Abstract
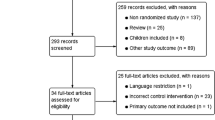
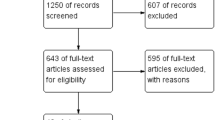
To compare the outcomes of three-port and four-port laparoscopic cholecystectomy. In compliance with PRISMA statement standards, electronic databases were searched to identify all comparative studies investigating outcomes of three-port vs four-port laparoscopic cholecystectomy. Two techniques were compared using direct comparison meta-analysis model. The risks of type 1 or type 2 error in the meta-analysis model were assessed using trial sequential analysis model. The certainty of evidence was assessed using GRADE system. Random effects modelling was applied to calculate pooled outcome data. Analysis of 2524 patients from 17 studies showed that both techniques were comparable in terms of operative time (MD:− 0.13, P = 0.88), conversion to open operation (OR:0.80, P = 0.43), gallbladder perforation (OR: 1.43, P = 0.13), bleeding from gallbladder bed (OR:0.81, P = 0.34), bile duct injury (RD: 0.00, P = 0.97), iatrogenic visceral injury (RD: − 0.00, P = 0.81), bile or stone spillage (OR:1.67, P = 0.08), port site infection (OR: 0.90, P = 0.76), port site hernia (RD: 0.00, P = 0.89), port site haematoma (RD: − 0.01, P = 0.23), port site seroma (RD: 0.00, P = 1.00), and need for reoperation (RD: − 0.00, P = 0.94). However, the three-port technique was associated with lower VAS pain score at 12 h (MD: − 0.66, P < 0.00001) and 24 h (MD: − 0.54, P < 0.00001) postoperatively, shorter length of hospital stay (MD:-0.09, P = 0.41), and shorter time to return to normal activities (MD: − 0.79, P = 0.02). Trial sequential analysis confirmed that the meta-analysis was conclusive with no significant risks of type 1 or type 2 error. Robust evidence (level 1 with high certainty) suggests that in an elective setting with uncomplicated cholelithiasis as indication for cholecystectomy, three-port laparoscopic cholecystectomy is comparable with the four-port technique in terms of procedural and morbidity outcomes and may be associated with less postoperative pain, shorter length of hospital stay and shorter time to return to normal activities.












Similar content being viewed by others
References
Litynski GS (1999) Profiles in laparoscopy: Mouret, Dubois, and Perissat: the laparoscopic breakthrough in Europe (1987–1988). JSLS 3(2):163–167
Antoniou SA, Antoniou GA, Koch OO, Pointner R, Granderath FA (2014) Meta-analysis of laparoscopic vs open cholecystectomy in elderly patients. World J Gastroenterol 20(46):17626–17634
Coccolini F, Catena F, Pisano M, Gheza F, Fagiuoli S, Di Saverio S et al (2015) Open versus laparoscopic cholecystectomy in acute cholecystitis. Systematic review and meta-analysis. Int J Surg 18:196–204
Arezzo A, Passera R, Forcignanò E, Rapetti L, Cirocchi R, Morino M (2018) Single-incision laparoscopic cholecystectomy is responsible for increased adverse events: results of a meta-analysis of randomized controlled trials. Surg Endosc 32(9):3739–3753
Liberati A, Altman DG, Tetzlaff J et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700
Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (eds) (2019) Cochrane handbook for systematic reviews of interventions, 2nd edn. Wiley, Chichester (UK)
Thorlund K, Engstrøm J, Wetterslev JG, Brok J, Imberger Gluud C (2011) User manual for trial sequential analysis (TSA). Copenhagen Trial Unit, Centre for Clinical Intervention Research, Copenhagen, Denmark. 2011. . p. 1–115. Available at www.ctu.dk/tsa. Accessed 28 Nov 2020
Schünemann H, Brożek J, Guyatt G, Oxman A (2013) GRADE handbook for grading quality of evidence and strength of recommendations. Updated October 2013. The GRADE Working Group, 2013. Available at GRADE handbook (gradepro.org). Accessed 28 Nov 2020
Higgins JPT, Savović J, Page MJ, Elbers RG, Sterne JAC. Chapter 8: Assessing risk of bias in a randomized trial. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.1 (updated September 2020). Cochrane, 2020. Available from www.training.cochrane.org/handbook. Accessed 28 Nov 2020
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919
Koirala R, Gurung T, Rajbhandari A, Rai P (2019) Three-port versus four-port laparoscopic cholecystectomy: a randomized controlled trial. Nepal Med Coll J 21(1):40–43
