Abstract
Background
Visualisation of the third dimension has been reported to increase effectiveness of correctly diagnosing traumatic dental injuries.
Aim
To assess the ability of paediatric dentists to detect and diagnose Traumatic Dental Injuries (TDI) using two different imaging modalities, intraoral radiographs (2D) and CBCT scans (3D). In addition, observer’s confidence regarding the obtained diagnosis, using either technique, was assessed.
Material and methods
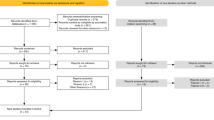
Both 2D and 3D images of 20 dental trauma cases in children were presented in random order to a panel of thirteen paediatric dentists. Observers received instructions for the screening of the images for radiographic findings related to dental trauma, using structured scoring sheets for 2D and 3D images. Observed data were compared to those recorded by two experienced benchmark observers. A ten-point scale was used for assessing observer’s confidence regarding their final diagnosis using 2D versus 3D images.
Results
Performance of individual observers showed wide variation. Statistical significance was reached for correctly detected and correctly diagnosed findings (p = 0.02), in favor of 3D. Most of the observers reported comparable confidence using 2D and 3D, two observers were more confident using 3D and one observer was more confident using 2D.
Conclusions
Paediatric dentist’s ability to detect and diagnose findings in patients with TDI was higher on 3D images. Most observers showed a similar confidence score of their diagnostic performance both on 2D and on 3D.


Similar content being viewed by others
References
Al-Salehi SK, Horner K. Impact of cone beam computed tomography (CBCT) on diagnostic thinking in endodontics of posterior teeth: a before—after study. J Dent. 2016;53:57–63.
Andreasen F, Andreasen J, Tsukiboshi M, Cohenca N (2019) Examination and diagnosis of dental injuries, in Textbook and color atlas of traumatic injuries of the teeth (5th ed), Oxford, Blackwell Munksgaard. Chapter 12; Pp 295–326.
Balasundaram A, Shah P, Hoen M, Wheater M, Bringas J, Gartner A, Geist J. Comparison of cone-beam computed tomography and periapical radiography in predicting treatment decision for periapical lesions: a clinical study. Int J Dent. 2012;2012:1–8.
Belmans N, Gilles L, Vermeesen R, Virag P, Hedesiu M, Salmon B, Baatout S, Lucas S, Lambrichts I, Jacobs R, Moreels M, DIMITRA Research Group. Quantification of DNA double strand breaks and oxidation response in children and adults undergoing dental CBCT scan. Sci Rep. 2020;10(1):2113.
Bornstein MM, Wölner-Hanssen AB, Sendi P. Comparison of intraoral radiography and limited cone beam computed tomography for the assessment of root-fractured permanent teeth. Dent Traumatol. 2009;25:571–7.
Brown J, Jacobs R, Levring Jäghagen E, Lindh C, Baksi G, Schulze D, Schulze R. Basic training requirements for the use of dental CBCT by dentists: a position paper prepared by the European Academy of DentoMaxilloFacial Radiology. Dentomaxillofacial Radiol. 2014;43:1–7.
Cohenca N, Silberman A. Contemporary imaging for the diagnosis and treatment of traumatic dental injuries: a review. Dent Traumatol. 2017;33:321–8.
Cohenca N, Simon J, Roges R, Morag Y, Malfaz J. Clinical indications for digital imaging in dento-alveolar trauma. Part 1: traumatic injuries. Dent Traumatol. 2007;23:95–104.
da Silva E, de Fátima NM, Queiroz M, Leles C. Factors influencing student’s performance in a Brazilian dental school. Braz Dent. 2010;21:80–6.
Doğan MS, Callea M, Kusdhany LS, Aras A, Maharani DA, Mandasari M, Adiatman M, Yavuz I. The evaluation of root fracture with Cone Beam Computed Tomography (CBCT): an Epidemiological Study. J Clin Exp Dent. 2018;10:e41-48.
Dunning D, Heath C, Suls JM. Flawed self-assessment: implications for health, education, and the workplace. Psychol Sci Public Interest. 2004;5:69–106.
Dutra KL, Haas L, Porporatti AL, Flores-Mir C, Nascimento Santos J, Mezzomo LA, Corrêa M, De Luca CG. Diagnostic accuracy of cone-beam computed tomography and conventional radiography on apical periodontitis: a systematic review and meta-analysis. J Endod. 2016;42:356–64.
Ee J, Fayad M, Johnson B. Comparison of endodontic diagnosis and treatment planning decisions using cone-beam volumetric tomography versus periapical radiography. J Endod. 2014;40:910–6.
EzEldeen M, Stratis A, Coucke W, Codari M, Politis C, Jacobs R. As low dose as sufficient quality: optimization of cone-beam computed tomographic scanning protocol for tooth autotransplantation planning and follow-up in children. J Endod. 2017;43:210–7.
Flores MT, Andersson L, Andreasen JO, et al. Guidelines for the management of traumatic dental injuries. I. Fractures and luxations of permanent teeth. Dent Traumatol. 2007;23:66–71.
