Abstract
Objective
Although masticatory performance is affected by age-related reduction in number of teeth (or treatment), the relationship between longitudinal changes in masticatory performance and diabetes mellitus is unknown. This longitudinal study investigated the association between changes in masticatory performance and new-onset diabetes mellitus among community-dwelling Japanese older adults.
Methods
The data of 214 older adults living in Ohnan Town, Shimane, Japan, who participated in two surveys conducted between 2012 and 2017 were analyzed. Diabetes mellitus was defined as a hemoglobin A1c level ≥ 6.5% or self-reported diabetes mellitus. The masticatory performance (measured by number of gummy jelly pieces collected after chewing) was evaluated by dental hygienists. Masticatory performance was categorized into two groups (high or low) based on the median in each survey; further, four groups (Group A: remained consistently high, Group B: changed from low to high, Group C: remained consistently low, Group D: changed from high to low) were used to determine longitudinal changes in masticatory performance. Logistic regression was used to analyze the association between changes in masticatory performance and new-onset diabetes mellitus.
Results
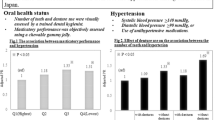
Overall, 10.3% of participants had diabetes mellitus at the follow-up survey. Multivariate analysis showed that Group D (odds ratio 8.69, 95% confidence interval 1.98–38.22) was positively associated with the development of diabetes mellitus compared with Group A after adjusting for sex, age, body mass index, alcohol consumption, physical activity, and eating speed.
Conclusions
Deteriorating masticatory performance for 5 years may cause diabetes mellitus among older adults.

Similar content being viewed by others
Data availability statement
Data are available upon reasonable request. This study used data from the Shimane CoHRE (Center for Community-Based Healthcare Research and Education) study. Some of the data are available from the CoHRE, Organization for Research and Academic Information, Shimane University, 223–8 Enya-cho, Izumo-shi, Shimane 693–8501, Japan.
References
Ramseier CA, Anerud A, Dulac M, Lulic M, Cullinan MP, Seymour GJ, Faddy MJ, Bürgin W, Schätzle M, Lang NP. Natural history of periodontitis: disease progression and tooth loss over 40 years. J Clin Periodontol. 2017;44:1182–91. https://doi.org/10.1111/jcpe.12782.
Naka O, Anastassiadou V, Pissiotis A. Association between functional tooth units and chewing ability in older adults: a systematic review. Gerodontology. 2014;31:166–77. https://doi.org/10.1111/ger.12016.
Iwasaki M, Hirano H, Ohara Y, Motokawa K. The association of oral function with dietary intake and nutritional status among older adults: latest evidence from epidemiological studies. Jpn Dent Sci Rev. 2021;57:128–37. https://doi.org/10.1016/j.jdsr.2021.07.002.
Ritchie CS, Joshipura K, Hung HC, Douglass CW. Nutrition as a mediator in the relation between oral and systemic disease: associations between specific measures of adult oral health and nutrition outcomes. Crit Rev Oral Biol Med. 2002;13:291–300. https://doi.org/10.1177/154411130201300306.
Yao B, Fang H, Xu W, Yan Y, Xu H, Liu Y, Mo M, Zhang H, Zhao Y. Dietary fiber intake and risk of type 2 diabetes: a dose–response analysis of prospective studies. Eur J Epidemiol. 2014;29:79–88. https://doi.org/10.1007/s10654-013-9876-x.
Fang X, Han H, Li M, Liang C, Fan Z, Aaseth J, He J, Montgomery S, Cao Y. Dose–response relationship between dietary magnesium intake and risk of type 2 diabetes mellitus: a systematic review and meta-regression analysis of prospective cohort studies. Nutrients. 2016;8:739. https://doi.org/10.3390/nu8110739.
Gil-Montoya JA, de Mello AL, Barrios R, Gonzalez-Moles MA, Bravo M. Oral health in the elderly patient and its impact on general well-being: a nonsystematic review. Clin Interv Aging. 2015;10:461–7. https://doi.org/10.2147/cia.s54630.
