Abstract
Aim
To assess the effectiveness of topically-administered haemocoagulase (batroxobin) (HC) following dental extractions in children.
Design
Split-mouth design, where either HC (test) or Normal Saline (control) (NS) was administered to children (5–9 years) requiring bilateral extractions of primary molars. Participants were randomised to (i) extraction sequence; (ii) test-solution administered thereafter. Outcome measure: time taken (in seconds) for complete cessation of bleeding.
Results
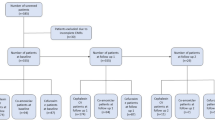
Thirty participants completed the trial receiving HS (n = 30) and NS (n = 30). No adverse events were reported. Time to bleeding cessation was lower in HS group (82.5 ± 13.99 s) than NS group (240.5 ± 54.34 s). Difference between groups (paired t test) was statistically very highly significant (P = 0.000).
Conclusion
Topical HC produced significant reductions in time for haemostasis and was clinically effective in controlling haemorrhage from extraction wounds in children. HC may be favourably utilised by paediatric dentists, especially with pre-cooperative or special-healthcare-needs patients, improving patient care.


Similar content being viewed by others
References
Alape-Giron A, Sanz L, Escolano J, et al. Snake venomics of the lancehead pitviper Bothrops asper: geographic, individual, and ontogenetic variations. J Proteome Res. 2008;7(8):3556–71. https://doi.org/10.1021/pr800332p.
Aslam S, Francis PG, Rao BH, et al. A double blind study on the efficacy of local application of hemocoagulase solution in wound healing. J Contemp Dent Pract. 2013;14(3):394–400.
Blomqvist M, Ek U, Fernell E, et al. Cognitive ability and dental fear and anxiety. Eur J Oral Sci. 2013;121(2):117–20. https://doi.org/10.1111/eos.12028.
Bruck H, Salem G. Reptilase, a hemostatic for prophylaxis and therapy in surgical operations. Wien Klin Wochenschr. 1954;66(22):395–7.
de Nicola P. Comments on Botropase®. haemostatic drugs: a critical appraisal. Dordrecht: Springer; 1977. pp. 94–9.
Eli I, Schwartz-Arad D, Bartal Y. Anxiety and ability to recognize clinical information in dentistry. J Dent Res. 2008;87(1):65–8. https://doi.org/10.1177/154405910808700111.
Harvey AL. Snake peptides. In: Kastin AJ, editor. Handbook of biologically active peptides. USA: Academic Press; 2013. p. 451–60.
Huang DX, Gai LY, Wang SR, et al. Defibrase, a purified fibrinolytic protease from snake venom in acute myocardial infarction. Acta Cardiol. 1992;47(5):445–58.
Joshi SA, Gadre KS, Halli R, Shandilya R. Topical use of Hemocoagulase (Reptilase): a simple and effective way of managing post-extraction bleeding. Ann Maxillofac Surg. 2014;4(1):119. https://doi.org/10.4103/2231-0746.133082.
Karapetian H. Reptilase time (RT). Methods Mol Biol (Clifton NJ). 2013;992:273–7. https://doi.org/10.1007/978-1-62703-339-8_20.
Klingberg G, Berggren U, Carlsson SG, Noren JG. Child dental fear: cause-related factors and clinical effects. Eur J Oral Sci. 1995;103(6):405–12.
Lowe O. Communicating with parents and children in the dental office. J Calif Dent Assoc. 2013;41(8):597–601.
Maeda M, Satoh S, Suzuki S, et al. Expression of cDNA for batroxobin, a thrombin-like snake venom enzyme. J Biochem. 1991;109(4):632–7.
Majumder K, Rao SJKD, et al. Effiacy of haemocoagulase as a topical haemostatic agent after minor oral surgical procedures—a Prospective Study. Int J Clin Med. 2014;5:875–83.
McCleary RJR, Kang TS, Kini RM. Reptile venoms as a platform for drug development. In: King GF, editor. Venoms to drugs: venom as a source for the development of human therapeutics. Cambridge: The Royal Society of Chemistry; 2015. pp. 129–62.
Mendoza-Mendoza A, Perea MB, Yanez-Vico RM, Iglesias-Linares A. Dental fear in children: the role of previous negative dental experiences. Clin Oral Investig. 2015;19(3):745–51. https://doi.org/10.1007/s00784-014-1380-5.
