Abstract
Background
In this study, we tested the feasibility of an interviewer-assisted analytic hierarchy process (AHP) in a special patient population with age-related macular degeneration (AMD).
Objectives
One aim was to generate preference weights regarding AMD treatment characteristics. A secondary aim was to explore the consistency of preference judgments and reasons for inconsistency.
Methods
We generated quantitative importance weights for decision criteria using the matrix multiplication method. A qualitative study component in the form of asking patients to think aloud throughout their judgments was implemented to facilitate understanding of quantitative findings. Consistency ratios were calculated as a measure of logical judgment performance within AHP. If consistency ratios exceeded 0.2, we explored reasons for inconsistency.
Results
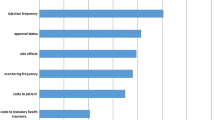
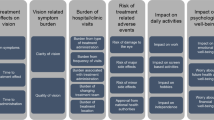
We interviewed 86 patients and generated preference weights for criteria. Patients rated the injection’s effect on visual function the highest (0.44), followed by the frequency of monitoring visits (0.18), approval status (0.13), injection frequency (0.13), and side effects (0.12). Inconsistency in judgments was prevalent at the subcriteria level. Whereas much of the observed inconsistency was due to an excessive use of high/extreme value judgments, these judgments seemed to result from patients reasonably trying to highlight their strong preferences.
Conclusion
Our study combines quantitative with qualitative data to explore patients’ preference weights and decision processes using the AHP. It suggests that the type of inconsistency observed in judgments of AMD patients mostly results from rational decision making, not from error or lack of understanding. Further research should address which type and extent of inconsistency might be acceptable in different AHP settings.



Similar content being viewed by others
References
Bridges JF, Hauber AB, Marshall D, Lloyd A, Prosser LA, Regier DA, et al. Conjoint analysis applications in health—a checklist: a report of the ISPOR Good Research Practices for Conjoint Analysis Task Force. Value Health. 2011;14(4):403–13. doi:10.1016/j.jval.2010.11.013.
Johnson RF, Lancsar E, Marshall D, Kilambi V, Muhlbacher A, Regier DA, et al. Constructing experimental designs for discrete-choice experiments: report of the ISPOR Conjoint Analysis Experimental Design Good Research Practices Task Force. Value Health. 2013;16(1):3–13. doi:10.1016/j.jval.2012.08.2223.
Liberatore MJ, Nydick RL. The analytic hierarchy process in medical and health care decision making: a literature review. Eur J Oper Res. 2008;189(1):194–207.
de Bekker-Grob EW, Ryan M, Gerard K. Discrete choice experiments in health economics: a review of the literature. Health Econ. 2012;21(2):145–72. doi:10.1002/hec.1697.
Marsh K, Lanitis T, Neasham D, Orfanos P, Caro J. Assessing the value of healthcare interventions using multi-criteria decision analysis: a review of the literature. Pharmacoeconomics. 2014;32(4):345–65. doi:10.1007/s40273-014-0135-0.
Clark MD, Determann D, Petrou S, Moro D, de Bekker-Grob EW. Discrete choice experiments in health economics: a review of the literature. Pharmacoeconomics. 2014;32(9):883–902.
Maruthur NM, Joy S, Dolan J, Segal JB, Shihab HM, Singh S. Systematic assessment of benefits and risks: study protocol for a multi-criteria decision analysis using the Analytic Hierarchy Process for comparative effectiveness research. F1000Res. 2013;2:160. doi:10.12688/f1000research.2-160.v1.
Maruthur NM, Joy SM, Dolan JG, Shihab HM, Singh S. Use of the analytic hierarchy process for medication decision-making in type 2 diabetes. PloS One. 2015;10(5):e0126625. doi:10.1371/journal.pone.0126625.
Danner M, Hummel JM, Volz F, van Manen JG, Wiegard B, Dintsios CM, et al. Integrating patients’ views into health technology assessment: Analytic hierarchy process (AHP) as a method to elicit patient preferences. Int J Technol Assess Health Care. 2011;27(4):369–75. doi:10.1017/S0266462311000523.
Ho MP, Gonzalez JM, Lerner HP, Neuland CY, Whang JM, McMurry-Heath M, et al. Incorporating patient-preference evidence into regulatory decision making. Surg Endosc. 2015;29(10):2984–93. doi:10.1007/s00464-014-4044-2.
Hummel JM, Bridges JF, IJzerman MJ. Group decision making with the analytic hierarchy process in benefit-risk assessment: a tutorial. Patient. 2014;7(2):129–40.
Saaty TL. A scaling method for priorities in hierarchical structures. J Math Psychol. 1977;15(3):234–281. doi:10.1016/0022-2496(77)90033-5.
Saaty TL. Highlights and critical points in the theory and application of the Analytic Hierarchy Process. Eur J Oper Res. 1994;74(3):426–447. doi:10.1016/0377-2217(94)90222-4.