Suzuki H, Fukushima M, Okamoto S, Takahashi O, Shimbo T, Kurose T, Yamada Y, Inagaki N, Seino Y, Fukui T. Effects of thorough mastication on postprandial plasma glucose concentrations in nonobese Japanese subjects. Metabolism. 2005;54:1593–9. https://doi.org/10.1016/j.metabol.2005.06.006.
Yamazaki T, Yamori M, Asai K, Nakano-Araki I, Yamaguchi A, Takahashi K, Sekine A, Matsuda F, Kosugi S, Nakayama T, Inagaki N, Bessho K, Nagahama study collaboration group. Mastication and risk for diabetes in a Japanese population: a cross-sectional study. PLoS ONE. 2013;8:e64113. https://doi.org/10.1371/journal.pone.0064113.
Abe T, Tominaga K, Ando Y, Toyama Y, Takeda M, Yamasaki M, Okuyama K, Hamano T, Isomura M, Nabika T, Yano S. Number of teeth and masticatory function are associated with sarcopenia and diabetes mellitus status among community-dwelling older adults: a Shimane CoHRE study. PLoS ONE. 2021;16: e0252625. https://doi.org/10.1371/journal.pone.0252625.
Ministry of Health, Labor and Welfare. Specific health checkups and specific health guidance; 2013. https://www.mhlw.go.jp/bunya/shakaihosho/iryouseido01/info03d.html. Accessed 16 Dec 2022
Divney AA, Murillo R, Rodriguez F, Mirzayi CA, Tsui EK, Echeverria SE. Diabetes prevalence by leisure-, transportation-, and occupation-based physical activity among racially/ethnically diverse U.S. adults. Diabet Care. 2019;42:1241–7. https://doi.org/10.2337/dc18-2432.
Tominaga K, Ando Y. A Study of the consistency between subjective and objective evaluation of mastication. J Dent Health. 2007;57:166–75.
Kudo A, Asahi K, Satoh H, Iseki K, Moriyama T, Yamagata K, et al. Fast eating is a strong risk factor for new-onset diabetes among the Japanese general population. Sci Rep. 2019;9:8210. https://doi.org/10.1038/s41598-019-44477-9.
Vittinghoff E, McCulloch CE. Relaxing the rule of ten events per variable in logistic and Cox regression. Am J Epidemiol. 2006;165:710–8. https://doi.org/10.1093/aje/kwk052.
Van Der Bilt A. Assessment of mastication with implications for oral rehabilitation: a review. J Oral Rehabil. 2011;38:754–80. https://doi.org/10.1111/j.1365-2842.2010.02197.x.
Kiesswetter E, Hengeveld LM, Keijser BJF, Volkert D, Visser M. Oral Health determinants of incident malnutrition in community-dwelling older adults. J Dent. 2019;85:73–80. https://doi.org/10.1016/j.jdent.2019.05.017.
Fushida S, Kosaka T, Nakai M, Kida M, Nokubi T, Kokubo Y, Watanabe M, Miyamoto Y, Ono T, Ikebe K. Lower masticatory performance is a risk for the development of the metabolic syndrome: The Suita Study. Front CardiovascMed. 2021;8: 752667. https://doi.org/10.3389/fcvm.2021.752667.
Sheiham A, Steele J. Does the condition of the mouth and teeth affect the ability to eat certain foods, nutrient and dietary intake and nutritional status amongst older people? Public Health Nutr. 2001;4:797–803. https://doi.org/10.1079/phn2000116.
Bui FQ, Almeida-da-Silva CLC, Huynh B, Trinh A, Liu J, Woodward J, Asadi H, Ojcius DM. Association between periodontal pathogens and systemic disease. Biomed J. 2019;42:27–35. https://doi.org/10.1016/j.bj.2018.12.001.
Borgnakke WS, Ylöstalo PV, Taylor GW, Genco RJ. Effect of periodontal disease on diabetes: systematic review of epidemiologic observational evidence. J Periodontol. 2013;84:S135–52. https://doi.org/10.1902/jop.2013.1340013.
Graves DT, Liu R, Alikhani M, Al-Mashat H, Trackman PC. Diabetes-enhanced inflammation and apoptosis–impact on periodontal pathology. J Dent Res. 2006;85:15–21. https://doi.org/10.1177/154405910608500103.
