is there evidence for sensitive periods in emotional development? Curr Opin Behav Sci 36:1–6. https://doi.org/10.1016/j.cobeha.2020.05.004
Sawyer SM, Afifi RA, Bearinger LH et al (2012) Adolescence: a foundation for future health. Lancet 379:1630–1640. https://doi.org/10.1016/S0140-6736(12)60072-5
Lewinsohn PM, Striegel-Moore RH, Seeley JR (2000) Epidemiology and natural course of eating disorders in young women from adolescence to young adulthood. J Am Acad Child Adolesc Psychiatry 39:1284–1292. https://doi.org/10.1097/00004583-200010000-00016
Stice E, Marti CN, Shaw H et al (2009) An 8-year longitudinal study of the natural history of threshold, subthreshold, and partial eating disorders from a community sample of adolescents. J Abnorm Psych 118:587–597. https://doi.org/10.1037/a0016481
Tanofsky-Kraff M, Sbrocco T, Theim KR et al (2013) Obesity and the US military family. Obes 21:2205–2220. https://doi.org/10.1002/oby.20566
Higgins Neyland MK, Shank LM, Burke NL et al (2020) Parental deployment and distress, and adolescent disordered eating in prevention-seeking military dependents. Int J Eat Disord 53:201–209. https://doi.org/10.1002/eat.23180
Creech SK, Hadley W, Borsari B (2014) The impact of military deployment and reintegration on children and parenting: a systematic review. Prof Psychol Res Pr 45:452–464. https://doi.org/10.1037/a0035055
Schvey NA, Sbrocco T, Stephens M et al (2015) Comparison of overweight and obese military-dependent and civilian adolescent girls with loss-of-control eating. Int J Eat Disord 48:790–794. https://doi.org/10.1002/eat.22424
Waasdorp CE, Caboot JB, Robinson CA et al (2007) Screening military dependent adolescent females for disordered-eating. Mil Med 172:962–967. https://doi.org/10.7205/milmed.172.9.962
Menzel JE, Schaefer LM, Burke NL et al (2010) Appearance-related teasing, body dissatisfaction, and disordered eating: a meta-analysis. Body Image 7:261–270. https://doi.org/10.1016/j.bodyim.2010.05.004
Phillips BA, Gaudette S, McCracken A et al (2012) Psychosocial functioning in children and adolescents with extreme obesity. J Clin Psychol Med Settings 19:277–284. https://doi.org/10.1007/s10880-011-9293-9
Rankin J, Matthews L, Cobley S et al (2016) Psychological consequences of childhood obesity: psychiatric comorbidity and prevention. Adolesc Health Med Ther 7:125–146. https://doi.org/10.2147/AHMT.S101631
Stojek MMK, Tanofsky-Kraff M, Shomaker LB et al (2017) Associations of adolescent emotional and loss of control eating with 1-year changes in disordered eating, weight, and adiposity. Int J Eat Disord 50:551–560. https://doi.org/10.1002/eat.22636
Kuczmarski RJ, Ogden CL, Guo SS et al (2000) 2000 CDC growth charts for the United States. Vital Health Stat 2002:246
Sonneville KR, Horton NJ, Micali N et al (2013) Longitudinal associations between binge eating and overeating and adverse outcomes among adolescents and young adults: does loss of control matter? JAMA Pediatr 167:149–155. https://doi.org/10.1001/2013.jamapediatrics.12
Spielberger CD, Edwards CD, Lushene RE et al (1973) Preliminary manual for the state-trait anxiety inventory for children. Psychologists Press, Palo Alto, CA
Tanofsky-Kraff M, Shomaker LB, Wilfley DE et al (2017) Excess weight gain prevention in adolescents: three-year outcome following a randomized controlled trial. J Consult Clin Psychol 85:218–227. https://doi.org/10.1037/ccp0000153
Hilbert A, Hartmann AS, Czaja J et al (2013) Natural course of preadolescent loss of control eating. J Abnorm Psychol 122:684. https://doi.org/10.1037/a0033330
Rieffe C, Oosterveld P, Terwogt MM (2006) An alexithymia questionnaire for children: factorial and concurrent validation results. Personal Individ Differ 40:123–133. https://doi.org/10.1016/j.paid.2005.05.013
Bagby RM, Da Parker J, Taylor GJ (1994) The twenty-item Toronto alexithymia scale—I. Item selection and cross-validation of the factor structure. J Psychosom Res 38:23–32. https://doi.org/10.1016/0022-3999(94)90005-1
Loas G, Braun S, Delhaye M et al (2017) The measurement of alexithymia in children and adolescents: psychometric properties of the alexithymia questionnaire for children and the twenty-item Toronto alexithymia scale in different non-clinical and clinical samples of children and adolescents. PLoS ONE 12:e0177982. https://doi.org/10.1371/journal.pone.0177982
Fairburn CG, Cooper Z, O’Connor M (1993) The eating disorder examination. Int J Eat Disord 6:1–8
