Abstract
Purpose
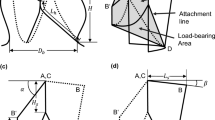
Pulmonary valve (PV) monocusp reconstruction in transannular patch (TAP) right ventricular outflow tract (RVOT) repair for Tetralogy of Fallot has variable clinical outcomes across different surgical approaches. The study purpose was to systematically evaluate how monocusp leaflet design parameters affect valve function in-vitro.
Methods
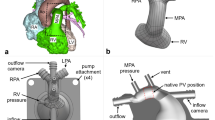
A 3D-printed, disease-specific RVOT model was tested under three infant physiological conditions. Monocusps were sewn into models with the native main pulmonary artery (MPA) forming backwalls that constituted 40% and 50% of the reconstructed circumference for z-score zero PV annulus and MPA diameters (native PV z-score − 3.52 and − 2.99 for BSA 0.32m2). Various leaflet free edge lengths (FEL) (relative to backwall), positions (relative to PV STJ), and scallop depths were investigated across both models. Pressure gradient, regurgitation, and coaptation were analyzed with descriptive statistics and regression models.
Results
Increasing FEL beyond 100% of the MPA backwall decreased gradient but mildly increased regurgitation to a peak of 25%. Positioning the free edge 2 mm past the STJ mildly increased gradient for each FEL without significantly changing regurgitation compared to STJ placement. Scalloping leaflets trivially affected performance. Pre-folding leaflets improved mobility and slightly reduced gradient.
Conclusions
Balancing gradient, regurgitation, and oversizing for growth, a set of leaflet designs have been selected for pre-clinical evaluation. Designs with leaflet widths 140–160% in the 40% backwall model (110–120% in the 50% backwall), positioned at or 2 mm past the STJ, demonstrated the best results. The next stage of ex-vivo testing will additionally consider native RVOT distensibility, native leaflet interactions, and TAP characteristics.








Similar content being viewed by others
Abbreviations
- BW:
-
Backwall (native MPA tissue in TAP repair)
- CI:
-
Cardiac Index
- ePTFE:
-
Expanded Polytetrafluoroethylene
- FEL:
-
Free Edge Length
- HCO:
-
High Cardiac Output
- HPVR:
-
High Pulmonary Vascular Resistance
- MPA:
-
Main Pulmonary Artery
- MCL:
-
Mock Circulatory Loop
- PI:
-
Pulmonary Insufficiency
- PV:
-
Pulmonary Valve
- RV:
-
Right Ventricle
- RVOT:
-
Right Ventricular Outflow Tract
- RVOTO:
-
Right Ventricular Outflow Tract Obstruction
- STJ:
-
Sinotubular Junction
- TAP:
-
Transannular Patch
- TOF:
-
Tetralogy of Fallot
- TPU:
-
Thermoplastic Polyurethane
References
F. A. Pigula, P. N. Khalil, J. E. Mayer, P. J. Del Nido, and R. A. Jonas, “Repair of tetralogy of Fallot in neonates and young infants,” Circulation, vol. 100, no. 19 SUPPL. 1999. https://doi.org/10.1161/circ.100.suppl_2.ii-157.
A. R. Castaneda, M. D. Freed, R. G. Williams, and W. I. Norwood, “Repair of tetralogy of Fallot in infancy. Early and late results,” Journal of Thoracic and Cardiovascular Surgery, vol. 74, no. 3, pp. 372–381, 1977, https://doi.org/10.1016/s0022-5223(19)41351-2.
M. N. Awori, W. Leong, J. H. Artrip, and C. O’Donnell, “Tetralogy of fallot repair: Optimal z-score use for transannular patch insertion,” European Journal of Cardio-thoracic Surgery, vol. 43, no. 3, pp. 483–486, 2013, https://doi.org/10.1093/ejcts/ezs372.
X. Wei et al., “Transannular patch repair of tetralogy of Fallot with or without monocusp valve reconstruction: a meta-analysis,” BMC Surgery, vol. 22, no. 1, pp. 1–11, 2022, https://doi.org/10.1186/s12893-022-01474-6.
N. M. Singh, R. S. Loomba, T. M. Gudausky, and M. E. Mitchell, “Monocusp valve placement in children with tetralogy of Fallot undergoing repair with transannular patch: A functioning pulmonary valve does not improve immediate postsurgical outcomes,” Congenital Heart Disease, vol. 13, no. 6, pp. 935–943, 2018, https://doi.org/10.1111/chd.12670.
V. A. Scavo et al., “Monocusp valve and transannular patch reconstruction of the right ventricular outflow tract: An experimental study,” ASAIO Journal, vol. 44, no. 5. 1998. https://doi.org/10.1097/00002480-199809000-00032.
