Abstract
Purpose of Review
Taste is the sensory system primarily devoted to the selection of what we eat. Various internal factors are likely involved in the modulation of taste sensitivity or homeostasis in the context of one’s general nutritional condition. For ameliorating or preventing lifestyle-related diseases, it is important to understand how our taste system is maintained and disrupted. This review focuses on insulin, the most potent anabolic agent in our body and a possible modulator of taste sensation, in the peripheral taste system.
Recent Findings
The insulin receptor is expressed in taste buds and taste progenitor/stem cells. Insulin expression itself is also reported in taste buds. Recent studies suggest that insulin signaling might contribute to the regulation of taste cell generation.
Summary
Insulin in blood circulation or in taste buds might influence taste cell turnover and certain taste sensitivities. Hyperinsulinemia is one possible cause of taste disorders frequently observed in diabetes patients.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
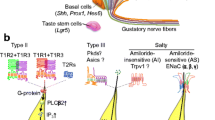
Chandrashekar J, Hoon MA, Ryba NJP, Zuker CS. The receptors and cells for mammalian taste. Nature. 2006. https://doi.org/10.1038/nature05401.
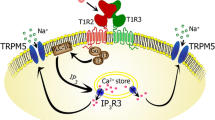
Takai S, Yoshida R, Shigemura N, Ninomiya Y. Peptide signaling in taste transduction. In: Chemosens. Transduct: Elsevier; 2016. p. 299–317.
Yoshida R, Ninomiya Y. New insights into the signal transmission from taste cells to gustatory nerve fibers. Int Rev Cell Mol Biol. 2010;279:101–34.
Roper SD, Chaudhari N. Taste buds: cells, signals and synapses. Nat Rev Neurosci. 2017. https://doi.org/10.1038/nrn.2017.68.
Huang AL, Chen X, Hoon MA, Chandrashekar J, Guo W, Tränkner D, et al. The cells and logic for mammalian sour taste detection. Nature. 2006;442:934–8.
Ishimaru Y, Inada H, Kubota M, Zhuang H, Tominaga M, Matsunami H. Transient receptor potential family members PKD1L3 and PKD2L1 form a candidate sour taste receptor. Proc Natl Acad Sci U S A. 2006;103:12569–74.
Teng B, Wilson CE, Tu Y-H, Joshi NR, Kinnamon SC, Liman Correspondence ER, et al. Cellular and neural responses to sour stimuli require the proton channel Otop1 article cellular and neural responses to sour stimuli require the Proton Channel Otop1. Curr Biol. 2019;29:3647–56.
Roper SD. Taste buds as peripheral chemosensory processors. Semin Cell Dev Biol. 2013. https://doi.org/10.1016/j.semcdb.2012.12.002.
Chaudhari N, Roper SD (2010) The cell biology of taste 190:285–296.
Ichimori Y, Ueda K, Okada H, Honma S, Wakisaka S. Histochemical changes and apoptosis in degenerating taste buds of the rat circumvallate papilla. Arch Histol Cytol. 2009;72:91–100.
Miura H, Scott JK, Harada S, Barlow LA. Sonic hedgehog -expressing basal cells are general post-mitotic precursors of functional taste receptor cells. Dev Dyn. 2014;243:1286–97.
Ohmoto M, Ren W, Nishiguchi Y, Hirota J, Jiang P, Matsumoto I. Genetic lineage tracing in taste tissues using Sox2-CreERT2 strain. Chem Senses. 2017;42:547–52.
Tanaka T, Komai Y, Tokuyama Y, Yanai H, Ohe S, Okazaki K, et al. Identification of stem cells that maintain and regenerate lingual keratinized epithelial cells. Nat Cell Biol. 2013;15:511–8.
Beidler LM, Smallman RL. Renewal of cells within taste buds. J Cell Biol. 1965;27:263–72.
Hamamichi R, Asano-Miyoshi M, Emori Y. Taste bud contains both short-lived and long-lived cell populations. Neuroscience. 2006;141:2129–38.
Perea-Martinez I, Nagai T, Chaudhari N. Functional cell types in taste buds have distinct longevities. PLoS One. 2013;8:e53399.
Yee KK, Li Y, Redding KM, Iwatsuki K, Margolskee RF, Jiang P. Lgr5-EGFP Marks taste bud stem/progenitor cells in posterior tongue. Stem Cells. 2013;31:992–1000.
Ren W, Lewandowski BC, Watson J, Aihara E, Iwatsuki K, Bachmanov AA, et al. Single Lgr5- or Lgr6-expressing taste stem/progenitor cells generate taste bud cells ex vivo. Proc Natl Acad Sci. 2014. https://doi.org/10.1073/pnas.1409064111.
Zhou Y, Liu H-X, Mistretta CM. Bone morphogenetic proteins and noggin: inhibiting and inducing fungiform taste papilla development. Dev Biol. 2006;297:198–213.
