Abstract
Background
There is limited information on the risks and benefits of anticoagulation in patients with atrial fibrillation receiving peritoneal dialysis.
Objective
The aim was to determine the risk of mortality, ischemic stroke, and bleeding associated with warfarin use in patients with atrial fibrillation receiving peritoneal dialysis.
Patients and methods
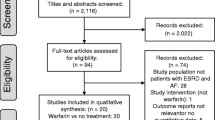
This is a retrospective observational study of a multi-ethnic cohort of patients with atrial fibrillation receiving peritoneal dialysis in the United States. Using a dialysis registry, we identified 476 patients with atrial fibrillation receiving peritoneal dialysis. Among these patients, 115 (24%) were treated with warfarin. Cox proportional hazard models were used to compare risks of mortality, ischemic stroke and bleeding between the groups.
Results
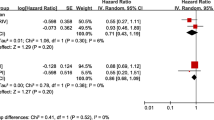
Compared to untreated patients, patients receiving warfarin were older (67.3 ± 10.8 vs 62.9 ± 13.3 years) and more likely to be white (42% vs 31%). Prevalence of comorbidities including hypertension, hyperlipidemia, diabetes, heart failure, and prior ischemic stroke were similar between the two groups. All cause mortality rates were 19.9 per 100 person-years in the warfarin group and 21.0 per 100 person-years in the untreated group. There was no difference between groups in the risk of mortality [hazard ratio (HR) 0.8, 95% confidence interval (CI) 0.53–1.2, p = 0.28], ischemic stroke (HR 2.3, 95% CI 0.94–5.4, p = 0.07), hemorrhagic stroke (HR 2.0, 95% CI 0.32–12.8, p = 0.46), gastrointestinal bleeding (HR 0.92, 95% CI 0.39–2.2, p = 0.86), or any bleeding (HR 1.2, 95% 0.60–2.3, p = 0.65). Even in the subgroup of patients with > 70% time in therapeutic range, no association was seen between warfarin treatment and mortality.
Conclusion
There is no significant association between warfarin treatment with risks of mortality, ischemic stroke or bleeding in patients with atrial fibrillation receiving peritoneal dialysis.


Similar content being viewed by others
References
Davis RC, Hobbs FD, Kenkre JE, et al. Prevalence of atrial fibrillation in the general population and in high-risk groups: the ECHOES study. Europace. 2012;14(11):1553–9.
Zimmerman D, Sood MM, Rigatto C, Holden RM, Hiremath S, Clase CM. Systematic review and meta-analysis of incidence, prevalence and outcomes of atrial fibrillation in patients on dialysis. Nephrol Dial Transpl. 2012;27(10):3816–22.
Genovesi S, Pogliani D, Faini A, et al. Prevalence of atrial fibrillation and associated factors in a population of long-term hemodialysis patients. Am J Kidney Dis. 2005;46(5):897–902.
Wetmore JB, Mahnken JD, Rigler SK, et al. The prevalence of and factors associated with chronic atrial fibrillation in Medicare/Medicaid-eligible dialysis patients. Kidney Int. 2012;81(5):469–76.
Hart RG, Pearce LA, Aguilar MI. Meta-analysis: antithrombotic therapy to prevent stroke in patients who have nonvalvular atrial fibrillation. Ann Intern Med. 2007;146(12):857–67.
Kirchhof P, Benussi S, Kotecha D, et al. 2016 ESC Guidelines for the management of atrial fibrillation developed in collaboration with EACTS. Eur Heart J. 2016;37(38):2893–962.
Winkelmayer WC, Liu J, Setoguchi S, Choudhry NK. Effectiveness and safety of warfarin initiation in older hemodialysis patients with incident atrial fibrillation. Clin J Am Soc Nephrol. 2011;6(11):2662–8.
