Abstract
Objective
The objective of this scoping review was to investigate the effectiveness and limitations of risk prediction models for postpartum glucose intolerance in women with gestational diabetes mellitus (GDM). The aim was to provide valuable insights for healthcare professionals in the development of robust risk prediction models.
Methods
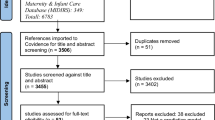
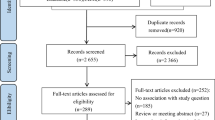
A comprehensive literature search was conducted across multiple databases, including PubMed, EBSCO, Web of Science Core Collection, Ovid Full-Text Medical Journal Database, ProQuest, Elsevier ClinicalKey, China National Knowledge Infrastructure, China Biology Medicine, and WanFang Database, spanning from January 1990 to July 2023. To assess the quality of the included models, the Predictive Model Risk of Bias Assessment Tool (PROBAST) was employed.
Results
Fourteen relevant studies were identified and included in the final review, all focusing on model development. The discrimination ability of the included models ranged from 0.725 to 0.940, indicating satisfactory prediction accuracy. However, a notable limitation was that nine of these models (64.3%) did not provide clear guidelines on the selection of potential predictors. Furthermore, only six models (42.86%) underwent internal validation, with none undergoing external validation. A high risk of bias was observed across the included models. Logistic regression, Cox regression, and machine learning were the primary methods employed in the construction of these models.
Conclusion
The risk prediction models included in this review demonstrated favorable prediction accuracy. However, due to variations in construction methodologies, direct comparison of their performance is challenging. These models exhibited certain shortcomings, such as inadequate handling of missing data and a lack of internal and external validation, resulting in a high risk of bias. Therefore, it is recommended that these models be updated and externally validated. The development of prospective, multi-center studies is encouraged to construct predictive models with low risk of bias and high clinical applicability, ultimately guiding evidence-based clinical practice.


Similar content being viewed by others
Data availability
All data is contained within the manuscript file and additional file.
References
Cho NH, Shaw JE, Karuranga S, et al. IDF diabetes atlas: global estimates of diabetes prevalence for 2017 and projections for 2045. Diabetes Res Clin Pract. 2018;138:271–81. https://doi.org/10.1016/j.diabres.2018;02.023.
International Diabetes Federation. IDF Diabetes Atlas. 10th ed. Brussels: International Diabetes Federation; 2021.
Alejandro EU, Mamerto TP, Chung G, et al. Gestational diabetes mellitus: a harbinger of the vicious cycle of diabetes. Int J Mol Sci. 2020;21(14):5003. https://doi.org/10.3390/ijms21145003.
Gomes D, von Kries R, Delius M, et al. Late-pregnancy dysglycemia in obese pregnancies after negative testing for gestational diabetes and risk of future childhood overweight: an interim analysis from a longitudinal mother-child cohort study. PLoS Med. 2018;15(10):e1002681. https://doi.org/10.1371/journal.pmed.1002681.
Green JB. Cardiovascular consequences of gestational diabetes. Circulation. 2021;143(10):988–90. https://doi.org/10.1161/CIRCULATIONAHA.120.052995.
El Ouahabi H, Doubi S, Boujraf S, et al. Gestational diabetes and risk of developing postpartum type 2 diabetes: how to improve follow-up? Int J Prev Med. 2019;10:51. https://doi.org/10.4103/ijpvm.IJPVM_3_17.
Olmos P, Borzone G, Poblete A. Basal glucose on tolerance test during pregnancy predicts impaired fasting glucose and type 2 diabetes within 2 months after gestational diabetes. Can J Diabetes. 2021;45(2):122–8. https://doi.org/10.1016/j.jcjd.2020.06.008.
Jotic AZ, Stoiljkovic MM, Milicic TJ, et al. Prevalence and metabolic predictors for early diagnosed prediabetes in women with previous gestational diabetes: observational cohort study. Diabetes Ther. 2021;12(10):2691–700. https://doi.org/10.1007/s13300-021-01144-5.
Bellamy L, Casas JP, Hingorani AD, et al. Type 2 diabetes mellitus after gestational diabetes: a systematic review and meta-analysis. Lancet. 2009;373(9677):1773–9. https://doi.org/10.1016/S0140-6736(09)60731-5.
Vounzoulaki E, Khunti K, Abner SC, et al. Progression to type 2 diabetes in women with a known history of gestational diabetes: systematic review and meta-analysis. BMJ. 2020;369:m1361. https://doi.org/10.1136/bmj.m1361.
Szmuilowicz ED, Josefson JL, Metzger BE. Gestational diabetes mellitus. Endocrinol Metab Clin N Am. 2019;48(3):479–93. https://doi.org/10.1016/j.ecl.2019.05.001.
Au EH, Francis A, Bernier-Jean A, et al. Prediction modeling-part 1: regression modeling. Kidney Int. 2020;97(5):877–84. https://doi.org/10.1016/j.kint.2020.02.007.
