Abstract
Background
We have previously shown that amplification of Mycobacterium tuberculosis specific DNA (TB PCR) from feces reliably diagnosed intestinal tuberculosis. This study was undertaken to determine how well this test would distinguish intestinal tuberculosis from Crohn’s disease in a country endemic for tuberculosis.
Methods
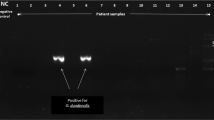
Consecutive patients with diagnoses of Crohn’s disease and intestinal tuberculosis were enrolled, and the diagnoses confirmed by follow up. DNA was extracted from fecal samples and subjected to polymerase chain reaction TB PCR for IS6110 sequence which is specific for M. tuberculosis.
Results
Twenty one of 24 patients with intestinal tuberculosis and 5 of 44 patients with Crohn’s disease tested positive by TB PCR. The sensitivity, specificity, positive predictive and negative predictive values for TB PCR in distinguishing tuberculosis from Crohn’s disease were 0.79 (95% confidence interval 0.57–0.92), 0.88 (0.75–0.96), 0.79 (0.57–0.92) and 0.88 (0.75–0.96), respectively. A combination of fecal TB PCR with mycobacterial culture of mucosal biopsy specimens identified 23 of 24 (96.2%) of patients with intestinal TB, with sensitivity, specificity, positive predictive and negative predictive values (95% CI) of 0.95 (0.78–0.99), 0.88 (0.75–0.96), 0.82 (0.63–0.93) and 0.97 (0.86–0.99), respectively.
Conclusion
Fecal TB PCR is a good screening test to distinguish intestinal tuberculosis from Crohn’s disease.

Similar content being viewed by others
References
Desai HG, Gupte PA. Increasing incidence of Crohn’s disease in India: is it related to improved sanitation? Indian J Gastroenterol. 2005;24:23–4.
Das K, Ghoshal UC, Dhali GK, Benjamin J, Ahuja V, Makharia GK. Crohn’s disease in India: a multicenter study from a country where tuberculosis is endemic. Dig Dis Sci. 2009;54:1099–107.
Isbister WH, Hubler M. Inflammatory bowel disease in Saudi Arabia: presentation and initial management. J Gastroenterol Hepatol. 1998;13:1119–24.
Ouyang Q, Tandon R, Goh KL, et al. The emergence of inflammatory bowel disease in the Asian Pacific region. Curr Opin Gastroenterol. 2005;21:408–13.
Dye C. Global epidemiology of tuberculosis. Lancet. 2006;367:938–40.
Almadi MA, Ghosh S, Aljebreen AM. Differentiating intestinal tuberculosis from Crohn’s disease: a diagnostic challenge. Am J Gastroenterol. 2009;104:1003–12.
Epstein D, Watermeyer G, Kirsch R. Review article: the diagnosis and management of Crohn’s disease in populations with high-risk rates for tuberculosis. Aliment Pharmacol Ther. 2007;25:1373–88.
Amarapurkar DN, Patel ND, Rane PS. Diagnosis of Crohn’s disease in India where tuberculosis is widely prevalent. World J Gastroenterol. 2008;14:741–6.
Pulimood AB, Peter S, Ramakrishna B, et al. Segmental colonoscopic biopsies in the differentiation of ileocolic tuberculosis from Crohn’s disease. J Gastroenterol Hepatol. 2005;20:688–96.
Makharia GK, Sachdev V, Gupta R, Lal S, Pandey RM. Anti-Saccharomyces cerevisiae antibody does not differentiate between Crohn’s disease and intestinal tuberculosis. Dig Dis Sci. 2007;52:33–9.
Amarapurkar DN, Patel ND, Amarapurkar AD, Agal S, Baigal R, Gupte P. Tissue polymerase chain reaction in diagnosis of intestinal tuberculosis and Crohn’s disease. J Assoc Physicians India. 2004;52:863–7.
Kim KM, Lee A, Choi KY, Lee KY, Kwak JJ. Intestinal tuberculosis: clinicopathologic analysis and diagnosis by endoscopic biopsy. Am J Gastroenterol. 1998;93:606–9.
Gan HT, Chen YQ, Ouyang Q, Bu H, Yang XY. Differentiation between intestinal tuberculosis and Crohn’s disease in endoscopic biopsy specimens by polymerase chain reaction. Am J Gastroenterol. 2002;97:1446–51.