S. Aydin et al., “The impact of pulmonary valve-sparing techniques on postoperative early and midterm results in tetralogy of Fallot repair,” Turkish Journal of Thoracic and Cardiovascular Surgery, vol. 26, no. 3, pp. 370–374, 2018, https://doi.org/10.5606/tgkdc.dergisi.2018.15499.
S. Pande, S. K. Agarwal, G. Majumdar, B. Chandra, P. Tewari, and S. Kumar, “Pericardial monocusp for pulmonary valve reconstruction: A new technique,” Asian Cardiovascular and Thoracic Annals, vol. 18, no. 3, pp. 279–284, 2010, https://doi.org/10.1177/0218492310369185.
S. Rawat et al., “Short-term outcome of polytetrafluoroethylene membrane valve versus transannular pericardial patch reconstruction of right ventricular outflow tract in tetralogy of Fallot: A randomized controlled trial,” Brazilian Journal of Cardiovascular Surgery, vol. 36, no. 1, pp. 39–47, 2021, https://doi.org/10.21470/1678-9741-2020-0059.
E. H. N. Sayyed, S. S. Rana, K. M. Anand, A. Eram, and S. Harkant, “Monocusp pulmonary valve reconstruction in childhood and adult TOF repairs: does a single cusped valve work?,” Indian Journal of Thoracic and Cardiovascular Surgery, vol. 32, no. 4, pp. 229–234, 2016, https://doi.org/10.1007/s12055-016-0457-y.
J. van den Berg et al., “Clinical condition at mid-to-late follow-up after transatrial-transpulmonary repair of tetralogy of Fallot,” Journal of Thoracic and Cardiovascular Surgery, vol. 133, no. 2, pp. 470–477, 2007, https://doi.org/10.1016/j.jtcvs.2006.10.022.
S. Attanawanich, M. Ngodgnamthaweesuk, N. Kitjanon, and C. Sitthisombat, “Pulmonary cusp augmentation in repair of tetralogy of Fallot,” Asian Cardiovascular and Thoracic Annals, vol. 21, no. 1, pp. 9–13, 2013, https://doi.org/10.1177/0218492312444284.
A. K. Kaza et al., “Long-term results of right ventricular outflow tract reconstruction in neonatal cardiac surgery: Options and outcomes,” Journal of Thoracic and Cardiovascular Surgery, vol. 138, no. 4, pp. 911–916, 2009, https://doi.org/10.1016/j.jtcvs.2008.10.058.
S. C. Hofferberth et al., “Valve-sparing repair with intraoperative balloon dilation in tetralogy of Fallot: Midterm results and therapeutic implications,” Journal of Thoracic and Cardiovascular Surgery, vol. 155, no. 3, pp. 1163–1173.e4, 2018, https://doi.org/10.1016/j.jtcvs.2017.08.147.
P. Anagnostopoulos, A. Azakie, S. Natarajan, N. Alphonso, M. M. Brook, and T. R. Karl, “Pulmonary valve cusp augmentation with autologous pericardium may improve early outcome for tetralogy of Fallot,” Journal of Thoracic and Cardiovascular Surgery, vol. 133, no. 3, pp. 640–647, 2007, https://doi.org/10.1016/j.jtcvs.2006.10.039.
M. W. Turrentine, R. P. McCarthy, P. Vijay, A. C. Fiore, and J. W. Brown, “Polytetrafluoroethylene monocusp valve technique for right ventricular outflow tract reconstruction,” Annals of Thoracic Surgery, vol. 74, no. 6, pp. 2202–2205, 2002, https://doi.org/10.1016/S0003-4975(02)03844-4.
A. Arya et al., “Assessment of untreated fresh autologous pericardium as material for construction of heart valve: Result at 5 years,” Annals of Cardiac Anaesthesia, vol. 22, no. 3, pp. 273–277, 2019, https://doi.org/10.4103/aca.ACA_50_18.
M. Homann et al., “Reconstruction of the RVOT with valved biological conduits: 25 Years experience with allografts and xenografts,” European Journal of Cardio-thoracic Surgery, vol. 17, no. 6, pp. 624–630, 2000, https://doi.org/10.1016/S1010-7940(00)00414-0.
M. W. Turrentine, R. P. McCarthy, P. Vijay, K. W. McConnell, and J. W. Brown, “PTFE monocusp valve reconstruction of the right ventricular outflow tract,” Annals of Thoracic Surgery, vol. 73, no. 3, pp. 871–880, 2002, https://doi.org/10.1016/S0003-4975(01)03441-5.