Vannucci A, Tanofsky-Kraff M, Shomaker LB et al (2012) Construct validity of the emotional eating scale adapted for children and adolescents. Int J Obes 36:938–943. https://doi.org/10.1038/ijo.2011.225
Kang Sim DE, Strong DR, Manzano M et al (2019) Evaluating psychometric properties of the emotional eating scale adapted for children and adolescents (EES-C) in a clinical sample of children seeking treatment for obesity: a case for the unidimensional model. Int J Obes 43:2565–2572. https://doi.org/10.1038/s41366-019-0427-8
Beck AT, Steer RA, Brown GK (1996) Manual for the Beck depression inventory-II. Psychological Corporation, San Antonio, TX
Karukivi M, Saarijärvi S (2014) Development of alexithymic personality features. World J Psychiatry 4:91–102. https://doi.org/10.5498/wjp.v4.i4.91
Visted E, Vøllestad J, Nielsen MB et al (2018) Emotion regulation in current and remitted depression: a systematic review and meta-analysis. Front Psychol 9:756. https://doi.org/10.3389/fpsyg.2018.00756
Patwardhan I, Mason WA, Chmelka MB et al (2019) Prospective relations between alexithymia, substance use and depression: findings from a national birth cohort. Nord J Psychiatry 73:340–348. https://doi.org/10.1080/08039488.2019.1634758
Gomez-Baya D, Mendoza R, Paino S et al (2017) Perceived emotional intelligence as a predictor of depressive symptoms during mid-adolescence: a two-year longitudinal study on gender differences. Personal Individ Differ 104:303–312. https://doi.org/10.1016/j.paid.2016.08.022
Salguero JM, Palomera R, Fernández-Berrocal P (2012) Perceived emotional intelligence as predictor of psychological adjustment in adolescents: a 1-year prospective study. Eur J Psychol Educ 27:21–34. https://doi.org/10.1007/s10212-011-0063-8
Hayes AF (2018) Introduction to mediation, moderation, and conditional process analysis second edition: a regression-based approach. Guilford Press, Guilford, NY
Eizaguirre AE, de Cabezón AOS, de Alda IO et al (2004) Alexithymia and its relationships with anxiety and depression in eating disorders. Personal Individ Differ 36:321–331. https://doi.org/10.1016/S0191-8869(03)00099-0
Torres S, Guerra MP, Lencastre L et al (2015) Alexithymia in anorexia nervosa: the mediating role of depression. Psychiatr Res 225:99–107. https://doi.org/10.1016/j.psychres.2014.10.023
Pink AE, Lee M, Price M et al (2019) A serial mediation model of the relationship between alexithymia and BMI: the role of negative affect, negative urgency and emotional eating. Appetite 133:270–278. https://doi.org/10.1016/j.appet.2018.11.014
Sahlan RN, Williams BM, Forrest LN et al (2020) Disordered eating, self-esteem, and depression symptoms in Iranian adolescents and young adults: a network analysis. Int J Eat Disord. https://doi.org/10.1002/eat.23365
Huang C, Chen J-H (2015) Meta-analysis of the factor structures of the Beck depression inventory–II. Assessment 22:459–472. https://doi.org/10.1177/1073191114548873
Fiorilli C, Grimaldi Capitello T, Barni D et al (2019) Predicting adolescent depression: the interrelated roles of self-esteem and interpersonal stressors. Front Psychol 10:565. https://doi.org/10.3389/fpsyg.2019.00565
Goossens L, Braet C, van Vlierberghe L et al (2009) Loss of control over eating in overweight youngsters: the role of anxiety, depression and emotional eating. Eur Eat Disord Rev 17:68–78. https://doi.org/10.1002/erv.892
van Strien T, Konttinen H, Homberg JR et al (2016) Emotional eating as a mediator between depression and weight gain. Appetite 100:216–224. https://doi.org/10.1016/j.appet.2016.02.034
Nolan LJ, Jenkins SM (2019) Food addiction is associated with irrational beliefs via trait anxiety and emotional eating. Nutrients. https://doi.org/10.3390/nu11081711
Knowles KA, Olatunji BO (2020) Specificity of trait anxiety in anxiety and depression: meta-analysis of the state-trait anxiety inventory. Clin Psychol Rev 82:101928. https://doi.org/10.1016/j.cpr.2020.101928
Schneider KL, Appelhans BM, Whited MC et al (2010) Trait anxiety, but not trait anger, predisposes obese individuals to emotional eating. Appetite 55:701–706. https://doi.org/10.1016/j.appet.2010.10.006
Elfhag K, Lundh L-G (2007) TAS-20 alexithymia in obesity, and its links to personality. Scand J Psychol 48:391–398. https://doi.org/10.1111/j.1467-9450.2007.00583.x
Preece DA, Becerra R, Robinson K et al (2020) What is alexithymia? Using factor analysis to establish its latent structure and relationship with fantasizing and emotional reactivity. J Pers 88:1162–1176. https://doi.org/10.1111/jopy.12563