Liebl DJ, Mbiene J-P, Parada LF. NT4/5 mutant mice have deficiency in gustatory papillae and taste bud formation. Dev Biol. 1999;213:378–89.
Petersen CI, Jheon AH, Mostowfi P, Charles C, Ching S, Thirumangalathu S, et al. FGF signaling regulates the number of posterior taste papillae by controlling progenitor field size. PLoS Genet. 2011;7:e1002098.
Biggs BT, Tang T, Krimm RF. Insulin-like growth factors are expressed in the taste system, but do not maintain adult taste buds. PLoS One. 2016. https://doi.org/10.1371/journal.pone.0148315.
Lu WJ, Mann RK, Nguyen A, Bi T, Silverstein M, Tang JY, et al. Neuronal delivery of hedgehog directs spatial patterning of taste organ regeneration. Proc Natl Acad Sci U S A. 2017;115:E200–9.
Iwatsuki K, Liu H-X, Gronder A, Singer MA, Lane TF, Grosschedl R, et al. Wnt signaling interacts with Shh to regulate taste papilla development. Proc Natl Acad Sci. 2007;104:2253–8.
Saltiel AR, Kahn CR. Insulin signalling and the regulation of glucose and lipid metabolism. Nature. 2001;414:799–806.
Baquero AF, Gilbertson TA. Insulin activates epithelial sodium channel (ENaC) via phosphoinositide 3-kinase in mammalian taste receptor cells. Am J Physiol Physiol. 2011;300:C860–71.
Heck GL, Mierson S, Desimone JA. Salt taste transduction occurs through an amiloride-sensitive sodium transport pathway. Science. 1984;223:403–5.
Blazer-Yost BL, Liu X, Helman SI. Hormonal regulation of eNaCs: insulin and aldosterone. Am J Phys Cell Phys. 1998. https://doi.org/10.1152/ajpcell.1998.274.5.c1373.
Wang J, Barbry P, Maiyar AC, Rozansky DJ, Bhargava A, Leong M, et al. SGK integrates insulin and mineralocorticoid regulation of epithelial sodium transport. Am J Physiol Ren Physiol. 2001. https://doi.org/10.1152/ajprenal.2001.280.2.f303.
• Doyle ME, Fiori JL, Gonzalez Mariscal I, Liu Q-R, Goodstein E, Yang H, et al. Insulin is transcribed and translated in mammalian taste bud cells. Endocrinology. 2018;159:3331–9. Firstly discovered insulin production in oral tissue in mice and human, however they did not mentioned about its function.
Calvo SSC, Egan JM. The endocrinology of taste receptors. Nat Rev Endocrinol. 2015;11:213–27. https://doi.org/10.1038/nrendo.2015.7.
Shin Y-K, Martin B, Kim W, et al. Ghrelin is produced in taste cells and ghrelin receptor null mice show reduced taste responsivity to salty (NaCl) and sour (citric acid) tastants. PLoS One. 2010;5:e12729.
Elson AET, Dotson CD, Egan JM, Munger SD. Glucagon signaling modulates sweet taste responsiveness. FASEB J. 2010. https://doi.org/10.1096/fj.10-158105.
Yee KK, Sukumaran SK, Kotha R, Gilbertson TA, Margolskee RF. Glucose transporters and ATP-gated K+ (KATP) metabolic sensors are present in type 1 taste receptor 3 (T1r3)-expressing taste cells. Proc Natl Acad Sci U S A. 2011;108:5431–6.
Shin YK, Martin B, Golden E, Dotson CD, Maudsley S, Kim W, et al. Modulation of taste sensitivity by GLP-1 signaling. J Neurochem. 2008;106:455–63.
•• Takai S, Watanabe Y, Sanematsu K, Yoshida R, Margolskee RF, Jiang P, et al. Effects of insulin signaling on mouse taste cell proliferation. PLoS One. 2019;14:e0225190. Proved that insulin from circulation (or within taste tissue) could make impact on taste cell differentiation/proliferation with using newly developed 3-D stem cell culture of taste buds.
Dazert E, Hall MN. mTOR signaling in disease. Curr Opin Cell Biol. 2011;23:744–55.
Avruch J, Long X, Ortiz-Vega S, Rapley J, Papageorgiou A, Dai N. Amino acid regulation of TOR complex 1. Am J Physiol Metab. 2009;296:E592–602.
Ma XM, Blenis J. Molecular mechanisms of mTOR-mediated translational control. Nat Rev Mol Cell Biol. 2009;10:307–18.
Zoncu R, Efeyan A, Sabatini DM. MTOR: from growth signal integration to cancer, diabetes and ageing. Nat Rev Mol Cell Biol. 2011. https://doi.org/10.1038/nrm3025.
Hay N, Sonenberg N. Upstream and downstream of mTOR. Genes Dev. 2004;18:1926–45.
Wirawan E, Vanden Berghe T, Lippens S, Agostinis P, Vandenabeele P. Autophagy: for better or for worse. Cell Res. 2012;22:43–61.
