Abstract
Background
There is paucity of data on the potential predictors of coronary plaque types among patients with diabetes mellitus(DM).
Aims
To assess the association of cardiovascular risk factors, pericardial fat volume (PFV) assessed by multi-detector CT(MDCT)angiography, and internal carotid intima media thickness with coronary atherosclerotic plaque types in patients with type 2 DM.
Patients and methods
Patients with suspected coronary artery disease who underwent 64-slice MDCT angiography were enrolled in this retrospective study.
Results
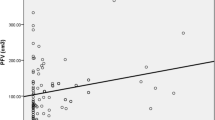
A total of 784 patients were enrolled in this study, 198 of whom had DM and 586 of whom did not. The prevalence of calcified and mixed plaques was significantly higher in the DM group than without DM group, while no significant difference was found in the distribution of non-calcified plaque between groups. There was significant association between smoking [OR(CI) = 4(2–10),P = 0.001] and increased age[OR(CI) = 1.1(1-1.3),P = 0.023] and calcified plaque presence. Regarding mixed and non-calcified plaque, increased PFV[OR(CI) = 1.1(1-1.3),P = 0.001] and positive family history[OR(CI) = 4(2–12),P = 0.049] showed a significant association with coronary mixed plaque presence while no significant association was observed between cardiovascular risk factors, PFV, and internal carotid intima media thickness and non-calcified plaque presence in patients with DM.
Conclusion
Increased PFV showed significant and independent association with mixed coronary plaques development, which suggests that PFV may be used as an imaging marker for early detection of increased risk for future coronary events in patients with DM.
Similar content being viewed by others
References
Khan A, Arbab-Zadeh A, Kiani AN, Magder LS, Petri M. Progression of noncalcified and calcified coronary plaque by CT angiography in SLE. Rheumatol Int. 2017;37(1):59–65. https://doi.org/10.1007/s00296-016-3615-z.
Tsushima H, Yamamoto H, Kitagawa T, Urabe Y, Tatsugami F, Awai K, et al. Association of epicardial and abdominal visceral adipose tissue with coronary atherosclerosis in patients with a coronary artery calcium score of zero. Circ J. 2015;79:1084–91.
Dwivedi A, Al’Aref SJ, Lin FY, Min JK. Evaluation of atherosclerotic plaque in non-invasive coronary imaging. Korean Circ J. 2018;48(2):124–33. https://doi.org/10.4070/kcj.2017.0392.
Jeevarethinam A, Venuraju S, Dumo A, Ruano S, Mehta VS, Rosenthal M, et al. Relationship between carotid atherosclerosis and coronary artery calcification in asymptomatic diabetic patients: a prospective multicenter study. Clin Cardiol. 2017;40(9):752–8. https://doi.org/10.1002/clc.22727.
Zellweger MJ, Maraun M, Osterhues HH, Keller U, Muller-Brand J, Jeger R, et al. Progression to overt or silent CAD in asymptomatic patients with diabetes mellitus at high coronary risk: main findings of the prospective multicenter BARDOT trial with a pilot randomized treatment substudy. J Am Coll Cardiol Img. 2014;7(10):1001–10.
Feuchtner GM, Plank F, Beyer C, Barbieri F, Widmann G, Spitaler P, Dichtl W. Cardiac Computed Tomography: state of the Art and Future Horizons. J Clin Med. 2022;11(15):4429. https://doi.org/10.3390/jcm11154429.
Nafakhi H, Al-Mosawi AA, Mudhafar MM. Pericardial fat versus BMI in the assessment of coronary atherosclerotic burden in patients with diabetes mellitus. Acta Diabetol. 2020;57(5):605–11. https://doi.org/10.1007/s00592-019-01465-9.
Tavares CA, Wajchjenberg BL, Rochitte C, Lerario AC. Screening for asymptomatic coronary artery disease in patients with type 2 diabetes mellitus. Arch Endocrinol Metab. 2016;60(2):143–51. https://doi.org/10.1590/2359-3997000000170.
Kocak MZ, Aktas G, Duman TT, Atak BM, Kurtkulagi O, Tekce H, et al. Monocyte lymphocyte ratio as a predictor of Diabetic kidney Injury in type 2 diabetes mellitus; the MADKID Study. J Diabetes Metab Disord. 2020;19(2):997–1002. https://doi.org/10.1007/s40200-020-00595-0.
Stojan G, Li J, Budoff M, Arbab-Zadeh A, Petri MA. High-risk coronary plaque in SLE: low-attenuation non-calcified coronary plaque and positive remodelling index. Lupus Sci Med. 2020;7(1):e000409. https://doi.org/10.1136/lupus-2020-000409.
Williams MC, Kwiecinski J, Doris M, McElhinney P, D’Souza MS, Cadet S, et al. Low-attenuation Noncalcified Plaque on Coronary computed Tomography Angiography predicts myocardial infarction: results from the Multicenter SCOT-HEART Trial (Scottish Computed Tomography of the HEART). Circulation. 2020;141(18):1452–62. https://doi.org/10.1161/CIRCULATIONAHA.119.044720.
Christiansen MK, Jensen JM, Nørgaard BL, Dey D, Bøtker HE, Jensen HK. Coronary plaque burden and adverse plaque characteristics are increased in healthy relatives of patients with early onset coronary artery disease. JACC Cardiovasc Imaging. 2017;10(10 Pt A):1128–35. https://doi.org/10.1016/j.jcmg.2016.10.014.
van Rosendael AR, Narula J, Lin FY, van den Hoogen IJ, Gianni U, Al Hussein Alawamlh O, et al. Association of High-Density calcified 1K plaque with risk of Acute Coronary Syndrome. JAMA Cardiol. 2020;5(3):282–90. https://doi.org/10.1001/jamacardio.2019.5315.
