Abstract
Background and Aims
The contribution of inactive Matrix Gla protein (MGP) to ectopic vascular calcification associated with type 2 diabetes mellitus (T2DM) is well recognized. However, its role in diabetic microvascular complications remains unknown. The study aim was to identify any association between inactive MGP and diabetic retinopathy (DR). Its relation to insulin resistance was also explored.
Methods
The study included 90 participants, 65 Type 2 diabetic patients (25 without DR and 40 with DR) and 25 healthy controls. Serum inactive MGP was measured using ELISA. HOMA-IR was also assessed.
Results
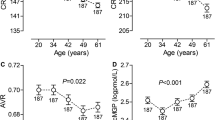
Inactive MGP was significantly higher in both diabetic groups compared to controls (P < 0.001), as well as in Type 2 diabetic patients with retinopathy compared to Type 2 diabetes without retinopathy (P = 0.002). Inactive MGP was positively correlated with HbA1c, HOMA-IR, LDL-C and triglycerides (P < 0.001), and negatively correlated with HDL-C (P = 0.008) and eGFR (P < 0.001). Logistic Regression Analysis showed that inactive MGP was one of the most associated factors with DR.
Conclusions
Inactive MGP was found to be related to DR, insulin resistance and other dysmetabolic risk factors. These findings highlight that inactive MGP may be a significant contributor to the pathogenesis, evolution, and progression of DR.

Similar content being viewed by others
Data availability
The data that support the findings of this study are available on request from the corresponding author.
References
Wong TY, Sabanayagam C. Strategies to tackle the global burden of diabetic retinopathy: from epidemiology to artificial intelligence. Ophthalmologica. 2020;243(1):9–20.
Nentwich MM, Ulbig MW. Diabetic retinopathy-ocular complications of diabetes mellitus. World J Diabetes. 2015;6(3):489.
Yau JW, Rogers SL, Kawasaki R, Lamoureux EL, Kowalski JW, Bek T, et al. Global prevalence and major risk factors of diabetic retinopathy. Diabetes Care. 2012;35(3):556–64.
Knapen MH, Braam LA, Drummen NE, Bekers O, Hoeks AP, Vermeer C. Menaquinone-7 supplementation improves arterial stiffness in healthy postmenopausal women. Thromb Haemost. 2015;113(5):1135–44.
Wei FF, Huang QF, Zhang ZY, Van Keer K, Thijs L, Trenson S, et al. Inactive matrix Gla protein is a novel circulating biomarker predicting retinal arteriolar narrowing in humans. Sci Rep. 2018;8(1):1–8.
Borrás T, Smith MH, Buie LK. A novel MGP-Cre knock-in mouse reveals an anticalcification/ antistiffness candidate gene in the trabecular meshwork and peripapillary scleral region. Invest Ophthalmol Vis Sci. 2015;56:2203–14.
Schurgers LJ, Teunissen KJ, Knapen MH, Kwaijtaal M, van Diest R, Appels A, et al. Novel conformation-specific antibodies against matrix gamma-carboxyglutamic acid (Gla) protein: Undercarboxylated matrix Gla protein as marker for vascular calcification. Arterioscler Thromb Vasc Biol. 2005;25(8):1629–33.
Shea CM, Edgar CM, Einhorn TA, Gerstenfeld LC. BMP treatment of C3H10T1/2 mesenchymal stem cells induces both chondrogenesis and osteogenesis. J Cell Biochem. 2003;90(6):1112–27.
Early Treatment Diabetic Retinopathy Study Research Group (ETDRS). Grading diabetic retinopathy from stereoscopic color fundus photographs - an extension of the modified airlie house classification. Ophthalmology. 2020;127(4):99–119.
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia. 1985;28(7):412–9.
Stevens L, Coresh J, Greene T, Levey A. Assessing kidney function measured and estimated glomerular filtration rate. N Engl J Med. 2006;354(23):2473–83.
Doyon M, Mathieu P, Moreau P. Decreased expression of gamma-carboxylase in diabetes-associated arterial stiffness: impact on matrix Gla protein. Cardiovasc Res. 2013;97(2):331–8.
Braam LA, Dissel P, Gijsbers BL, Spronk HM, Hamulyak K, Soute BA, et al. Assay for human matrix GLA protein in serum: potential applications in the cardiovascular field. Arterioscler Thromb Vasc Biol. 2000;20(5):1257–61.