Ministry of Health, Labour and Welfare of Japan: The National Health and Nutrition Survey in Japan, 2019 (December, 2020). https://www.mhlw.go.jp/content/000710991.pdf (2019).
Okada A, Yasunaga H. Prevalence of noncommunicable diseases in Japan using a newly developed administrative claims database covering young, middle-aged, and elderly people. JMA J. 2022. https://doi.org/10.31662/jmaj.2021-0189.
Gonçalves TMSV, Schimmel M, van der Bilt A, Chen J, van der Glas HW, Kohyama K, Hennequin M, Peyron MA, Woda A, Leles CR, José PL. Consensus on the terminologies and methodologies for masticatory assessment. J Oral Rehabil. 2021;48:745–61. https://doi.org/10.1111/joor.13161.
Graziani F, Gennai S, Solini A, Petrini M. A systematic review and meta-analysis of epidemiologic observational evidence on the effect of periodontitis on diabetes An update of the EFP-AAP review. J Clin Periodontol. 2018;45:167–87. https://doi.org/10.1111/jcpe.12837.
Glurich I, Acharya A. Updates from the evidence base examining association between periodontal disease and type 2 diabetes mellitus: current status and clinical relevance. Curr Diabetes Rep. 2019;19:121. https://doi.org/10.1007/s11892-019-1228-0.
Jawed M, Shahid SM, Qader SA, Azhar A. Dental caries in diabetes mellitus: role of salivary flow rate and minerals. J Diabetes Complications. 2011;25:183–6. https://doi.org/10.1016/j.jdiacomp.2010.07.001.
Teshome A, Yitayeh A. The effect of periodontal therapy on glycemic control and fasting plasma glucose level in type 2 diabetic patients: systematic review and meta-analysis. BMC Oral Health. 2016;17:31. https://doi.org/10.1186/s12903-016-0249-1.
Engebretson S, Kocher T. Evidence that periodontal treatment improves diabetes outcomes: a systematic review and meta-analysis. J Periodontol. 2013;84:S153–69. https://doi.org/10.1902/jop.2013.1340017.
Wang X, Han X, Guo X, Luo X, Wang D. The effect of periodontal treatment on hemoglobin a1c levels of diabetic patients: a systematic review and meta-analysis. PLoS ONE. 2014;9: e108412. https://doi.org/10.1371/journal.pone.0108412.
Furuta M, Shimazaki Y, Takeshita T, Shibata Y, Akifusa S, Eshima N, Kiyohara Y, Ninomiya T, Hirakawa Y, Mukai N, Nagata M, Yamashita Y. Gender differences in the association between metabolic syndrome and periodontal disease: the Hisayama Study. J Clin Periodontol. 2013;40:743–52. https://doi.org/10.1111/jcpe.12119.
Acknowledgements
We greatly appreciate the cooperation from participants in Ohnan Town and thank the Shimane CoHRE study members for their skillful assistance.
Funding
This study was supported by the Japan Society for the Promotion of Science (KAKENHI; Grant number 16K13029). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
MI and TN organized and conducted the study. TA. and TH. collected data. KT, TA, and SY performed the statistical analysis, interpreted the results, proposed the structure of the paper, and formulated the paper. YA and TH made substantial contributions to the data analysis and draft revision. MI and TN critically appraised the paper and made final suggestions. All the authors reviewed and revised the manuscript and agreed to the submission of the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Kazumichi Tominaga, Takafumi Abe, Yuichi Ando, Tsuyoshi Hamano, Minoru Isomura, Toru Nabika, and Shozo Yano declare that they have no conflicts of interest.
Human rights
All the procedures followed were in accordance with the ethical standards of the Medical Research Ethics Committee, Shimane University Faculty of Medicine (May 11, 2017/#20051214-3) and with the Helsinki Declaration of 1964 and later versions.
Informed consent to participate
Residents provided consent via signature to participate in the study after receiving written and oral explanations of the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Tominaga, K., Abe, T., Ando, Y. et al. Changes in masticatory performance and the new onset of diabetes mellitus in older adults: a 5-year longitudinal study. Diabetol Int 14, 165–171 (2023). https://doi.org/10.1007/s13340-022-00613-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13340-022-00613-x