Abstract
Purpose
The cross-limb (CL) technique is a commonly used endovascular treatment for addressing unfavorable anatomical features in patients with abdominal aortic aneurysm (AAA). The configuration of CL stent-graft plays a critical role in determining the postoperative hemodynamic properties and physiological behaviors, which ultimately impact the efficacy and safety of endovascular AAA treatment. This study aims to investigate the relationship between hemodynamics and CL stent-graft configuration from a hemodynamic perspective.
Methods
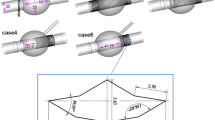
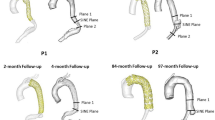
Five distinct geometric models of cross-limb (CL) stent-graft configurations were constructed by optimizing the real clinical computed tomography angiography (CTA) data. These models varied in main body lengths and cross angles and were used to perform numerical simulations to analyze various hemodynamic parameters. Flow pattern, distribution of wall shear stress (WSS)-related parameters, localized normalized helicity (LNH), pressure drop, and the displacement force of all models were examined in this paper.
Results
In patient-specific cases, helical flow and WSS increase with the main body. However, it also generated secondary flow in localized areas, leading to increased oscillation in the WSS direction. Notably, increasing the stent graft’s main body length or decreasing the cross angle reduced the displacement force exerted on the stent-graft. Reducing the cross angle did not significantly alter the hemodynamic characteristics.
Conclusion
In the clinical practice of CL deployment, it is crucial to carefully consider the stent-graft configuration and the patient specific to achieve optimal postoperative outcomes. This study provides valuable insights for guiding stent selection and treatment planning in patients with abdominal aortic aneurysm undergoing CL techniques, from a hemodynamic perspective.










Similar content being viewed by others
Data Availability
The datasets used and/or analyzed during the current study available from the corresponding author on reasonable request.
References
Yue, J., Y. Zhao, J. Wang, Y. Fan, and T. Zheng. Comparison of stent displacement and displacement force after endovascular aneurysm repair with cross-limb or parallel-limb stent. Sheng Wu Yi Xue Gong Cheng Xue Za Zhi. 39:645–650, 2022. https://doi.org/10.7507/1001-5515.202107038.
Wang, J., J. Zhao, Y. Ma, B. Huang, Y. Yang, D. Yuan, C. Weng, and T. Wang. Mid term outcomes of crossed limb vs. standard limb configuration in endovascular abdominal aortic aneurysm repair: a propensity score analysis. Eur. J. Vasc. Endovasc. Surg. 61:579–588, 2021. https://doi.org/10.1016/j.ejvs.2021.01.018.
Ashraf, F., T. Ambreen, C. W. Park, and D.-I. Kim. Comparative evaluation of ballet-type and conventional stent graft configurations for endovascular aneurysm repair: a CFD analysis. Clin. Hemorheol. Microcirc. 78:1–27, 2021. https://doi.org/10.3233/CH-200996.
Dattani, N., J. Wild, D. Sidloff, G. Fishwick, M. Bown, E. Choke, and R. Sayers. Outcomes following limb crossing in endovascular aneurysm repairs. Vasc. Endovasc. Surg. 49:52–57, 2015. https://doi.org/10.1177/1538574415587512.
Yagihashi, K., H. Nishimaki, Y. Ogawa, K. Chiba, K. Murakami, D. Ro, H. Ono, Y. Sakurai, T. Miyairi, and Y. Nakajima. Early and mid-term results of endovascular aortic repair using a crossed-limb technique for patients with severely splayed iliac angulation. Ann. Vasc. Dis. 11:91–95, 2018. https://doi.org/10.3400/avd.oa.16-00135.