Mirza AA, Asif M, Sukh N, Saeed A, Jamil K, Zaidi AH (2017) Outcome of three ports versus four ports laparoscopic cholecystectomy in terms of mean operative time, hospital stay and pain. Ann Pak Inst Med Sci 13(2):169–172
Shah SF, Waqar SH, Chaudry MA, Hameed S (2017) Three ports versus four ports laparoscopic cholecystectomy. RMJ 42(3):359–362
Sharma PK, Mehta KS (2017) Three port versus standard four port laparoscopic cholecystectomy—a prospective study. JK Sci 17(1):38–42
Khorgami Z, Shoar S, Anbara T, Soroush A, Nasiri S, Movafegh A et al (2014) A randomized clinical trial comparing 4-port, 3-port, and single-incision laparoscopic cholecystectomy. J Invest Surg 27(3):147–154
Harsha HS, Gunjiganvi M, Singh C, Moirangthem GS (2013) A study of three-port versus four-port laparoscopic cholecystectomy. J Med Soc 27:208–211
Mohamed AE, Zaazou MM (2020) Three-port versus conventional four-port laparoscopic cholecystectomy: a comparative study. Egypt J Surg 39:119–123
Kumar M, Agrawal CS, Gupta RK (2007) Three-port versus standard four-port laparoscopic cholecystectomy: a randomized controlled clinical trial in a community-based teaching hospital in eastern Nepal. JSLS 11(3):358–362
Hashimoto D, Hirota M, Yagi Y, Baba H (2011) Umbilicus saving three-port laparoscopic cholecystectomy. Webmed Cent Laparosc 2(4):WMC001882
Eroler E, Dilektasli E, Tihan D, Duman U, Bayam EM, Erol FM et al (2016) Reducing one port in laparoscopic cholecystectomy: does that really make a difference? Int J Clin Exp Med 9(6):11558–11565
Akay T, Örün S, Leblebici M (2019) Three-port versus standard four-port laparoscopic cholecystectomy: a clinical trial. Laparosc Endosc Surg Sci 26(4):175–180
Al-Azawi D, Houssein N, Rayis AB, McMahon D, Hehir DJ (2007) Three-port versus four-port laparoscopic cholecystectomy in acute and chronic cholecystitis. BMC Surg 13(7):8
Bari S, Islam F, Rather A, Malik A (2019) Three port versus four port laparoscopic cholecystectomy: a prospective comparative clinical study. Int J Res Med Sci 7(8):3054–3059
Kumar A, Kumar D, Gupta P, Shakya JPS (2018) Three port versus four port laparoscopic cholecystectomy: a comparative study. Indian J Appl Res 8(10):18–20
Mayir B, Dogan U, Koc U, Aslaner A, Bılecık T, Ensarı CO et al (2014) Safety and effectiveness of three-port laparoscopic cholecystectomy. Int J Clin Exp Med 7(8):2339–2342
Reshie AA, Rather ZM, Bhat MY, Salroo NA, Majid AN, Ahmed MM (2015) Three port versus four port laparoscopic cholecystectomy: a comparative study. Int J of Adv Res 3:1040–1044
Wilkinson TRV, Mehrotra P, Bansod P, Akhtar M (2017) Three port versus four port laparoscopic cholecystectomy—a prospective study. Int J Med Res Rev 5(03):235–241
Sun S, Yang K, Gao M, He X, Tian J, Ma B (2009) Three-port versus four-port laparoscopic cholecystectomy: meta-analysis of randomized clinical trials. World J Surg 33(9):1904–1908
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
Conception and design: TS, SH. Data collection: DAF, SH. Analysis and interpretation: all authors. Writing the article: SH, DAF. Critical revision of the article: all authors. Final approval of the article: all authors. Statistical analysis: SH, AYYM, SH, DAF.
Corresponding author
Ethics declarations
Conflict of interest
All authors included in this work declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix I
Appendix I
Search No | Search strategya |
|---|---|
#1 | Three port: TI,AB,KW |
#2 | Three-port: TI,AB,KW |
#3 | 3-Port: TI,AB,KW |
#4 | 3 Port: TI,AB,KW |
#5 | #1 OR #2 OR #3 OR #4 |
#6 | Four port: TI,AB,KW |
#7 | Four-port: TI,AB,KW |
#8 | 4-Port: TI,AB,KW |
#9 | 4 Port: TI,AB,KW |
#10 | Standard: TI,AB,KW |
#11 | Conventional: TI,AB,KW |
#12 | #6 OR #7 OR #8 OR #9 OR #10 OR #11 |
#13 | MeSH descriptor: [laparoscopic cholecystectomy] explode all trees |
#14 | Laparosco* near2 cholecystectomy: TI,AB,KW |
#15 | Cholecystectomy: TI,AB,KW |
#16 | #13 OR #14 OR #15 |
#17 | #5 AND #11 AND #16 |
Rights and permissions
About this article
Cite this article
Hajibandeh, S., Finch, D.A., Mohamedahmed, A.Y.Y. et al. Meta-analysis and trial sequential analysis of three-port vs four-port laparoscopic cholecystectomy (level 1 evidence). Updates Surg 73, 451–471 (2021). https://doi.org/10.1007/s13304-021-00982-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13304-021-00982-z