Abstract
Background
Microbiological confirmation cannot be obtained in approximately two-third patients with tuberculous meningitis. In this study, we sought to identify epidemiological, clinical, cerebrospinal fluid, and imaging parameters that could indicate the possibility of microbiological confirmation among patients with suspected tuberculous meningitis.
Materials and methods
In this prospective observational study, patients with tuberculous meningitis were evaluated for clinical, laboratory (cerebrospinal fluid microscopy, culture, and polymerase chain reaction), and neuroimaging parameters. All patients received anti-tuberculosis drugs and corticosteroids. The patients were followed for a period of 6 months.
Results
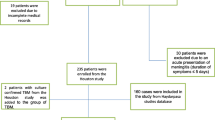
Among 118 cases of tuberculous meningitis, there were 43 (36 %) definite (microbiologically confirmed) cases, 59 (50 %) probable and 16 (14 %) possible cases. Among 43 definite cases, tuberculosis polymerase chain reaction (PCR) was positive in 42 (35 %) patients, culture was positive in 1 case and microscopy, after Ziehl–Neelsen staining, was positive in 3 cases. Three factors, modified Barthel index score at admission ≤12 (p = 0.008), cerebrospinal fluid total cell count >100/mm3 (p = 0.016), and basal exudates on imaging (p = 0.015), were significantly associated with definite tuberculous meningitis. Among 20 patients who died within 6 months, 13 belonged to definite tuberculous meningitis group (p < 0.001). Stage III tuberculous meningitis (p = 0.004), baseline-modified Barthel index score ≤12 (p = 0.013), and positive tuberculosis PCR (p = 0.007) were independently associated with poor outcome on multivariate analysis.
Conclusion
Severe disability, cerebrospinal fluid cells >100 mm3, and basal exudates are significantly related to the presence of microbiologically confirmed definite tuberculous meningitis. Microbiologically confirmed tuberculous meningitis is associated with poorer outcome.


Similar content being viewed by others
References
Graham SM, Donald PR. Death and disability: the outcomes of tuberculous meningitis. Lancet Infect Dis. 2014;14:902–4.
Chin JH. Tuberculous meningitis: diagnostic and therapeutic challenges. Neurol Clin Pract. 2014;4:199–205.
Chiang SS, Khan FA, Milstein MB, Tolman AW, Benedetti A, Starke JR, et al. Treatment outcomes of childhood tuberculous meningitis: a systematic review and meta-analysis. Lancet Infect Dis. 2014;14:947–57.
Chaidir L, Ganiem AR, Vander Zanden A, Muhsinin S, Kusumaningrum T, Kusumadewi I, et al. Comparison of real time IS6110-PCR, microscopy, and culture for diagnosis of tuberculous meningitis in a cohort of adult patients in Indonesia. PLoS ONE. 2012;7:e52001.
Nhu NT, Heemskerk D, Thu do DA, Chau TT, Mai NT, Nghia HD, et al. Evaluation of GeneXpert MTB/RIF for diagnosis of tuberculous meningitis. J Clin Microbiol. 2014;52:226–33.
Marais S, Thwaites G, Schoeman JF, Török ME, Misra UK, Prasad K, et al. Tuberculous meningitis: a uniform case definition for use in clinical research. Lancet Infect Dis. 2010;10:803–12.
Bhanu NV, Singh UB, Chakraborty M, Suresh N, Arora J, Rana T, et al. Improved diagnostic value of PCR in the diagnosis of female genital tuberculosis leading to infertility. J Med Microbiol. 2005;54(Pt 10):927–31.
Thwaites GE, Nguyen DB, Nguyen HD, Hoang TQ, Do TT, Nguyen TC, et al. Dexamethasone for the treatment of tuberculous meningitis in adolescents and adults. N Engl J Med. 2004;351:1741–51.
World Health Organization. Treatment of tuberculosis: guidelines. 4th ed. (WHO/HTM/TB/2009.420) World Health Organization, http://whqlibdoc.who.int/publications/2010/9789241547833_eng.pdf (2010). Accessed 25 Sept 2014.
Thwaites GE, Chau TT, Stepniewska K, Phu NH, Chuong LV, Sinh DX, et al. Diagnosis of adult tuberculous meningitis by use of clinical and laboratory features. Lancet. 2002;360:1287–92.
Thwaites GE, Chau TT, Farrar JJ. Improving the bacteriological diagnosis of tuberculous meningitis. J Clin Microbiol. 2004;42:378–9.
Feng GD, Shi M, Ma L, Chen P, Wang BJ, Zhang M, et al. Diagnostic accuracy of intracellular Mycobacterium tuberculosis detection for tuberculous meningitis. Am J Respir Crit Care Med. 2014;189:475–81.
Thwaites GE, van Toorn R, Schoeman J. Tuberculous meningitis: more questions, still too few answers. Lancet Neurol. 2013;12:999–1010.
Botha H, Ackerman C, Candy S, Carr JA, Griffith-Richards S, Bateman KJ. Reliability and diagnostic performance of CT imaging criteria in the diagnosis of tuberculous meningitis. PLoS ONE. 2012;7:e38982.
Ruslami R, Ganiem AR, Dian S, Apriani L, Achmad TH, van der Ven AJ, et al. Intensified regimen containing rifampicin and moxifloxacin for tuberculous meningitis: an open-label, randomised controlled phase 2 trial. Lancet Infect Dis. 2013;13:27–35.
Turkova A, Seddon JA, Nunn AJ, Gibb DM. Phillips PP. Short intensified treatment in children with drug-susceptible tuberculous meningitis. Pediatr Infect Dis J. 2014;33:993.
Thwaites GE, Duc Bang N, Huy Dung N, Thi Quy H, Thi Tuong Oanh D, Thi Cam Thoa N, et al. The influence of HIV infection on clinical presentation, response to treatment, and outcome in adults with tuberculous meningitis. J Infect Dis. 2005;192:2134–41.
Garg RK, Jain A, Malhotra HS, Agrawal A, Garg R. Drug-resistant tuberculous meningitis. Expert Rev Anti Infect Ther. 2013;11:605–21.
Conflict of interest
None for all the authors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jha, S.K., Garg, R.K., Jain, A. et al. Definite (microbiologically confirmed) tuberculous meningitis: predictors and prognostic impact. Infection 43, 639–645 (2015). https://doi.org/10.1007/s15010-015-0756-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-015-0756-z