Kral BG, Becker LC, Vaidya D, Yanek LR, Qayyum R, Zimmerman SL, et al. Noncalcified coronary plaque volumes in healthy people with a family history of early onset coronary artery disease. Circ Cardiovasc Imaging. 2014;7(3):446–53. https://doi.org/10.1161/CIRCIMAGING.113.000980. Epub 2014 Feb 27.
Thomas IC, Forbang NI, Criqui MH. The evolving view of coronary artery calcium and cardiovascular disease risk. Clin Cardiol. 2018;41(1):144–50. https://doi.org/10.1002/clc.22842.
Puri R, Nicholls SJ, Shao M, Kataoka Y, Uno K, Kapadia SR, et al. Impact of statins on serial coronary calcification during atheroma progression and regression. J Am Coll Cardiol. 2015;65(13):1273–82. https://doi.org/10.1016/j.jacc.2015.01.036.
Hou ZH, Lu B, Gao Y, Jiang SL, Wang Y, Li W, et al. Prognostic value of coronary CT angiography and calcium score for major adverse cardiac events in outpatients. JACC Cardiovasc Imaging. 2012;5(10):990–9. https://doi.org/10.1016/j.jcmg.2012.06.006.
Murai T, Takebe N, Nagasawa K, Todate Y, Nakagawa R, Nakano R, et al. Association of epicardial adipose tissue with serum level of cystatin C in type 2 diabetes. PLoS ONE. 2017;12(9):e0184723.
Hwang IC, Park HE, Choi SY. Epicardial adipose tissue contributes to the development of non-calcified coronary plaque: a 5-Year computed Tomography follow-up study. J Atheroscler Thromb. 2017;24(3):262–74.
Kim U, Leipsic JA, Sellers SL, Shao M, Blanke P, Hadamitzky M, et al. Natural history of Diabetic Coronary atherosclerosis by quantitative measurement of serial coronary computed Tomographic Angiography: results of the PARADIGM study. JACC Cardiovasc Imaging. 2018;11(10):1461–71. https://doi.org/10.1016/j.jcmg.2018.04.009.
Yang J, Dou G, Tesche C, De Cecco CN, Jacobs BE, Schoepf UJ, et al. Progression of coronary atherosclerotic plaque burden and relationship with adverse cardiovascular event in asymptomatic diabetic patients. BMC Cardiovasc Disord. 2019;19(1):39. https://doi.org/10.1186/s12872-019-1016-4.
Yamaura H, Otsuka K, Ishikawa H, Shirasawa K, Fukuda D, Kasayuki N. Determinants of non-calcified low-attenuation coronary plaque burden in patients without known coronary artery disease: a coronary CT Angiography Study. Front Cardiovasc Med. 2022;9:824470. https://doi.org/10.3389/fcvm.2022.824470.
Talman AH, Psaltis PJ, Cameron JD, Meredith IT, Seneviratne SK, Wong DT. Epicardial adipose tissue: far more than a fat depot. Cardiovasc Diagn Ther. 2014;4(6):416–29. https://doi.org/10.3978/j.issn.2223-3652.2014.11.05.
Darabian S, Hormuz M, Latif MA, Pahlevan S, Budoff MJ. The role of carotid intimal thickness testing and risk prediction in the development of coronary atherosclerosis. Curr Atheroscler Rep. 2013;15(3):306. https://doi.org/10.1007/s11883-012-0306-4.
Inaba Y, Chen JA, Bergmann SR. Carotid plaque, compared with carotid intima-media thickness, more accurately predicts coronary artery disease events: a meta-analysis. Atherosclerosis. 2012;220(1):128–33. https://doi.org/10.1016/j.atherosclerosis.2011.06.044.
Cohen GI, Aboufakher R, Bess R, Frank J, Othman M, Doan D, et al. Relationship between carotid disease on ultrasound and coronary disease on CT angiography. JACC Cardiovasc Imaging. 2013;6(11):1160–7. https://doi.org/10.1016/j.jcmg.2013.06.007.
Kathiresan S, Larson MG, Keyes MJ, Polak JF, Wolf PA, D’Agostino RB, et al. Assessment by cardiovascular magnetic resonance, electron beam computed tomography, and carotid ultrasonography of the distribution of subclinical atherosclerosis across Framingham risk strata. Am J Cardiol. 2007;99(3):310–4. https://doi.org/10.1016/j.amjcard.2006.08.028.
Bytyçi I, Shenouda R, Wester P, Henein MY. Carotid atherosclerosis in Predicting Coronary Artery Disease: a systematic review and Meta-analysis. Arterioscler Thromb Vasc Biol. 2021;41(4):e224–37. https://doi.org/10.1161/ATVBAHA.120.315747.
Funding
There were no external funding sources for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standard
The study was approved by the local Institutional Review Board.
Statement of human and animal rights
The study protocol was performed according to the principles stated in the Declaration of Helsinki as revised in 2000.
Informed consent
Verbal informed consent was obtained from all participants
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nafakhi, H., Elwali, H.Q., Al-Sharea, K.M.K. et al. Relationship of cardiovascular risk factors, pericardial fat, and carotid thickness with coronary plaque type in patients with diabetes mellitus. J Diabetes Metab Disord 22, 713–719 (2023). https://doi.org/10.1007/s40200-023-01190-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40200-023-01190-9