Abstract
Introduction
Illicitly manufactured fentanyl (IMF) is responsible for a growing number of deaths. Some case series have suggested that IMF overdoses require significantly higher naloxone doses than heroin overdoses. Our objective was to determine if the naloxone dose required to treat an opioid overdose is associated with the finding of fentanyl, opiates, or both on urine drug screen (UDS).
Methods
A retrospective chart review was conducted at a single emergency department and its affiliated emergency medical services (EMS) agency. The charts of all patients who received naloxone through this EMS from 1/1/2017 to 6/15/2018 were reviewed. The study included patients diagnosed with a non-suicidal opioid overdose whose UDS was positive for opiates, fentanyl, or both. Data collected included demographics, vital signs, initial GCS, EMS and ED naloxone administrations, response to treatment, laboratory findings, and ED disposition. The fentanyl-only and fentanyl + opiate groups were compared to the opiate-only group using the stratified (by ED provider) variant of the Mann-Whitney U test.
Results
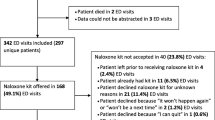
Eight hundred and thirty-seven charts were reviewed, and 121 subjects were included in the final analysis. The median age of included subjects was 38 years and 75% were male. In the naloxone dose analysis, neither the fentanyl-only (median 0.8 mg, IQR 0.4–1.6; p = 0.68) nor the fentanyl + opiate (median 0.8 mg, IQR 0.4–1.2; p = 0.56) groups differed from the opiate-only group (median 0.58 mg, IQR 0.4–1.6).
Conclusion
Our findings refute the notion that high potency synthetic opioids like illicitly manufactured fentanyl require increased doses of naloxone to successfully treat an overdose. There were no significant differences in the dose of naloxone required to treat opioid overdose patients with UDS evidence of exposure to fentanyl, opiates, or both. Further evaluation of naloxone stocking and dosing protocols is needed.


Similar content being viewed by others
References
Ahmad F, Rossen L, Spencer M, Warner M, Sutton P. Provisional drug overdose death counts. National Center for Health Statistics; 2018.
Kochanek K, Muprhy S, Xu J, Arias E. Mortality in the United States, 2016 National Center for Health Statistics; 2017.
Peterson AB, Gladden RM, Delcher C, Spies E, Garcia-Williams A, Wang Y, et al. Increases in fentanyl-related overdose deaths—Florida and Ohio, 2013-2015. MMWR Morb Mortal Wkly Rep. 2016;65(33):844–9.
CDC Health Alert Network. Increases in fentanyl drug confiscations and fentanyl-related overdose fatalities. 2015. https://emergency.cdc.gov/han/han00384.asp. Accessed 10 Apr 2019.
Rudd R, Seth P, David F, Scholl L. Increases in drug and opioid-involved overdose deaths—United States, 2010–2015. MMWR Morb Mortal Wkly Rep. 2016;65:1445–52.
Hedegaard H, Warner M, Miniño AM. Drug overdose deaths in the United States, 1999–2017: National Center for Health Statistics; 2018.
Stogner JM. The potential threat of acetyl fentanyl: legal issues, contaminated heroin, and acetyl fentanyl disguised as other opioids. Ann Emerg Med. 2014;64(6):637–9.
Wanger K, Brough L, Macmillan I, Goulding J, MacPhail I, Christenson JM. Intravenous vs subcutaneous naloxone for out-of-hospital management of presumed opioid overdose. Acad Emerg Med. 1998;5(4):293–9.
Robertson TM, Hendey GW, Stroh G, Shalit M. Intranasal naloxone is a viable alternative to intravenous naloxone for prehospital narcotic overdose. Prehosp Emerg Care. 2009;13(4):512–5.
Schumann H, Erickson T, Thompson TM, Zautcke JL, Denton JS. Fentanyl epidemic in Chicago, Illinois and surrounding Cook County. Clin Toxicol. 2008;46(6):501–6.
Somerville NJ, O'Donnell J, Gladden RM, Zibbell JE, Green TC, Younkin M, et al. Characteristics of fentanyl overdose—Massachusetts, 2014-2016. MMWR Morb Mortal Wkly Rep. 2017;66(14):382–6.
Scheuermeyer FX, DeWitt C, Christenson J, Grunau B, Kestler A, Grafstein E, et al. Safety of a brief emergency department observation protocol for patients with presumed fentanyl overdose. Ann Emerg Med. 2018;72:1):1–8. e1.
Cretikos MA, Bellomo R, Hillman K, Chen J, Finfer S, Flabouris A. Respiratory rate: the neglected vital sign. Med J Aust. 2008;188(11):657–9.
Evans J, Hogg M, Lunn J, Rosen M. Degree and duration of reversal by naloxone of effects of morphine in conscious subjects. Br Med J. 1974;2(5919):589–91.
McDonald R, Lorch U, Woodward J, Bosse B, Dooner H, Mundin G, et al. Pharmacokinetics of concentrated naloxone nasal spray for opioid overdose reversal: phase I healthy volunteer study. Addiction. 2018;113(3):484–93.
Food and Drug Administration. Prescribing information for naloxone nasal spray. https://www.accessdata.fda.gov/drugsatfda_docs/label/2015/208411lbl.pdf. Accessed 10 Apr 2019.
Immunalysis Corporation. Fentanyl urine HEIA drug screening kit. https://immunalysis.com/wp-content/uploads/2016/10/Fentanyl_HEIA_MKT50368_2.pdf. Accessed 10 Apr 2019.
Boyer EW. Management of opioid analgesic overdose. N Engl J Med. 2012;367(2):146–55.
Osterwalder JJ. Naloxone—for intoxications with intravenous heroin and heroin mixtures-harmless or hazardous? A prospective clinical study. J Toxicol Clin Toxicol. 1996;34(4):409–16.
Carroll JJ, Marshall BD, Rich JD, Green TC. Exposure to fentanyl-contaminated heroin and overdose risk among illicit opioid users in Rhode Island: a mixed methods study. Int J Drug Policy. 2017;46:136–45.
Ciccarone D, Ondocsin J, Mars SG. Heroin uncertainties: exploring users’ perceptions of fentanyl-adulterated and-substituted ‘heroin’. Int J Drug Policy. 2017;46:146–55.
National Institute on Drug Abuse. Opioid overdose reversal with naloxone (Narcan, Evzio). https://www.drugabuse.gov/related-topics/opioid-overdose-reversal-naloxone-narcan-evzio. Accessed 10 Apr 2019.
Harm Reduction Coalition. Guide to developing and managing overdose prevention and take-home naloxone projects. 2012.
Strang J, Manning V, Mayet S, Best D, Titherington E, Santana L, et al. Overdose training and take-home naloxone for opiate users: prospective cohort study of impact on knowledge and attitudes and subsequent management of overdoses. Addiction. 2008;103(10):1648–57.
Silverstein JH, Rieders MF, McMullin M, Schulman S, Zahl K. An analysis of the duration of fentanyl and its metabolites in urine and saliva. Anesth Analg. 1993;76(3):618-21.
Vandevenne M, Vandenbussche H, Verstraete A. Detection time of drugs of abuse in urine. Acta Clin Belg. 2000;55(6):323–33.
Funding
This work was unfunded.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
None.
Additional information
Supervising Editor: Michael Levine, MD
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Carpenter, J., Murray, B.P., Atti, S. et al. Naloxone Dosing After Opioid Overdose in the Era of Illicitly Manufactured Fentanyl. J. Med. Toxicol. 16, 41–48 (2020). https://doi.org/10.1007/s13181-019-00735-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13181-019-00735-w