Abstract
Purpose of review
Mindset theory has been applied to a wide range of educational and health topics, and more recently, to addictions. The present preregistered scoping review was conducted, following the PRISMA-ScR guidelines, in order to answer three questions: (1) To what extent has mindset theory literature been linked to addiction research (including substance addiction and behavioral addiction)? (2) What interventional tools based on mindset theory have been used, in this context, in order to improve patients’ health, and to what effects? (3) What gaps and limitations exist in today’s literature, and where to guide future research in order to properly assess the effects of mindset theory on addictions?
Recent findings
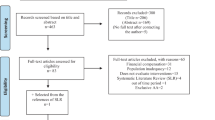
Database search included APA PsychINFO and PubMed, and a manual search was also conducted. A total of 1903 documents were reviewed. Screening processes resulted in the inclusion of 18 articles. Analysis revealed that the field is still in a nascent state. More research is needed in order to properly evaluate the effect of mindset theory on addictions. Mindset interventions and manipulations have seldom been implemented. Most studies used cross-sectional designs, preventing from making causal inferences. Studies were also limited by the use of self-report data. Questions were raised concerning the hypothesis of similarity and specificity between mindset and addiction, and the place of mindset theory within known addiction frameworks.
Summary
The present scoping review points out that more research, using intervention procedure and objective data collection, should be conducted in order to properly assess the impact of mindset theory on addictions.

Similar content being viewed by others
Data availability
Data regarding this review (i.e., Zotero Database) is available at: https://osf.io/35fa6/?view_only=dba2a59fa0a44e3e9c36ebaeb38f608c
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Dweck CS. Mindsets and human nature: promoting change in the Middle East, the schoolyard, the racial divide, and willpower. Am Psychol. 2012;67(8):614–22. https://doi.org/10.1037/a0029783.
Dweck CS, Leggett EL. A social-cognitive approach to motivation and personality. Psychol Rev. 1988;95(2):256–73. https://doi.org/10.1037/0033-295X.95.2.256.
Yeager DS, Hanselman P, Walton GM, Murray JS, Crosnoe R, Muller C, Tipton E, Schneider B, Hulleman CS, Hinojosa CP, Paunesku D, Romero C, Flint K, Roberts A, Trott J, Iachan R, Buontempo J, Yang SM, Carvalho CM, … Dweck CS. A national experiment reveals where a growth mindset improves achievement. Nature, 2019;573(7774), 364–369. https://doi.org/10.1038/s41586-019-1466-y
Burnette JL. Implicit theories of body weight: entity beliefs can weigh you down. Pers Soc Psychol Bull. 2010;36(3):410–22. https://doi.org/10.1177/0146167209359768.
Burnette JL, Finkel EJ. Buffering against weight gain following dieting setbacks: an implicit theory intervention. J Exp Soc Psychol. 2012;48(3):721–5. https://doi.org/10.1016/j.jesp.2011.12.020.
Schleider J, Weisz J. A single-session growth mindset intervention for adolescent anxiety and depression: 9-month outcomes of a randomized trial. J Child Psychol Psychiatry. 2018;59(2):160–70. https://doi.org/10.1111/jcpp.12811.
Burnette JL, Knouse LE, Vavra DT, O’Boyle E, Brooks MA. Growth mindsets and psychological distress: a meta-analysis. Clin Psychol Rev. 2020;77:101816. https://doi.org/10.1016/j.cpr.2020.101816.
• Burnette JL, Forsyth RB, Desmarais SL, Hoyt CL. Mindsets of addiction: implications for treatment intentions. J Soc Clin Psychol. 2019;38(5):367–94. https://doi.org/10.1521/jscp.2019.38.5.367. This study is one of the first to properly develop the rationale between mindset theory and addiction and to propose a mindset manipulation in relation with addiction outcomes.
Sridharan V, Shoda Y, Heffner JL, Bricker J. Addiction mindsets and psychological processes of quitting smoking. Subst Use Misuse. 2019;54(7):1086–95. https://doi.org/10.1080/10826084.2018.1555259.