Ramos-Jorge J, Marques LS, Homem MA, et al. Degree of dental anxiety in children with and without toothache: prospective assessment. Int J Paediatr Dent. 2013;23(2):125–30. https://doi.org/10.1111/j.1365-263X.2012.01234.x.
Sanders JM, Holtkamp CA, Buchanan GR. The bleeding time may be longer in children than in adults. Am J Pediatr Hematol/Oncol. 1990;12(3):314–8.
Shenoy AK, Ramesh KV, Chowta MN, Adhikari PM, Rathnakar UP. Effects of botropase on clotting factors in healthy human volunteers. Perspect Clin Res. 2014;5(2):71–4. https://doi.org/10.4103/2229-3485.128024.
Slagboom J, Kool J, Harrison RA, Casewell NR. Haemotoxic snake venoms: their functional activity, impact on snakebite victims and pharmaceutical promise. Br J Haematol. 2017;177(6):947–59. https://doi.org/10.1111/bjh.14591.
Solanki DA, Modha ND. Role of hemo-coagulase as a local hemostatic agent after extraction of tooth. Int J Res Med. 2015;4(3):14–7.
Stocker K. Defibrinogenation with thrombin-like snake venom enzymes. In: Markwardt F, editor. Fibrinolytics and antifibrinolytics. Berlin Heidelberg: Springer; 1978. pp. 451–84.
ten Berg M. Dental fear in children: clinical consequences. Suggested behaviour management strategies in treating children with dental fear. Eur Arch Paediatr Dent. 2008;9(Suppl 1):41–6.
Vasiliki B, Konstantinos A, Nikolaos K, et al. Relationship between child and parental dental anxiety with child’s psychological functioning and behavior during the administration of local anesthesia. J Clin Pediatr Dent. 2016;40(6):431–7. https://doi.org/10.17796/1053-4628-40.6.431.
Wang Z, Li J, Cao L, et al. Hypofibrinogenemia caused by long-term administration of hemocoagulase: three cases report and literature review. Zhonghua Xue Ye Xue Za Zhi. 2014;35(1):50–2. https://doi.org/10.3760/cma.j.issn.0253-2727.2014.01.013.
Weiner AA. Anxiety sensitivity levels: a predictor of treatment compliance or avoidance. J Mass Dent Soc. 2013;62(1):18–20.
Wilson S. Management of child patient behavior: quality of care, fear and anxiety, and the child patient. J Endod. 2013;39(3 Suppl):73-7. https://doi.org/10.1016/j.joen.2012.11.040.
Xu YY, Ma XH, Zhang SJ. Hemocoagulase agkistrodon-induced anaphylactic shock: a case report and literature review. Int J Clin Pharmacol Ther. 2016;54(2):129–34. https://doi.org/10.5414/cp202296.
You WK, Choi WS, Koh YS, et al. Functional characterization of recombinant batroxobin, a snake venom thrombin-like enzyme, expressed from Pichia pastoris. FEBS Lett. 2004;571(1–3):67–73. https://doi.org/10.1016/j.febslet.2004.06.060.
Acknowledgements
The authors thank Mrs. Pallavi Nachinolkar (Statistician) for her assistance with Statistical computations, and Dr. Vinayak Kamath (Department of Public Health Dentistry) for his advice on study design and sample-size calculations. We also place on record our appreciation of the parents and children who participated in the study.
Funding
None.
Author information
Authors and Affiliations
Contributions
We declare that all authors have made substantial contributions. DFS and ESB conceived the idea, collected the data, and analysed the data; DFS and SR critically reviewed and formulated the study design, and analysed the data; DFS led the manuscript writing; all the authors revised and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional (Institutional Review Board Certificate Number ETHICAL COMM./GDCH/2017-1/PEDO-1) and national research committee (Registration Number: CTRI/2017/09/009784) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Trial status and registration: Closed trial. Clinical Trials Registry of India, Registration number: CTRI/2017/09/009784.
Rights and permissions
About this article
Cite this article
Swamy, D.F., Barretto, E.S. & Rodrigues, J.S.L. Effectiveness of topical haemocoagulase as a haemostatic agent in children undergoing extraction of primary teeth: a split-mouth, randomised, double-blind, clinical trial. Eur Arch Paediatr Dent 20, 311–317 (2019). https://doi.org/10.1007/s40368-018-0406-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40368-018-0406-0