Shah M, Avgil Tsadok M, Jackevicius CA, et al. Warfarin use and the risk for stroke and bleeding in patients with atrial fibrillation undergoing dialysis. Circulation. 2014;129(11):1196–203.
Bonde AN, Lip GY, Kamper AL, et al. Net clinical benefit of antithrombotic therapy in patients with atrial fibrillation and chronic kidney disease: a nationwide observational cohort study. J Am Coll Cardiol. 2014;64(23):2471–82.
January CT, Wann LS, Alpert JS, et al. 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines and the Heart Rhythm Society. Circulation. 2014;130(23):2071–104.
Turakhia MP, Blankestijn PJ, Carrero JJ, et al. Chronic kidney disease and arrhythmias: conclusions from a Kidney Disease: improving Global Outcomes (KDIGO) Controversies Conference. Eur Heart J. 2018;39(24):2314–25.
Chan PH, Huang D, Yip PS, et al. Ischaemic stroke in patients with atrial fibrillation with chronic kidney disease undergoing peritoneal dialysis. Europace. 2016;18(5):665–71.
Koebnick C, Langer-Gould AM, Gould MK, et al. Sociodemographic characteristics of members of a large, integrated health care system: comparison with US Census Bureau data. Perm J. 2012;16(3):37–41.
Camm AJ, Lip GY, De Caterina R, et al. 2012 focused update of the ESC guidelines for the management of atrial fibrillation: an update of the 2010 ESC guidelines for the management of atrial fibrillation. Developed with the special contribution of the European Heart Rhythm Association. Eur Heart J. 2012;33(21):2719–47.
Olesen JB, Lip GY, Hansen PR, et al. Bleeding risk in ‘real world’ patients with atrial fibrillation: comparison of two established bleeding prediction schemes in a nationwide cohort. J Thromb Haemost. 2011;9(8):1460–7.
Rosendaal FR, Cannegieter SC, van der Meer FJ, Briet E. A method to determine the optimal intensity of oral anticoagulant therapy. Thromb Haemost. 1993;69(3):236–9.
Gallagher AM, Setakis E, Plumb JM, Clemens A, van Staa TP. Risks of stroke and mortality associated with suboptimal anticoagulation in atrial fibrillation patients. Thromb Haemost. 2011;106(5):968–77.
R: A language and environment for statistical computing. R Foundation for Statistical Computing [computer program]. Vienna, Austria. 2008.
Bleyer AJ, Hartman J, Brannon PC, Reeves-Daniel A, Satko SG, Russell G. Characteristics of sudden death in hemodialysis patients. Kidney Int. 2006;69(12):2268–73.
Clase CM, Holden RM, Sood MM, et al. Should patients with advanced chronic kidney disease and atrial fibrillation receive chronic anticoagulation? Nephrol Dial Transpl. 2012;27(10):3719–24.
Bertoli SV, di Belgiojoso GB, Trezzi M, et al. Reduced blood levels of coagulation inhibitors in chronic hemodialysis compared with CAPD. Adv Perit Dial. 1995;11:127–30.
Yang F, Khin LW, Lau T, et al. Hemodialysis versus peritoneal dialysis: a comparison of survival outcomes in South-East Asian patients with end-stage renal disease. PLoS One. 2015;10(10):e0140195.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No sources of funding were used to assist in the preparation of this study.
Conflict of Interest
Derek Phan, MD, Su-Jau Yang, PhD, Albert Y.-J. Shen, MD, and Ming-Sum Lee, MD, PhD, have no conflicts of interest that are directly relevant to the content of this study.
Rights and permissions
About this article
Cite this article
Phan, D., Yang, SJ., Shen, A.YJ. et al. Effect of Warfarin on Ischemic Stroke, Bleeding, and Mortality in Patients with Atrial Fibrillation Receiving Peritoneal Dialysis. Am J Cardiovasc Drugs 19, 509–515 (2019). https://doi.org/10.1007/s40256-019-00347-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40256-019-00347-3