Wang C, Luo J, Nie P, Wang D. Growth mindset can reduce the adverse effect of substance use on adolescent reasoning. Front Psychol. 2019;10. https://doi.org/10.3389/fpsyg.2019.01852.
Chatters R, Cooper K, Day E, Knight M, Lagundoye O, Wong R, Kaltenthaler E. Psychological and psychosocial interventions for cannabis cessation in adults: a systematic review. Addiction Research & Theory. 2016;24(2):93–110. https://doi.org/10.3109/16066359.2015.1073719.
Sileo KM, Miller AP, Wagman JA, Kiene SM. Psychosocial interventions for reducing alcohol consumption in sub-Saharan African settings: a systematic review and meta-analysis. Addiction. 2021;116(3):457–73. https://doi.org/10.1111/add.15227.
Crescenzo FD, Ciabattini M, D’Alò GL, Giorgi RD, Giovane CD, Cassar C, Janiri L, Clark N, Ostacher MJ, Cipriani A. Comparative efficacy and acceptability of psychosocial interventions for individuals with cocaine and amphetamine addiction: a systematic review and network meta-analysis. PLoS Med. 2018;15(12):e1002715. https://doi.org/10.1371/journal.pmed.1002715.
Quilty LC, Wardell JD, Thiruchselvam T, Keough MT, Hendershot CS. Brief interventions for problem gambling: a meta-analysis. PLoS ONE. 2019;14(4):1–17. https://doi.org/10.1371/journal.pone.0214502.
Wild TC, Hammal F, Hancock M, Bartlett NT, Gladwin KK, Adams D, Loverock A, Hodgins DC. Forty-eight years of research on psychosocial interventions in the treatment of opioid use disorder: a scoping review. Drug Alcohol Depend. 2021;218:108434. https://doi.org/10.1016/j.drugalcdep.2020.108434.
American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders (5th ed.). https://doi.org/10.1176/appi.books.9780890425596
Grant JE, Chamberlain SR. Expanding the definition of addiction: DSM-5 vs. ICD-11. CNS Spectrums. 2016;21(4):300–3. https://doi.org/10.1017/S1092852916000183.
Momen NC, Plana-Ripoll O, Agerbo E, Benros ME, Børglum AD, Christensen MK, Dalsgaard S, Degenhardt L, Jonge de P, Debost J-CPG, Fenger-Grøn M, Gunn JM, Iburg KM, Kessing LV, Kessler RC, Laursen TM, Lim CCW, Mors O, Mortensen PB … McGrath JJ. Association between mental disorders and subsequent medical conditions. N Engl J Med. 2020; https://doi.org/10.1056/NEJMoa1915784.
Plana-Ripoll O, Pedersen CB, Holtz Y, Benros ME, Dalsgaard S, Jonge de P, Fan CC, Degenhardt L, Ganna A, Greve AN, Gunn J, Iburg KM, Kessing LV, Lee BK, Lim CCW, Mors O, Nordentoft M, Prior A, Roest AM … McGrath JJ. Exploring comorbidity within mental disorders among a Danish national population. JAMA Psychiat. 2019; 76(3) 259-270. https://doi.org/10.1001/jamapsychiatry.2018.3658.
Santucci K. Psychiatric disease and drug abuse. Curr Opin Pediatr. 2012;24(2):233–7. https://doi.org/10.1097/MOP.0b013e3283504fbf.
Lim SS, Vos T, Flaxman AD, Danaei G, Shibuya K, Adair-Rohani H, Amann M, Anderson HR, Andrews KG, Aryee M, Atkinson C, Bacchus LJ, Bahalim AN, Balakrishnan K, Balmes J, Barker-Collo S, Baxter A, Bell ML, Blore JD … Memish ZA. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet (London, England). 2012;380(9859): 2224-2260. https://doi.org/10.1016/S0140-6736(12)61766-8.
Peacock A, Leung J, Larney S, Colledge S, Hickman M, Rehm J, Giovino GA, West R, Hall W, Griffiths P, Ali R, Gowing L, Marsden J, Ferrari AJ, Grebely J, Farrell M, Degenhardt L. Global statistics on alcohol, tobacco and illicit drug use: 2017 status report. Addiction. 2018;113(10):1905–26. https://doi.org/10.1111/add.14234.