Poldrack RA, Huckins G, Varoquaux G. Establishment of best practices for evidence for prediction: a review. JAMA Psychiatry. 2020;77(5):534–40. https://doi.org/10.1001/jamapsychiatry.2019.3671.
Bianchi C, de Gennaro G, Brocchi A, et al. Risk factors associated with postpartum impaired glucose regulation in women with previous gestational diabetes. J Diabetes Complicat. 2021;35(4):107854. https://doi.org/10.1016/j.jdiacomp.2021.107854.
Lai M, Fang F, Ma Y, et al. Elevated Midtrimester triglycerides as a biomarker for postpartum hyperglycemia in gestational diabetes. J Diabetes Res. 2020;2020:3950652. https://doi.org/10.1155/2020/3950652.
Muche AA, Olayemi OO, Gete YK. Predictors of postpartum glucose intolerance in women with gestational diabetes mellitus: a prospective cohort study in Ethiopia based on the updated diagnostic criteria. BMJ Open. 2020;10(8):e036882. https://doi.org/10.1136/bmjopen-2020-036882.
Arksey H, O'Malley L. Scoping studies:towards a methodological framework. Int J Soc Res Methodol. 2005;8(1):19–32. https://doi.org/10.1080/1364557032000119616.
Moons KGM, Wolff RF, Riley RD, et al. PROBAST: a tool to assess risk of Bias and applicability of prediction model studies: explanation and elaboration. Ann Intern Med. 2019;170(1):W1–W33. https://doi.org/10.7326/M18-1377.
Peduzzi P, Concato J, Kemper E, et al. A simulation study of the number of events per variable in logistic regression analysis. J Clin Epidemiol. 1996;49(12):1373–9. https://doi.org/10.1016/s0895-4356(96)00236-3.
van Smeden M, Moons KG, de Groot JA, et al. Sample size for binary logistic prediction models: beyond events per variable criteria. Stat Methods Med Res. 2019;28(8):2455–74. https://doi.org/10.1177/0962280218784726.
Finazzi S, Poole D, Luciani D, et al. Calibration belt for quality-of-care assessment based on dichotomous outcomes. PLoS One. 2011;6(2):e16110. https://doi.org/10.1371/journal.pone.0016110.
Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. https://doi.org/10.1136/bmj.n71.
Kondo M, Nagao Y, Mahbub MH, et al. Factors predicting early postpartum glucose intolerance in Japanese women with gestational diabetes mellitus: decision-curve analysis. DiabetMed. 2018;35(8):1111–7. https://doi.org/10.1111/dme.13657.
McElnay JC, Elnour AA. Risk factor model for developing postpartum diabetes mellitus in patients with gestational diabetes mellitus. Int J Med. 2006. https://www.priory.com/med/postpartumdiabetes.htm.
Bartáková V, Barátová B, Pácal L, et al. Development of a new risk score for stratification of women with gestational diabetes mellitus at high risk of persisting postpartum glucose intolerance using routinely assessed parameters. Life (Basel). 2021;11(6):464. https://doi.org/10.3390/life11060464.
Bengtson AM, Dice ALE, Clark MA, et al. Predicting progression from gestational diabetes to impaired glucose tolerance using peri-delivery data: an observational study. Am J Perinatol. 2022. https://doi.org/10.1055/a-1877-9587.
Allalou A, Nalla A, Prentice KJ, et al. A predictive metabolic signature for the transition from gestational diabetes mellitus to type 2 diabetes. Diabetes. 2016;65(9):2529–39. https://doi.org/10.2337/db15-1720.
Li W, Leng J, Liu H, et al. Nomograms for incident risk of postpartum type 2 diabetes in Chinese women with prior gestational diabetes mellitus. Clin Endocrinol. 2019;90(3):417–24. https://doi.org/10.1111/cen.13863.
Man B, Schwartz A, Pugach O, et al. A clinical diabetes risk prediction model for prediabetic women with prior gestational diabetes. PLoS One. 2021;16(6):e0252501. https://doi.org/10.1371/journal.pone.0252501.
Kwak SH, Choi SH, Kim K, et al. Prediction of type 2 diabetes in women with a history of gestational diabetes using a genetic risk score. Diabetologia. 2013;56(12):2556–63. https://doi.org/10.1007/s00125-013-3059-x.
Kumar M, Ang LT, Ho C, et al. Machine learning-derived prenatal predictive risk model to guide intervention and prevent the progression of gestational diabetes mellitus to type 2 diabetes: prediction model development study. JMIR Diabetes. 2022;7(3):e32366. https://doi.org/10.2196/32366.
Ignell C, Ekelund M, Anderberg E, et al. Model for individual prediction of diabetes up to 5 years after gestational diabetes mellitus. Springerplus. 2016;5:318. https://doi.org/10.1186/s40064-016-1953-7.
Wang XM, Gao Y, Eriksson JG, et al. Metabolic signatures in the conversion from gestational diabetes mellitus to postpartum abnormal glucose metabolism: a pilot study in Asian women. Sci Rep. 2021;11(1):16435. https://doi.org/10.1038/s41598-021-95903-w.