Saha, P., J. Hughes, A. S. Patel, T. Donati, M. Sallam, S. D. Patel, R. E. Bell, K. Katsanos, B. Modarai, and H. A. Zayed. Medium-term outcomes following endovascular repair of infrarenal abdominal aortic aneurysms with an unfavourable proximal neck. Cardiovasc. Interv. Radiol. 38:840–845, 2015. https://doi.org/10.1007/s00270-014-1038-3.
Georgiadis, G. S., E. I. Georgakarakos, G. A. Antoniou, G. Trellopoulos, A. Christos, E. S. Nikolopoulos, D. Charalampidis, N. G. Schoretsanitis, and M. K. Lazarides. Clinical outcomes after crossed-limb vs. conventional endograft configuration in endovascular AAA repair. J. Endovasc. Ther. 20:853–862, 2013. https://doi.org/10.1583/13-4286MR.1.
Rödel, S. G. J., R. H. Geelkerken, R. J. Prescott, H. J. Florek, P. Kasprzak, and J. Brunkwall. The AnacondaTM AAA stent graft system: 2-year clinical and technical results of a multicentre clinical evaluation. Eur. J. Vasc. Endovasc. Surg. 38:732–740, 2009. https://doi.org/10.1016/j.ejvs.2009.08.007.
Qiao, Y., L. Mao, Y. Ding, T. Zhu, K. Luo, and J. Fan. Fluid-structure interaction: Insights into biomechanical implications of endograft after thoracic endovascular aortic repair. Comput. Biol. Med.138:104882, 2021. https://doi.org/10.1016/j.compbiomed.2021.104882.
Hirschhorn, M., V. Tchantchaleishvili, R. Stevens, J. Rossano, and A. Throckmorton. Fluid–structure interaction modeling in cardiovascular medicine—a systematic review 2017–2019. Med. Eng. Phys. 78:1–13, 2020. https://doi.org/10.1016/j.medengphy.2020.01.008.
Amirbekian, S., R. C. Long, M. A. Consolini, J. Suo, N. J. Willett, S. W. Fielden, D. P. Giddens, W. R. Taylor, and J. N. Oshinski. In vivo assessment of blood flow patterns in abdominal aorta of mice with MRI: implications for AAA localization. Am. J. Physiol. Heart Circ. Physiol. 297:H1290–H1295, 2009. https://doi.org/10.1152/ajpheart.00889.2008.
Harrison, S. C., A. J. Winterbottom, P. A. Coughlin, P. D. Hayes, and J. R. Boyle. Editor’s choice—mid-term migration and device failure following endovascular aneurysm sealing with the Nellix stent graft system—a single centre experience. Eur. J. Vasc. Endovasc. Surg. 56:342–348, 2018. https://doi.org/10.1016/j.ejvs.2018.06.031.
Georgakarakos, E., A. Xenakis, C. Manopoulos, G. S. Georgiadis, S. Tsangaris, and M. Lazarides. Geometric factors affecting the displacement forces in an aortic endograft with crossed limbs: a computational study. J. Endovasc. Ther. 20:191–199, 2013. https://doi.org/10.1583/1545-1550-20.2.191.
Liu, M., A. Sun, and X. Deng. Numerical and experimental investigation of the hemodynamic performance of bifurcated stent grafts with various torsion angles. Sci. Rep. 8:12625, 2018. https://doi.org/10.1038/s41598-018-31015-2.
Georgakarakos, E., A. Xenakis, and G. S. Georgiadis. Estimating the hemodynamic influence of variable main body-to-iliac limb length ratios in aortic endografts. Int. Angiol. 37:41–45, 2018. https://doi.org/10.23736/S0392-9590.17.03883-4.
Kandail, H., M. Hamady, and X. Y. Xu. Patient-specific analysis of displacement forces acting on fenestrated stent grafts for endovascular aneurysm repair. J. Biomech. 47:3546–3554, 2014. https://doi.org/10.1016/j.jbiomech.2014.08.011.