J. W. Brown, M. Ruzmetov, P. Vijay, M. D. Rodefeld, and M. W. Turrentine, “Right ventricular outflow tract reconstruction with a polytetrafluoroethylene monocusp valve: A twelve-year experience,” Journal of Thoracic and Cardiovascular Surgery, vol. 133, no. 5, pp. 1336–1343, 2007, https://doi.org/10.1016/j.jtcvs.2006.12.045.
M. Kumar, M. W. Turrentine, M. D. Rodefeld, T. Bell, and J. W. Brown, “Right Ventricular Outflow Tract Reconstruction With a Polytetrafluoroethylene Monocusp Valve: A 20-Year Experience,” Seminars in Thoracic and Cardiovascular Surgery, vol. 28, no. 2, pp. 463–470, 2016, https://doi.org/10.1053/j.semtcvs.2016.05.003.
R. B. B. Mee, “Fate of trileaflet equine pericardial extracardiac conduit used for the correction of anomalies having pulmonic ventricle-pulmonary arterial discontinuity: Invited commentary,” Annals of Thoracic Surgery, vol. 64, no. 1, p. 158, 1997, https://doi.org/10.1016/S0003-4975(97)00341-X.
L. A. Vricella, S. R. Gundry, H. Izutani, M. A. Kuhn, N. Mulla, and L. L. Bailey, “Fate of polytetrafluoroethylene monocusp pulmonary valves in animal model,” Asian Cardiovascular and Thoracic Annals, vol. 11, no. 4, pp. 280–284, 2003, https://doi.org/10.1177/021849230301100402.
L. Sasson et al., “Right ventricular outflow tract strategies for repair of tetralogy of Fallot: Effect of monocusp valve reconstruction,” European Journal of Cardio-thoracic Surgery, vol. 43, no. 4, pp. 743–751, 2013, https://doi.org/10.1093/ejcts/ezs479.
I. S. O. S. Order, “INTERNATIONAL STANDARD Cardiovascular implants — Cardiac valve prostheses — substitutes,” vol. 2015, no. 5840–3, pp. 15–17, 2015.
S. B. Kizilski et al., “An In Vitro Circulatory Loop Model of the Pediatric Right Ventricular Outflow Tract as a Platform for Valve Evaluation,” 2022.
Mishaly D, Birk E, Elami A, Vidne BA. Autologous monocusp pulmonary valve: Preliminary results. Ann Thorac Surg. 1996;61(6):1811–1815. https://doi.org/10.1016/0003-4975(96)00181-6
Gundry SR, Razzouk AJ, Boskind JF, et al. Fate of the pericardial monocusp pulmonary valve for right ventricular outflow tract reconstruction: Early function, late failure without obstruction. J Thorac Cardiovasc Surg. 1994;107(3):908–913. https://doi.org/10.1016/s0022-5223(94)70349-3
Roughneen PT, DeLeon SY, Parvathaneni S, Cetta F, Eidem B, Vitullo DA. The Pericardial Membrane Pulmonary Monocusp: Surgical Technique and Early Results. Echocardiography. 1985;2(5):370–374. https://doi.org/10.1111/j.1540-8175.1985.tb01309.x
Bigras JL, Boutin C, McCrindle BW, Rebeyka IM. Short-term effect of monocuspid valves on pulmonary insufficiency and clinical outcome after surgical repair of tetralogy of fallot. J Thorac Cardiovasc Surg. 1996;112(1):33–37. https://doi.org/10.1016/S0022-5223(96)70175-7
He GW. A New Technique of Transannular Monocusp Patch-Repair of the Right Ventricular Outflow Tract in Repair of Tetralogy of Fallot. Hear Lung Circ. 2007;16(2):107–112. https://doi.org/10.1016/j.hlc.2006.10.013
Acknowledgements
None.
Funding
This work was supported by internal funds.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
X. Zhang, S.B. Kizilski, D.P. Recco, M.D. Chaillo Lizarraga, N.E. Kneier, N.E. Schulz, C.W. Baird, P.E. Hammer, and D.M. Hoganson declare that they have no conflicts of interest.
Informed Patient Consent
In-vitro studies performed with exemption by the Boston Children’s Hospital Institutional Review Board.
Meeting Presentation(s)
Presented as a poster at the AATS 2023 meeting in Los Angeles, Ca on May 8th, 2023.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Editorial responsibility Sarah Vigmostad, Ph.D.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, X., Kizilski, S.B., Recco, D.P. et al. Systematic Analysis of PTFE Monocusp Leaflet Design in a Patient-Based 3D in-Vitro Model of Tetralogy of Fallot. Cardiovasc Eng Tech 14, 827–839 (2023). https://doi.org/10.1007/s13239-023-00690-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13239-023-00690-2