West R, McEwen A, Bolling K, Owen L. Smoking cessation and smoking patterns in the general population: a 1-year follow-up. Addiction (Abingdon, England). 2001;96(6):891–902. https://doi.org/10.1046/j.1360-0443.2001.96689110.x.
Holden C. ‘Behavioral’ addictions: do they exist? Science. 2001;294(5544):980–2. https://doi.org/10.1126/science.294.5544.980.
Marks I. Behavioural (non-chemical) addictions. Br J Addict. 1990;85(11):1389–94. https://doi.org/10.1111/j.1360-0443.1990.tb01618.x.
• Shaffer, H. J., & Shaffer, P. M. (2016). Behavioral addiction. In Encyclopedia of Mental Health (pp. 135–142). Elsevier. https://doi.org/10.1016/B978-0-12-397045-9.00077-XThis paper argues for the inclusion of a broad range of problematic behaviors as behavioral addictions.
Hyman SE, Malenka RC, Nestler EJ. Neural mechanisms of addiction: the role of reward-related learning and memory. Annu Rev Neurosci. 2006;29(1):565–98. https://doi.org/10.1146/annurev.neuro.29.051605.113009.
Ujhelyi Gomez K, Goodwin L, Jackson L, Jones A, Chisholm A, Rose AK. Are psychosocial interventions effective in reducing alcohol consumption during pregnancy and motherhood? A systematic review and meta-analysis. Addiction. 2021;116(7):1638–63. https://doi.org/10.1111/add.15296.
Sisk VF, Burgoyne AP, Sun J, Butler JL, Macnamara BN. To what extent and under which circumstances are growth mind-sets important to academic achievement? Two meta-analyses. Psychological Science. 2018;29(4):549–71. https://doi.org/10.1177/0956797617739704.
Blackwell LS, Trzesniewski KH, Dweck CS. Implicit theories of intelligence predict achievement across an adolescent transition: a longitudinal study and an intervention. Child Dev. 2007;78(1):246–63. https://doi.org/10.1111/j.1467-8624.2007.00995.x.
Burnette JL, O’Boyle EH, VanEpps EM, Pollack JM, Finkel EJ. Mind-sets matter: a meta-analytic review of implicit theories and self-regulation. Psychol Bull. 2013;139(3):655–701. https://doi.org/10.1037/a0029531.
Claro S, Paunesku D, Dweck CS. Growth mindset tempers the effects of poverty on academic achievement. Proc Natl Acad Sci. 2016;113(31):8664–8. https://doi.org/10.1073/pnas.1608207113.
Yeager DS, Johnson R, Spitzer BJ, Trzesniewski KH, Powers J, Dweck CS. The far-reaching effects of believing people can change: implicit theories of personality shape stress, health, and achievement during adolescence. J Pers Soc Psychol. 2014;106(6):867–84. https://doi.org/10.1037/a0036335.
Parada S, Verlhiac J-F. Growth mindset intervention among French university students, and its articulation with proactive coping strategies. Educ Psychol. 2021;1–20. https://doi.org/10.1080/01443410.2021.1917519.
• Sridharan V, Shoda Y, Heffner J, Bricker J. A pilot randomized controlled trial of a web-based growth mindset intervention to enhance the effectiveness of a smartphone app for smoking cessation. JMIR Mhealth Uhealth. 2019;7(7):e14602. https://doi.org/10.2196/14602. This study is one of the first to propose a growth mindset intervention and assess its effects on addiction outcomes.
Michie S, Richardson M, Johnston M, Abraham C, Francis J, Hardeman W, Eccles MP, Cane J, Wood CE. The behavior change technique taxonomy (v1) of 93 hierarchically clustered techniques: building an international consensus for the reporting of behavior change interventions. Ann Behav Med. 2013;46(1):81–95. https://doi.org/10.1007/s12160-013-9486-6.
Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D, Moher D, Peters MDJ, Horsley T, Weeks L, Hempel S, Akl EA, Chang C, McGowan J, Stewart L, Hartling L, Aldcroft A, Wilson MG, Garritty C … Straus SE. PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med. 2018;169(7)467-473. https://doi.org/10.7326/M18-0850.
Arksey H, O’Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(1):19–32. https://doi.org/10.1080/1364557032000119616.
Levac D, Colquhoun H, O’Brien KK. Scoping studies: advancing the methodology. Implement Sci. 2010;5(1):69. https://doi.org/10.1186/1748-5908-5-69.
Lindgren KP, Burnette JL, Hoyt CL, Peterson KP, Neighbors C. Growth mindsets of alcoholism buffer against deleterious effects of drinking identity on problem drinking over time. Alcohol Clin Exp Res. 2020;44(1):233–43. https://doi.org/10.1111/acer.14237.
Thai CL, Rice EL, Taber JM, Kaufman AR, Klein WMP. Implicit theories of smoking and association with interest in quitting among current smokers. J Behav Med. 2020;43(4):544–52. https://doi.org/10.1007/s10865-019-00058-9.
Bőthe B, Baumgartner C, Schaub MP, Demetrovics Z, Orosz G. Hands-off: feasibility and preliminary results of a two-armed randomized controlled trial of a web-based self-help tool to reduce problematic pornography use. J Behav Addict, 2021;1(aop). https://doi.org/10.1556/2006.2021.00070.
Bőthe B, Tóth-Király I, Demetrovics Z, Orosz G. The pervasive role of sex mindset: beliefs about the malleability of sexual life is linked to higher levels of relationship satisfaction and sexual satisfaction and lower levels of problematic pornography use. Pers Individ Differ. 2017;117:15-22.psyh. https://doi.org/10.1016/j.paid.2017.05.030.
Champagne J, Gardner B, Dommett EJ. Modelling predictors of UK undergraduates’ attitudes towards smart drugs. Trends in Neuroscience and Education. 2019;14:33–9. https://doi.org/10.1016/j.tine.2019.02.001.
Fitz CC. Thinking it can get better makes it better: lay theories of prejudice and substance use willingness among undergraduate students of color (2015–99020–350; Issues 7-B(E)) 2015 [ProQuest Information & Learning]. psyh. https://search.ebscohost.com/login.aspx?direct=true&db=psyh&AN=2015-99020-350&lang=fr&site=ehost-live. Accessed 7 Feb 2022.
Fitz CC, Kaufman A, Moore PJ. Lay theories of smoking and young adult nonsmokers’ and smokers’ smoking expectations. J Health Psychol. 2015;20(4):438–45. https://doi.org/10.1177/1359105313502694.
Grand AM. Implicit beliefs about the malleability of substance abuse: implications for treatment motivation and outcome (2001–95006–085; Issues 9-B) 2001 [ProQuest Information & Learning]. psyh. https://search.ebscohost.com/login.aspx?direct=true&db=psyh&AN=2001-95006-085&lang=fr&site=ehost-live. Accessed 7 Feb 2022.
Japutra A, Song Z. Mindsets, shopping motivations and compulsive buying: insights from China. J Consum Behav. 2020. https://doi.org/10.1002/cb.1821.
Johnson VD. Growth mindset as a predictor of smoking cessation (2010–99011–153; Issues 7-A) 2010 [ProQuest Information & Learning]. Psyh. https://search.ebscohost.com/login.aspx?direct=true&db=psyh&AN=2010-99011-153&lang=fr&site=ehost-live. Accessed 7 Feb 2022.
Lindgren KP, Baldwin SA, Ramirez JJ, Olin CC, Peterson KP, Wiers RW, Teachman BA, Norris J, Kaysen D, Neighbors C. Self-control, implicit alcohol associations, and the (lack of) prediction of consumption in an alcohol taste test with college student heavy episodic drinkers. PLoS ONE. 2019;14(1):e0209940. https://doi.org/10.1371/journal.pone.0209940.
Schroder HS, Dawood S, Yalch MM, Donnellan MB, Moser JS. Evaluating the domain specificity of mental health–related mind-sets. Social Psychological and Personality Science. 2016;7(6):508–20. https://doi.org/10.1177/1948550616644657.