Makharia GK, Srivastava S, Das P, et al. Clinical, endoscopic, and histological differentiations between Crohn’s disease and intestinal tuberculosis. Am J Gastroenterol. 2010;105:642–51.
Pulimood AB, Peter S, Rook GW, Donoghue HD. In situ PCR for Mycobacterium tuberculosis in endoscopic mucosal biopsy specimens of intestinal tuberculosis and Crohn disease. Am J Clin Pathol. 2008;129:846–51.
Balamurugan R, Venkataraman S, John KR, Ramakrishna BS. PCR amplification of the IS6110 insertion element of Mycobacterium tuberculosis in fecal samples from patients with intestinal tuberculosis. J Clin Microbiol. 2006;44:1884–6.
Shah S, Thomas V, Mathan M, et al. Colonoscopic study of 50 patients with colonic tuberculosis. Gut. 1992;33:347–51.
Pugazhendhi S, Amte A, Balamurugan R, Subramanian V, Ramakrishna BS. Common NOD2 mutations are absent in patients with Crohn’s disease in India. Indian J Gastroenterol. 2008;27:201–3.
Hogan WJ, Hensley GT, Geenen JE. Endoscopic evaluation of inflammatory bowel disease. Med Clin North Am. 1980;64:1083–102.
Katoch VM. Newer diagnostic techniques for tuberculosis. Indian J Med Res. 2004;120:418–28.
Chauhan DS, Sharma VD, Parashar D, et al. Molecular typing of Mycobacterium tuberculosis isolates from different parts of India based on IS6110 element polymorphism using RFLP analysis. Indian J Med Res. 2007;125:577–81.
Singh SK, Verma R, Shah DH. Molecular fingerprinting of clinical isolates of Mycobacterium bovis and Mycobacterium tuberculosis from India by restriction fragment length polymorphism (RFLP). J Vet Sci. 2004;5:331–5.
Tzen CY, Wu TY, Tzen CY. Detection of mycobacteria in Crohn’s disease by a broad spectrum polymerase chain reaction. J Formos Med Assoc. 2006;105:290–8.
Chiappini E, de Martino M, Mangiantini F, Lionetti P. Crohn disease and mycobacterial infection in children: an intriguing relationship. J Pediatr Gastroenterol Nutr. 2009;49:550–8.
Garcia-Vidal C, Rodríguez-Fernández S, Teijón S, et al. Risk factors for opportunistic infections in infliximab-treated patients: the importance of screening in prevention. Eur J Clin Microbiol Infect Dis. 2009;28:331–7.
Bruns H, Meinken C, Schauenberg P, et al. Anti-TNF immunotherapy reduces CD8+ T cell-mediated antimicrobial activity against Mycobacterium tuberculosis in humans. J Clin Invest. 2009;119:1167–77.
Caviglia R, Boskoski I, Cicala M. Long-term treatment with infliximab in inflammatory bowel disease: safety and tolerability issues. Expert Opin Drug Saf. 2008;7:617–32.
Mow WS, Abreu-Martin MT, Papadakis KA, Pitchon HE, Targan SR, Vasiliauskas EA. High incidence of anergy in inflammatory bowel disease patients limits the usefulness of PPD screening before infliximab therapy. Clin Gastroenterol Hepatol. 2004;2:309–13.
Lalvani A, Millington KA. Screening for tuberculosis infection prior to initiation of anti-TNF therapy. Autoimmun Rev. 2008;8:147–52.
Acknowledgements
The study was supported by an intramural Fluid Research Grant from the Christian Medical College, Vellore. Balamurugan Ramadass was supported by a Senior Research Fellowship from the Indian Council of Medical Research. The laboratory was supported by FIST grant no. SR/FST/LSI-141/2002 from the Department of Science and Technology, Government of India.
Competing Interest
None to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ramadass, B., Chittaranjan, S., Subramanian, V. et al. Fecal polymerase chain reaction for Mycobacterium tuberculosis IS6110 to distinguish Crohn’s disease from intestinal tuberculosis. Indian J Gastroenterol 29, 152–156 (2010). https://doi.org/10.1007/s12664-010-0022-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12664-010-0022-3