Joglekar MV, Wong WKM, Ema FK, et al. Postpartum circulating microRNA enhances prediction of future type 2 diabetes in women with previous gestational diabetes. Diabetologia. 2021;64(7):1516–26. https://doi.org/10.1007/s00125-021-05429-z.
Köhler M, Ziegler AG, Beyerlein A. Development of a simple tool to predict the risk of postpartum diabetes in women with gestational diabetes mellitus. Acta Diabetol. 2016;53(3):433–7. https://doi.org/10.1007/s00592-015-0814-0.
Li H, Liu M. Cohort studies in health management research. Chin J Health Manag. 2019;13(3):268–72. https://doi.org/10.3760/cma.j.issn.1674-0815.2019.03.021.
Gu H, Wang J, Zhou Z, et al. Clinical predictive models: construction. Chin J Evid-Bases Cardiovasc Med. 2019;11(1):14–16,23. https://doi.org/10.3969/j.issn.1674-4055.2019.01.04.
Liu Z, Zhang Q, Liu L, et al. Risk factors associated with early postpartum glucose intolerance in women with a history of gestational diabetes mellitus: a systematic review and meta-analysis. Endocrine. 2023;16. https://doi.org/10.1007/s12020-023-03472-x.
Kawasaki M, Arata N, Sakamoto N, et al. Risk factors during the early postpartum period for type 2 diabetes mellitus in women with gestational diabetes. Endocr J. 2020;67:427–37. https://doi.org/10.1507/endocrj.EJ19-0367.
Quansah DY, Gross J, Mbundu-Ilunga R, et al. The utility of diagnostic tests in the detection and prediction of glucose intolerance in the early and late postpartum period in women after gestational diabetes: a longitudinal cohort study. Diabetol Metab Syndr. 2021;13(1):31. https://doi.org/10.1186/s13098-021-00650-7.
Kim C, Newton KM, Knopp RH. Gestational diabetes and the incidence of type 2 diabetes: a systematic review. Diabetes Care. 2002;25(10):1862–8. https://doi.org/10.2337/diacare.25.10.1862.
Yefet E, Schwartz N, Sliman B, et al. Good glycemic control of gestational diabetes mellitus is associated with the attenuation of future maternal cardiovascular risk: a retrospective cohort study. Cardiovasc Diabetol. 2019;18(1):75. https://doi.org/10.1186/s12933-019-0881-6.
Ngiam KY, Khor IW. Big data and machine learning algorithms for healthcare delivery. Lancet Oncol. 2019;20(5):e262–73. https://doi.org/10.1016/S1470-2045(19)30149-4.
Austin PC, White IR, Lee DS, et al. Missing data in clinical research: a tutorial on multiple imputation. Can J Cardiol. 2021;37(9):1322–31. https://doi.org/10.1016/j.cjca.2020.11.010.
Collins GS, Reitsma JB, Altman DG, et al. Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): the TRIPOD statement. BMJ. 2015;350:g7594. https://doi.org/10.1136/bmj.g7594.
Steyerberg EW, Harrell FE Jr. Prediction models need appropriate internal, internal-external, and external validation. J Clin Epidemiol. 2016;69:245–7. https://doi.org/10.1016/j.jclinepi.2015.04.005.
Wang J, Zhang Z, Zhou Z, et al. Clinical prediction models: model validation. Chin J Evid-Bases Cardiovasc Med. 2019;11(02):141–4. https://doi.org/10.3969/j.issn.1674-4055.2019.02.04.
Moons KG, Kengne AP, Grobbee DE, et al. Risk prediction models: II. External validation, model updating, and impact assessment. Heart. 2012;98(9):691–8. https://doi.org/10.1136/heartjnl-2011-301247.
Luo JC, Zhao QY, Tu GW. Clinical prediction models in the precision medicine era: old and new algorithms. Ann Transl Med. 2020;8(6):274. https://doi.org/10.21037/atm.2020.02.63.
Vickers AJ, Elkin EB. Decision curve analysis: a novel method for evaluating prediction models. Med Decis Mak. 2006;26(6):565–74. https://doi.org/10.1177/0272989X06295361.
Van Calster B, Wynants L, Verbeek JFM, et al. Reporting and interpreting decision curve analysis: a guide for investigators. Eur Urol. 2018;74(6):796–804. https://doi.org/10.1016/j.eururo.2018.08.038.
Acknowledgments
Thanks to the National Natural Science Foundation of China for supporting this research (project number: 71904133).
Funding
This work was supported by the National Natural Science Foundation of China for supporting this research (project number: 71904133).
Author information
Authors and Affiliations
Contributions
All authors participated contributed to the study conception and design. Material preparation, data collection and analysis were performed by Zhe Liu, Huiziqiang Zhang and Nan Jia. Zhe Liu drafted the work and Weiwei Liu revised it critically for important intellectual content. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
Not applicable.
Competing interests
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 24 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, Z., Jia, N., Zhang, Q. et al. Risk prediction models for postpartum glucose intolerance in women with a history of gestational diabetes mellitus: a scoping review. J Diabetes Metab Disord (2023). https://doi.org/10.1007/s40200-023-01330-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40200-023-01330-1