Glendor U. Epidemiology of traumatic dental injuries a 12 year review of the literature. Dent Traumatol. 2008;24:603–11.
Horner K, Barry S, Dave M, Dixon C, Littlewood A, Pang CL, Sengupta A, Srinivasan V. Diagnostic efficacy of cone beam computed tomography in paediatric dentistry: a systematic review. Eur Arch Paediatr Dent. 2020;21:407–26.
Kühnisch J, Anttonen V, Duggal MS, Loizides Spyridonos M, Rajasekharan S, Sobczak M, Stratigaki E, Van Acker JWG, Aps JKM, Horner K, Tsiklakis K. Best clinical practice guidance for prescribing dental radiographs in children and adolescents: an EAPD policy document. Eur Arch Paediatr Dent. 2020;21:375–86.
Kullman L, Al SM. Guidelines for dental radiography immediately after a dento-alveolar trauma, a systematic literature review. Dent Traumatol. 2012;28:193–9.
Lam R. Epidemiology and outcomes of traumatic dental injuries: a review of the literature. Aus Dent J. 2016;61(1 Suppl):4–20.
Lima TF, Gamba TO, Zaia AA, Soares AJ. Evaluation of cone beam computed tomography and periapical radiography in the diagnosis of root resorption. Aust Dent J. 2016;61:425–31.
Lin S, Pilosof N, Karawani M, Wigler R, Kaufman AY, Teich ST. Occurrence and timing of complications following traumatic dental injuries: a retrospective study in a dental trauma department. J Clin Exp Dent. 2016;8:e429-436.
Mota de Almeida FJ, Knutsson K, Flygare L. The effect of cone beam CT (CBCT) on therapeutic decision-making in endodontics. Dentomaxillofacial Radiol. 2014;43:1–8.
Mota de Almeida FJ, Knutsson K, Flygare L. The impact of cone beam computed tomography on the choice of endodontic diagnosis. Int Endod J. 2015;48:564–72.
Oenning A, Jacobs R, Pauwels R, Stratis A, Hedesiu M, Salmon B, DIMITRA Research Group (2018) Cone-beam CT in paediatric dentistry: DIMITRA project position statement. Pediatr Radiol. 48:308–316. http://www.dimitra.be.
Pauwels R, Beinsberger J, Collaert B, Theodorakou C, Rogers J, Walker A, Cockmartin L, Bosmans H, Jacobs R, Bogaerts R, Horner K. Sedentexct project consortium. Effective dose range for dental cone beam computed tomography scanners. Eur J Radiol. 2012;81:267–71.
Pauwels R, Cockmartin L, Ivanauskaité D, Urboniené A, Gavala S, Donta C, Tsiklakis K, Jacobs R, Bosmans H, Bogaerts R, Horner K. The SEDENTEXCT Project Consortium. Estimating cancer risk from dental cone-beam CT exposures based on skin dosimetry. Phys Med Biol. 2014;59:3877–91.
Plohl N. Musil B Do I know as much as I think I do? The Dunning-Kruger effect, overclaiming, and the illusion of knowledge. Horizons Psychol. 2018;27:20–30.
Scarfe WC, Li Z, Aboelmaaty W, Scott SA, Farman AG. Maxillofacial cone beam computed tomography: essence, elements and steps to interpretation. Aust Dent J. 2012;57(Suppl 1):46–60.
Siegel J, Sacks B, Pennington C, Welsh J. Dose optimization to minimize radiation risk for children undergoing CT and nuclear medicine imaging is misguided and detrimental. J Nucl Med. 2017;58:865–8.
Theodorakou C, Walker A, Horner K, Pauwels R, Bogaerts R, Jacobs R, SEDENTEXCT Project Consortium. Estimation of paediatric organ and effective doses from dental cone beam CT using anthropomorphic phantoms. Br J Radiol. 2012;85:153–60.
Yamashita FC, Previdelli ITS, Pavan NNO, Endo MS. Retrospective study on sequelae in traumatized permanent teeth. Eur J Dent. 2017;11:275–80.
Yendreka VC, Fonseca GM. A “borderline” dental trauma with 12 y of evolution justifying CBCT as diagnostic method. Biomed Res. 2018;29:2800–5.
Acknowledgements
The authors are grateful to all participating paediatric dentists and to Wim Coucke for his contribution to data analysis.
Author information
Authors and Affiliations
Contributions
DD, ML and GVG designed the research setup; ML and GVG collected the data; ML, GVG, DD and RJ analysed and interpreted the data; G.V.G. drafted the paper; and all authors critically revised the manuscript prior to its submission.
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflicts of interest and completed the conflict of interest disclosure.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Van Gorp, G., Lambrechts, M., Jacobs, R. et al. Paediatric dentist’s ability to detect and diagnose dental trauma using 2D versus 3D imaging. Eur Arch Paediatr Dent 22, 699–705 (2021). https://doi.org/10.1007/s40368-021-00611-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40368-021-00611-8