Parker BD, Schurgers LJ, Vermeer C, Schiller NB, Whooley MA, Ix JH. The association of uncarboxylated matrix Gla protein with mitral annular calcification differs by diabetes status: The Heart and Soul study. Atherosclerosis. 2010;210(1):320–5.
Jeannin AC, Salem JE, Massy Z, Aubert CE, Vemeer C, Amouyal C, et al. Inactive matrix GLA protein plasma levels are associated with peripheral neuropathy in Type 2 diabetes. PLoS ONE. 2020;15(2):e0229145.
Antonopoulos AS, Siasos G, Tousoulis D. Microangiopathy, arterial stiffness, and risk stratification in patients with type 2 diabetes. JAMA cardiology. 2017;2(7):820–1.
Schurgers LJ, Uitto J, Reutelingsperger CP. Vitamin K-dependent carboxylation of matrix Gla-protein: a crucial switch to control ectopic mineralization. Trends Mol Med. 2013;19(4):217–26.
Dalmeijer GW, Van der Schouw YT, Vermeer C, Magdeleyns EJ, Schurgers LJ, Beulens JW. Circulating matrix Gla protein is associated with coronary artery calcification and vitamin K status in healthy women. J Nutr Biochem. 2013;24(4):624–8.
Mayer O Jr, Seidlerová J, Wohlfahrt P, Filipovský J, Vaněk J, Cífková R, et al. Desphospho-uncarboxylated matrix Gla protein is associated with increased aortic stiffness in a general population. J Hum Hypertens. 2016;30(7):418–23.
Pivin E, Ponte B, Pruijm M, Ackermann D, Guessous I, Ehret G, et al. Inactive matrix Gla-protein is associated with arterial stiffness in an adult population-based study. Hypertension. 2015;66(1):85–92.
Liu YP, Gu YM, Thijs L, Knapen MH, Salvi E, Citterio L, et al. Inactive MGP is causally related to adverse health outcomes: a Mendelian randomization study in a Flemish population. Hypertension. 2015;65(2):463–70.
Liabeuf S, Olivier B, Vemeer C, Theuwissen E, Magdeleyns E, Aubert CE, et al. Vascular calcification in patients with type 2 diabetes: the involvement of matrix Gla protein. Cardiovasc Diabetol. 2014;13(1):1–8.
Puzantian H, Akers SR, Oldland G, Javaid K, Miller R, Ge Y, et al. Circulating dephospho-uncarboxylated matrix Gla-protein is associated with kidney dysfunction and arterial stiffness. Am J Hypertens. 2018;31(9):988–94.
Griffin TP, Islam MN, Wall D, Ferguson J, Griffin DG, Griffin MD, et al. Plasma dephosphorylated-uncarboxylated Matrix Gla-Protein (dp-ucMGP): reference intervals in Caucasian adults and diabetic kidney disease biomarker potential. Sci Rep. 2019;9(1):1–13.
Sardana M, Vasim I, Varakantam S, Kewan U, Tariq A, Koppula MR, et al. Inactive matrix Gla-protein and arterial stiffness in type 2 diabetes mellitus. Am J Hypertens. 2017;30(2):196–201.
Acknowledgements
We would like to thank the managerial and nursing staff of the Departments of Endocrinology and Metabolism and Ophthalmology et al.-Zahraa University Hospital, Faculty of Medicine (Girls), Al-Azhar University, Cairo, who facilitate patient identification and sampling, and helped us to complete this work. Also, thanks are due to the staff of Biochemistry and Molecular Biology Department, Faculty of Pharmacy (Boys), Al-Azhar University, Cairo, who enabled us to accomplish the practical work using the central lab facilities.
Author information
Authors and Affiliations
Contributions
All authors were involved in the design of this study. OF, EM and NSM were responsible for patients’ diagnosis, clinical recruitment and sampling. HA and EGK carried out the practical part of the work and contributed in statistical analysis and data collection. All authors contributed equally in literature collection, manuscript writing, and thorough reviewing. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
The study was approved by the Research Ethics committee of the Faculty of Medicine for Girls, Al-Azhar University, Cairo, Egypt and was in accordance with the tenets of the Helsinki Declaration. A written consent was taken from all participants.
Conflict of interest
The authors declared that they have no conflict of interest. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Adel, H., Fawzy, O., Mahmoud, E. et al. Inactive matrix Gla protein in relation to diabetic retinopathy in type 2 diabetes. J Diabetes Metab Disord 22, 603–610 (2023). https://doi.org/10.1007/s40200-022-01180-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40200-022-01180-3