Angelis A, Kanavos P. Value-based assessment of new medical technologies: towards a robust methodological framework for the application of multiple criteria decision analysis in the context of health technology assessment. Pharmacoeconomics. 2016;34(5):435–46. doi:10.1007/s40273-015-0370-z.
Saaty TL. Fundamentals of decision making and prority theory with the Analytic Hierarchy Process. Analytic hierarchy process series, vol 6. Pittsburgh: RWS Publications; 2011.
Dolan JG, Isselhardt BJ Jr, Cappuccio JD. The analytic hierarchy process in medical decision making: a tutorial. Med Decis Making. 1989;9(1):40–50.
Reddy BP, Kelly MP, Thokala P, Walters SJ, Duenas A. Prioritising public health guidance topics in the National Institute for Health and Care Excellence using the analytic hierarchy process. Public Health. 2014;128(10):896–903. doi:10.1016/j.puhe.2014.07.003.
van Til JA, Renzenbrink GJ, Dolan JG, Ijzerman MJ. The use of the analytic hierarchy process to aid decision making in acquired equinovarus deformity. Arch Phys Med Rehabil. 2008;89(3):457–62. doi:10.1016/j.apmr.2007.09.030.
Hummel JM, Snoek GJ, van Til JA, van Rossum W, Ijzerman MJ. A multicriteria decision analysis of augmentative treatment of upper limbs in persons with tetraplegia. J Rehabil Res Dev. 2005;42(5):635–44.
Benaim C, Perennou DA, Pelissier JY, Daures JP. Using an analytical hierarchy process (AHP) for weighting items of a measurement scale: a pilot study. Rev Epidemiol Sante Publique. 2010;58(1):59–63. doi:10.1016/j.respe.2009.09.004.
Dolan JG, Boohaker E, Allison J, Imperiale TF. Can streamlined multicriteria decision analysis be used to implement shared decision making for colorectal cancer screening? Med Decis Making. 2013;34(6):746–55. doi:10.1177/0272989X13513338.
Dolan JG, Boohaker E, Allison J, Imperiale TF. Patients’ preferences and priorities regarding colorectal cancer screening. Med Decis Making. 2013;33(1):59–70. doi:10.1177/0272989X12453502.
Muhlbacher AC, Bethge S, Kaczynski A, Juhnke C. Objective criteria in the medicinal therapy for type II diabetes: an analysis of the patients’ perspective with analytic hierarchy process and best-worst scaling. Gesundheitswesen. 2015. doi:10.1055/s-0034-1390474 (Epub 8 Apr 2015).
Kuruoglu E, Guldal D, Mevsim V, Gunvar T. Which family physician should I choose? The analytic hierarchy process approach for ranking of criteria in the selection of a family physician. BMC Med Inform Decis Making. 2015;15:63. doi:10.1186/s12911-015-0183-1.
Hummel MJ, Volz F, van Manen JG, Danner M, Dintsios CM, Ijzerman MJ, et al. Using the analytic hierarchy process to elicit patient preferences: prioritizing multiple outcome measures of antidepressant drug treatment. Patient. 2012;5(4):225–37. doi:10.2165/11635240-000000000-00000.
Ijzerman MJ, van Til JA, Bridges JF. A comparison of analytic hierarchy process and conjoint analysis methods in assessing treatment alternatives for stroke rehabilitation. Patient. 2012;5(1):45–56.
IJzerman MJ, van Til JA, Snoek GJ. Comparison of two multi-criteria decision techniques for eliciting treatment preferences in people with neurological disorders. Patient. 2008;1(4):265–72.
Schmidt-Erfurth U, Chong V, Loewenstein A, Larsen M, Souied E, Schlingemann R, et al. Guidelines for the management of neovascular age-related macular degeneration by the European Society of Retina Specialists (EURETINA). Br J Ophthalmol. 2014;98(9):1144–67. doi:10.1136/bjophthalmol-2014-305702.
Schmid MK, Bachmann LM, Fas L, Kessels AG, Job OM, Thiel MA. Efficacy and adverse events of aflibercept, ranibizumab and bevacizumab in age-related macular degeneration: a trade-off analysis. Br J Ophthalmol. 2015;99(2):141–6. doi:10.1136/bjophthalmol-2014-305149.
Moja L, Lucenteforte E, Kwag KH, Bertele V, Campomori A, Chakravarthy U, et al. Systemic safety of bevacizumab versus ranibizumab for neovascular age-related macular degeneration. Cochrane Database Syst Rev. 2014;9:CD011230. doi:10.1002/14651858.CD011230.pub2.
Danner M, Vennedey V, Hiligsmann M, Fauser S, Stock S. Focus groups in elderly ophthalmologic patients: setting the stage for quantitative preference elicitation. Patient. 2016;9(1):47–57. doi:10.1007/s40271-015-0122-3.
Orme BK. Getting started with conjoint analysis: strategies for product design and pricing research. Madison, WI: Research Publishers; 2010.
