Abstract
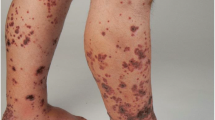
Anticoagulation-related nephropathy (ARN) is a rare form of acute kidney injury where the use of anticoagulation causes hemorrhage in various compartments of nephron including glomerulus, renal tubules, and interstitial compartment. Also, warfarin-induced vasculitis is an extremely rare condition characterized by the appearance of purpuric lesions on the skin which on biopsy are suggestive of leukocytoclastic vasculitis (LV). We hereby report a case presenting with coexistent warfarin-induced nephropathy and cutaneous vasculitis. A 64-year-old male, on warfarin for 10 years, presented with complaints of palpable purpuric rashes over lower limbs, hematuria, and decrease urine output. INR was in the supratherapeutic range (INR-6.3). Skin biopsy of the lesion was suggestive of LV and kidney biopsy showed RBCs in Bowman’s capsule, RBCs and RBC casts in tubules suggestive of ARN. All vasculitic markers were negative. Thus, a diagnosis of warfarin-induced nephropathy and cutaneous vasculitis was made. Warfarin was discontinued and oral steroids were started. Gradually, his skin lesions improved, and he became dialysis independent. He was then discharged on apixaban. On follow-up after 3 months, his skin lesions had disappeared with partial recovery of kidney function (cr-5.49).




Similar content being viewed by others
References
Brodsky S, Eikelboom J, Hebert LA. Anticoagulant-related nephropathy. J Am Soc Nephrol. 2018;29(12):2787–93.
Crowson AN, Mihm MC, Magro CM. Cutaneous vasculitis: a review. J Cutan Pathol. 2003;30(3):161–73.
Hsu CY, Chen WS, Sung SH. Warfarin-induced leukocytoclastic vasculitis: a case report and review of literature. Intern Med. 2012;51(6):601–6.
Kamo H, Shinozaki E, Sugase T, et al. Leukocytoclastic vasculitis with purpura and renal failure induced by the anti-epidermal growth factor receptor antibody panitumumab: a case report. J Med Case Rep. 2019;13(1):13.
Pingili CS, Okon EE. Vancomycin-induced leukocytoclastic vasculitis and acute renal failure due to tubulointerstitial nephritis. Am J Case Rep. 2017;18:1024–7.
Day C, Bridger J, Rylance P, Jackson M, Nicholas J, Odum J. Leukocytoclastic vasculitis and interstitial nephritis with carbimazole treatment. Nephrol Dial Transplant. 2003;18(2):429–31.
Kapoor KG, Bekaii-Saab T. Warfarin-induced allergic interstitial nephritis and leucocytoclastic vasculitis. Intern Med J. 2008;38(4):281–3.
Borrás-Blasco J, Girona E, Navarro-Ruiz A, et al. Acenocoumarol-Induced Henoch-Schönlein purpura. Ann Pharmacother. 2004;38(2):261–4.
Yaghoubian B, Ngo B, Mak M, Ostrzega E, Tesoro J, MoriguchiMitani GH. Warfarin-induced leukocytoclastic vasculitis. Cutis. 2005;75(6):329–38.
Jumean K, Arqoub A, Hawatmeh A, Qaqa F, Bataineh A, Shaaban H. Warfarin-induced leukocytoclastic vasculitis and proteinuria. J Fam Med Prim Care. 2016;5(1):160.
Howitt AJ, Williams AJ, Skinner C. Warfarin-induced vasculitis: a dose-related phenomenon in susceptible individuals? Postgrad Med J. 1982;58(678):233–4.
Brodsky SV, Satoskar A, Chen J, et al. Acute kidney injury during warfarin therapy associated with obstructive tubular red blood cell casts: a report of 9 cases. Am J Kidney Dis. 2009;54(6):1121–6.
de Aquino Moura KB, Behrens PMP, Pirolli R, et al. Anticoagulant-related nephropathy: systematic review and meta-analysis. Clin Kidney J. 2019;12(3):400–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have declared that no conflict of interest exists.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Bhandari, G., Tiwari, V., Gupta, A. et al. Double whammy: anticoagulant-related nephropathy with leukocytoclastic vasculitis due to warfarin. CEN Case Rep 11, 154–158 (2022). https://doi.org/10.1007/s13730-021-00642-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13730-021-00642-6