Montebarocci O, Surcinelli P (2018) Correlations between TSIA and TAS-20 and their relation to self-reported negative affect: a study using a multi-method approach in the assessment of alexithymia in a nonclinical sample from Italy. Psychiatr Res 270:187–193. https://doi.org/10.1016/j.psychres.2018.09.036
Celikel FC, Kose S, Erkorkmaz U et al (2010) Alexithymia and temperament and character model of personality in patients with major depressive disorder. Compr Psychiatry 51:64–70. https://doi.org/10.1016/j.comppsych.2009.02.004
Levant RF, Hall RJ, Williams CM et al (2009) Gender differences in alexithymia. Psych Men Masc 10:190–203. https://doi.org/10.1037/a0015652
Öksüz E, Guvenc G (2018) Relationship of premenstrual and menstrual symptoms to alexithymia among nursing students. Perspect Psychiatr Care 54:391–397. https://doi.org/10.1111/ppc.12271
Ouwens MA, van Strien T, van Leeuwe JFJ (2009) Possible pathways between depression, emotional and external eating. A structural equation model. Appetite 53:245–248. https://doi.org/10.1016/j.appet.2009.06.001
van Strien T, Ouwens MA (2007) Effects of distress, alexithymia and impulsivity on eating. Eat Behav 8:251–257. https://doi.org/10.1016/j.eatbeh.2006.06.004
Margiotta FD (2019) Changing U.S. military manpower realities. Routledge, New York, NY
McMahon CJ, Bernard CJ (2019) Storm clouds on the horizon. Naval War Coll Rev 72:84–100
Steinhausen H-C, Gavez S, Winkler Metzke C (2005) Psychosocial correlates, outcome, and stability of abnormal adolescent eating behavior in community samples of young people. Int J Eat Disord 37:119–126. https://doi.org/10.1002/eat.20077
Dixon JB (2010) The effect of obesity on health outcomes. Mol Cell Endocrinol 316:104–108. https://doi.org/10.1016/j.mce.2009.07.008
Cruz-Sáez S, Pascual A, Wlodarczyk A et al (2020) The effect of body dissatisfaction on disordered eating: the mediating role of self-esteem and negative affect in male and female adolescents. J Health Psychol 25:1098–1108. https://doi.org/10.1177/1359105317748734
O’Brien KS, Latner JD, Puhl RM et al (2016) The relationship between weight stigma and eating behavior is explained by weight bias internalization and psychological distress. Appetite 102:70–76. https://doi.org/10.1016/j.appet.2016.02.032
Pearlman AT, Schvey NA, Higgins Neyland MK et al (2020) Associations between family weight-based teasing, eating pathology, and psychosocial functioning among adolescent military dependents. Int J Env Res Public Health 17:24. https://doi.org/10.3390/ijerph17010024
Schvey NA, Barmine M, Bates D et al (2017) Weight stigma among active duty US military personnel with overweight and obesity. Stigma Health 2:281. https://doi.org/10.1037/sah0000057
Disclaimer
D. Klein, B. Ford, and C. Ford are Commissioned Officers in the United States (U.S.) Air Force or Navy. The opinions and assertions expressed herein are those of the authors and are not to be construed as reflecting the views of USU, the U.S. Air Force, the U.S. Navy, or the U.S. Department of Defense.
Funding
Funding for this study was provided by NIDDK 1R01DK104115 to M. Tanofsky-Kraff and the Defense Health Agency, MED 83-10180 to M. Haigney. J. A. Yanovski is supported by the Intramural Research Program, Eunice Kennedy Shriver National Institute of Child Health and Human Development, ZIA-HD-00641. The funding sources had no role in the study design, collection, analysis or interpretation of the data, writing the manuscript, or the decision to submit the paper for publication.
Author information
Authors and Affiliations
Contributions
All authors variously contributed to the study conception, design, data collection, and/or material preparation. A. Rice performed data analyses and wrote the first draft of the manuscript. All authors commented on previous versions of the manuscript, and read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
Approval was provided by the Uniformed Services University of the Health Sciences Institutional Review Board and the Fort Belvoir Community Hospital Research Office.
Consent to participate
Informed consent and assent were obtained from parents/guardians and study participants, respectively.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rice, A., Lavender, J.M., Shank, L.M. et al. Associations among alexithymia, disordered eating, and depressive symptoms in treatment-seeking adolescent military dependents at risk for adult binge-eating disorder and obesity. Eat Weight Disord 27, 3083–3093 (2022). https://doi.org/10.1007/s40519-022-01429-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-022-01429-z