Forman E, Peniwati K. Aggregating individual judgements and priorities with the analytic hierarchy process. Eur J Oper Res. 1998;108:165-169. doi:10.1016/S0377-2217(97)00244-0.
Forman EH. Random indices for incomplete pairwise comparison matrices. Eur J Oper Res. 1990. doi:10.1016/0377-2217(90)90072-J.
Forman E. Expert choice: comparison help document. Expert Choice; 2015.
Forman E, Selly MA. Decision by objectives (How to convince others that you are right). World Scientific Publishing; 2001.
Droege KM, Caramoy A, Kersten A, Luberichs-Fauser J, Zilkens K, Müller D, et al. Patient preference of ranibizumab treatment regimen for neovascular age-related macular degeneration—monthly injections versus pro re nata. Graefes Arch Clin Exp Ophthalmol. 2014;252(1):31–4.
Mueller S, Agostini H, Ehlken C, Bauer-Steinhusen U, Hasanbasic Z, Wilke T. Patient preferences in the treatment of neovascular age-related macular degeneration a discrete choice experiment. Ophthalmology. 2016;123(4):876–83. doi:10.1016/j.ophtha.2015.12.001.
Baxter JM, Fotheringham AJ, Foss AJ. Determining patient preferences in the management of neovascular age-related macular degeneration: a conjoint analysis. Eye. 2016. doi:10.1038/eye.2016.18.
Holder RD. Some comments on the analytic hierarchy process. J Oper Res Soc. 1990;41(11):1073–6. doi:10.2307/2582904.
Dong Y, Xu Y, Li H, Dai M. A comparative study of the numerical scales and the prioritization methods in AHP. Eur J Oper Res. 2008;186(1):229–42. doi:10.1016/j.ejor.2007.01.044.
Ji P, Jiang R. Scale transitivity in the AHP. J Oper Res Soc. 2003;54(8):896–905.
Ishizaka A, Balkenborg D, Kaplan T. Influence of aggregation and measurement scale on ranking a compromise alternative in AHP. J Oper Res Soc 2011;62(4):700–10.
Finan JS, Hurley WJ. Transitive calibration of the AHP verbal scale. Eur J Oper Res. 1999;112(2):367–72. doi:10.1016/S0377-2217(97)00411-6.
Lootsma FA. Conflict resolution via pairwise comparison of concessions. Eur J Oper Res. 1989;40(1):109–16. doi:10.1016/0377-2217(89)90278-6.
Harker PT, Vargas LG. The theory of ratio scale estimation: Saaty’s analytic hierarchy process. Manag Sci. 1987;33(11):1383–403. doi:10.1287/mnsc.33.11.1383.
Helm R, Steiner M, Scholl A, Manthey L. A Comparative empirical study on common methods for measuring preferences. Jena Schr Wirtsch. 2004. doi:10.1504/IJMDM.2008.017408.
Hummel JM, Steuten LG, Groothuis-Oudshoorn CJ, Mulder N, Ijzerman MJ. Preferences for colorectal cancer screening techniques and intention to attend: a multi-criteria decision analysis. Appl Health Econ Health Policy. 2013;11(5):499–507. doi:10.1007/s40258-013-0051-z.
Kinoshita E. Why we need AHP/ANP instead of utility theory in today’s complex world—AHP from the perspective of bounded rationality. The International Society on the Analytic Hierarchy Process (ISAHP). 2005. http://www.isahp.org/2005Proceedings/Papers/KinoshitaE_AHP&ANPvsUtilityTheory.pdf. Accessed 29 May 2016.
Acknowledgments
The authors thank Dirk Müller, Philipp Müther, and Fabian Jülich for their input during study design; Fabian Jülich and Markos-Charalabos Dintsios for their review of the final manuscript; and Sabrina Liebner and Fatjana Bylo for their support during patient recruitment. The authors would also like to thank all patients for their participation.
Authors contributions
Marion Danner and Vera Vennedey conducted and analyzed the AHP interviews and drafted the manuscript. Christian Gross supported data analyses. Mickaël Hilligsmann and Sascha Fauser critically revised and contributed to the final manuscript. Stephanie Stock facilitated the project. Marion Danner acts as guarantor for the content of the paper.
Funding
Financial support for this investigator-initiated study was provided by Bayer Vital GmbH, Germany (who markets the product aflibercept). The funding agreement ensured the author’s independence in designing the study; collecting, analyzing, and interpreting the data; and writing and publishing the report. The authors Stephanie Stock, Christian Gross, Sascha Fauser, Mickaël Hiligsmann, Vera Vennedey, and Marion Danner report no additional conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Danner, M., Vennedey, V., Hiligsmann, M. et al. How Well Can Analytic Hierarchy Process be Used to Elicit Individual Preferences? Insights from a Survey in Patients Suffering from Age-Related Macular Degeneration. Patient 9, 481–492 (2016). https://doi.org/10.1007/s40271-016-0179-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40271-016-0179-7