Suzuki Y, Takeda M, Sakakura Y, Suzuki N. Distinct expression pattern of insulin-like growth factor family in rodent taste buds. J Comp Neurol. 2005;482:74–84.
Biggs BT, Tang T, Krimm RF. Insulin-like growth factors are expressed at high levels in the taste system, but do not maintain taste bud structure. Chem Senses. 2015;40:600.
Zhang C, Cotter M, Lawton A, Oakley B, Wong L, Zeng Q. Keratin 18 is associated with a subset of older taste cells in the rat. Differentiation. 1995;59:155–62.
Suzuki Y, Takeda M, Sakakura Y, Suzuki N. Distinct expression pattern of insulin-like growth factor family in rodent taste buds. J Comp Neurol. 2005;482:74–84.
Schumachers R, Mosthafs L, Schlessingerj J, Brandenburgll D, Ullrichs A (1991) THE JOURNAL OF BIOLOGICAL CHEMISTRY insulin and insulin-like growth factor-1 binding specificity is determined by distinct regions of their cognate receptors*.
Nakae J, Kido Y, Accili D Distinct and Overlapping Functions of Insulin and IGF-I Receptors.
Kawaguchi H, Murata K. Electric gustatory threshold in diabetics and its clinical significance. Nippon Jibiinkoka Gakkai Kaiho. 1995;98:1291–12961363.
Schelling JL, Tetreault L, Lasagna L, Davis M. Abnormal taste threshold in diabetes. Lancet (London, England). 1965;1:508–12.
De Carli L, Gambino R, Lubrano C, Rosato R, Bongiovanni D, Lanfranco F, et al. Impaired taste sensation in type 2 diabetic patients without chronic complications: a case–control study. J Endocrinol Investig. 2018;41:765–72.
Gondivkar SM, Indurkar A, Degwekar S, Bhowate R. Evaluation of gustatory function in patients with diabetes mellitus type 2. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;108:876–80.
Wasalathanthri S, Hettiarachchi P, Prathapan S. Sweet taste sensitivity in pre-diabetics, diabetics and normoglycemic controls: a comparative cross sectional study. BMC Endocr Disord. 2014;14:67.
Yu JH, Shin MS, Lee JR, Choi JH, Koh EH, Lee WJ, et al. Decreased sucrose preference in patients with type 2 diabetes mellitus. Diabetes Res Clin Pract. 2014;104:214–9.
Yoon M-S. The role of mammalian target of Rapamycin (mTOR) in insulin signaling. Nutrients. 2017. https://doi.org/10.3390/nu9111176.
Le Floch JP, Le Lievre G, Sadoun J, Perlemuter L, Peynegre R, Hazard J. Taste impairment and related factors in type I diabetes mellitus. Diabetes Care. 1989;12:173–8.
Hardy SL, Brennand CP, Wyse BW. Taste thresholds of individuals with diabetes mellitus and of control subjects. J Am Diet Assoc. 1981;79:286–9.
Pavlidis P, Gouveris H, Kekes G, Maurer J. Electrogustometry thresholds, tongue tip vascularization, and density and morphology of the fungiform papillae in diabetes. B-ENT. 2014;10:271–8.
Le Floch JP, Le Lièvre G, Verroust J, Philippon C, Peynegre R, Perlemuter L. Factors related to the electric taste threshold in type 1 diabetic patients. Diabet Med. 1990;7:526–31.
Abbasi AA. Diabetes: diagnostic and therapeutic significance of taste impairment. Geriatrics. 1981;36:73–8.
Negrato C, Tarzia O. Buccal alterations in diabetes mellitus. Diabetol Metab Syndr. 2010;2:1–11. https://doi.org/10.1186/1758-5996-2-3.
Takai S, Yasumatsu K, Inoue M, Iwata S, Yoshida R, Shigemura N, et al. Glucagon-like peptide-1 is specifically involved in sweet taste transmission. FASEB J. 2015. https://doi.org/10.1096/fj.14-265355.
Martin B, Dotson CD, Shin YK, Ji S, Drucker DJ, Maudsley S, et al. Modulation of taste sensitivity by GLP-1 signaling in taste buds. Ann N Y Acad Sci. 2009. https://doi.org/10.1111/j.1749-6632.2009.03920.x.
Noel CA, Sugrue M, Dando R. Participants with pharmacologically impaired taste function seek out more intense, higher calorie stimuli. Appetite. 2017;117:74–81.
Funding
This work was supported by the Japan Society for the Promotion of Science Grants-in-Aid for Scientific Research (KAKENHI) grants 17 K17938 (S.T.) and 19H03818 (N.S.). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Animal Experiments
Mouse husbandry and all mouse experiments were carried out under the ethical guidelines of Kyushu University. All experimental protocols and procedures were approved by the committee for Laboratory Animal Care and Use at Kyushu University in accordance with the National Institutes of Health Guide for the Care and Use of Laboratory Animals (approval number: A29–206).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Oral Disease and Nutrition