Georgakarakos, E., C. Argyriou, N. Schoretsanitis, C. V. Ioannou, N. Kontopodis, R. Morgan, and D. Tsetis. Geometrical factors influencing the hemodynamic behavior of the AAA stent grafts: essentials for the clinician. Cardiovasc. Interv. Radiol. 37:1420–1429, 2014. https://doi.org/10.1007/s00270-014-0927-9.
Zhan, F., Y. Fan, and X. Deng. Swirling flow created in a glass tube suppressed platelet adhesion to the surface of the tube: its implication in the design of small-caliber arterial grafts. Thromb. Res. 125:413–418, 2010. https://doi.org/10.1016/j.thromres.2009.02.011.
Stefanov, F., T. McGloughlin, and L. Morris. A computational assessment of the hemodynamic effects of crossed and non-crossed bifurcated stent-graft devices for the treatment of abdominal aortic aneurysms. Med. Eng. Phys. 38:1458–1473, 2016. https://doi.org/10.1016/j.medengphy.2016.09.011.
Liu, M., A. Sun, and X. Deng. Hemodynamic performance within crossed stent grafts: computational and experimental study on the effect of cross position and angle. Biomed. Eng. Online. 17:85, 2018. https://doi.org/10.1186/s12938-018-0517-1.
Perinajova, R., J. F. Juffermans, J. J. M. Westenberg, R. L. F. van der Palen, P. J. van den Boogaard, H. J. Lamb, and S. Kenjeres. Geometrically induced wall shear stress variability in CFD-MRI coupled simulations of blood flow in the thoracic aortas. Comput. Biol. Med.133:104385, 2021. https://doi.org/10.1016/j.compbiomed.2021.104385.
Pinho, N., L. C. Sousa, C. F. Castro, C. C. Antonio, M. Carvalho, W. Ferreira, R. Ladeiras-Lopes, N. D. Ferreira, P. Braga, N. Bettencourt, and S. I. S. Pinto. The impact of the right coronary artery geometric parameters on hemodynamic performance. Cardiovasc. Eng. Technol. 10:257–270, 2019. https://doi.org/10.1007/s13239-019-00403-8.
Campinho, P., A. Vilfan, and J. Vermot. Blood flow forces in shaping the vascular system: a focus on endothelial cell behavior. Front. Physiol. 2020. https://doi.org/10.3389/fphys.2020.00552. Accessed April 7, 2023.
Krüger-Genge, A., A. Blocki, R.-P. Franke, and F. Jung. Vascular endothelial cell biology: an update. Int. J. Mol. Sci. 20:4411, 2019. https://doi.org/10.3390/ijms20184411.
Courtial, E.-J., L. Fanton, M. Orkisz, P. C. Douek, L. Huet, and R. Fulchiron. Hyper-viscoelastic behavior of healthy abdominal aorta. IRBM. 37:158–164, 2016. https://doi.org/10.1016/j.irbm.2016.03.007.
Shek, T. L. T., L. W. Tse, A. Nabovati, and C. H. Amon. Computational fluid dynamics evaluation of the cross-limb stent graft configuration for endovascular aneurysm repair. J. Biomech. Eng. 2012. https://doi.org/10.1115/1.4007950.
De Nisco, G., A. Hoogendoorn, C. Chiastra, D. Gallo, A. M. Kok, U. Morbiducci, and J. J. Wentzel. The impact of helical flow on coronary atherosclerotic plaque development. Atherosclerosis. 300:39–46, 2020. https://doi.org/10.1016/j.atherosclerosis.2020.01.027.
Liu, X., A. Sun, Y. Fan, and X. Deng. Physiological significance of helical flow in the arterial system and its potential clinical applications. Ann. Biomed. Eng. 43:3–15, 2015. https://doi.org/10.1007/s10439-014-1097-2.
De Nisco, G., A. M. Kok, C. Chiastra, D. Gallo, A. Hoogendoorn, F. Migliavacca, J. J. Wentzel, and U. Morbiducci. The atheroprotective nature of helical flow in coronary arteries. Ann. Biomed. Eng. 47:425–438, 2019. https://doi.org/10.1007/s10439-018-02169-x.