Thai CL, Coa KI, Kaufman AR. Implicit theories of smoking and association with current smoking status. J Health Psychol. 2018;23(9):1234–9. https://doi.org/10.1177/1359105316648483.
Zeldman A, Ryan RM, Fiscella K. Motivation, autonomy support, and entity beliefs: their role in methadone maintenance treatment. J Soc Clin Psychol. 2004;23(5):675-696.psyh. https://doi.org/10.1521/jscp.23.5.675.50744.
Paunesku D, Walton GM, Romero C, Smith EN, Yeager DS, Dweck CS. Mind-set interventions are a scalable treatment for academic underachievement. Psychol Sci. 2015;26(6):784–93. https://doi.org/10.1177/0956797615571017.
Yeager DS, Romero C, Paunesku D, Hulleman CS, Schneider B, Hinojosa C, Lee HY, O’Brien J, Flint K, Roberts A, Trott J, Greene D, Walton GM, Dweck CS. Using design thinking to improve psychological interventions: the case of the growth mindset during the transition to high school. J Educ Psychol. 2016;108(3):374–91. https://doi.org/10.1037/edu0000098.
Dweck CS (1999) Self-theories: Their role in motivation, personality, and development. Psychology Press
Dweck CS, Chiu C, Hong Y. Implicit theories and their role in judgments and reactions: a word from two perspectives. Psychol Inq. 1995;6(4):267–85. https://doi.org/10.1207/s15327965pli0604_1.
McLellan AT, Kushner H, Metzger D, Peters R, Smith I, Grissom G, Pettinati H, Argeriou M. The fifth edition of the addiction severity index. J Subst Abuse Treat. 1992;9(3):199–213. https://doi.org/10.1016/0740-5472(92)90062-s.
Collins RL, Parks GA, Marlatt GA. Social determinants of alcohol consumption: the effects of social interaction and model status on the self-administration of alcohol. J Consult Clin Psychol. 1985;53(2):189–200. https://doi.org/10.1037/0022-006X.53.2.189.
World Health Organization. AUDIT: the Alcohol Use Disorders Identification Test : guidelines for use in primary health care (WHO/MSD/MSB/01.6a). World Health Organization. 200 1. https://apps.who.int/iris/handle/10665/67205. Accessed 14 Mar 2022.
White HR, Labouvie EW. Towards the assessment of adolescent problem drinking. J Stud Alcohol. 1989;50(1):30–7. https://doi.org/10.15288/jsa.1989.50.30.
Pilkonis PA, Yu L, Colditz J, Dodds N, Johnston KL, Maihoefer C, Stover AM, Daley DC, McCarty D. Item banks for alcohol use from the patient-reported outcomes measurement information system (PROMIS®): use, consequences, and expectancies. Drug Alcohol Depend. 2013;130(1–3):167–77. https://doi.org/10.1016/j.drugalcdep.2012.11.002.
Brown RL, Rounds LA. Conjoint screening questionnaires for alcohol and other drug abuse: criterion validity in a primary care practice. Wis Med J. 1995;94(3):135–40.
Siu AFY. Validation of the substance use risk profile scale for adolescents in Hong Kong. J Psychoeduc Assess. 2011;29(1):75–83. https://doi.org/10.1177/0734282910362044.
Heatherton TF, Kozlowski LT, Frecker RC, Fagerström KO. The Fagerström test for nicotine dependence: a revision of the Fagerström tolerance questionnaire. Br J Addict. 1991;86(9):1119–27. https://doi.org/10.1111/j.1360-0443.1991.tb01879.x.
Bőthe B, Tóth-Király I, Zsila Á, Griffiths MD, Demetrovics Z, Orosz G. The development of the problematic pornography consumption scale (PPCS). J Sex Res. 2018;55(3):395–406. https://doi.org/10.1080/00224499.2017.1291798.
Ridgway NM, Kukar-Kinney M, Monroe KB (2008) An expanded conceptualization and a new measure of compulsive buying. https://doi.org/10.1086/591108.
