Abstract
Background
Chemotherapy for Acute Lymphoblastic Leukemia (ALL) is known to render children immuno-deficient. A concomitant suppression of local defence mechanisms, such as saliva may further aggravate the adverse consequences of chemotherapy. The present study was conducted to evaluate alterations in salivary flow rate, pH and buffering capacity and to correlate these parameters with Absolute Neutrophil Counts (ANC).
Methods
A cohort of 43 patients, aged 3–12 years were evaluated for the aforementioned parameters at baseline, post-induction and post-consolidation phases. Salivary collection was done and ANC was measured from routine haematological reports.
Results
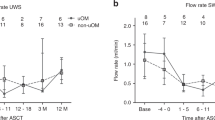
A decrease in the salivary parameters was observed at the end of Induction phase as compared to baseline, with a statistically significant decrease in unstimulated salivary flow rates (p < 0.01). Statistically significant positive correlations were found between ANC and salivary flow rate (p = 0.005), pH (p < 0.00) and buffering capacity (p < 0.00). On testing the significance of these correlations, all the values for these parameters were found to be statistically significant.
Conclusion
Salivary parameters showed derangements over the phases of chemotherapy, with maximum decrease at the end of induction phase. The positive correlations of salivary parameters with ANC of the subjects may be considered indicative of a concomitant immunological compromise in these children.

Similar content being viewed by others
Data availability
Yes.
References
Anirudhan D, Bakhshi S, Xess I, Broor S, Arya LS, et al. Etiology and outcome of oral mucosal lesions in children on chemotherapy for acute lymphoblastic leukemia. Indian Pediatr. 2008;45(1):47–51.
Arora RS, Arora B. Acute leukemia in children: a review of the current Indian data. South Asian J Cancer. 2016;5(3):155–60.
Carlén A, Hassan H, Lingström P. The ‘strip method’: a simple method for plaque pH assessment. Caries Res. 2010;44:341–4.
Ericson D, Bratthall D. Simplified method to estimate salivary buffer capacity. Eur J Oral Surg. 1989. https://doi.org/10.1111/j.1600-0722.1989.tb01453.x.
Francisconi CF, Caldas RJ, Oliveira Martins LJ, Fischer Rubira CM, da Silva Santos PS. Leukemic oral manifestations and their management. Asian Pac J Cancer Prev. 2016;17(3):911–5.
Hegde AM, Joshi S, Rai K, Shetty S. Evaluation of oral hygiene status, salivary characteristics and dental caries experience in acute lymphoblastic leukemic (ALL) children. J Clin Pediatr Dent. 2011;35(3):319–23.
Hong CH, Napeñas JJ, Hodgson BD, Stokman MA, Mathers-Stauffer V, Elting LS, et al. A systematic review of dental disease in patients undergoing cancer therapy. Support Care Cancer. 2010;18(8):1007–21.
Inaba H, Greaves M, Mullighan CG, et al. Acute lymphoblastic leukaemia. Lancet. 2013;381(9881):1943–55.
Kapoor G, Goswami M, Sharma S, Mehta A, Dhillon JK. Assessment of oral health status of children with Leukemia: a cross-sectional study. Spec Care Dentist. 2019;39(6):564–71.
Llena-Puy C. The rôle of saliva in maintaining oral health and as an aid to diagnosis. Med Oral Patol Oral Cir Bucal. 2006;11(5):449–55.
Mathur VP, Dhillon JK, Kalra G. Oral health in children with leukemia. Indian J Palliat Care. 2012;18(1):12–8.
Mishra R, Kapur A. A tailor-made approach for providing oral care to children undergoing chemotherapy: is it the need of the hour. Spec Care Dentist. 2021;41(4):140–1.
Narula G, Prasad M, Jatia S, Subramaniam PG, Patkar N, Tembhare P, et al. Clinico epidemiological profiles, clinical practices, and the impact of holistic care interventions on outcomes of pediatric hematolymphoid malignancies—a 7-year audit of the pediatric hematolymphoid disease management group at Tata Memorial Hospital. 2017;54(4):609–15.
Navazesh M, Christensen CM. A comparison of whole mouth resting and stimulated salivary measurement procedures. J Den Res. 1982;61(10):1158–62.
Ou-Yang LW, Chang PC, Tsai AI, Jaing TH, Lin SY. Salivary microbial counts and buffer capacity in children with acute lymphoblastic leukemia. Pediatr Dent. 2010;32(3):218–22.
Pajari U, Larmas M, Lanning M. Caries incidence and prevalence in children receiving antineoplastic therapy. Caries Res. 1988;22(5):318–20.
Parkin DM, Stefan C. Editorial: childhood cancer in sub-Saharan Africa. Ecancermedicalscience. 2017;11:69.
Pels E, Mielnik-Błaszczak M. Oral hygiene in children suffering from acute lymphoblastic leukemia living in rural and urban regions. Ann Agric Environ Med. 2012;19(3):529–33.
Schmiegelow K, Nersting J, Nielsen SN, Heyman M, Wesenberg F, Kristinsson J, et al. Maintenance therapy of childhood acute lymphoblastic leukemia revisited-should drug doses be adjusted by white blood cell, neutrophil, or lymphocyte counts? Pediatr Blood Cancer. 2016;63(12):2104–11.
Sil A, Betkerur J, Das NK. P-value demystified. Indian Dermatol Online J. 2019;10(6):745–50.
Squier CA. Oral complications of cancer therapies. Mucosal Alterations NCI Monogr. 1990;9:169–72.
Terwilliger T, Abdul-Hay M. Acute lymphoblastic leukemia: a comprehensive review and update. Blood Cancer J. 2017;7(6):577.
van der Velden WJ, Herbers H, Netea MG, Blijlevens NM. Mucosal barrier injury, fever and infection in neutropenic patients with cancer: introducing the paradigm febrile mucositis. Br J Haematol. 2014;167(4):441–52.
Wilberg P, Kanellopoulos A, Ruud E, Hjermstad MJ, Fosså SD, Herlofson BB. Dental abnormalities after chemotherapy in long-term survivors of childhood acute lymphoblastic leukemia 7–40 years after diagnosis. Support Care Cancer. 2016;24(4):1497–506.
Funding
None.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. The first draft of the manuscript was written by RM and all authors commented on previous versions of the manuscript. RM: conception, Study design, acquisition of data, analysis and interpretation. AK: conception, study design analysis and interpretation. AG: study design, analysis and interpretation. KG: conception, study design. AT: acquisition of data, analysis and interpretation. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mishra, R., Kapur, A., Goyal, A. et al. Salivary parameters and their correlation with neutrophil counts in children with acute lymphoblastic leukemia. Eur Arch Paediatr Dent 23, 281–287 (2022). https://doi.org/10.1007/s40368-021-00679-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40368-021-00679-2