Avgerinos, E. D., I. Dalainas, J. Kakisis, K. Moulakakis, T. Giannakopoulos, and C. D. Liapis. Endograft accommodation on the aortic bifurcation: an overview of anatomical fixation and implications for long-term stent-graft stability. J. Endovasc. Ther. 18:462–470, 2011. https://doi.org/10.1583/11-3411.1.
Qiu, Y., D. Yuan, Y. Wang, J. Wen, and T. Zheng. Hemodynamic investigation of a patient-specific abdominal aortic aneurysm with iliac artery tortuosity. Comput. Methods Biomech. Biomed. Eng. 21:824–833, 2018. https://doi.org/10.1080/10255842.2018.1522531.
Heidari, A., S. Rahmani, C. Pop, B. Saed, A. Mahpour, M. Navidbakhsh, and M. Alizadeh. Three-dimensional computational modeling of an extra-descending aortic assist device using fluid-structure interaction. IRBM. 42:35–47, 2021. https://doi.org/10.1016/j.irbm.2020.11.003.
Meng, H., V. M. Tutino, J. Xiang, and A. Siddiqui. High WSS or low WSS? Complex interactions of hemodynamics with intracranial aneurysm initiation, growth, and rupture: toward a unifying hypothesis. Am. J. Neuroradiol. 35:1254–1262, 2014. https://doi.org/10.3174/ajnr.A3558.
Malek, A. M. Hemodynamic shear stress and its role in atherosclerosis. JAMA. 282:2035, 1999. https://doi.org/10.1001/jama.282.21.2035.
Li, F., Y. Zhu, H. Song, H. Zhang, L. Chen, and W. Guo. Analysis of postoperative remodeling characteristics after modular inner branched stent-graft treatment of aortic arch pathologies using computational fluid dynamics. Bioengineering. 10:164, 2023. https://doi.org/10.3390/bioengineering10020164.
Liffman, K., M. M. Lawrence-Brown, J. B. Semmens, A. Bui, M. Rudman, and D. E. Hartley. Analytical modeling and numerical simulation of forces in an endoluminal graft. J. Endovasc. Ther. 8:358–371, 2001. https://doi.org/10.1583/1545-1550(2001)008%3c0358:AMANSO%3e2.0.CO;2.
Veerapen, R., A. Dorandeu, I. Serre, J.-P. Berthet, C. H. Marty-Ane, H. Mary, and P. Alric. Improvement in proximal aortic endograft fixation: an experimental study using different stent-grafts in human cadaveric aortas. J. Endovasc. Ther. 10:1101–1109, 2003. https://doi.org/10.1177/152660280301000613.
Funding
This work was funded by Open Foundation of Institute of Human Biomechanics, Ningbo University (CJ-HBIO202103), National Natural Science Foundation of China [12002231], the Beijing Municipal Natural Science Foundation [7212095], Ningbo Natural Science Foundation (2021J240), “1331 project” Key Innovation Teams of Shanxi Province, and Central Guidance on Local Science and Technology Development Found of Shanxi Province (YDZJSX2021A021).
Author information
Authors and Affiliations
Contributions
YX: contributed to writing part of original draft, YZ and HZ: contributed to the design of the study, YS and YZ: contributed to processing the results of the calculation, FL: designing of the study and reconstructed the CADs, HS: performed the numerical simulation, LC: validated the numerical results, WG: co-supervised the research. All authors have read and agreed to the published version of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Ethical Approval
Any potentially identifiable images or data included in this article has been released with the individual’s written informed consent.
Additional information
Associate Editor Alison Marsden, Ph.D. oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xie, Y., Zhu, Y., Shi, Y. et al. Impact of Cross-Limb Stent-Graft Configuration on Hemodynamics in Abdominal Aortic Aneurysm Interventional Therapy. Cardiovasc Eng Tech (2023). https://doi.org/10.1007/s13239-023-00702-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s13239-023-00702-1