Desmarais SL, Van Dorn RA, Sellers BG, Young MS, Swartz MS. Accuracy of self-report, biological tests, collateral reports and clinician ratings in identifying substance use disorders among adults with schizophrenia. Psychol Addict Behav. 2013;27(3):774–87. https://doi.org/10.1037/a0031256.
Hughes JS. Support for the domain specificity of implicit beliefs about persons, intelligence, and morality. Personality Individ Differ. 2015;86:195–203. https://doi.org/10.1016/j.paid.2015.05.042.
Ajzen I. Constructing a TpB questionnaire: conceptual and methodological considerations. Undefined. 2002 https://www.semanticscholar.org/paper/Constructing-a-TpB-Questionnaire%3A-Conceptual-and-Ajzen/6074b33b529ea56c175095872fa40798f8141867. Accessed 17 Mar 2022.
Volkow ND, Koob GF, McLellan AT. Neurobiologic advances from the brain disease model of addiction. N Engl J Med. 2016;374(4):363–71. https://doi.org/10.1056/NEJMra1511480.
Volkow ND, Koob G. Brain disease model of addiction: why is it so controversial? The Lancet Psychiatry. 2015;2(8):677–9. https://doi.org/10.1016/S2215-0366(15)00236-9.
Heather N, Best D, Kawalek A, Field M, Lewis M, Rotgers F, Wiers RW, Heim D. Challenging the brain disease model of addiction: European launch of the addiction theory network. Addiction Research & Theory. 2018;26(4):249–55. https://doi.org/10.1080/16066359.2017.1399659.
Leshner AI. Addiction is a brain disease, and it matters. Science (New York, NY). 1997;278(5335):45–7. https://doi.org/10.1126/science.278.5335.45.
Satel S, Lilienfeld SO. Addiction and the brain-disease fallacy. Front Psych. 2014;4:141. https://doi.org/10.3389/fpsyt.2013.00141.
Lebowitz MS, Appelbaum PS. Beneficial and detrimental effects of genetic explanations for addiction. Int J Soc Psychiatry. 2017;63(8):717–23. https://doi.org/10.1177/0020764017737573.
Wiens TK, Walker LJ. The chronic disease concept of addiction: helpful or harmful? Addiction Research & Theory. 2015;23(4):309–21. https://doi.org/10.3109/16066359.2014.987760.
Heyman GM, Mims V. What addicts can teach us about addiction: a natural history approach. In Addiction and Choice: Oxford University Press; 2016. https://doi.org/10.1093/acprof:oso/9780198727224.003.0021.
Kourgiantakis T, Ashcroft R. Family-focused practices in addictions: a scoping review protocol. BMJ Open. 2018;8(1):e019433. https://doi.org/10.1136/bmjopen-2017-019433.
Funding
This research was supported by the National Cancer Institute (Institut National du Cancer—INCa_16214).
Author information
Authors and Affiliations
Contributions
Sacha Parada had the original idea for the article, Sacha Parada and Jean-François Verlhiac performed the literature search and data analysis, Sacha Parada drafted the article, Eve Legrand critically revised the work, Elsa Taschini, Xavier Laqueille and Jean-François Verlhiac reviewed and validated the final draft.
Corresponding author
Ethics declarations
Ethical Approval
This research was exempted of the Ethics Committee Approval due to the nature of the paper (scoping review).
Conflict of Interest
The authors have no conflict of interest to declare. Authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this manuscript.
Preregistration
This study’s design and analysis plan were preregistered; see https://osf.io/m6fdt/
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Emotion and Addiction
Public health significance statements: This review found that mindset theory and interventions are increasingly being studied in relation to substance and behavior addiction. Results on addiction outcomes are encouraging, but more research is needed to fully assess their impact.
Rights and permissions
About this article
Cite this article
Parada, S., Legrand, E., Taschini, E. et al. Dweck’s Mindset Theory Applied to Addictions: a Scoping Review. Curr Addict Rep 9, 133–150 (2022). https://doi.org/10.1007/s40429-022-00427-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40429-022-00427-6